When pain starts shaping your day, the search for a specialist usually doesn't begin in a calm, organized way. It begins when getting out of bed takes planning, when driving hurts, when sleep stops feeling restorative, or when you've already heard some version of “try to give it time” one too many times.
Most patients don't need just any specialist. They need the right specialist for the kind of pain they're living with.
The Search Begins When Pain Becomes Your Everyday
A common pattern looks like this. Your back, neck, joint, or nerve pain starts as something manageable. Then it lingers. Then it spreads into work, walking, exercise, sleep, and mood. You may have already seen an urgent care doctor, a primary care physician, or another provider and still feel like nobody has connected the dots.
That frustration is real, especially for people trying to decide whether they need a neurologist, orthopedic surgeon, physiatrist, chiropractor, or pain specialist. If your symptoms are persistent, radiating, post-surgical, injury-related, or affecting daily function, the better question is often not “Who treats pain?” but “Who treats my kind of pain with the right tools?”

For patients in Illinois, there is an access advantage, but it shouldn't create false confidence. The U.S. physician supply varies by geography, with a 3.5-fold difference between the best- and worst-supplied areas, and the Chicago metropolitan area generally offers stronger access to specialists than underserved regions, according to NEJM CareerCenter physician workforce tracking. Better access helps. It doesn't automatically lead you to the right doctor.
Why local access still requires a strategy
If you live in Oak Lawn, Palos Hills, Palos Heights, Worth, Bridgeview, Hickory Hills, Alsip, Burbank, Evergreen Park, Orland Park, or near Chicago Ridge, you have more options than many patients elsewhere in the country. That's good news.
The challenge is that more options can also create more confusion. A long provider list doesn't tell you who treats lumbar radiculopathy, facet pain, sacroiliac dysfunction, post-laminectomy pain, vertebral compression fractures, chronic migraine, or nerve-related pain with a thoughtful plan.
The right referral changes the whole course of care. The wrong one can cost months.
A smart first step is to define the problem as specifically as possible. Instead of searching “back pain,” search by pattern and condition. If you're not sure what those categories are yet, reviewing a clear list of pain conditions commonly evaluated by an interventional clinic can help you describe what you're feeling more accurately before you book.
Building Your Initial List of Potential Specialists
Begin broad, then narrow quickly. Many individuals waste time doing the reverse.
If you're asking “How to find a specialist doctor?” for chronic pain, begin with three channels at the same time: professional referrals, insurance filtering, and targeted local search. That combination gives you a workable list without relying on whichever website happens to rank first.

Recent workforce data adds urgency. 78% of physician recruitment searches focused on specialists, and interventional pain management and related fields are among the specialties facing projected shortages, according to the American Medical Association specialty demand overview. That means vague searching and delayed follow-up can leave patients stuck on waitlists or in the wrong office.
Start with people who know your case
The best first referrals often come from clinicians who already understand your history.
- Primary care physicians: They know your medication history, prior imaging, and medical comorbidities.
- Chiropractors and rehab providers: They often recognize when pain is no longer responding to conservative care alone and needs procedural evaluation.
- Surgeons or post-op teams: If you've had spine, joint, or injury-related treatment, they may know which pain doctors handle more complex cases well.
When you ask for a referral, don't ask only “Who do you send patients to?” Ask, “Who handles this specific problem well?” That's a better question.
Use your insurance directory carefully
Insurance directories are useful for creating a first-pass list. They are not reliable enough to be your final decision tool.
Search under terms such as:
- Pain medicine
- Interventional pain management
- Pain management physician
- Anesthesiology with pain medicine
- Spine and pain specialist
Then narrow by city. Search phrases like:
- pain specialist Orland Park IL
- interventional pain doctor Oak Lawn
- pain management Palos Heights IL
- back pain specialist Evergreen Park IL
- nerve pain doctor Alsip IL
- interventional pain management Bridgeview IL
- pain doctor Hickory Hills IL
- pain specialist Burbank IL
- pain management Worth IL
- interventional pain physician Palos Hills IL
Build a list with filters that matter
Once you have names, keep only the doctors and clinics that appear to match your actual needs.
Look for these signs on the practice website or appointment page:
- Procedure-based care: The site mentions image-guided injections, radiofrequency ablation, spinal cord stimulation, epidural procedures, facet treatment, sacroiliac interventions, kyphoplasty, MILD, or Vertiflex.
- Condition clarity: The practice explains what it treats, not just that it “manages pain.”
- Care coordination: The office references working with surgeons, primary care doctors, chiropractors, or therapists.
- Practical access: The office clearly states how to request an appointment, what insurance steps may apply, and what records to bring.
Practical rule: Build a list of several realistic options, then vet them hard. Don't commit based on the first name you see online.
