A cluster headache attack doesn’t feel like a typical headache. It often hits fast, centers around one eye or temple, and drives people to pace, rock, or press a hand against the side of the face because sitting still feels impossible. Many patients in the Chicago Ridge area describe the timing as almost cruel. The attacks can come at night, at the same hour, or in repeating cycles that make everyday life feel unpredictable.
The good news is that effective treatment exists, and the best care usually combines fast rescue treatment with a plan to reduce future attacks. For many people in Oak Lawn, Palos Hills, Palos Heights, Worth, Bridgeview, Hickory Hills, Alsip, Burbank, Evergreen Park, and Orland Park, the actual challenge isn’t just finding something that works. It’s finding a clinic that can diagnose the condition correctly, move quickly, and coordinate evidence-based, opioid-sparing treatment without wasting time.
The Unmistakable Pain of Cluster Headaches
A person with cluster headaches often knows the attack is coming before anyone else in the room does. One eye starts to ache. The pain sharpens quickly. The eye may water, the nose may clog or run on the same side, and the person becomes restless instead of wanting to lie down in a dark room. That pattern matters because it helps separate cluster headache from migraine and from sinus or dental pain, which patients are often told they have before the right diagnosis is made.
In practice, this is one of the clearest stories patients tell. The pain is one-sided, severe, and repetitive. It tends to arrive in clusters over days or weeks, then may quiet down for a period before returning. That predictable but brutal rhythm is part of why cluster headache can take over sleep, work, and family routines so quickly.
For patients searching for answers, the most important point is this: cluster headaches are treatable, and treatment should be targeted. Opioids are not the answer here. The strongest evidence supports rapid abortive therapies that stop an attack while it is happening, plus preventive strategies and, when needed, interventional options for harder cases.
If you’ve been dealing with severe one-sided head pain and haven’t found a clear explanation, it helps to start with a clinic that evaluates headache disorders as part of a broader pain diagnosis process. You can see the range of conditions treated at Midwest Pain & Wellness to understand how headache fits into an integrated pain management setting.
Cluster headaches are alarming, but they are not untreatable. The biggest mistake is treating them like ordinary headaches and losing time on the wrong plan.
Understanding the Science Behind Cluster Attacks
Cluster headache is a neurological disorder, not just a bad headache. That distinction matters because the biology explains why certain treatments work quickly and why others do very little. If you understand the mechanism, the treatment pathway makes more sense.
The faulty alarm circuit
A useful way to think about cluster headache is as a faulty biological alarm circuit. One part of that circuit involves the trigeminal system, which carries facial pain. Another part involves autonomic pathways that control tearing, nasal congestion, and other automatic responses. A brain region tied to biological timing is also thought to be involved, which helps explain why attacks often come with striking regularity.
When that circuit switches on, the result is not subtle. Pain builds around one eye or the temple. The eye can become red or watery. The nostril on that side may feel blocked. Many people feel agitated rather than withdrawn.
This is why cluster headaches don’t behave like tension headaches, and why they don’t always behave like migraine either.
How cluster headache differs from migraine
Patients often ask, “How do you treat cluster headaches if they seem similar to migraine?” The first step is recognizing the features that separate them.
Here’s the practical comparison clinicians make:
| Feature | Cluster headache | Migraine |
|---|---|---|
| Pain location | Usually one-sided, often around the eye or temple | Can be one-sided but may be broader |
| Behavior during attack | Restless, pacing, unable to stay still | Often prefers stillness, reduced activity |
| Autonomic symptoms | Tearing, red eye, nasal congestion on the painful side | Can occur, but less defining |
| Pattern | Comes in clusters or cycles | Often less tightly patterned |
| Attack length | Shorter, abrupt, highly intense | Often longer-lasting |
That difference in behavior is one of the most useful clues. A migraine patient often tries to stay motionless. A cluster headache patient often can’t.
Why the biology changes the treatment
Because cluster headache involves this trigeminal autonomic pathway, treatment has to be fast and specific. Standard over-the-counter pain relievers are often too slow. Opioids don’t address the underlying mechanism and can create new problems without reliably stopping attacks.
Better options target the pathway itself. Some constrict dilated cranial vessels and alter trigeminal signaling. Others interrupt pain transmission through nerve-focused approaches. Preventive therapies aim to quiet the cycle before the next attack starts.
