That sharp pain from the low back into the buttock, thigh, or calf can change your whole day fast. People across Chicago Ridge and nearby communities like Oak Lawn, Palos Hills, Palos Heights, Worth, Bridgeview, Hickory Hills, Alsip, Burbank, Evergreen Park, and Orland Park often try to push through it, hoping it will settle down on its own.
Sometimes it does. Sometimes it doesn't.
If you're trying to figure out how to ease sciatica pain, the best approach is usually a sequence. Start with the right home steps. Add gentle movement instead of shutting down completely. Watch for warning signs. Then, if the pain keeps hanging on, move toward targeted, opioid-sparing treatment from a pain specialist who can identify what is irritating the nerve.
First Steps for Sciatica Pain Relief at Home
A typical flare starts the same way for many patients I see from Chicago Ridge, Oak Lawn, and Orland Park. You bend, twist, get out of the car, or stand up from a desk, and pain shoots from the low back into the buttock or leg. The first job at home is to quiet the irritation enough to sleep, walk short distances, and keep the problem from escalating.
Start simple. Stay out of bed for long stretches unless you are physically unable to stand. Prolonged bed rest tends to stiffen the back, tighten the hip muscles, and make the nerve more reactive.
Use cold first, then heat
During the first couple of days, cold is usually the better tool. It can help settle local irritation around the low back or upper buttock, especially if the pain feels sharp, hot, or recently aggravated.
Use a wrapped cold pack for 15 to 20 minutes at a time, then give the skin a break before the next session. Do that several times through the day if it helps you move more comfortably afterward. Do not sleep on an ice pack or heating pad.
After the early flare, heat often becomes more useful. Heat does not fix the nerve irritation itself, but it can relax the muscles that start guarding around the low back, hip, and pelvis. If one feels better than the other, use the one that improves your ability to stand upright and walk with less pulling into the leg.
A practical schedule looks like this:
First two to three days
Use a wrapped cold pack on the low back or upper buttock for 15 to 20 minutes.Repeat through the day
Space sessions out and check the skin each time.After the early flare settles
Switch to heat if the area feels tight, stiff, or cramped.If symptoms vary by the hour
Try cold after activity and heat later when muscle tension is the bigger problem.
Practical rule: Use the option that improves movement after the session.
Keep moving, but shrink the range
I tell patients this often in clinic. Sciatica usually responds better to measured movement than to complete shutdown.
That does not mean going to the gym, stretching hard, or trying to walk through a severe limp. It means short walks around the house, standing up every 30 to 45 minutes, and changing positions before pain builds. If the leg pain starts traveling farther down, your activity dose is too high. Back off and shorten the session.
This is one of the main trade-offs early on. Too little movement feeds stiffness. Too much movement stirs up the nerve.
Find positions that reduce pressure
Positioning matters more than many people expect, especially at night or during long hours sitting at work in Palos Hills or driving through traffic toward downtown.
A few useful setups:
For sleep on your side
Put a pillow between the knees so the pelvis stays level.For sleep on your back
Place a pillow under the knees to reduce pull on the low back.For sitting at a desk
Sit back in the chair with support behind the low back and both feet flat on the floor.For driving
Move the seat close enough that you are not reaching with the legs or collapsing into a rounded posture.
This posture often helps at night:

Be careful with over-the-counter medication
Many patients try ibuprofen or naproxen first. That can be reasonable for a short period if your primary doctor has said these medications are safe for you. They are not a good fit for everyone. People with kidney disease, a history of stomach bleeding or ulcers, certain heart conditions, or blood thinner use need more caution.
Medication may take the edge off. It rarely solves the underlying pain generator by itself.
What to avoid in the first few days
Small mistakes can keep a new flare going longer than it needs to.
Deep stretching into leg pain
A stretch should not create a sharp pull, burning, or electric pain below the knee.Long couch sessions
Soft furniture often rounds the spine and increases pressure through the low back.Heavy lifting or repeated bending
Laundry baskets, grocery cases, and garage work are common setbacks.Trying to push through worsening leg pain
If pain is traveling farther down the leg, getting more intense, or causing weakness, stop.
If symptoms keep returning, or if the pain pattern does not behave like a simple muscle strain, it helps to review the pain conditions our clinic evaluates and treats. In an interventional pain clinic, the goal is to identify what is irritating the nerve and decide when home care is enough and when a more targeted, opioid-sparing treatment plan makes sense.
Targeted Stretches and Core Exercises for Sciatica
Once the initial flare isn't dominating every movement, the next step is controlled motion. At this stage, many people either help themselves or accidentally stir the nerve up again.
