Understanding the Real Results Behind PRP Treatment
How effective is PRP? The answer depends largely on what condition you’re treating. Research shows that platelet-rich plasma (PRP) has strong evidence supporting its use for knee osteoarthritis, tennis elbow (lateral epicondylitis), and male pattern baldness. However, results for other conditions like Achilles tendinitis and ankle osteoarthritis remain less compelling. Here’s what the evidence tells us:
PRP Effectiveness by Condition:
- Most Effective: Knee osteoarthritis, lateral epicondylitis (tennis elbow), plantar fasciitis, carpal tunnel syndrome
- Moderately Effective: Hair loss (androgenetic alopecia), rotator cuff tendinopathy, hip osteoarthritis
- Less Effective: Achilles tendinitis, ankle osteoarthritis, acute muscle injuries
- Typical Timeline: Initial results in 2-4 weeks; full effects in 3-6 months
- Duration of Relief: 6-18 months, depending on the condition
- Cost Range: $250-$1,500 per session; usually not covered by insurance
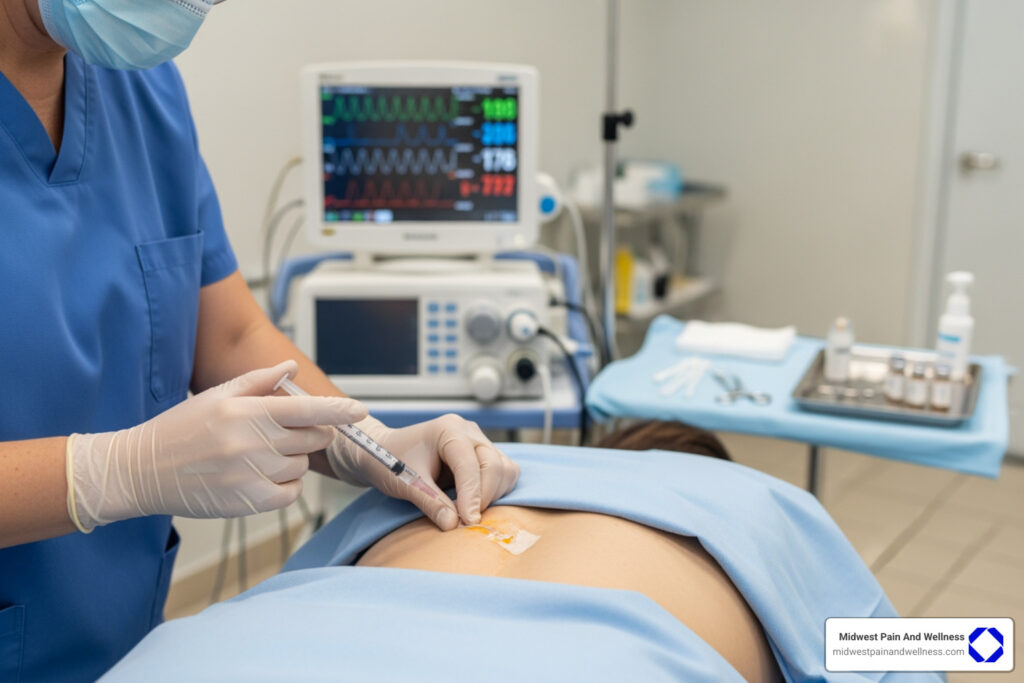
PRP isn’t a miracle cure, but it’s not just hype either. The treatment uses your own blood—specifically, concentrated platelets containing growth factors—to potentially stimulate healing in damaged tissues. Doctors inject this concentrated solution into injured areas, triggering your body’s natural repair mechanisms.
The challenge? Results vary significantly between patients, and medical organizations worldwide still debate the strength of evidence for many applications. Some people experience substantial pain relief and improved function. Others see little to no benefit. And researchers still can’t reliably predict who will respond best to treatment.
What makes PRP particularly appealing is its safety profile. Because it uses your own blood cells, the risk of allergic reactions is minimal. Side effects typically include temporary pain, swelling, and bruising at the injection site—far less concerning than long-term steroid use or surgical complications.
As Dr. Yaw Donkoh, a double board-certified physician specializing in interventional pain management and regenerative medicine, I’ve seen how patients often ask “how effective is PRP?” after hearing about it from athletes or celebrities. My approach focuses on matching treatment to evidence—using PRP where research supports it and being transparent about its limitations where the science remains unclear.
The Science of Healing: What is PRP and How Does It Work?
