Your Body’s Hidden Pain Control Center
The dorsal root ganglion is a cluster of sensory nerve cell bodies located along your spinal cord. These crucial structures act as relay stations, transmitting sensory information—like pain, temperature, and touch—from your body to your brain.
Quick Facts About the Dorsal Root Ganglion:
- Location: Found in the openings between vertebrae (intervertebral foramina) along your spine.
- Structure: Contains up to 15,000 sensory neuron cell bodies per ganglion.
- Function: The first stop for sensory signals traveling from your skin, muscles, and organs to your spinal cord.
- Cell Type: Houses pseudounipolar neurons, unique cells with a single axon that splits in two.
- Pain Connection: Plays a critical role in chronic and neuropathic pain.
For those with chronic pain, the DRG is important because it’s often where pain signals originate or become amplified. When injured or inflamed, these ganglia can become hyperexcitable, firing pain signals without an actual threat. This makes the DRG a key target for advanced pain treatments.
Research shows that therapies targeting the DRG, like specialized nerve stimulation, can reduce chronic pain by an average of 70% in some patients. Unlike systemic medications, DRG-focused treatments offer targeted relief with fewer side effects.
The DRG is uniquely positioned between the peripheral and central nervous systems, making it both vulnerable to injury and accessible for treatment. It lacks the protective blood-brain barrier, leaving it exposed to inflammatory substances in the blood.
For people seeking alternatives to opioids or surgery, understanding how the DRG works opens new possibilities for managing pain at its source.
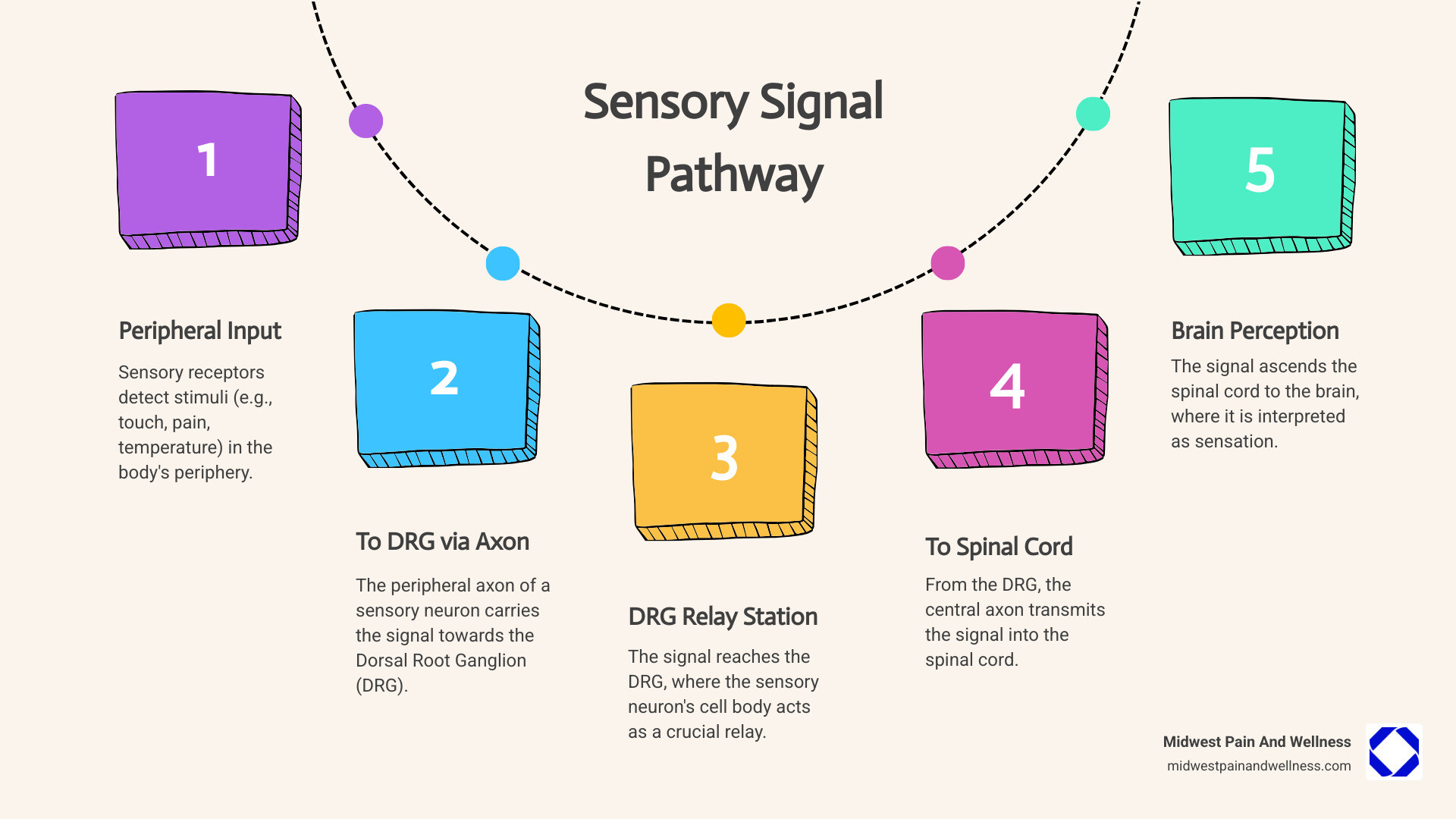
What is the Dorsal Root Ganglion (DRG) and How Does It Work?
Think of your body as a communication network. The dorsal root ganglion (DRG) is a critical relay station in this network, collecting sensory information from your body and ensuring it reaches your brain. Without these structures, you wouldn’t feel touch, temperature, or pain.
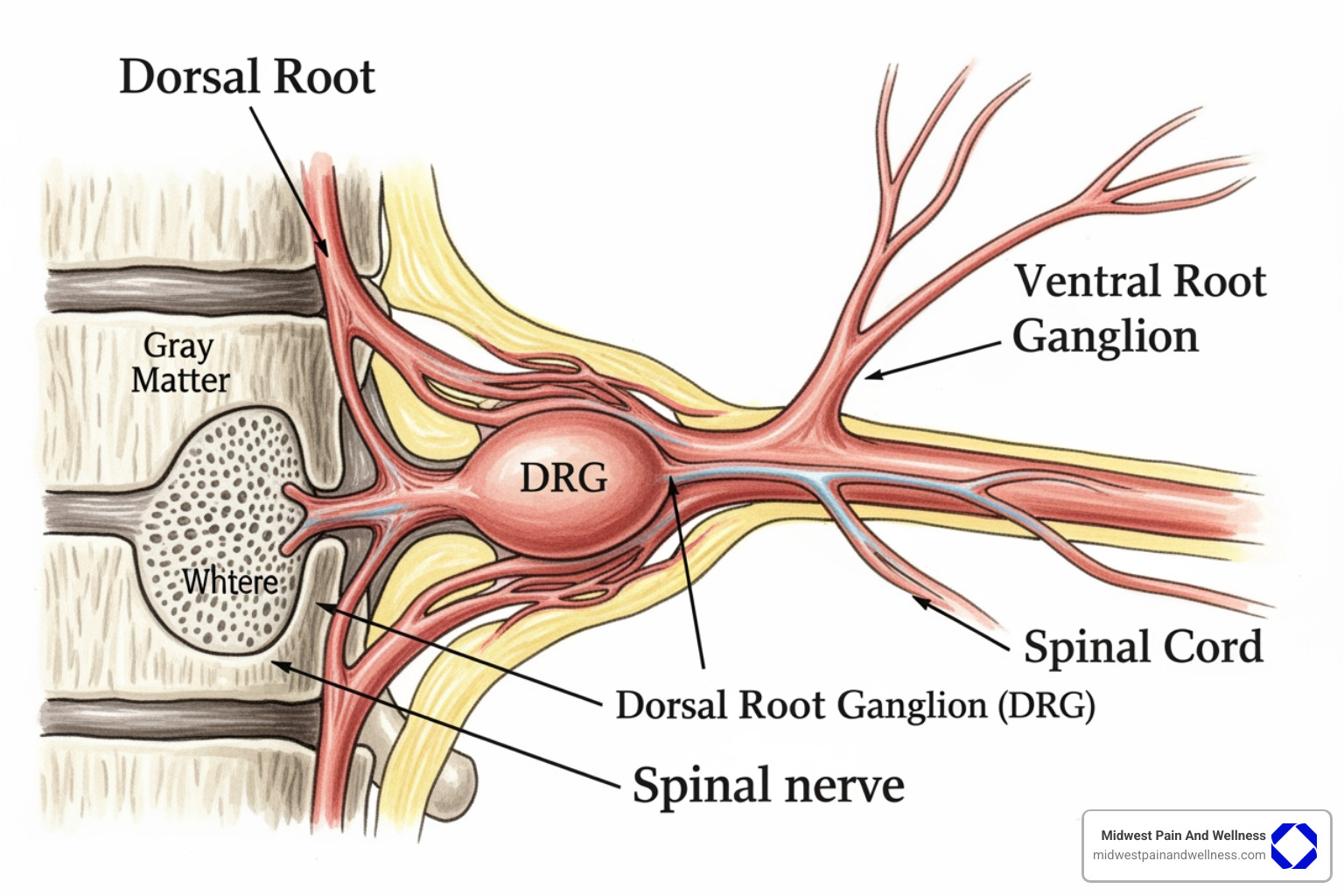
Anatomy and Location
The dorsal root ganglion is a cluster of sensory neuron cell bodies. A pair of these ganglia is found at each spinal nerve root, tucked into openings between your vertebrae called the intervertebral foramina. With 31 spinal segments, you have 31 pairs of DRGs distributed along your cervical (neck), thoracic (mid-back), lumbar (lower back), and sacral (tailbone) spine.
Each DRG can contain up to 15,000 sensory neurons, surrounded by supportive satellite glial cells that are crucial for maintaining neuron health. MRI studies show that DRG placement is highly consistent, which allows doctors to reliably target these structures for diagnosis and treatment. For more detail, scientific research on DRG neuroanatomy offers comprehensive insights.