How to Vet a Doctor's Expertise Beyond Online Reviews
Online reviews can tell you whether a front desk is disorganized or whether parking is difficult. They are much less reliable for judging procedural skill.
That matters in pain medicine because two doctors may both be called “pain specialists” while practicing very differently. One may focus mainly on medication management. Another may perform image-guided procedures every week, evaluate surgical alternatives appropriately, and coordinate care when conservative treatment fails.
What credentials actually tell you
Start with board certification and fellowship training. In pain medicine, these aren't decorative credentials. They tell you whether the physician completed advanced training focused on diagnosis, procedures, and complex pain conditions.
For interventional care, it also helps to look for a doctor whose background aligns with the procedures you may need. A physician trained in anesthesiology and pain medicine, for example, often has a strong procedural foundation. If you want to understand what that looks like in a real physician profile, Dr. Yaw Donkoh's background and training offers a concrete example of the credentials patients should learn to verify.
Ask about the procedure, not just the diagnosis
If you have chronic back pain, the diagnosis alone isn't enough. The essential question is whether the doctor has experience with the specific treatment path under consideration.
Verified guidance on specialist selection shows that procedure-specific volume matters. Specialists who perform more than 50 annual cases of a specific procedure can reduce revision rates by 15%, and patient reviews have only a 60 to 70% correlation with actual competence, according to guidance on researching a surgeon and procedural expertise.
That leads to better questions:
| Category | Question to Ask |
|---|---|
| Credentials | Are you board-certified in pain medicine, and what fellowship training did you complete? |
| Diagnosis fit | Do you treat my condition often, or is this outside your usual case mix? |
| Procedure volume | How many of this specific procedure do you perform in a year? |
| Imaging guidance | Do you use fluoroscopy or other image guidance for injections and spine procedures? |
| Treatment philosophy | Do you emphasize opioid-sparing and multimodal care when appropriate? |
| Care pathway | If the first treatment doesn't help, what is your next step? |
| Coordination | Do you communicate with my primary doctor, surgeon, or therapist? |
| Follow-up | How do you monitor outcomes after a procedure? |
Ask people who see technical skill up close
This is an underused strategy, and it's often one of the most revealing. If you know anyone connected to surgery or hospital care, ask whether they have insight into a doctor's technical reputation.
One especially useful question from the verified guidance above is: “Which surgeon would you choose for your mother?” Nurses, anesthesiologists, scrub techs, and OR staff often have a sharper view of judgment, precision, and consistency than public review sites do.
Warning signs during vetting
Some signals should lower your confidence early.
- Vague answers about experience: If nobody can tell you whether the doctor regularly performs your procedure, that's a problem.
- No clear diagnostic reasoning: A good doctor should explain why they believe the pain source is a nerve root, facet joint, sacroiliac joint, disc, compression fracture, headache generator, or something else.
- Heavy dependence on reviews: If the strongest evidence for a clinic is “patients love us,” keep looking.
- No affiliation or coordination: A specialist who practices in isolation may still be competent, but complex pain usually requires communication beyond one office.
A specialist should be able to explain not only what they do, but why your pain pattern makes that treatment reasonable.
Finding a Partner in Pain Management Not Just a Provider
You may start with a simple search. Back pain specialist. Sciatica doctor. Migraine treatment. Then you arrive at a long list of names that all look qualified, while your day still revolves around pain, sleep disruption, missed work, and canceled plans.
That is where the crucial decision starts. A pain doctor's title tells you very little about how that practice treats patients. Some clinics focus mainly on medication management. Others are built around interventional pain care, using image-guided procedures, careful diagnosis, and function-based treatment plans with an opioid-sparing approach when appropriate. Standard doctor directories rarely show that difference clearly.
Treatment philosophy matters as much as diagnosis.
Two people can both carry the label "low back pain" and need completely different care. One may have facet joint pain and respond to medial branch blocks or radiofrequency ablation. Another may have lumbar spinal stenosis and need evaluation for MILD or Vertiflex. A third may have persistent nerve pain after surgery and need a neuromodulation workup. Good pain care starts with identifying the pain generator, then matching the treatment to that problem, not forcing every patient into the same menu.
Look for a practice that can explain when it uses, and when it does not use, options such as:
- Image-guided injections to confirm the pain source and treat it precisely
- Radiofrequency ablation for selected facet-mediated pain
- Spinal cord stimulation or peripheral nerve stimulation for carefully chosen nerve-related cases
- MILD and Vertiflex for appropriate lumbar stenosis patients
- Kyphoplasty for vertebral compression fractures
- PRP or regenerative treatments in the right clinical setting
- Botox for certain headache disorders or cervical dystonia
In my field, restraint matters. A strong interventional pain physician should be comfortable saying, "A procedure is not the right next step yet," and explaining what needs to happen first.