Platelet-rich plasma, or PRP, is a cutting-edge treatment that harnesses your body’s natural healing abilities. At its core, PRP is a concentrated solution derived from your own blood, specifically designed to accelerate healing and regeneration in damaged tissues. But what exactly is it, and how does this remarkable process unfold?
What is Platelet-Rich Plasma (PRP)?
PRP consists of two primary components: plasma, the liquid portion of your blood, and platelets, a type of blood cell primarily known for its role in clotting. However, platelets are far more than just clotting agents. They contain a rich supply of proteins called growth factors—bioactive molecules that play a critical role in tissue repair, cell reproduction, and regeneration. When concentrated, these growth factors can be delivered directly to an injured or degenerating area, kickstarting your body’s healing cascade.
How is PRP Prepared?
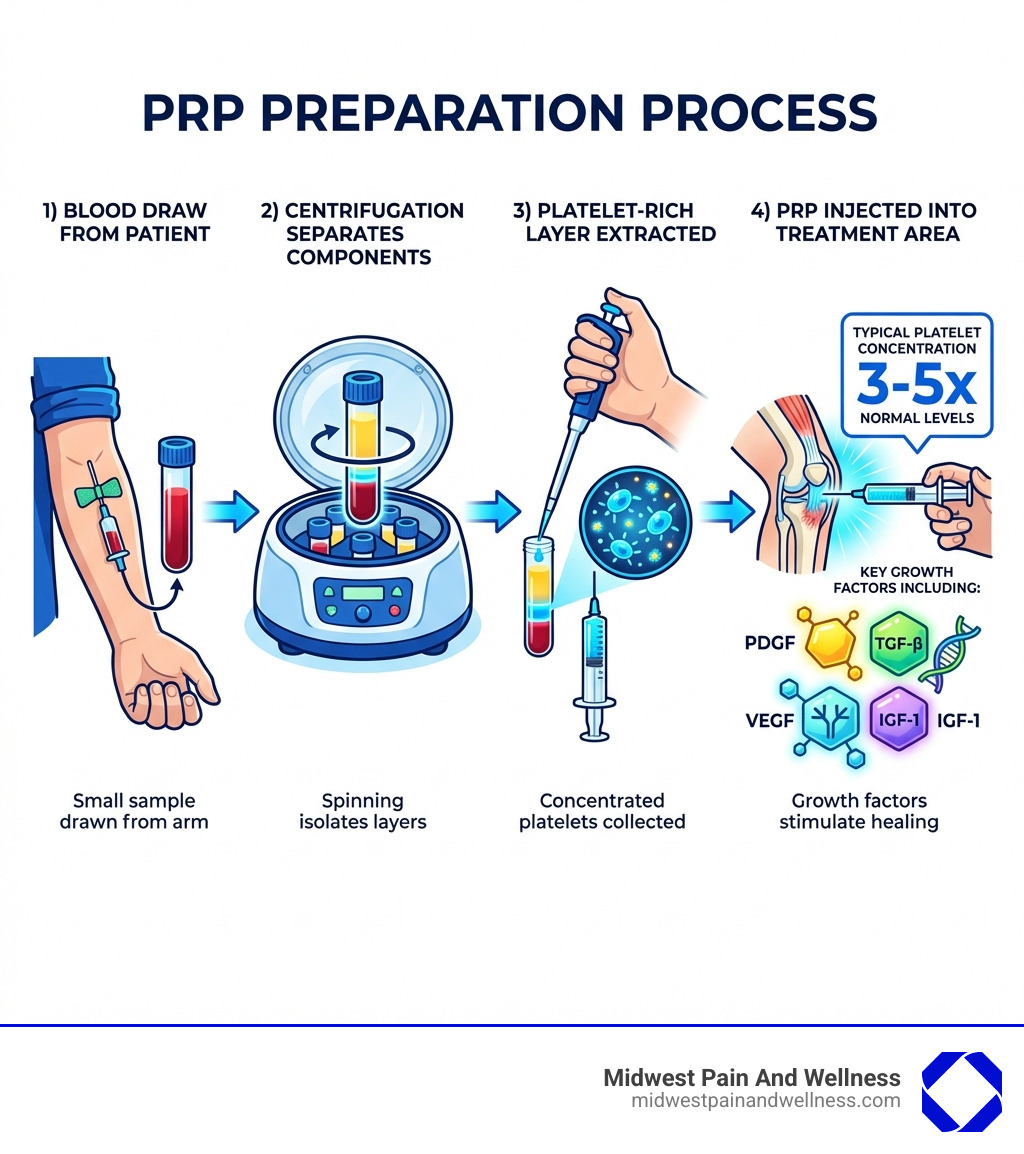
The preparation of PRP is a precise, three-step process that typically takes about 30 minutes in our Chicago Ridge clinic:
- Blood Draw: First, a small amount of your blood, usually about 2 to 4 tablespoons, is drawn from your arm, similar to a routine blood test.