The Primary Function of the Dorsal Root Ganglion
The dorsal root ganglion is your body’s sensory gateway. All sensations you feel pass through a DRG before reaching your brain. The neurons within the DRG detect and transmit several types of sensation:
- Touch: From a light brush to firm pressure.
- Pressure: The feeling of weight or clothing against your skin.
- Temperature: Alerts you to potentially harmful heat or cold.
- Pain: A vital protective mechanism warning of tissue damage.
- Proprioception: Your sense of body position and movement.
As the first nerve cells in the sensory pathway (“first-order neurons”), they pick up signals from receptors in your skin, muscles, and organs and relay them to the spinal cord and brain for interpretation.
Axons: The Central vs. Peripheral Pathways
DRG neurons have a unique “pseudounipolar” structure: a single short axon splits into two branches, forming a T-junction.
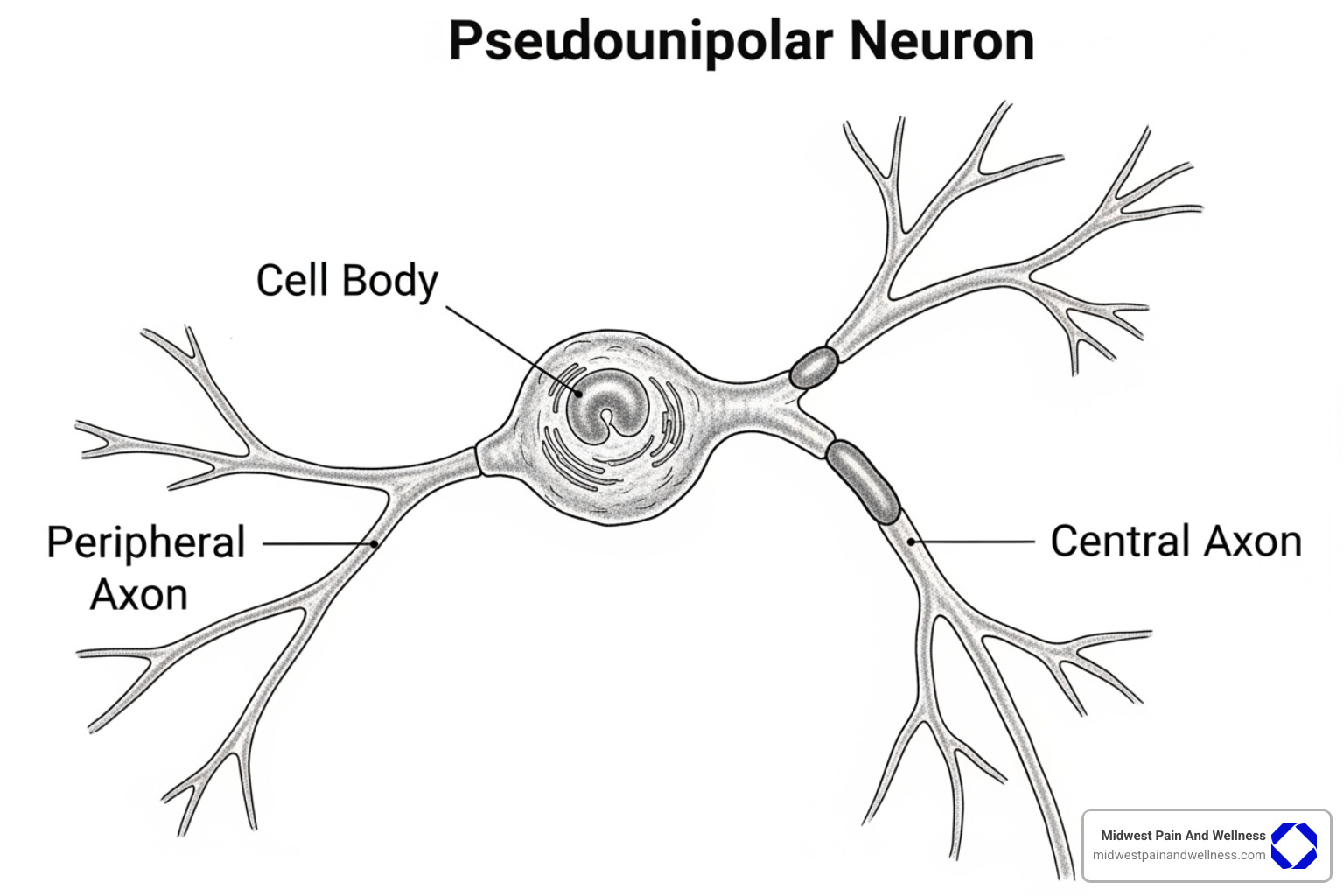
- The peripheral axon extends to your skin, muscles, and organs to gather sensory information. This branch can be very long (e.g., from your back to your toe) and has a better capacity for regeneration after injury.
- The central axon carries information from the DRG into the spinal cord, where it connects with other neurons that send the message to the brain.
When a receptor is stimulated, the signal travels along the peripheral axon, through the T-junction, and along the central axon into the spinal cord, often bypassing the cell body. This design allows for rapid signal transmission, which is crucial for quick reactions. Understanding these pathways is key to figuring out what goes wrong in chronic pain conditions and how to treat them.
The Dorsal Root Ganglion and Its Role in Chronic Pain
While the dorsal root ganglion is essential for normal sensation, it can become a source of persistent pain when things go wrong. When nerve injury or inflammation affects the DRG, it can get stuck in overdrive, like a faulty fire alarm, constantly sending pain messages to the brain.
When chronic pain develops, nerve injury and inflammation can damage DRG neurons and surrounding glial cells. This triggers a persistent immune response, and the neurons become hyperexcitable, firing with little or no stimulus. This spontaneous activity, called ectopic firing, is a primary cause of chronic neuropathic pain, as damaged DRG neurons generate their own pain signals.
This is complicated by cross-talk, where firing neurons trigger their neighbors, amplifying small pain signals into significant discomfort. Activated satellite glial cells also contribute by releasing substances that make neurons even more sensitive, worsening the pain cycle.