The key is restraint. A useful stretch or exercise should create a mild release, not a hard pull, burn, or electric jolt down the leg.
Start with two gentle stretches
These aren't meant to be dramatic. They are meant to reduce pressure and restore movement.
Single knee to chest
Lie on your back. Bend one knee and bring it toward the chest with your hands behind the thigh or around the shin, whichever feels easier. Keep the other leg relaxed.
Hold briefly, then release. If the stretch increases shooting pain below the knee, back off and shorten the motion.
Figure four or piriformis stretch
Lie on your back. Cross the ankle of the painful side over the opposite knee. Gently bring the bottom leg toward you until you feel a stretch in the buttock or hip.
You should feel tension in the hip, not a nerve zing down the calf or foot.
This type of hip opening can be helpful when the buttock muscles are adding tension around the nerve pathway:

Use the sciatic nerve slider carefully
One of the most useful techniques for some patients is the seated sciatic nerve slider, also called a neural mobilization or nerve flossing movement. The goal is not to stretch the nerve hard. The goal is to help it glide more normally.
According to OrthoNJ's sciatic stretch and exercise guide, 70 to 80% of patients who perform the seated sciatic nerve slider correctly report more than a 30% reduction in pain after two weeks, and a randomized controlled trial found a 62% success rate at 4 weeks compared with 38% for static stretching alone.
How to do it
- Sit near the edge of a firm chair.
- Keep your chest upright.
- Straighten the affected leg forward.
- Pull the toes up gently.
- At the same time, look slightly upward.
- Then reverse it. Bend the knee back in, relax the foot downward, and tuck the chin.
- Repeat slowly.
This should feel like a light tug, not a deep strain.
If the movement leaves your leg more irritable for hours afterward, you did too much. Reduce the range, slow it down, or stop until you've been evaluated.
Keep the range small at first
In Palos Hills, Hickory Hills, and surrounding suburbs, I often see people who got into trouble because they found a stretch online and attacked it too aggressively. Sciatic pain doesn't usually reward force.
A few good guardrails:
Stay in a pain-free or near pain-free range
Mild tension is fine. Sharp pain isn't.Move slowly
Fast repetitions often add guarding.Stop if symptoms travel farther down the leg
That's usually a sign the nerve is getting more irritated.Choose consistency over intensity
Gentle daily work is usually better than one long session.
Build support with basic core control
Core exercise for sciatica does not mean high-rep crunches or intense abdominal circuits. It means teaching the trunk and pelvis to stay more stable during daily movement.
A simple starting sequence can include:
| Exercise | What to focus on | Common mistake |
|---|---|---|
| Pelvic tilt | Small controlled motion of the low back | Forcing a large flattening movement |
| Abdominal brace | Light tightening while breathing normally | Holding your breath |
| Bridge, partial range | Squeeze glutes and lift only as tolerated | Arching the low back |
| Bird dog, modified | Reach one limb at a time with control | Twisting through the trunk |
These aren't flashy. They matter because many people with recurrent sciatica don't just have a pain problem. They also have a movement-control problem.
What works better than random internet stretching
A short, focused routine beats a long list of exercises. If you're trying to decide what to keep and what to drop, use this filter:
- Keep it if it improves walking, sitting tolerance, or the ability to stand upright after you finish.
- Drop it if it causes more numbness, more leg weakness, or pain that travels farther.
- Modify it if the same movement helps one day but irritates you the next. That usually means the dose is the issue, not necessarily the exercise itself.
For many patients, the best home routine is surprisingly small. A brief walk. One hip stretch. One nerve slider. One or two core-control drills. That's often enough to tell whether you're improving or whether it's time for more targeted treatment.
Red Flags When to Call a Pain Specialist in Illinois
Not every sciatic flare needs a procedure. Some do need timely medical attention.
The hardest part for patients in Worth, Bridgeview, or Palos Heights is knowing when to stop self-managing and get evaluated. Waiting too long can make the problem harder to calm down, especially if weakness starts to appear or pain keeps dominating daily life.
Symptoms that need urgent action
Some symptoms should not wait for a routine office visit.
If you develop bowel or bladder changes, rapidly progressive leg weakness, or major loss of control in the foot, you need immediate medical evaluation. Those symptoms can point to severe nerve compression.
Other signs deserve prompt specialist review rather than another week of hoping:
- Progressive numbness
- Foot drop
- Severe pain not relieved by two weeks of conservative care
A 2025 study in Pain Medicine found that delaying specialist care beyond 6 weeks led to 40% worse outcomes at one year, and only 25% of that group achieved significant pain reduction compared with 65% of early intervention patients, as summarized in Healthline's review of sciatica stretches and escalation guidance.