A correct diagnosis changes everything. Once a clinician identifies the syndrome for what it is, treatment becomes far more strategic instead of trial-and-error.
Acute Treatments for Stopping an Attack in Its Tracks
A cluster attack at 1:30 a.m. does not leave much room for trial and error. The patient in Orland Park who is pacing the floor needs a treatment that works within minutes, not a medication that might help later in the morning.
That is the standard for acute care. Fast onset. Correct delivery. A plan the patient can access at home, at work, or while trying to get through a cluster cycle in the Chicago suburbs.
The first-line options with the strongest support are high-flow 100% oxygen and subcutaneous sumatriptan. They do not solve the whole disorder, but they are the treatments most likely to stop a single attack quickly. Which one fits best depends on timing, cardiovascular history, insurance coverage, equipment access, and whether the patient can realistically use the treatment the moment pain starts.
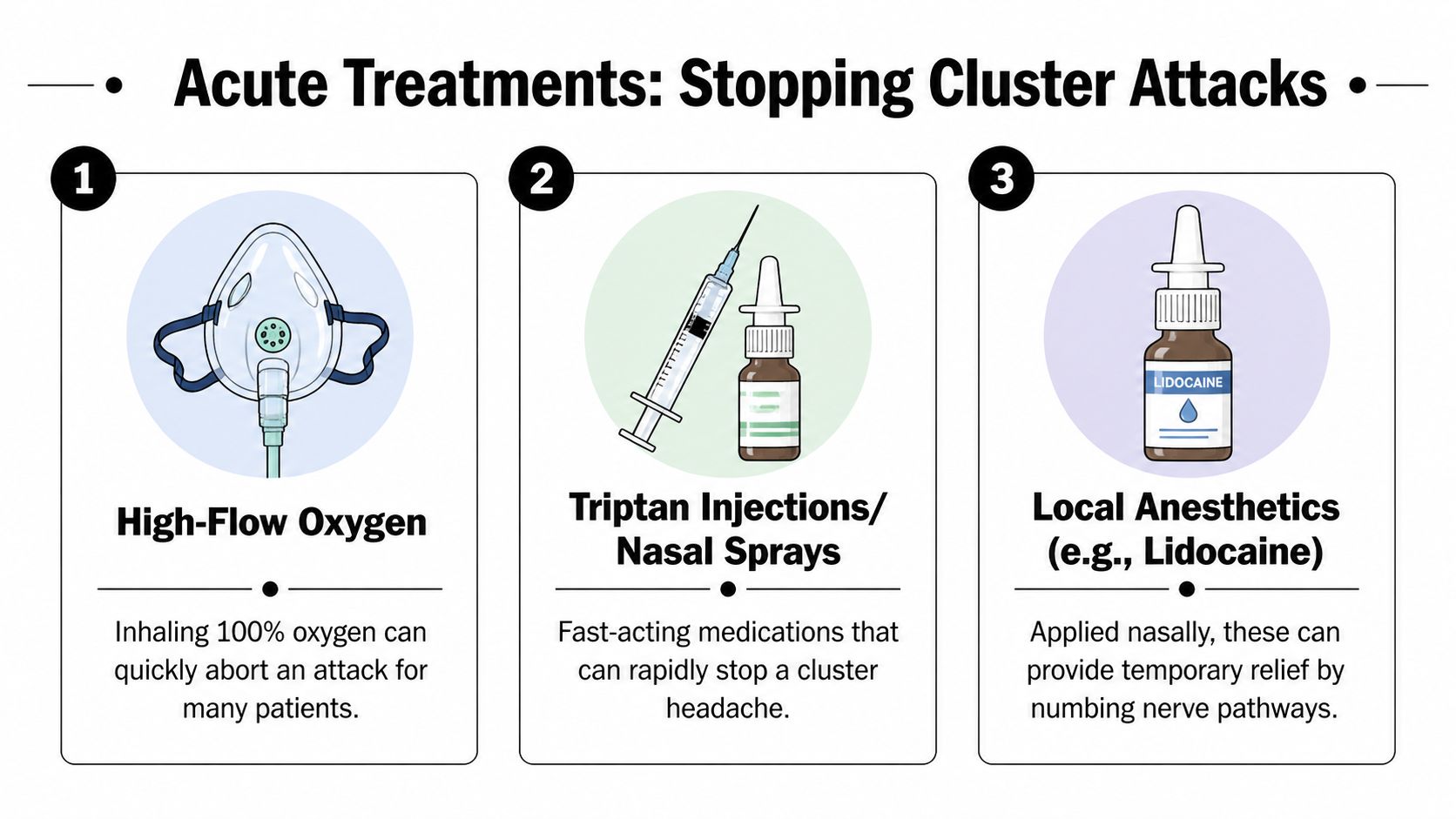
High-flow oxygen
For many patients, high-flow oxygen is the cleanest first rescue option because it can work quickly and avoids medication side effects. The European Academy of Neurology recommends 100% oxygen at at least 12 L/min by non-rebreather mask for 15 minutes, with many attacks stopping rapidly, according to the guideline summary at PubMed.