How the DRG Contributes to Neuropathic Pain
Neuropathic pain—often described as burning, shooting, or electric—frequently originates in the dorsal root ganglion. It’s pain caused by a malfunctioning nervous system. The spontaneous firing of DRG neurons creates pain sensations without any real threat, which the brain interprets as real pain.
At the molecular level, changes in voltage-gated sodium channels make neurons easier to trigger after nerve injury. This increased sensitivity leads to:
- Allodynia: Pain from a non-painful touch.
- Hyperalgesia: An exaggerated response to painful stimuli.
The DRG is uniquely vulnerable because it lacks a strong blood-brain barrier. Its porous blood vessels allow inflammatory substances from the bloodstream to directly access and sensitize the neurons. During inflammation, the release of substances like Substance P and CGRP creates a persistent pain cycle, turning the DRG into a “pain generator.”
Conditions Involving DRG Pathophysiology
Understanding the DRG’s role helps explain why certain conditions are so difficult to treat. These conditions often involve neuropathic pain where the DRG is a central player.
- Complex Regional Pain Syndrome (CRPS): A severe condition, often affecting a limb after a minor injury, with intense, disproportionate pain. DRG-targeted treatments have shown remarkable success for CRPS.
- Causalgia (CRPS Type 2): Similar to CRPS but occurs specifically after a traumatic nerve injury, causing persistent burning pain.
- Postherpetic neuralgia: Occurs when the shingles virus, which lies dormant in the DRG, reactivates. After the rash heals, some people experience persistent nerve pain.
- Painful diabetic peripheral neuropathy: Results from nerve damage due to high blood sugar, with the DRG being particularly susceptible. It causes pain, numbness, and tingling, often in the feet and legs.
- Phantom limb pain: Can occur after amputation because the DRG neurons that once served the limb can become hyperexcitable and generate pain signals.
- Other conditions: The DRG is also implicated in axial low back pain, discogenic pain, perineal pain, and groin pain.
At Midwest Pain And Wellness, we understand that these conditions require targeted strategies. By focusing on the DRG’s role in your pain, we address the source, offering hope for long-term, opioid-free relief. Explore our comprehensive services to learn about our individualized treatment plans.
Therapeutic Approaches Targeting the DRG
When traditional treatments fail for chronic pain involving the dorsal root ganglion, specialized therapies that target the DRG directly can make a significant difference. At Midwest Pain And Wellness, these treatments are a key part of our comprehensive, opioid-free, interventional approach. You can explore our interventional pain treatments.
Modern approaches include nerve blocks (injecting anesthetics and steroids near the DRG) and radiofrequency ablation (RFA), a minimally invasive procedure using heat to disrupt pain signals. A gentler variation, pulsed RFA, modulates nerve activity without permanent damage.
Perhaps the most exciting advancement is neurostimulation, which uses an implanted device to deliver mild electrical pulses directly to the DRG, altering pain signals before they reach the brain.
How Does Dorsal Root Ganglion Stimulation Work?
Dorsal root ganglion (DRG) stimulation is a cutting-edge therapy for hard-to-treat, localized chronic pain. Unlike traditional spinal cord stimulation (SCS), it precisely targets the specific ganglia causing pain. The system involves a small, implantable generator that sends mild electrical pulses through thin wires (leads) that are carefully placed near the target DRG.
The pulses modify pain signals, often replacing pain with a more tolerable sensation or no sensation at all. A remote control allows you to adjust the stimulation, giving you control over your pain relief.
DRG stimulation differs from traditional SCS by offering greater precision for focal pain, often providing paresthesia-free relief (no tingling), and maintaining consistent stimulation regardless of body position. Conditions that respond well include CRPS, causalgia, phantom limb pain, post-herpetic neuralgia, painful diabetic peripheral neuropathy, and focal pain in areas like the foot or groin, where traditional SCS is often less effective.
The landmark ACCURATE study confirmed that DRG stimulation is superior to conventional SCS for certain conditions, with higher success rates holding steady at one year, especially for CRPS.
Benefits and Limitations of DRG Stimulation
Dorsal root ganglion stimulation offers significant hope but has both benefits and potential challenges.
Benefits:
- Highly targeted pain relief for focal areas like the foot, knee, or groin.
