Back pain usually starts with a small bargain you make with yourself. Give it a few days. Stretch a little. Use a heating pad. Sit differently in the car. Wait until the weekend. Then a few days turn into weeks, the pain starts shaping your schedule, and every search result seems to offer a different answer.
That's the problem with most advice about how to fix back pain. It treats every back the same.
A person in Oak Lawn who flared up after lifting at work, a retired adult in Palos Heights with spinal stenosis, and a commuter from Orland Park whose leg pain worsens every time they sit in traffic do not need the same plan. Some people improve with simple self-care and a structured return to movement. Others need a more precise diagnosis, coordinated rehabilitation, and targeted interventional treatment to stop the cycle before it becomes chronic.
Navigating Back Pain in the Chicago Suburbs
If you live in Orland Park, Alsip, Burbank, Evergreen Park, or the towns around Chicago Ridge, you've probably seen how back pain changes ordinary routines first. The drive gets harder. Sleep gets lighter. Carrying groceries, getting out of a chair, or standing at the sink starts to feel like a calculation instead of an automatic movement.
That experience is common, but it shouldn't be normalized. Low back pain affected an estimated 619 million people worldwide in 2020, and up to 80% of people in the United States experience it at some point. In the U.S., chronic low back pain impacts 16 million adults and contributes to $86 billion in yearly healthcare costs, according to the World Health Organization fact sheet on low back pain.
What matters to a patient is simpler. Why does it still hurt, and what works?
Back pain care works best when it follows a sequence. Start with the basics that calm an acute flare. Build a spine that tolerates normal life again. Watch for signs that the problem is more than a strain. If self-care stalls, move to a specialist who can pinpoint the pain generator and use opioid-sparing treatment that matches the diagnosis.
Back pain becomes harder to treat when people bounce between random stretches, prolonged rest, repeated urgent care visits, and medications that never address the source.
That's why expertise matters. A physician trained in interventional pain medicine looks beyond “your back hurts” and asks a better question: Is this disc-related pain, facet pain, sacroiliac dysfunction, nerve irritation, spinal stenosis, a compression fracture, or a mixed pattern? Patients looking for a specialist in the Chicago suburbs can learn more about Dr. Yaw Donkoh's background and training.
Immediate Steps for Back Pain Relief at Home