The biggest mistake isn't trying home care first. It's staying in home-care mode long after the body has shown that it isn't enough.
Sciatica symptoms when to seek care
| Symptom Level | What It Looks Like | Recommended Action |
|---|---|---|
| Mild and improving | Pain travels down the leg but is easing with activity changes and home care | Continue conservative care and monitor closely |
| Persistent | Pain is still limiting sitting, walking, work, or sleep after a couple of weeks | Schedule a pain specialist consultation |
| Concerning neurologic change | Increasing numbness, foot weakness, tripping, or foot drop | Seek prompt specialist evaluation |
| Emergency | Bowel or bladder changes with severe nerve symptoms | Go to the ER immediately |
When a pain specialist visit makes sense
You don't need to wait for an emergency to ask for help. A specialist evaluation is appropriate when pain remains stubborn, when daily function is sliding, or when you're not sure whether the issue is a disc, spinal stenosis, joint pain, or another nerve source.
In those situations, scheduling a pain consultation in Chicago Ridge can help clarify the next step before an acute problem becomes a chronic one.
Advanced Sciatica Treatments for Lasting Relief
By the time patients from Chicago Ridge, Oak Lawn, Palos Hills, or Orland Park reach our clinic, the pattern is usually familiar. They have already tried ice, heat, over the counter medication, online stretches, a different chair, and cutting back on activity. The pain still shoots from the low back or buttock into the leg, and daily life starts shrinking around it.
That is the point where a pain and wellness clinic can add something different.
Our job is to identify the structure driving the nerve irritation, confirm whether the symptoms fit true sciatica or a mixed pain pattern, and choose treatment that reduces pain without making opioids the center of the plan. That matters because leg pain can come from a disc herniation, spinal stenosis, inflammation around a nerve root, sacroiliac dysfunction, or more than one problem at the same time.
What a proper evaluation looks like
Sciatica describes a symptom pattern. It does not explain the cause.
A useful specialist visit starts with a focused history and exam that answers practical questions:
- Where the pain begins and how far it travels
- Whether numbness, tingling, or weakness is present
- Which positions make it worse, such as sitting, standing, coughing, bending, or walking
- Whether the pattern fits a disc problem, spinal narrowing, inflammation, or another pain source
If the exam suggests nerve compression, MRI imaging may help identify the level involved. In some cases, additional testing helps separate spine-related leg pain from hip, joint, or peripheral nerve problems. That distinction changes treatment.
This is the pathway many patients follow:
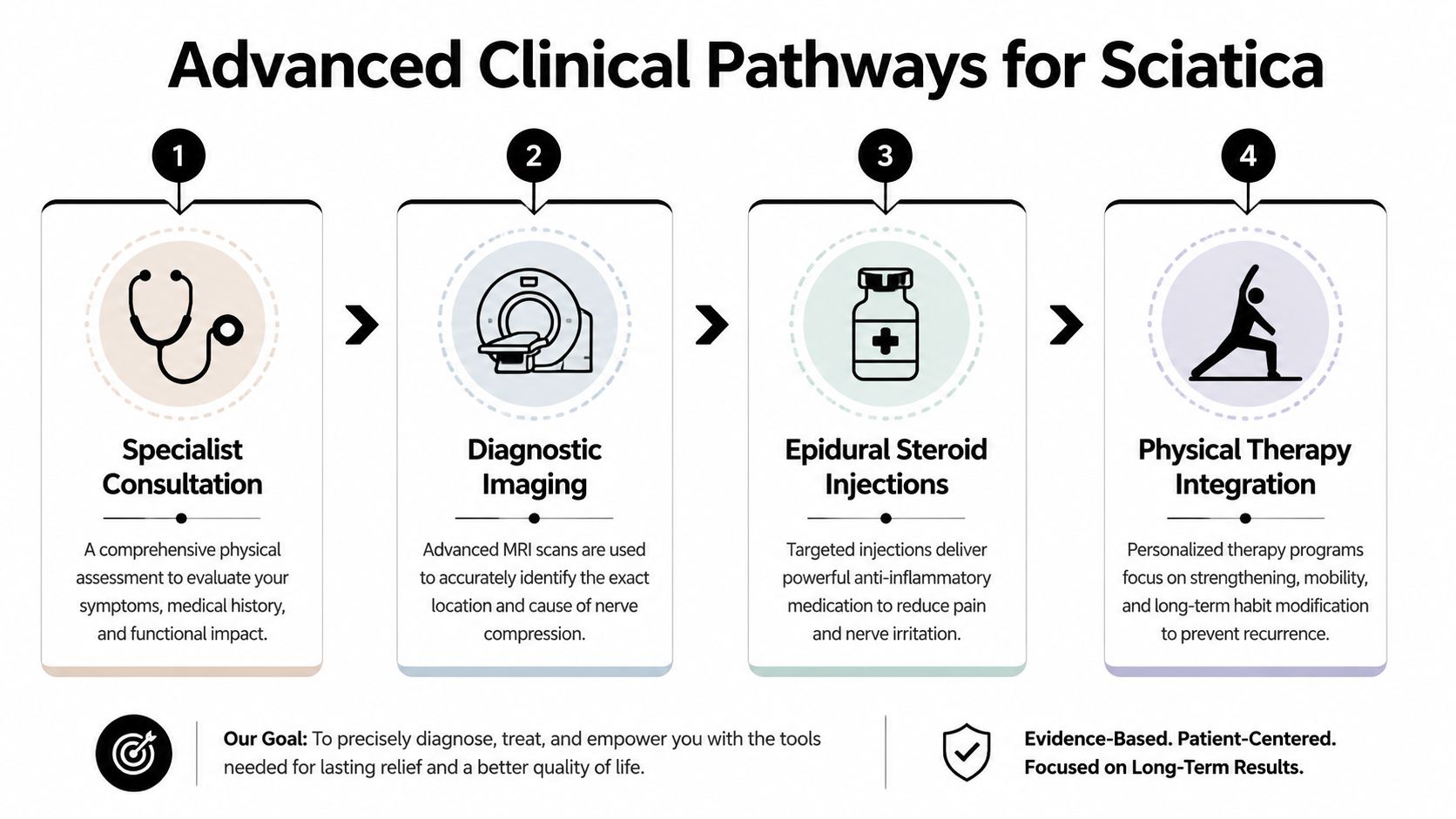
Why opioid-sparing treatment matters
Severe sciatic pain can make people desperate for quick relief. I understand that. But with nerve-root pain, the better strategy is to calm the irritated structure and restore function so the patient can sit, walk, sleep, and participate in recovery again.