- Superior outcomes for CRPS and causalgia compared to traditional SCS.
- Significant pain reduction (studies show an average of 70%), leading to less reliance on opioids.
- Paresthesia-free relief and stable stimulation that doesn’t change with posture.
- Effective for hard-to-treat conditions like phantom limb pain and post-herpetic neuralgia.
Limitations:
- It is a surgical procedure and carries risks like infection, bleeding, or nerve damage.
- Lead migration (movement of the wires) may require a repositioning procedure.
- The device’s battery will eventually need replacement through a minor surgery.
- The therapy is best for focal, localized pain, not widespread pain.
- A trial period is required to ensure effectiveness before permanent implantation.
- Individual results can vary.
At Midwest Pain And Wellness, we carefully assess if DRG stimulation is right for you, ensuring you understand the benefits and risks. Our goal is to create a custom care plan for lasting relief.
A Deeper Dive into DRG Science
The dorsal root ganglion is a sophisticated structure whose unique biology helps explain its crucial role in both normal sensation and chronic pain. Understanding these deeper aspects reveals why the DRG is such an important target for modern pain therapies.
Embryological Development
Unlike most of the nervous system, which develops from the neural tube, the DRG originates from specialized neural crest cells. Early in development, these cells migrate from the developing neural tube to form various tissues, including the sensory neurons and satellite glial cells of the DRGs. This process requires specific signals from the developing spinal cord to ensure the DRGs form correctly. This unique origin helps explain some of the DRG’s distinct characteristics and vulnerabilities.
Blood Supply and Lymphatic Drainage
The DRG’s blood supply has profound implications for health and disease. Crucially, the blood vessels within the DRG are “fenestrated” (have pores), creating a loose blood-nerve interface. This differs from the tight blood-brain barrier protecting most of the nervous system.
This high permeability is a double-edged sword: it allows easy nutrient access but also exposes the neurons to inflammatory substances and toxins from the bloodstream. This vulnerability helps explain why the DRG can become a source of chronic pain, as these substances can sensitize the neurons. While the DRG has lymphatic drainage to clear waste, the loose interface can allow inflammation to persist, contributing to chronic pain.
Key Differences Between Human and Animal DRGs
Pain research often begins with animal models, but significant differences between human and animal DRGs pose a challenge for translating findings into effective human treatments.