When back pain first flares, the goal isn't to “fix” everything in a day. The goal is to calm the irritated tissue, keep the body from stiffening up, and avoid turning a short episode into a longer one.
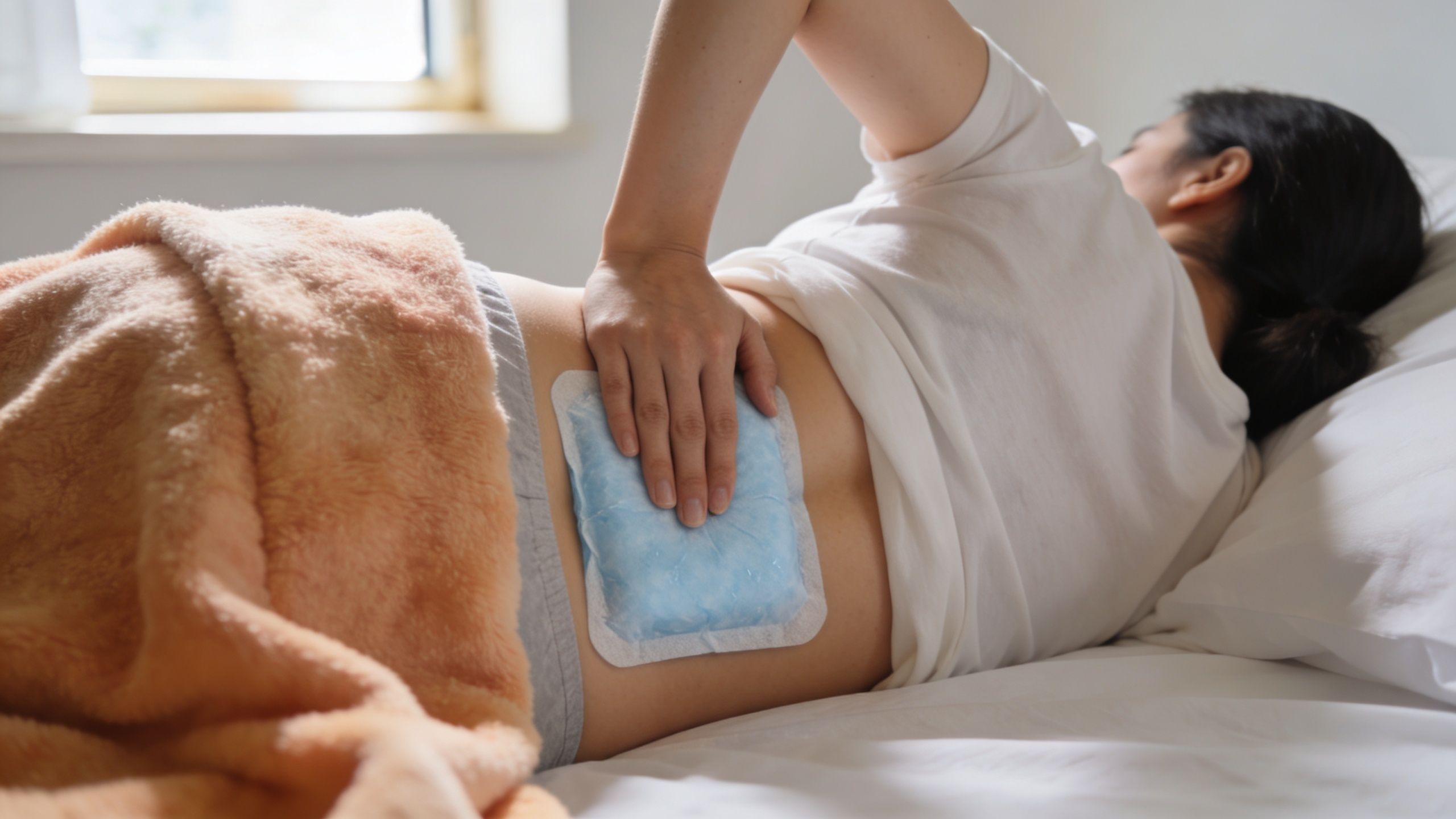
Use cold and heat for different jobs
Many people ask whether ice or heat is better. The answer depends on what the pain is doing.
Use cold when the area feels newly inflamed, sharply aggravated, or more irritated after activity. A cooling gel pack or wrapped ice pack can help settle an acute flare, especially in the first stretch after pain starts or after you overdo it.
Use heat when the main problem feels like muscle guarding, stiffness, or a back that loosens only after you move around. A warm shower, heating pad, or heated wrap can reduce that protective spasm.
A practical approach:
| Situation | Better starting choice | Why |
|---|---|---|
| Fresh flare after lifting, twisting, or a sudden spasm | Cold | Helps calm irritation |
| Tight, stiff back that feels worse after sitting still | Heat | Helps relax guarded muscles |
| Soreness after activity | Cold first | Often useful if the area feels irritated |
| Stiffness later in the day or first thing in the morning | Heat | Eases movement |
Some patients also like alternating the two. If you do that, keep it simple and pay attention to your symptoms. If one clearly helps more, stick with that.
Don't choose bed rest
Complete bed rest is one of the most common mistakes I see. It feels protective, but too much rest usually leads to more stiffness, more fear of movement, and slower recovery.
Active recovery works better. That means doing small, tolerable movements instead of forcing exercise.
Try these examples:
- Short walks: Start with a brief walk inside the house or down the block. Stop before your mechanics get sloppy.
- Gentle position changes: Alternate sitting, standing, and lying down instead of staying in one posture for long stretches.
- Easy pelvic tilts or supported knee-to-chest motions: Use light movement to reduce stiffness, not to chase a dramatic stretch.
- Calm diaphragmatic breathing: Slow breathing reduces the muscle bracing that often amplifies pain.
Practical rule: If a movement causes a clear spike that lingers, back off. If it loosens you up without increasing symptoms afterward, that's usually a good sign.
Find a position that takes pressure off
Back pain often improves when you reduce spinal load in a simple way.
A few reliable options:
- On your back with knees bent and a pillow under the knees.
- On your side with a pillow between the knees if rotation feels irritating.
- Reclined rather than bolt upright if sitting straight makes symptoms worse.
- Supported lumbar curve with a small rolled towel if that feels relieving.