In practice, that usually means a layered plan. Medication may still play a role, but the center of care is often a targeted procedure, careful activity guidance, and follow-up based on how the nerve responds. That approach aims to reduce pain while avoiding the sedation, constipation, tolerance, and dependence risks that often come with prolonged opioid use.
A good treatment plan should help you do more than survive the day. It should help you get back to driving, working, sleeping, and moving with less fear.
Treatments commonly considered for persistent sciatica
Epidural steroid injections
For many patients, this is the main interventional option when a disc bulge, disc herniation, or inflamed nerve root is driving the pain. The medication is placed near the irritated nerve under image guidance.
The goal is straightforward. Reduce inflammation around the nerve so pain settles enough for normal movement and recovery to restart. It is not the right choice for every patient, and it does not fix every structural problem, but it can make a major difference when the diagnosis fits.
Selective nerve root blocks
Sometimes the diagnosis is mostly clear, but not completely. A selective nerve root block can help confirm which nerve is causing the symptoms while also providing treatment. This matters when MRI findings and the pain pattern do not match perfectly, which is common in real clinic practice.
That kind of precision matters before choosing the next step.
Medial branch and related diagnostic blocks
Some patients come in saying they have sciatica, but the full picture includes significant facet-related back pain along with leg symptoms. In that setting, medial branch blocks may help determine whether a second pain generator is contributing.
A careful pain specialist does not force every back and leg complaint into one diagnosis. Mixed pain patterns are common, especially in older adults and in patients who have been hurting for months.
Radiofrequency ablation
Radiofrequency ablation is used more often for facet-mediated back pain than for classic nerve-root sciatica. Still, it can be helpful when diagnostic blocks confirm that facet joints are part of the ongoing pain picture.
This is one of the trade-offs I discuss with patients. If the main problem is a compressed nerve root, RFA is not the primary answer. If the pain is mixed, treating the facet component may lower the total pain burden and improve function.
Minimally invasive lumbar decompression and related options
Some patients do not have a primary disc herniation. They have spinal stenosis or ligament-related narrowing that crowds the nerves, especially with standing and walking. When the anatomy fits, minimally invasive decompression procedures such as MILD may be appropriate.
For older patients in Orland Park, Palos Heights, or Burbank, this can be an important middle ground. It offers more than medication and exercise alone, while avoiding a larger surgical procedure when that is not the right fit.