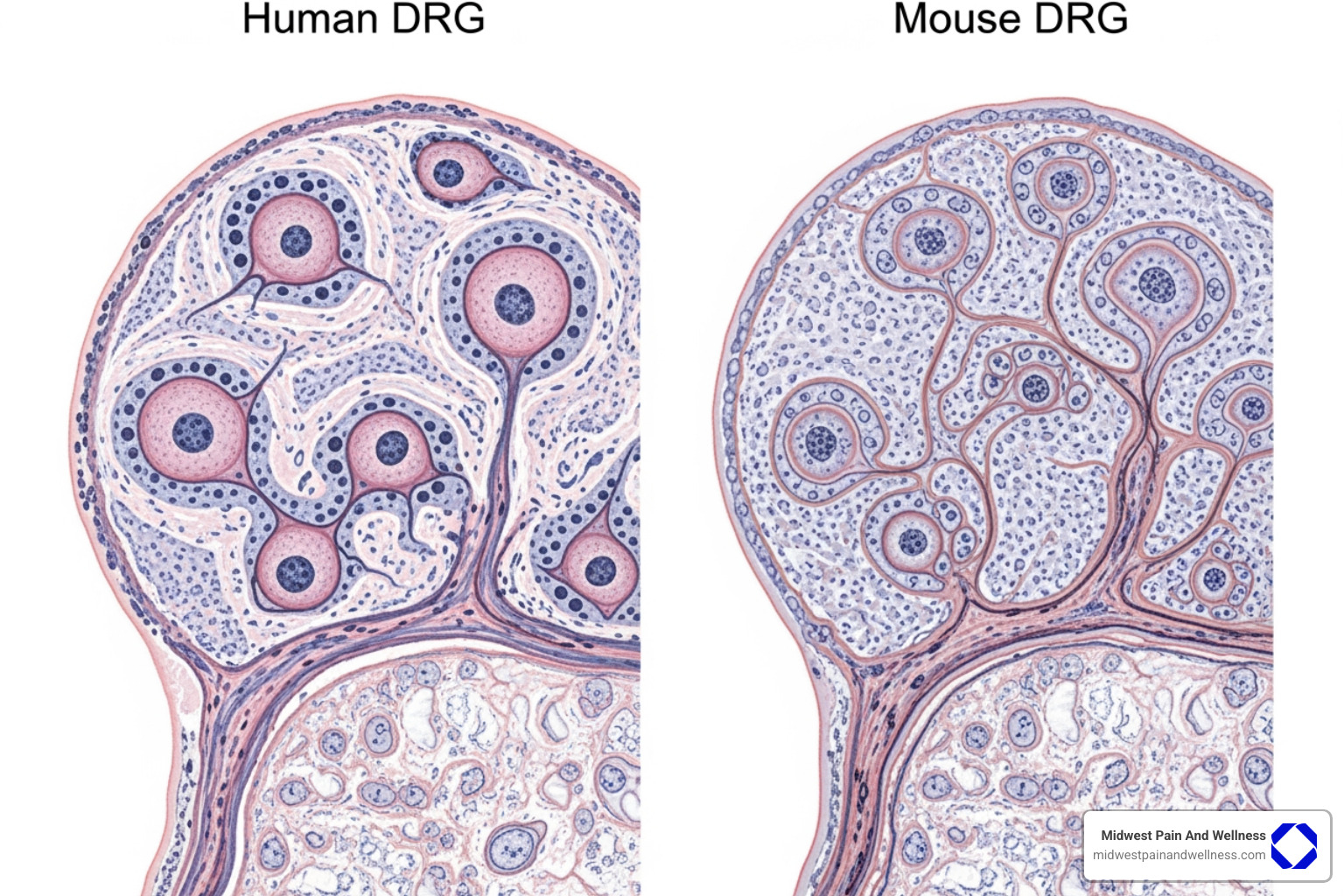
- Neuron Size and Number: Human DRGs are much larger and contain far more neurons than rodent DRGs, with different proportions of neuron subtypes.
- Ion Channel Expression: The expression and behavior of key pain-related sodium channels (like Nav1.7) differ significantly between humans and rodents. This can affect how drugs work, explaining why a drug effective in mice may fail in humans.
- Receptor Differences: The function and distribution of various pain receptors also vary between species. This helps explain why some drugs that work in animal models have failed in human clinical trials.
These differences highlight why many clinical trials based on animal models fail. Researchers now emphasize studying human DRGs directly, using resources like the review “Human Dorsal Root Ganglia” to bridge this knowledge gap. Understanding these molecular differences is key to developing more effective pain treatments for humans.
At Midwest Pain And Wellness, we stay current with this evolving science to provide our patients with the most effective, evidence-based treatments available.
Conclusion
The dorsal root ganglion is more than a simple relay station; it’s a dynamic hub that actively shapes your perception of touch, temperature, and pain. For those with chronic neuropathic pain, the DRG is often the source. When injured or inflamed, it can become a relentless pain generator. Understanding this is the first step toward effective treatment.
Fortunately, modern medicine offers targeted therapies like DRG stimulation. This approach intervenes precisely at the source, providing significant relief—often 70% or more—for previously untreatable conditions, moving beyond systemic medications or invasive surgeries.
At Midwest Pain And Wellness, we witness the life-changing impact of these advances. Our double board-certified doctors use a multi-modal, interventional approach to create custom, opioid-free care plans. Whether you suffer from Complex Regional Pain Syndrome, diabetic neuropathy, or focal pain in the foot, knee, or groin, we are dedicated to finding a path to lasting relief.
Living with chronic pain is exhausting. Understanding the science behind your pain is the first step toward reclaiming your life. The second is finding an expert team that listens and has the expertise to help.
If you’re ready to explore what’s possible, connect with us. Learn how we create custom care plans at https://midwestpainandwellness.com/services/. You don’t have to settle for pain as your new normal. Hope begins with understanding your body, right down to the dorsal root ganglion.