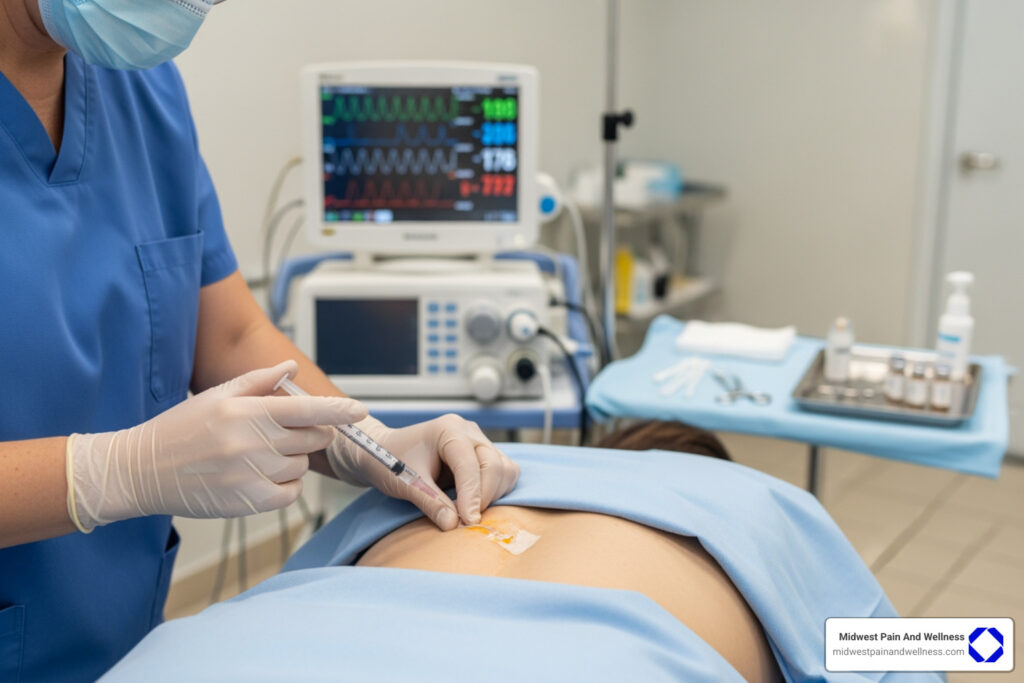
The Reality of Living with Chronic Back Pain
Chronic back pain is defined as back pain lasting more than three months. If you’re experiencing persistent discomfort that won’t go away, you need to know:
- What it is: Pain in the lower back lasting longer than 12 weeks, even after initial treatment
- How common it is: Up to 23% of adults worldwide suffer from chronic low back pain
- Why it matters: It’s the leading cause of disability globally, affecting work, relationships, and daily activities
- What causes it: 90% of cases are “mechanical” (muscle strain, disc problems, arthritis) rather than serious disease
- Key fact: Most chronic back pain can be managed effectively without surgery or opioids
Back pain is one of the most common reasons people seek medical help or miss work. In 2020 alone, approximately 619 million people experienced low back pain—that’s roughly 1 in 13 people worldwide. This number is expected to rise to 843 million by 2050.
The good news? While chronic back pain can be frustrating and life-altering, it’s rarely caused by a serious medical condition. Most cases respond well to a combination of evidence-based treatments that don’t involve surgery or long-term pain medication.
This guide will help you understand what’s causing your pain, what treatments actually work (and which ones to avoid), and how to partner with healthcare providers to find lasting relief. You’ll learn about the latest recommendations from the World Health Organization and other leading health authorities, all translated into practical steps you can take today.
Whether your pain started after an injury, developed gradually over time, or appeared without any clear cause, understanding your condition is the first step toward taking control of your life again.

Understanding Chronic Back Pain: Causes, Risks, and Impact
Living with persistent back pain can feel like a complex puzzle. Understanding its origins, risk factors, and how it affects your life is the first step toward finding relief. For most people, chronic back pain isn’t a sign of a serious underlying disease, but rather a combination of mechanical and lifestyle factors.