What patients should realistically expect
A good clinic visit should leave you with a clear plan, not more confusion.
| Question | What you should hear |
|---|---|
| What is causing the pain pattern | A working diagnosis based on your history, exam, and imaging if needed |
| Why this treatment fits | A reason tied to your symptoms, exam findings, and anatomy |
| What the procedure can and cannot do | Expected benefit, limitations, and how success will be measured |
| What happens after the procedure | Activity guidance, medication review, and follow-up planning |
Procedures are tools, not standalone solutions. Their value is highest when they are part of a broader care plan that may include medication adjustment, structured exercise, lifestyle changes, and surgical referral if weakness is progressing or the anatomy calls for it.
The best next step is often sooner, not later
One of the most common problems I see in the Chicago suburbs is delay. Patients from Evergreen Park, Oak Lawn, and nearby communities often spend months rearranging life around the pain before they get evaluated. By then, walking tolerance is down, sleep is poor, work is harder, and the nerve has stayed irritated for far too long.
Earlier evaluation does not mean rushing into a procedure. It means getting the diagnosis right before temporary nerve irritation turns into a longer recovery.
If you want a clearer picture of what may be available beyond home care, review the clinic's interventional procedures used for pain treatment before your visit. It makes the conversation more specific, and that usually makes the decision process easier.
Building a Sciatica-Resistant Lifestyle in the Chicago Area
Once the pain settles, the next job is keeping it from coming right back. That's where daily setup matters more than commonly realized.
Many flare-ups aren't caused by one dramatic injury. They build from repeated sitting, poor workstation mechanics, long commutes, awkward lifting, and letting small warning signs pile up.
Fix your sitting setup before it fixes you
Occupational data shows 60% of sciatica cases are linked to prolonged sitting, and a 2025 study found that desk workers who adjusted their chair setup to allow for 90 to 110 degrees of hip flexion reduced recurrence by 55% over six months. The same source notes that a lumbar support pillow can reduce spinal compression by up to 35%, according to HSSH's sciatica relief article.
That has direct day-to-day implications for desk workers in Burbank, Evergreen Park, and Palos Hills.
A better desk position usually means:
Hips slightly open
Don't jam yourself into a rigid 90-degree folded position if a slightly more open angle feels better.Low back supported
A small lumbar support pillow often helps people maintain a more neutral sitting posture.Feet planted
Avoid perching on the edge of the chair or tucking one leg under you.Frequent resets
Stand up, walk briefly, or change position before stiffness fully sets in.
Driving and commuting need their own strategy
People who drive for work or spend a lot of time commuting from Orland Park, Worth, or Bridgeview often notice that the car is one of the worst places for sciatic pain.
A few practical adjustments help:
- Move the seat close enough that your knees aren't fully straight while driving.
- Keep the backrest supportive rather than reclined too far.
- Use a small lumbar support if the seat pushes you into a slump.
- Get out and walk briefly during longer drives when possible.
The best posture isn't one perfect posture you hold all day. It's the posture you change often enough that one tissue doesn't take all the load.
Make movement part of the workday
This matters as much as the chair itself. Static posture is often the actual problem.
For office workers and drivers, a realistic prevention routine looks like this:
- Brief walking breaks during the day
- Gentle nerve slider or hip mobility work if it has helped you before
- Simple core control drills several days a week
- Less weekend overcorrection, where you sit all week and then do one punishing workout
People in Hickory Hills and Palos Heights often tell me they do fine until they combine long sitting with one heavy lifting task at home. That combination is common. The answer is usually better consistency, not more heroics.
Use better mechanics for everyday lifting
You don't need a warehouse job to aggravate sciatica. Laundry, pet food, cases of water, gardening supplies, and grandkids can all do it.
A few rules help:
- Keep the load close
- Pivot the feet instead of twisting through the spine
- Break up large loads
- If the leg is already irritated, don't test it with repetitive bending
Keep the recovery habits that actually worked
Once pain improves, many people abandon the exact habits that got them better. Then the cycle repeats.
The most useful maintenance plan is usually simple:
| Habit | Why it matters |
|---|---|
| Walking regularly | Keeps the body from stiffening into prolonged sitting patterns |
| Using supportive sitting posture | Reduces repeated strain during work and driving |
| Continuing a small home routine | Maintains mobility and control without overdoing it |
| Addressing flares early | Prevents a mild setback from becoming a major episode |
If you've been trying to figure out how to ease sciatica pain, the long-term answer is rarely one trick. It's a combination of better mechanics, timely response to flare-ups, and getting evaluated when self-care stops moving the problem in the right direction.
If sciatica is still limiting your work, sleep, or ability to move comfortably around Chicago Ridge, Oak Lawn, Palos Hills, Orland Park, or nearby Illinois communities, Midwest Pain & Wellness offers opioid-sparing, interventional care focused on identifying the pain source and building a personalized plan for lasting relief.