In practice, oxygen succeeds or fails based on setup. That is where patients often get frustrated. They were technically prescribed oxygen, but the tank was delayed, the regulator did not reach an adequate flow rate, or they were given the wrong mask. Then an effective treatment gets labeled ineffective.
Three details matter most:
- Use a non-rebreather mask. Nasal cannulas and low-delivery masks usually do not give enough oxygen for cluster treatment.
- Start early. The best results come when oxygen begins at the first sign of an attack.
- Confirm the equipment order. Flow rate, mask type, and home delivery logistics need to be specified clearly.
I pay close attention to access barriers here because they are common in Illinois suburbs. A treatment plan on paper is not enough if the DME order is incomplete or the patient cannot get the equipment delivered promptly. Good acute care includes handling those details.
Subcutaneous sumatriptan
Subcutaneous sumatriptan 6 mg is the fastest medication-based abortive treatment used routinely for cluster headache. A randomized trial found that it reduced headache severity within 15 minutes much more often than placebo, as summarized in this PMC review of cluster headache treatment.
This route matters. Oral medications are usually too slow for cluster headache. By the time a tablet is absorbed, the attack may already be near peak intensity or starting to fade on its own.
Sumatriptan works through 5-HT1B/1D receptor agonism, which helps suppress trigeminal signaling involved in the attack, as noted in the guideline summary cited earlier. The trade-off is safety screening. It is not a casual option for patients with certain cardiovascular or cerebrovascular risks, and some patients dislike self-injection even when it works well.
That is a real-world discussion, not a minor detail. The best abortive treatment is the one the patient can use correctly, quickly, and safely every time.
Nasal sprays and other rescue options
Some patients need a backup when injections are not acceptable or not appropriate. Intranasal sumatriptan can help, although it is generally less effective and less reliable than the injected form. The previously cited review also describes benefit with intranasal delivery, but the practical message is simple. It is a reasonable second choice, not the benchmark.
Other alternatives exist for selected patients. As noted earlier in the guideline summary, octreotide 100 mcg subcutaneously may be considered in refractory cases, and non-invasive vagus nerve stimulation may help some patients. These options are most useful when standard first-line treatment is limited by side effects, contraindications, or poor response.
Specialty care matters here because choosing among these options is rarely just about efficacy. It is also about who can obtain the device, who can be trained on it, and how quickly the plan can be adjusted if a cluster cycle is already underway.
Treatments that commonly disappoint
Patients deserve a direct answer about what usually does not work well.
- Over-the-counter pain relievers are often too slow for the speed of a cluster attack.
- Opioids do not reliably abort cluster attacks and add risk without addressing the underlying mechanism.
- Low-flow oxygen or the wrong mask can make a good treatment fail.
- Delaying treatment lowers the chance of stopping the attack early.
A strong acute plan should be specific. It should tell the patient exactly what to use, how to use it, what backup option comes next, and how to get help if the standard approach is not enough. That level of coordination is often the difference between repeated ER visits and a patient who can manage attacks more effectively at home.
Preventive Strategies to Reduce Attack Frequency and Severity
A patient can have the right rescue treatment and still feel trapped if attacks keep returning day after day. Prevention changes that pattern. The goal is to reduce how often attacks hit, shorten the cluster period when possible, and make the whole cycle more manageable.
Verapamil is usually the first preventive medication
For many patients, verapamil is the starting point for prevention. It has the best track record among standard preventive medications for cluster headache, and it is often the first option discussed once attacks become frequent enough to disrupt sleep, work, or daily function.