Partnership also means coordinated care. Complex pain often crosses specialties. A patient may need an injection, medication changes, physical therapy, updated imaging, a surgical opinion, and communication with a primary care doctor. If each part happens in isolation, progress stalls and patients get conflicting advice.
The better model is a team that communicates. In the Chicago area, that often means a pain specialist who works well with spine surgeons, primary care clinicians, therapists, chiropractors, and rehabilitation staff when the case calls for it. Midwest Pain & Wellness is one example of that kind of coordinated, interventional practice, and patients who want to start care can request an appointment with an interventional pain specialist.
A few patterns should make you cautious:
- Medication-first care without a clear diagnostic plan
- The same treatment recommendation for every patient with the same body part complaint
- Little discussion of function, goals, or what success would look like
- No communication with outside clinicians
- Procedures offered without careful patient selection
The right doctor does more than prescribe or perform injections. The right doctor helps you understand the problem, choose the next step for the right reason, and adjust the plan when your body gives new information.
Navigating Insurance Referrals and Appointment Logistics
A good specialist isn't helpful if you can't get through the front door. Insurance rules, referrals, accepted plans, and scheduling details derail a lot of patients before care even begins.
One verified point is especially important here. HMO plans can reduce out-of-pocket costs by 50 to 70%, but they often restrict access to top specialists, and online directories may be outdated. That's why it's essential to confirm coverage directly with the office, as explained in this guidance on finding the right doctor and verifying insurance details.
Call the office before you assume you're covered
Don't stop at “I found them in my directory.”
When you call, ask:
- Do you accept my exact insurance plan?
- Are you accepting new patients?
- Do I need a referral or authorization before the visit?
- Do you treat my condition or perform evaluations for my type of pain?
- What records should I send before the appointment?
- Do you see workers' compensation or personal injury cases?
If you have an HMO, ask your primary care office whether the referral must name a specific doctor, a specific location, or both. Small administrative errors can delay care.
Use a short script and write everything down
Keep it simple. “I have chronic back and leg pain. I'd like to confirm whether Dr. X is in-network for my exact plan, whether new patients are being accepted, and whether I need a referral or prior authorization before scheduling.”
Then write down the date, the person you spoke with, and what they told you. If coverage turns into a dispute later, that note matters.
Logistics can signal how a practice runs
Pay attention to how the office handles your first contact.
- Clear answers are a good sign
- Confusion about insurance may mean billing problems later
- Long delays in basic communication can predict a frustrating care experience
If you live in Bridgeview, Burbank, Hickory Hills, or nearby communities and your pain is related to a work injury or accident, ask directly whether the clinic handles those case types. Not every practice does. If you're ready to book or verify next steps, a direct appointment request page for Midwest Pain & Wellness shows the kind of information an organized clinic should make easy to find.