- Centrifugation: This blood sample is then placed into a specialized device called a centrifuge. This machine spins the blood at high speeds, causing its components to separate based on their density. The red blood cells, white blood cells, and plasma layers become distinct.
- Platelet Concentration: The concentrated layer of plasma, now rich in platelets (and thus growth factors), is extracted. This “platelet-rich plasma” typically contains a 3 to 5 times higher concentration of platelets than normal blood. This concentrated solution is then ready for injection.
This autologous nature of PRP—meaning it comes from your own body—is a key advantage, significantly reducing the risk of allergic reactions or disease transmission.
The Proposed Mechanisms of Action
Once injected into the target area, the concentrated platelets release their powerful cargo of growth factors. These include:
- Platelet-Derived Growth Factor (PDGF): Promotes cell growth and blood vessel formation.
- Changing Growth Factor-beta (TGF-β): Stimulates cell proliferation, differentiation, and extracellular matrix production.
- Vascular Endothelial Growth Factor (VEGF): Crucial for forming new blood vessels (angiogenesis).
- Epidermal Growth Factor (EGF): Encourages cell growth and wound healing.
- Insulin-like Growth Factor-1 (IGF-1): Supports cell growth, survival, and tissue repair.
These bioactive proteins trigger a cascade of biological events, including:
- Inflammation Modulation: While initially creating a controlled inflammatory response (similar to what happens after an injury), PRP’s growth factors can also help modulate chronic inflammation, which is often a significant contributor to pain and tissue degeneration.
- Cell Proliferation and Differentiation: They stimulate the multiplication of local cells (like fibroblasts, chondrocytes, and osteoblasts) and guide them to differentiate into specific tissue types needed for repair.
- Extracellular Matrix Synthesis: PRP promotes the production of collagen and other components that form the structural scaffolding of tissues, essential for strength and integrity.
- Angiogenesis: The formation of new blood vessels improves blood supply to the injured area, delivering vital oxygen and nutrients necessary for healing.
By enhancing these natural processes, PRP aims not just to alleviate symptoms but to promote genuine tissue repair and regeneration.
While the equipment used to produce PRP and the injections themselves have been cleared by the FDA, the procedure is still considered investigational and has not been officially approved by the FDA for most uses. This distinction means that while the components are safe, the specific applications for various conditions are still undergoing rigorous study.
For a deeper dive into the fundamental science, you can explore scientific research on PRP biology and classification.
How Effective is PRP for Osteoarthritis and Joint Pain?
Osteoarthritis (OA) is a common, debilitating condition affecting millions, causing pain, stiffness, and reduced mobility as cartilage wears down. For our patients in Chicago Ridge struggling with joint pain, particularly in the knees, hips, and shoulders, the question of how effective is PRP is highly relevant. The research on PRP for OA is extensive and, while sometimes varied, often points to promising results, especially when compared to traditional treatments.
Knee Osteoarthritis
The knee is perhaps the most studied joint for PRP therapy in OA. We’ve seen a growing body of evidence, including Level I research, supporting PRP’s effectiveness.
- Pain and Function Improvement: Studies indicate that PRP injections are an effective treatment for improving pain, stiffness, and function in patients with mild-to-moderate knee OA. A meta-analysis of 30 randomized controlled trials (RCTs) found that PRP had the best overall outcome at 12 months compared to corticosteroids, hyaluronic acid (HA), and placebo.
- Duration of Effect: Unlike some treatments that offer only short-term relief, PRP has shown improvement in knee OA symptoms for up to five years in some cases. This longer-lasting effect is a significant advantage for patients seeking sustained relief.
- Inflammation Reduction: PRP injections help treat OA pain and stiffness by modulating the joint environment and reducing inflammation. This is crucial because chronic inflammation contributes significantly to cartilage degradation.
- Multiple Injections: Research suggests that multiple PRP injections can be more effective than single injections and hyaluronic acid for early-stage knee OA.
- Intra-osseous Injections: For more severe knee OA, a combination of intra-articular (into the joint) and intra-osseous (into the bone) PRP injections is being explored, with pilot studies showing promising results by targeting the subchondral bone structures.