Relief positions aren't treatment by themselves, but they can break a pain spike and make it easier to move again.
Use over-the-counter medication carefully
Some people get short-term relief from over-the-counter pain relievers. If you're considering them, use the label directions and think about your own medical history first. Anti-inflammatory medicines are not right for everyone, especially if you have stomach, kidney, blood pressure, or bleeding concerns. Acetaminophen also isn't right for everyone, especially if liver issues are a concern.
If you already take prescription medication, or if you're older and managing several health conditions, it's smart to check with your physician or pharmacist before adding anything.
What usually doesn't work at home
The biggest trap is doing too much, too fast, because you want the pain gone immediately.
Avoid these common errors:
- Aggressive stretching: If the tissue is irritated, forcing a deep stretch can make it angrier.
- All-day sitting with “perfect posture”: Rigid posture isn't the goal. Frequent position changes matter more.
- Random online exercise routines: They may help one type of back pain and aggravate another.
- Ignoring leg symptoms: Pain that shoots, burns, or travels down the leg often needs more than generic home care.
If your symptoms are settling, keep going with calm movement and simple symptom control. If they aren't, the next step is not to do more random exercises. It's to build a more deliberate plan.
Building a Resilient Spine with Movement and Ergonomics
Pain relief is only part of how to fix back pain. The longer-term job is teaching the spine and the surrounding muscles to tolerate daily life again. That means movement with good mechanics, followed by changes in the way you sit, lift, sleep, and work.
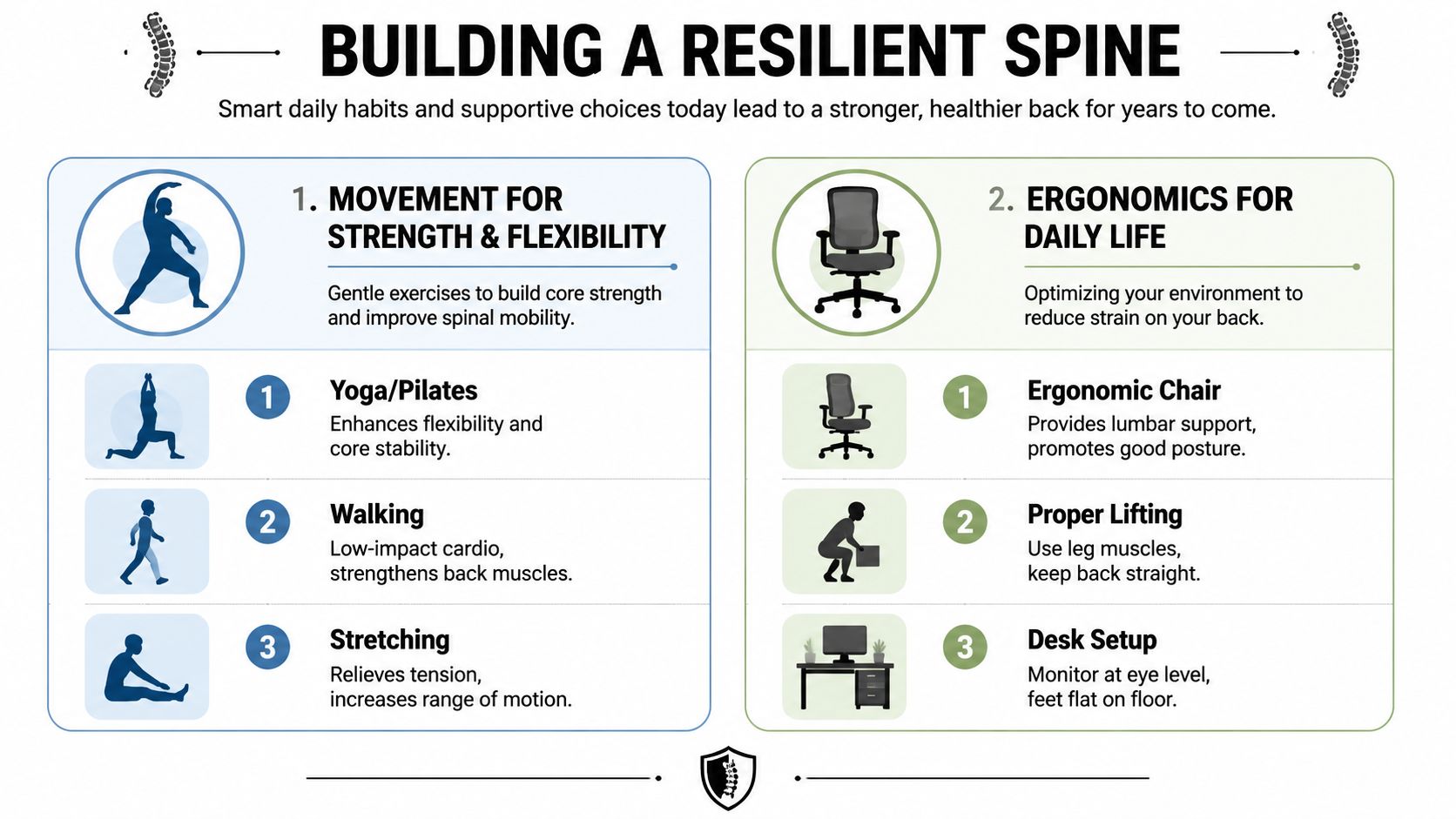
Train stability before intensity
Many patients hear “strengthen your core” and assume they need harder workouts. Usually, they need better control first.