What Causes Persistent Back Pain?
About 90% of cases are considered “mechanical,” meaning the pain originates in the spine’s structures. Common causes include:
- Muscle or Ligament Strain: Overstretching or tearing the muscles and ligaments that support the spine, often from improper lifting or sudden movements.
- Degenerative Disc Disease (DDD): The natural wear and tear of the spinal discs, which act as shock absorbers. Over time, they can thin and lose cushioning, leading to pain.
- Herniated or Bulging Discs: When the soft center of a spinal disc pushes through its tougher exterior, it can press on nearby nerves, causing pain, numbness, or weakness, sometimes radiating down the leg (sciatica).
- Spinal Stenosis: The narrowing of the spinal canal, which can put pressure on the spinal cord and nerves.
- Osteoarthritis: This “wear-and-tear” arthritis can affect the small facet joints in your spine, causing pain and stiffness.
- Osteoporosis: This condition causes bones to become weak and brittle, making them susceptible to painful fractures in the vertebrae.
- Myofascial Pain Syndrome: A chronic pain disorder where pressure on sensitive points in your muscles (trigger points) causes pain in seemingly unrelated parts of your body.
Often, it’s a combination of these factors, and a specific cause isn’t always identifiable. However, not having a precise diagnosis doesn’t make your pain any less real or treatable.
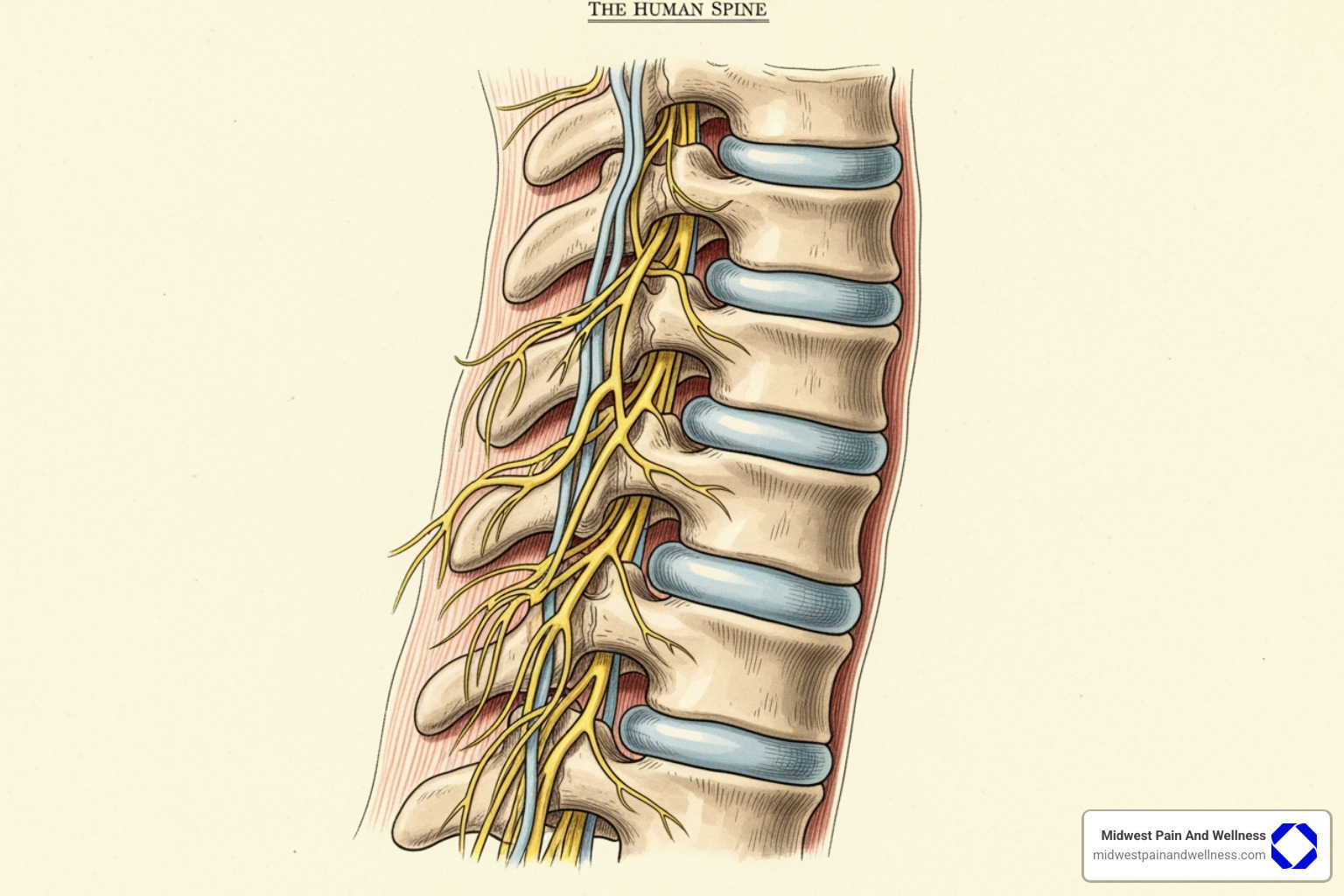
Are You at Risk? Key Factors to Consider
While anyone can develop chronic back pain, certain factors increase your risk:
- Age: It’s most common to first experience back pain between ages 30 and 50.
- Lack of Exercise: Weak back and abdominal muscles can’t properly support the spine.
- Excess Weight: Extra body weight puts added stress on your back.
- Smoking: It can reduce blood flow to the spine and contribute to osteoporosis.
- Occupation: Jobs that require heavy lifting, repetitive movements, or prolonged sitting can strain the back.
- Improper Lifting: Using your back instead of your legs to lift heavy objects is a common cause of injury.
- Psychological Factors: Stress, anxiety, and depression can amplify pain perception and make recovery more difficult.