It’s important to acknowledge that some larger studies, including those published in JAMA in 2021, have raised questions about PRP’s efficacy for knee OA when compared to placebo. However, the overall trend in recent Level 1 evidence reviews, like the one by Pretorius et al. (2023), still points to strong support for its use, highlighting the evolving nature of medical research and the importance of specific PRP formulations and patient selection.
Scientific research on PRP for knee symptomatic management further explores the comparison between PRP and corticosteroid injections for symptomatic management of knee OA.
Hip Osteoarthritis
While research for hip OA is not as extensive as for the knee, initial findings are encouraging. Intra-articular PRP injections for hip OA have been shown to be safe and to offer some efficacy in pain reduction and improved function. However, the data is still considered limited, and some studies suggest that any advantage PRP might have over hyaluronic acid may diminish over time.
Shoulder Osteoarthritis
For shoulder OA, specifically glenohumeral OA, PRP has also been shown to be an effective treatment in improving both pain and function. PRP injections are broadly indicated for a wide variety of shoulder-related soft-tissue and bony conditions, including subacromial impingement syndrome, where PRP has demonstrated superiority over corticosteroids and physiotherapy at eight weeks.
Comparing PRP, Corticosteroids, and Hyaluronic Acid for Joint Pain
When considering treatment options for joint pain, it’s helpful to understand how PRP stacks up against other common injectables.
| Feature | Platelet-Rich Plasma (PRP) ## The Science of Healing: What is PRP and How Does It Work?
At Midwest Pain and Wellness, we believe in treatments that address the root cause of your pain, not just its symptoms. Platelet-Rich Plasma (PRP) therapy is one such regenerative approach that harnesses your body’s innate capacity for healing. But what exactly is PRP, and how does this sophisticated process work to help you achieve lasting relief?
What Exactly is Platelet-Rich Plasma (PRP)?
In simple terms, PRP is your blood, but better! It’s a concentrated preparation of platelets and plasma derived from your own blood. While platelets are commonly known for their role in clotting, they are also a powerhouse of essential proteins called growth factors. These growth factors are crucial biological messengers that orchestrate the complex processes of wound healing and tissue regeneration.
Our blood normally contains about 150,000 to 350,000 platelets per microliter. In PRP, this concentration can be amplified to over 1,000,000 platelets per microliter, delivering a potent dose of healing potential directly to the site of injury or degeneration.
How Do We Prepare Your PRP?
The preparation of PRP is a straightforward, in-office procedure that adheres to strict safety protocols. The entire process, from blood draw to injection, typically takes around 30 minutes to an hour.
- A Small Blood Sample: First, a small quantity of your blood—usually 2 to 4 tablespoons—is gently drawn from your arm, much like a routine blood test. This is a quick and minimally invasive step.
- Specialized Centrifugation: Your blood sample is then placed into a specialized medical device called a centrifuge. This device spins the blood at a high speed, causing its various components (red blood cells, white blood cells, plasma, and platelets) to separate into distinct layers based on their density.
- Concentration and Extraction: The magic happens here! After centrifugation, the layer rich in concentrated platelets and plasma is carefully extracted. This concentrated solution is your personalized platelet-rich plasma, ready for therapeutic use.
This method ensures that the PRP we use is autologous, meaning it comes directly from your own body. This significantly minimizes the risk of allergic reactions or communicable diseases, making it a very safe option for our patients.
The Mechanism of Action: How PRP Stimulates Healing
Once prepared, this concentrated PRP is precisely injected into the targeted area—whether it’s an arthritic joint, a damaged tendon, or even the scalp to stimulate hair follicles. The real work begins when these highly concentrated platelets become activated and release their potent array of growth factors.
These growth factors are like the conductors of an orchestra, signaling cells to begin the repair process. Key growth factors include:
- Platelet-Derived Growth Factor (PDGF): A primary stimulator of cell division and new blood vessel formation.
- Changing Growth Factor-beta (TGF-β): Promotes tissue repair and collagen production, essential for structural integrity.
- Vascular Endothelial Growth Factor (VEGF): Crucial for forming new blood vessels, which improves nutrient and oxygen supply to healing tissues.
- Epidermal Growth Factor (EGF): Stimulates cell growth and wound healing processes.
- Insulin-like Growth Factor-1 (IGF-1): Supports cellular growth, survival, and overall tissue repair.