A resilient spine depends on coordinated support from the abdominal wall, back muscles, glutes, hips, and breathing pattern. The goal isn't to flatten the back or hold a rigid brace all day. The goal is to control motion so the spine doesn't keep getting irritated by small daily tasks.
A clinical rehabilitation perspective emphasizes graded exercise, not symptom chasing. Graded exercise programs show superior 5-year outcomes compared with education alone, and an expert benchmark notes that physical therapy used as a first-line treatment can cut opioid use, imaging, and costs by 50% to 70% in workers' compensation cohorts, as summarized in this clinical review on chronic low back pain rehabilitation.
That matters because many people only exercise once the pain is gone. A better approach is to work in a tolerable range, progress carefully, and respect form.
Start with low-threat movements
These foundational exercises are useful because they build support without requiring heavy spinal loading.
Bird-dog
Start on hands and knees. Keep the spine neutral, then extend one leg back without rotating the pelvis. If that stays controlled, add the opposite arm.
What it trains:
- Cross-body control
- Spinal stability during limb movement
- Awareness of rotation you didn't know you had
Common mistake: reaching too high and arching the low back.
Glute bridge
Lie on your back with knees bent. Tighten the glutes and lift the hips without flaring the ribs or overextending the low back.
Why it helps:
- It shifts work into the hips.
- It reduces the habit of moving from the lumbar spine every time you stand up, climb stairs, or lift.
Side-lying leg work or clamshells
These movements aren't glamorous, but they matter. Weak lateral hip control often shows up as poor pelvic control when you walk, climb, and stand on one leg.
Supported hip hinge
Use a dowel, wall, or countertop if needed. Practice bending from the hips while keeping the trunk organized.
This is one of the most useful movement patterns in back care because everyday life is full of hinging. Reaching into the washer, unloading a dishwasher, picking up a child, and grabbing a package from the floor all depend on it.
You don't build a stronger back by repeatedly provoking it. You build it by restoring control, then layering tolerance.
Progression matters more than variety
People often switch exercises too quickly. They assume boredom means progress. It doesn't.
A better progression looks like this:
- Master position and breathing
- Add small, controlled repetitions
- Increase time under tension
- Add load only when mechanics stay clean
- Carry the same mechanics into real tasks
If a person can perform basic stability work well but rounds, twists, or overextends during daily life, the rehab hasn't transferred yet.
Stretching has a place, but it's not the whole answer
Stretching can reduce tension. It can help a stiff hip, tight hamstring, or guarded low back feel less restricted. But stretching alone rarely solves persistent back pain.
Use stretching as support, not as the center of the plan. The body usually needs a mix of:
- Mobility where you're stiff
- Stability where you're uncontrolled
- Load tolerance where you're deconditioned
- Better movement habits in ordinary tasks
Fix the environment that keeps re-irritating your back
A good exercise program can be undone by the way you spend the other part of the day.
For many people in Hickory Hills, Bridgeview, Worth, and Palos Hills, back pain is shaped less by one dramatic injury and more by repetition. Long drives. Desk work. Standing in one place. Poor lifting mechanics. Collapsing into the couch at night.