The practical issue is dose. Many patients do not improve on a low starting dose, so treatment often has to be increased step by step. That takes follow-up, clear instructions, and patience. In clinic, I make that point early because verapamil can help a great deal, but it rarely works as a casual prescription with no monitoring.
Why safe titration matters
Verapamil can affect heart rhythm and electrical conduction. That is why ECG monitoring is often part of the plan, especially as the dose rises or if the patient already has cardiovascular risk factors.
That requirement sounds simple on paper. In real life, it can slow care if the patient is trying to coordinate appointments across different offices in Orland Park, Oak Lawn, or other Chicago suburbs. Good preventive care depends on logistics as much as pharmacology. The right medication only helps if the patient can get monitored, adjust the dose on time, and report side effects before the cluster cycle gets worse.
Prevention gives patients a chance to break the rhythm of repeated attacks instead of living from one flare to the next.
Transitional treatment and second-line options
Some patients need help before a preventive medication has time to work. In that setting, clinicians may use corticosteroids as a short bridge to calm the cycle. Steroids can be useful for a brief period, but they are not a long-term solution because the side effects add up quickly.
Lithium is another option in selected cases, especially when the pattern is harder to control or the patient cannot use verapamil effectively. The trade-off is monitoring. Lithium requires careful prescribing, lab follow-up, and attention to kidney, thyroid, and medication-interaction issues.
Prevention works best when the plan is specific to the patient in front of you. These are the questions that shape that decision:
- How many attacks are happening each day or week
- How much disability the cycle is causing
- How well acute treatment is working
- Whether heart disease, blood pressure issues, or other medical conditions limit medication choices
- Whether the pattern looks episodic or chronic
- Whether a procedure-based option may be needed alongside medication
For some patients, medication alone is enough. For others, a more coordinated plan that includes procedure-based care makes better sense, especially when access, side effects, or incomplete control keep getting in the way. Patients considering that next step can review interventional pain procedures used for treatment as part of an opioid-sparing care plan.
Advanced Interventional Options for Lasting Relief
A common story in clinic goes like this. The diagnosis finally makes sense, the patient has tried oxygen or triptans, a preventive has been started, and attacks are still breaking through often enough to disrupt sleep, work, and basic daily function. At that point, procedure-based treatment deserves a serious discussion, especially for patients in Orland Park, Oak Lawn, and nearby suburbs who have already spent months bouncing between urgent care, neurology, and primary care.
Interventional care adds another layer of treatment for patients with refractory or hard-to-control cluster headache. The goal is to reduce attack burden without piling on more systemic medication, and without defaulting to opioids, which are generally a poor fit for cluster headache.
Nerve blocks that can calm an active cycle
A greater occipital nerve block is one of the more practical interventional tools in selected patients. It can reduce pain signaling and sometimes quiet the system enough to help during an active cluster period, particularly while preventive treatment is still being adjusted.
This option has a clear advantage. It targets a specific pathway instead of exposing the whole body to another daily medication. That matters for patients who are already dealing with medication side effects, blood pressure issues, heart rhythm concerns, or a long list of prior treatment failures.
The trade-off is that relief may be temporary, and response is not uniform. A nerve block works best as part of a larger plan, not as a stand-alone answer.
Neuromodulation for selected patients
Neuromodulation aims to change pain signaling with electrical stimulation rather than medication. For cluster headache, the best-known example is noninvasive vagus nerve stimulation. As noted earlier in the article, guideline-supported data suggest it can help some patients, particularly when the pattern and timing are a good match for the device.
Sphenopalatine ganglion stimulation is more specialized and is usually considered in carefully selected refractory cases. It is not something every patient can access easily. Device availability, insurance approval, candidacy, and follow-up logistics all matter. That is often the barrier for patients in the south and southwest Chicago suburbs. The treatment may exist, but getting evaluated, approved, and coordinated can still be difficult.
Pulsed radiofrequency and other procedure-based options
For refractory cases, sphenopalatine ganglion focused procedures, including pulsed radiofrequency in appropriate settings, may be considered by experienced interventional specialists. The reason to consider them is straightforward. They may offer longer-lasting benefit than a short bridge treatment in the right patient.