These powerful molecules work synergistically to:
- Reduce Inflammation: By modulating the inflammatory environment, PRP helps calm chronic pain and creates a more conducive setting for healing.
- Stimulate Cell Proliferation: They encourage the multiplication of local cells, such as fibroblasts (which produce collagen), chondrocytes (cartilage cells), and osteoblasts (bone-forming cells), to rebuild damaged tissue.
- Improve Tissue Regeneration: PRP promotes the synthesis of new extracellular matrix components, which are the building blocks of healthy tissue, and can encourage the regeneration of damaged cartilage, tendons, and ligaments.
- Improve Blood Supply: Through angiogenesis (new blood vessel formation), PRP ensures that the healing tissues receive an optimal supply of oxygen and nutrients.
Essentially, we’re giving your body a highly concentrated dose of its own natural repair tools, directing them precisely where they’re needed most. This approach aims to not just mask pain, but to facilitate genuine, long-term healing.
It’s worth noting that the FDA classifies PRP as a medical device. This means that while the equipment and the procedure itself are cleared for use, the specific clinical applications for various conditions are still considered investigational and not fully “approved” in the same way a new drug would be. This distinction is important for understanding research and insurance coverage. For a deeper dive into the fundamental science, you can explore scientific research on PRP biology and classification.
How Effective is PRP for Osteoarthritis and Joint Pain?
For many in Chicago Ridge suffering from the persistent aches of osteoarthritis (OA) and other forms of joint pain, PRP therapy offers a guide of hope. The question, how effective is PRP for these conditions, is one we encounter daily. While the journey of scientific findy is ongoing, the evidence for PRP in joint pain, especially knee OA, is becoming increasingly robust.
Knee Osteoarthritis (OA)
Knee OA is a degenerative condition that affects millions, causing pain, stiffness, and reduced mobility. Conventional treatments often focus on symptom management. PRP, however, aims to promote healing and slow progression.
- Strong Evidence for Pain and Function: Level I research, the highest quality of evidence, strongly supports PRP’s effectiveness in managing knee OA. Multiple studies and meta-analyses, including one that synthesized 30 RCTs, have concluded that PRP provides superior outcomes for pain relief and functional improvement at 12 months compared to corticosteroids, hyaluronic acid (HA), and even placebo.
- Long-Lasting Relief: A significant advantage of PRP is the duration of its effects. Patients often experience sustained improvement in knee OA symptoms, potentially lasting from six months to a year or even longer, with some studies reporting benefits for up to five years. This contrasts with the often temporary relief offered by other injectables.
- Targeting the Joint Environment: PRP works by modulating the joint environment, reducing the chronic inflammation that often drives cartilage breakdown. It can also stimulate the repair of damaged tissues within the joint.
- Multiple Injections and Intra-osseous Approaches: For optimal results, particularly in early OA, a series of multiple PRP injections may be more effective than a single shot. Furthermore, innovative approaches like combining intra-articular (into the joint) with intra-osseous (into the bone) PRP injections are showing promise for severe OA by addressing the underlying bony structures contributing to the condition.
While some studies, particularly older ones or those with different PRP formulations, have presented mixed results, the consensus from recent high-quality research is increasingly positive. We encourage our patients to explore scientific research on PRP for knee symptomatic management to understand these comparisons better.
Hip Osteoarthritis (OA)
Hip OA can be particularly debilitating, impacting daily activities. While the evidence base for hip OA isn’t as vast as for knee OA, the data is encouraging. Intra-articular PRP injections have been found to be safe and effective in reducing pain and improving function for hip OA. Although some studies suggest that PRP’s advantage over hyaluronic acid may lessen over time, it remains a viable option for many seeking relief.
Shoulder Pain and Osteoarthritis
The shoulder, a complex joint prone to both OA and various soft-tissue injuries, also responds well to PRP. PRP has been shown to be an effective treatment for improving pain and function in glenohumeral (shoulder) OA. For conditions like subacromial impingement syndrome, PRP injections have demonstrated superiority over corticosteroids and physiotherapy in improving symptoms in the short to mid-term. This broad applicability makes PRP a valuable tool in addressing a wide array of shoulder-related pain.
Comparing PRP, Corticosteroids, and Hyaluronic Acid for Joint Pain
At Midwest Pain and Wellness, we offer a range of interventional pain management options. Understanding how PRP compares to other common joint injections can help you make an informed decision:
| Feature | Platelet-Rich Plasma (PRP) | Feature | Platelet-Rich Plasma (PRP) | Feature | Platelet-Rich Plasma (PRP)