Workstation basics
If you work at a desk, make these changes:
- Chair support: Use lumbar support that fills the curve of your low back.
- Feet position: Keep feet flat rather than dangling.
- Screen height: Bring the monitor closer to eye level so you're not folding forward all day.
- Keyboard placement: Keep elbows near your sides instead of reaching.
The best desk posture is the one you change often. Set reminders to stand up, walk briefly, or reset your sitting position.
Car setup for commuters
Commuting can aggravate disc pain, sciatica, and stenosis differently. What helps most is reducing the time spent slumped and vibrating in one position.
Try this short checklist:
| Driving issue | Adjustment |
|---|---|
| Low back aching after short drives | Add a small lumbar support |
| Hamstrings and back feel tight when exiting the car | Bring the seat a bit closer to avoid overreaching the pedals |
| Leg symptoms worsen in traffic | Change position when safely stopped and take movement breaks when possible |
| Twisting hurts when getting out | Pivot the whole body instead of twisting out of the seat |
Lifting mechanics
People are often told to “lift with your legs,” which is true but incomplete. Good lifting also depends on keeping the load close, using a hip hinge, and avoiding rotation under load.
A few practical rules:
- Get close to the object
- Brace before the lift
- Use hips and legs to rise
- Turn with the feet instead of twisting through the spine
- Break large awkward tasks into smaller lifts
Sleeping posture can help or hurt
If you wake up worse than you went to bed, your sleep position may be part of the issue.
For many patients:
- Back sleeping improves with a pillow under the knees.
- Side sleeping improves with a pillow between the knees.
- Stomach sleeping often aggravates lumbar extension and neck rotation.
No sleep posture is universal, but the best one is usually the position that lets the back stay supported and the hips stay neutral.
When Self-Care Is Not Enough Recognizing the Red Flags
A lot of people wait too long because they assume all back pain eventually “works itself out.” Some episodes do. Some don't. The skill is knowing the difference.

Red flags that need urgent medical attention
These symptoms can signal a problem that shouldn't wait:
- Loss of bladder or bowel control
- Sudden or progressive leg weakness
- Numbness in the groin or saddle area
- Fever with significant back pain
- Pain after a serious fall or trauma
- Back pain with unexplained weight loss or a known cancer history
These findings raise concern for nerve compression, fracture, infection, or another serious condition. If they're present, the right move isn't more stretching. It's urgent evaluation.
If your leg is getting weaker, or you can't control bladder or bowel function, treat that as a medical issue, not a pain-management experiment.
Yellow flags that mean it's time to see a specialist
These signs are less dramatic, but they matter because they suggest the problem is no longer responding to basic care.
Consider specialist evaluation if:
- Pain keeps returning
- Symptoms persist despite home care
- Pain travels into the buttock, thigh, or below the knee
- Numbness, tingling, or burning becomes part of the pattern
- Walking or standing tolerance keeps shrinking
- You can't sleep, work, drive, or function normally
- You're relying more and more on medication without real recovery
Many people get stuck at this point. They are not in an emergency, but they are no longer dealing with a simple strain either.
The reason to move beyond DIY care is not impatience. It's pattern recognition. A 2023 meta-analysis in The Lancet Rheumatology found that self-directed stretches provided short-term relief but failed long-term, with 70% recurrence rates, while multimodal plans including interventional treatments yielded 60% to 80% sustained relief at 1 year, as described in this summary discussing escalation beyond self-directed stretching.
What a specialist adds
A specialist doesn't just offer a stronger version of home care. The value is diagnostic clarity.
Pain in the low back can come from several structures that create different symptom patterns:
- Disc-related pain
- Facet joint pain
- Sacroiliac joint pain
- Lumbar radiculopathy or sciatica
- Spinal stenosis
- Compression fracture
- Mixed mechanical and nerve pain
Those conditions can overlap, but they don't respond to the same treatment. If your symptoms suggest you've moved beyond simple self-care, review the back, spine, and pain conditions commonly evaluated in specialty care.
A Guide to Advanced Interventional Pain Management
Once conservative care has done what it can, the next question is not whether you've “failed” treatment. The better question is which structure is driving the pain, and which targeted option fits that pattern.