You might have heard many things about back pain that simply aren’t true. For instance, some people believe complete bed rest is always best, or that a special mattress will magically fix everything. We encourage you to get the real facts and debunk common misconceptions by exploring [Debunking 8 common myths about back pain](https://newsnetwork.mayoclinic.org/?p=403643).
The Broader Impact on Your Life
Chronic back pain is more than just a physical ailment; it’s the leading cause of disability worldwide. It can profoundly affect your quality of life, leading to:
- Daily Function: Difficulty with simple activities like walking, sitting, sleeping, or playing with children.
- Mental Health: Increased rates of anxiety, depression, and stress due to constant discomfort and frustration.
- Work and Finances: It’s a top reason for missed work days, leading to lost income and potential job loss. The cost of treatments can also create a significant financial strain.
- Social Life: Pain can make it hard to participate in hobbies and social events, leading to isolation.
- Long-Term Complications: If left unmanaged, inactivity can lead to muscle weakness, weight gain, and a cycle of worsening pain and disability.
Recognizing this wide-ranging impact is the first step toward seeking comprehensive care that addresses you as a whole person, not just a symptom.
Finding Relief: A Guide to Non-Surgical Treatments
Here’s something that might surprise you: most people with chronic back pain can find real, lasting relief without ever going under the knife. At Midwest Pain And Wellness, we’ve built our entire practice around this truth. We focus on modern, evidence-based strategies that help you reclaim your life through treatments that work with your body, not against it.
The key is taking a comprehensive approach—one that addresses not just your physical symptoms, but your whole well-being. Let’s explore the treatments that can make a real difference.
The Foundation: Physical and Lifestyle-Based Therapies
Think of these therapies as your first line of defense—and often, your most powerful tool. They put you in the driver’s seat of your own recovery.
- Physical Therapy & Exercise: A physical therapist can design a program to strengthen your core, improve flexibility, and teach you better body mechanics. This is far more effective than guessing on your own. Continuing with low-impact aerobic activities like walking or swimming is crucial for building endurance and releasing natural pain-relieving endorphins.