Your First Visit Green Flags and Red Flags
Your first visit should help you decide whether this doctor is someone you trust with an ongoing problem. It is not only about receiving a treatment recommendation. It is also about judging the quality of the thinking behind that recommendation.
Bring your imaging reports, procedure history, medication list, prior treatment records, and a short summary of what makes the pain better or worse. If the pain radiates, causes numbness, interrupts sleep, limits walking, or affects work, say that clearly. Functional impact matters.
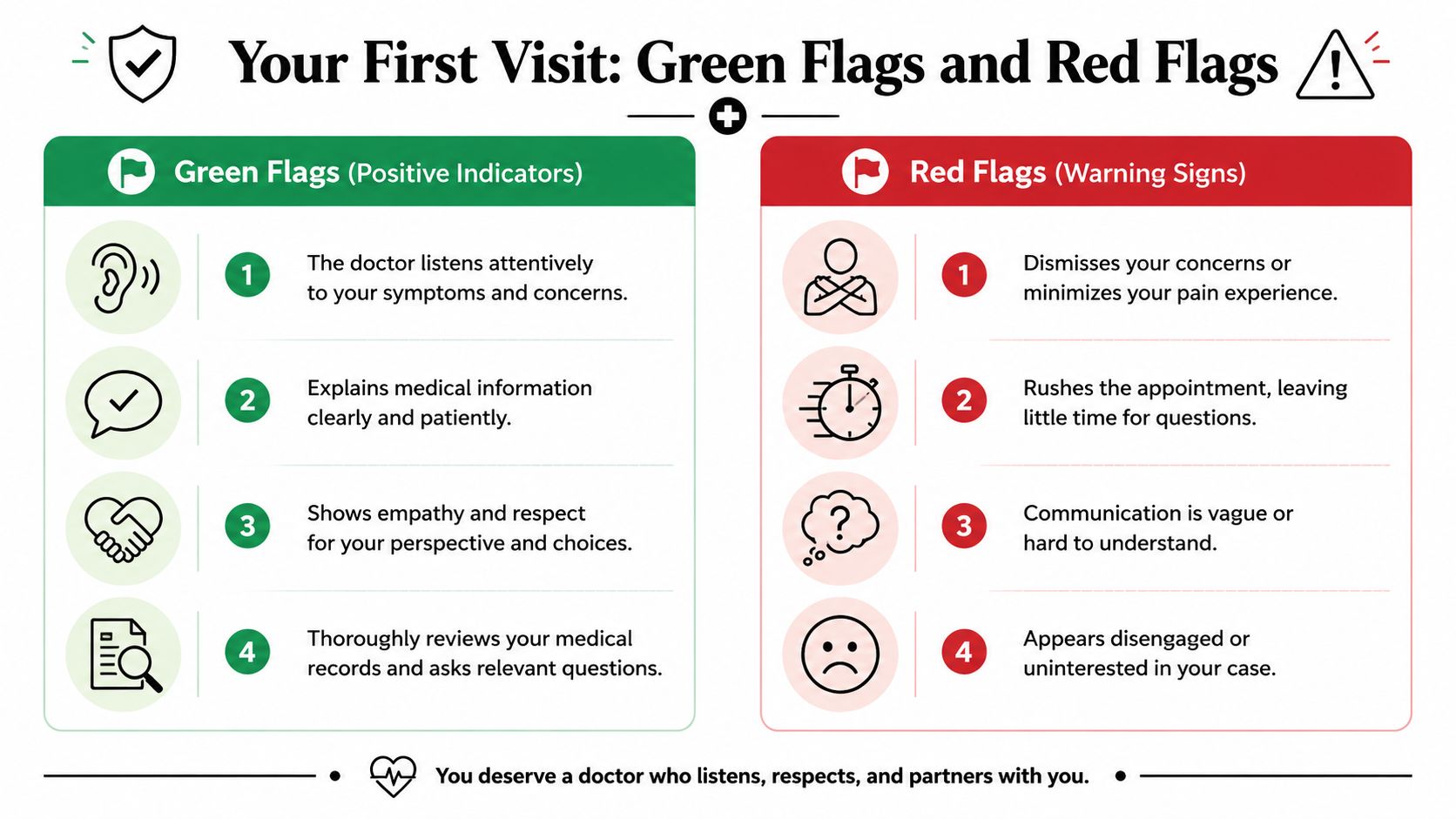
Green flags worth noticing
A strong first visit usually feels structured, thoughtful, and calm.
- They listen before they conclude: The doctor lets you describe the pattern of pain, not just the location.
- They examine with a purpose: The physical exam connects to the history instead of feeling rushed or generic.
- They explain the suspected pain generator clearly: You should hear a working diagnosis in plain language.
- They offer a stepwise plan: Good care usually includes diagnostic clarity, initial treatment, and a backup plan if the first step doesn't help.
- They discuss alternatives: A specialist should explain why a procedure, medication adjustment, rehab strategy, or surgical referral does or doesn't make sense.
- They think in teams when needed: For complex pain, the specialist's network matters as much as individual skill. Top-tier specialists coordinate with surgeons, primary care providers, and therapists, while fragmented care can lead to duplicative testing and delayed relief, according to the National Institute on Aging guidance on choosing a doctor you can talk to.
Good pain care sounds specific. It doesn't sound scripted.
Red flags that should make you pause
Some warning signs appear early.
- Your pain is minimized: If the doctor seems dismissive, you're unlikely to get careful long-term management.
- The plan is vague: “Let's just see” is not enough if there is no diagnostic reasoning behind it.
- Everything points to medication immediately: Medication can have a role, but a specialist should still evaluate why the pain exists and whether targeted treatment fits.
- They promise too much: Be cautious with “guaranteed relief,” “miracle fix,” or anything that skips uncertainty.
- No one talks about coordination: If the office has no process for communicating with your surgeon, primary doctor, or therapist when needed, that's a practical problem.
A simple decision test
After the visit, ask yourself three questions:
- Do I understand what this doctor thinks is causing my pain?
- Do I understand the next step and the reason for it?
- Do I feel this office will stay engaged if the first treatment doesn't solve everything?
If the answer to those questions is no, keep looking. A specialist relationship should leave you better informed, not more confused.
If you're in Oak Lawn, Palos Hills, Palos Heights, Worth, Bridgeview, Hickory Hills, Alsip, Burbank, Evergreen Park, Orland Park, or near Chicago Ridge and need evaluation for spine, joint, nerve, injury, post-surgical, or headache-related pain, Midwest Pain & Wellness offers interventional, opioid-sparing care with coordinated treatment planning.