A modern pain strategy is usually multimodal. That means movement-based rehab, symptom-guided medication when appropriate, and targeted procedures when the exam and imaging support them. According to this overview of coordinated multidisciplinary management for chronic low back pain, a multidisciplinary approach that combines exercise, manual therapy, and targeted interventions is optimal, early PT can reduce advanced care needs by 50%, and siloed care has a 60% to 80% failure rate.
That last point matters. A person with persistent back pain often doesn't need “more” care. They need coordinated care.
Image-guided injections for inflammation and nerve irritation
Injections are often misunderstood. They are not magic, and they are not merely temporary numbing shots. Used correctly, they can clarify diagnosis, calm inflammation, and create a window for rehabilitation.
Epidural steroid injections
These are commonly used when pain radiates down the leg or when inflammation around a spinal nerve contributes to sciatica-type symptoms.
Best suited for:
- Lumbar radiculopathy
- Disc-related nerve irritation
- Some cases of spinal stenosis with leg symptoms
Why image guidance matters:
- It improves precision.
- It helps place medication where the inflamed structure is.
Expected role:
- Reduce inflammation enough to improve walking, sleep, and participation in rehab.
- Sometimes help confirm that the irritated nerve root is the pain generator.
Selective nerve root blocks
These are more targeted than a broader epidural. When the question is which nerve is involved, a selective block can be useful diagnostically and therapeutically.
They're helpful when symptoms and imaging don't line up perfectly, or when more than one level could be responsible.
Facet and sacroiliac interventions for mechanical back pain
Not all low back pain comes from discs. Many people have pain generated by the facet joints in the spine or the sacroiliac joint lower in the pelvis.
These patients often describe pain with:
- Standing upright
- Twisting
- Getting out of a chair
- Transitional movements
- Extension-based positions
Medial branch blocks
These are diagnostic injections used to evaluate whether facet joints are a major contributor to pain. If the block provides clear relief in the expected pattern, it supports the diagnosis.
That matters because the next step may be a longer-lasting treatment.
Sacroiliac joint injections
SI joint pain can mimic lumbar pain, buttock pain, and even leg discomfort. Careful history and exam help identify it, but an image-guided SI injection can both confirm the source and reduce inflammation.
Radiofrequency ablation for longer-lasting relief
If diagnostic blocks show that facet-mediated pain is present, radiofrequency ablation may be a strong option.
RFA uses heat generated by radiofrequency energy to disrupt the small nerves carrying pain signals from the facet joints. It does not “burn the spine,” and it does not damage the structural integrity of the back. Its job is to interrupt a pain pathway that has been identified with prior blocks.
Who tends to benefit:
- Patients with confirmed facet joint pain
- People with mechanical low back pain that returns after temporary block relief
- Those trying to avoid escalating medication use
Why patients like it:
- It is opioid-sparing
- It targets a known source
- It can provide durable improvement for the right pattern of pain
Minimally invasive options for lumbar spinal stenosis
Spinal stenosis often produces a distinctive story. Patients say they can stand only briefly, walking becomes limited, and leaning forward on a cart or counter feels better than standing upright.
These cases deserve more than generic exercise advice. When conservative care is no longer enough, minimally invasive procedures may help without moving straight to major surgery.
MILD procedure
Minimally invasive lumbar decompression, often called MILD, is designed for certain patients with lumbar spinal stenosis related to ligament thickening. Through a small access point, the goal is to reduce tissue contributing to canal narrowing.
This option may fit patients who:
- Have neurogenic claudication symptoms
- Struggle with standing and walking tolerance
- Want a less invasive option than open surgery
Vertiflex Superion
The Vertiflex Superion procedure is an interspinous spacer option for selected patients with lumbar stenosis. It helps maintain space in a way that can reduce nerve crowding in extension.
This may be considered when:
- Symptoms improve with bending forward
- Walking and standing are limited
- Anatomy and imaging support the indication
Many stenosis patients don't need to jump from “I tried stretches” to “I need open surgery.” There's often a middle ground.
Spinal cord stimulation and peripheral nerve stimulation
Some pain persists even after surgery, repeated flares, or long-standing nerve irritation. In these cases, neuromodulation may be part of the conversation.