They also require careful patient selection. Procedure-based care should follow a confident diagnosis, a review of prior medication trials, and a discussion of expected benefit versus invasiveness. In practice, that means asking whether the headache pattern accurately fits cluster headache, whether standard acute and preventive options were used correctly, and whether the patient can realistically complete the follow-up that advanced treatment requires.
Where a specialized interventional clinic helps
Patients often do better when one team can connect the pieces instead of leaving them spread across several offices. That includes confirming the diagnosis, coordinating acute treatment, deciding whether a block or neuromodulation option makes sense, and accounting for other pain problems that may complicate the picture, such as cervical pain or post-surgical pain.
That coordination matters in real life. A patient from Oak Lawn should not have to piece together one plan for headache, another for neck pain, and a third for medication management, all with different instructions.
Patients who want a clearer sense of the procedure-based side of care can review the interventional pain procedures used for treatment at Midwest Pain & Wellness.
For the right patient, advanced intervention can turn repeated crisis management into a more stable, opioid-sparing treatment path.
Your Treatment Path at Midwest Pain & Wellness
When patients come in with suspected cluster headaches, the first priority is getting the diagnosis right. That starts with a careful history. Where is the pain? How long do attacks last? Does the eye water? Does the nose run on the same side? Is the patient pacing, or trying to lie perfectly still? Those details guide the next step far more than a generic label like “bad headaches.”
Step one is assessment
An effective plan begins with pattern recognition and safety screening. That includes reviewing prior diagnoses, medication history, cardiovascular history, and whether previous treatments matched cluster headache best practice. Many patients have tried something called “oxygen” or “migraine medication” without ever receiving the correct setup or dosing.
This is also where a specialist decides whether the presentation fits cluster headache cleanly or whether another trigeminal autonomic headache, migraine variant, or secondary cause needs to be considered.
Step two is building a practical acute plan
For confirmed or strongly suspected cluster headache, patients need an acute plan they can realistically use. In many cases that means arranging high-flow oxygen correctly and deciding whether a triptan is appropriate.
Access is a real problem. A 2023 to 2024 survey found that 40% of sufferers struggle with access to oxygen, as summarized by Cleveland Clinic’s cluster headache resource. That barrier is one of the biggest reasons patients remain undertreated even when the therapy itself is well established.
For patients in Worth, Bridgeview, Hickory Hills, Alsip, Burbank, and Evergreen Park, this practical support matters as much as the prescription itself. The treatment has to be available, affordable, and set up correctly.
Step three is reducing future attacks
Once acute care is in place, the focus shifts to prevention and escalation planning. If a patient is in a cluster period, the goal is to reduce the cycle, not just survive each attack. That may include preventive medication, a transitional strategy, or procedure-based options when the pattern is refractory or complex.
In such cases, pain medicine can be especially useful. A patient may need a broader plan that also accounts for neck pain, post-surgical pain, sleep disruption, work limitations, or other chronic pain conditions. A specialist has to treat the person, not just the headache label.
A sound pathway usually includes:
- Diagnosis confirmation so treatment matches the syndrome
- Acute rescue planning with oxygen, triptan therapy, or alternatives when appropriate
- Preventive treatment when attacks are recurring in a cycle
- Interventional escalation for patients who remain refractory
- Ongoing coordination with other treating clinicians when comorbid pain issues are present
Why specialized care makes a difference
Cluster headache care often breaks down for simple reasons. Appointments are delayed. Oxygen access is denied or delayed. The wrong device is prescribed. Medication limits create confusion. Patients are told to keep using treatments that are too slow to matter.
That is why specialized, opioid-sparing care matters. A pain clinic with headache experience can move from recognition to treatment to procedural options more efficiently than a fragmented system can.
For patients who want to learn more about the physician leading that care model, visit Dr. Yaw Donkoh’s profile.
Fast treatment is important, but coordinated treatment is what prevents patients from falling through the cracks every time a new cluster cycle begins.
If cluster headaches are disrupting your life in Chicago Ridge, Oak Lawn, Palos Hills, Palos Heights, Worth, Bridgeview, Hickory Hills, Alsip, Burbank, Evergreen Park, or Orland Park, Midwest Pain & Wellness offers evidence-based, opioid-sparing care designed around rapid relief and long-term control. The team evaluates headache patterns carefully, helps patients overcome practical barriers like oxygen access, and builds personalized treatment plans that may include medication management, interventional procedures, and coordinated follow-up.