- Lifestyle Modifications: Learning to pace yourself is key. Listen to your body and take breaks. Small, consistent changes, like a daily walk or stretching, can have a big impact.
- Weight Management: Every extra pound adds stress to your spine. A healthy diet also supports bone health and can reduce inflammation.
- Ergonomics: How you sit, stand, and lift matters. Sit with your back supported, stand tall, and always lift with your legs, not your back. Keep objects close to your body and avoid twisting while lifting.

Mind-Body and Complementary Approaches
Your brain and your back are in constant conversation. Addressing the psychological side of pain is essential for recovery.
- Cognitive Behavioral Therapy (CBT): Helps you change negative thought patterns about your pain and develop effective coping strategies.
- Mindfulness and Meditation: Teaches you to observe pain without judgment, which can reduce its intensity and the distress it causes.
- Acupuncture: This ancient technique is now recommended in modern guidelines for chronic back pain relief.
- Massage, Yoga, and Tai Chi: These practices help relax tense muscles, improve flexibility and balance, and reduce stress. Gentle forms of yoga and the slow, flowing movements of Tai Chi are particularly effective. Scientific research on Tai Chi for low back pain has shown it can improve pain and function.
Medications and Interventional Procedures
When other therapies aren’t enough, medications and interventional procedures can provide the relief needed to get you moving again. At Midwest Pain And Wellness, we specialize in these approaches as part of a comprehensive, opioid-free strategy.
- Medications: Non-steroidal anti-inflammatory drugs (NSAIDs) are a common first step. In some cases, certain antidepressants or short-term muscle relaxants may be prescribed to manage pain and spasms.
- Injection-Based Treatments: These procedures deliver powerful medication directly to the source of the pain. Epidural steroid injections can reduce nerve inflammation, while nerve blocks can help diagnose and treat pain from specific joints.
- Radiofrequency Ablation: For longer-lasting relief, this procedure uses heat to interrupt pain signals from specific nerves, often providing relief for several months or more.
At Midwest Pain And Wellness, our double board-certified doctors use a multi-modal, interventional approach. We collaborate with physical therapists, psychologists, and other practitioners to create custom care plans designed specifically for you. Our goal isn’t just to reduce your pain—it’s to help you restore function and get back to the life you want to live.
What to Do vs. What to Avoid: Evidence-Informed Guidelines
When you’re living with chronic back pain, it’s natural to want to try everything that might help. But not all treatments are created equal. The World Health Organization (WHO) and other leading health authorities have developed guidelines to help you focus on what works and avoid what doesn’t.
Recommended Interventions for Chronic Back Pain
Evidence-based guidelines prioritize active, patient-centered care. Effective treatments include:
- Patient Education: Understanding your condition and learning self-management skills is the foundation of recovery.
- Structured Exercise Programs: This is one of the most powerful tools. It includes physical therapy, core strengthening, flexibility work, and low-impact aerobic activities like walking or swimming.
- Manual & Mind-Body Therapies: Spinal manipulative therapy, massage, and Cognitive Behavioral Therapy (CBT) are all proven to help manage pain and improve function.
- Medications (when appropriate): Non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen can be useful for managing flare-ups as part of a broader treatment plan.
Interventions NOT Recommended for Chronic Back Pain
Just as important as knowing what to do is knowing what to avoid. The following are generally not recommended for the routine management of chronic back pain because they lack strong evidence or may even be harmful:
- Prolonged Bed Rest: More than a day or two of rest can lead to muscle weakness and deconditioning, making pain worse in the long run. Movement is medicine.
- Lumbar Braces or Belts: Routine use can weaken the core muscles that are essential for supporting your spine.
- Traction: Studies have not shown this to be an effective long-term treatment for chronic back pain.