Spinal cord stimulation
A spinal cord stimulator uses electrical signals to change how pain is processed. It does not repair the original anatomy, but it can reduce the intensity of chronic nerve-related pain and improve function in selected patients.
Often considered for:
- Persistent spine-related pain after surgery
- Chronic radicular pain
- Cases where further surgery is not the best option
Peripheral nerve stimulation
For certain focal pain patterns, peripheral nerve stimulation may offer targeted relief by modulating specific peripheral nerves rather than the spinal cord itself.
These technologies require patient selection, trialing when appropriate, and careful follow-up. They're not first-line treatments, but they are important tools for the right patient.
Kyphoplasty for compression fractures
A vertebral compression fracture is different from ordinary mechanical back pain. The pain often starts suddenly, often in older adults or after a strain that shouldn't have caused severe pain.
Kyphoplasty is a minimally invasive procedure used in selected patients with compression fractures. It can help stabilize the fractured vertebra and reduce severe pain that doesn't respond well to bracing and time alone.
Regenerative options such as PRP
Some patients ask about platelet-rich plasma, or PRP, particularly for degenerative spine-related pain patterns. Regenerative treatments are part of the broader opioid-sparing conversation and may be considered in carefully selected cases.
The important point is that regenerative care should be diagnosis-driven, not trend-driven. It's not a substitute for a proper exam, and it is not the answer for every form of back pain.
What interventional care does better than repeated medication use
Long-term opioid reliance often creates a poor trade. Patients may get partial symptom blunting without better function, while side effects, tolerance, and dependence risk continue to rise.
Interventional pain management aims for a more useful outcome:
- Identify the pain generator
- Target it precisely
- Create function, not just temporary sedation
- Support rehab and activity
- Reserve surgery for cases that require it
For readers who want to understand the full range of diagnostic and treatment options, including injections, nerve procedures, and minimally invasive spine interventions, this overview of interventional procedures used for spine and pain treatment is a good starting point.
Partnering for Your Recovery in Chicago Ridge and Beyond
A vast majority of individuals do not require a lecture about back pain. They require a plan that fits the stage they're in.
If your pain is new and clearly mechanical, basic self-care and smart movement may be enough. If your back keeps flaring, your leg symptoms are growing, or your walking and sleep are getting worse, the answer usually isn't more random stretching. It's a proper evaluation, a diagnosis that makes sense, and treatment that matches the anatomy involved.
That matters not just for comfort, but for cost and function over time. U.S. spending on spine pain rose from $87.6 billion in 2013 to $134.5 billion in 2016, and patients with back pain incur 2.5 times higher healthcare costs, according to this NCBI review on spinal stenosis and chronic back pain management. When care is delayed, fragmented, or overly dependent on medication, patients often pay more in every sense. More appointments, more missed work, more limitations, and more frustration.
The better model is coordinated and opioid-sparing. That means looking carefully at whether the problem is disc pain, facet pain, sacroiliac dysfunction, spinal stenosis, nerve irritation, fracture, or a combination. It means using rehabilitation when it's the right first step, adding image-guided procedures when they're indicated, and keeping the focus on restored function.
For patients in Chicago Ridge, Oak Lawn, Palos Hills, Palos Heights, Worth, Bridgeview, Hickory Hills, Alsip, Burbank, Evergreen Park, and Orland Park, specialized pain care should feel clear, not intimidating. You should know why a treatment is being recommended, what problem it aims to solve, and what the actual trade-offs are.
Workers' compensation and personal injury cases add another layer. Those patients often need timely diagnosis, coordinated records, functional improvement, and a treatment plan that helps them move forward rather than stay stuck in a loop of imaging, medication changes, and delayed referrals. The same principle applies. Target the cause. Protect function. Avoid unnecessary opioid dependence.
If you've been trying to fix back pain on your own and the pattern keeps repeating, that's useful information. It means your next step should be more precise, not just more effort.
If you're ready for a diagnosis-driven, opioid-sparing plan for persistent back pain, Midwest Pain & Wellness serves patients in Chicago Ridge and the surrounding Illinois communities with extensive interventional pain care. The clinic evaluates chronic back and leg pain, spinal stenosis, injury-related pain, post-surgical pain, and work-related cases, then builds personalized treatment plans that may include rehabilitation, image-guided injections, radiofrequency ablation, neuromodulation, or minimally invasive spine procedures.