- Routine Use of Opioid Pain Killers: The significant risks of dependence and side effects often outweigh the limited benefits for chronic, non-cancer back pain. This is why our approach at Midwest Pain And Wellness is opioid-free.
Understanding Chronic Back Pain: Causes, Risks, and Impact
Living with persistent back pain is common and usually stems from mechanical issues in and around the spine rather than serious disease. For many in Chicago Ridge and beyond, understanding the basics is the first step to relief.
What Causes Persistent Back Pain?
About 90% of cases are mechanical. Common contributors include:
- Muscle or Ligament Strain
- Degenerative Disc Disease (DDD)
- Herniated or Bulging Discs (sometimes causing sciatica)
- Spinal Stenosis
- Osteoarthritis (facet joint pain and stiffness)
- Osteoporosis (vertebral fractures)
- Myofascial Pain Syndrome (trigger points)
Often, several factors overlap—and even when an exact cause isn’t found, pain is real and treatable.
Are You at Risk? Key Factors to Consider
- Age 30–50+
- Low activity/weak core
- Excess weight
- Smoking
- Occupational strain (heavy lifting, twisting, or prolonged sitting/standing)
- Improper lifting techniques
- Stress, anxiety, depression (can amplify pain)
Get facts and avoid common misconceptions: Debunking 8 common myths about back pain.
The Broader Impact on Your Life
Chronic back pain can limit daily function, affect mood, reduce work capacity, strain finances, and disrupt relationships. If unaddressed, inactivity can fuel a cycle of weakness and worsening pain. A comprehensive, evidence-based plan can break that cycle and restore function.
Finding Relief: A Guide to Non-Surgical Treatments
Most people find lasting improvement without surgery. At Midwest Pain And Wellness, we focus on evidence-based, opioid-free care to help you return to the activities you value.
The Foundation: Physical and Lifestyle-Based Therapies
- Physical Therapy & Structured Exercise: Targeted core strengthening, flexibility work, and low-impact cardio (walking, swimming, cycling) outperform “going it alone.”
- Lifestyle & Pacing: Build activity gradually; take brief, planned breaks.
- Diet & Weight Management: Reducing excess weight eases spinal load; aim for balanced nutrition that supports bone and overall health.
- Ergonomics: Stand tall, sit with lumbar support, and lift with your legs—keep objects close and avoid twisting.
Mind-Body and Complementary Approaches
- CBT: Builds coping skills and reduces pain-related distress.
- Mindfulness/Meditation: Lowers pain intensity and stress.
- Acupuncture, Massage, Yoga, Tai Chi: Helpful additions; Scientific research on Tai Chi for low back pain supports benefits for pain and function.
Medications and Interventional Procedures
- NSAIDs (as appropriate); sometimes low-dose antidepressants for pain or short courses of muscle relaxants.
- Image-guided injections: Epidural steroid injections and targeted nerve blocks to calm inflammation and clarify pain sources.
- Radiofrequency Ablation: Interrupts specific pain signals for longer relief when appropriate.
Our double board-certified physicians coordinate multi-modal plans custom to you—prioritizing function, safety, and long-term results.
What to Do vs. What to Avoid: Evidence-Informed Guidelines
Global guidelines emphasize active, patient-centered care. Focus on what works—and skip what doesn’t.
Recommended Interventions for Chronic Back Pain
- Patient education and self-management (understand your condition; stay active)
- Structured exercise programs (PT-guided core, flexibility, and low-impact aerobics)
- Spinal manipulative therapy and massage (as part of an active plan)
- Cognitive Behavioural Therapy (CBT) to improve coping and function
- NSAIDs (when appropriate) for symptom flares
Interventions NOT Recommended for Chronic Back Pain
- Prolonged bed rest (beyond 1–2 days)—leads to deconditioning
- Routine use of lumbar braces/belts—can weaken core support
- Traction—limited evidence for chronic pain relief
- Routine use of opioid pain killers—risks outweigh benefits for most chronic, non-cancer back pain
These principles guide our opioid-free, multi-modal approach at Midwest Pain And Wellness.