Understanding Your Pelvic Pain: Why Relief Starts with Knowledge
Pelvic pain relief begins with understanding the source of your discomfort. Whether it’s a sharp, stabbing sensation or a dull, persistent ache, effective relief is possible through a personalized, multi-modal approach.
Quick Relief Options for Pelvic Pain:
- Heat therapy – Apply a heating pad to the lower abdomen for 15-20 minutes.
- Over-the-counter pain relievers – Use NSAIDs like ibuprofen as directed.
- Gentle movement – Try light walking or stretching to improve blood flow.
- Pelvic floor physical therapy – Seek specialized treatment for muscle-related pain.
- Stress reduction – Practice deep breathing, meditation, or mindfulness.
- Medical interventions – Consider trigger point injections or other opioid-free treatments.
Pelvic pain affects approximately 1 in 7 women and many men, making it a common condition. This discomfort, located below your belly button and between your hips, can be acute (short-term) or chronic (lasting 3-6 months or more). The pain can stem from reproductive, urinary, digestive, or musculoskeletal issues, and often a combination of factors. This complexity means that an estimated 50% of cases remain undiagnosed despite thorough evaluation.
However, relief is achievable. Understanding the source of your pain and exploring the right treatments can significantly improve your quality of life. This guide will cover common causes, diagnosis, and the full spectrum of treatment options—from home remedies to advanced, opioid-free interventional procedures.
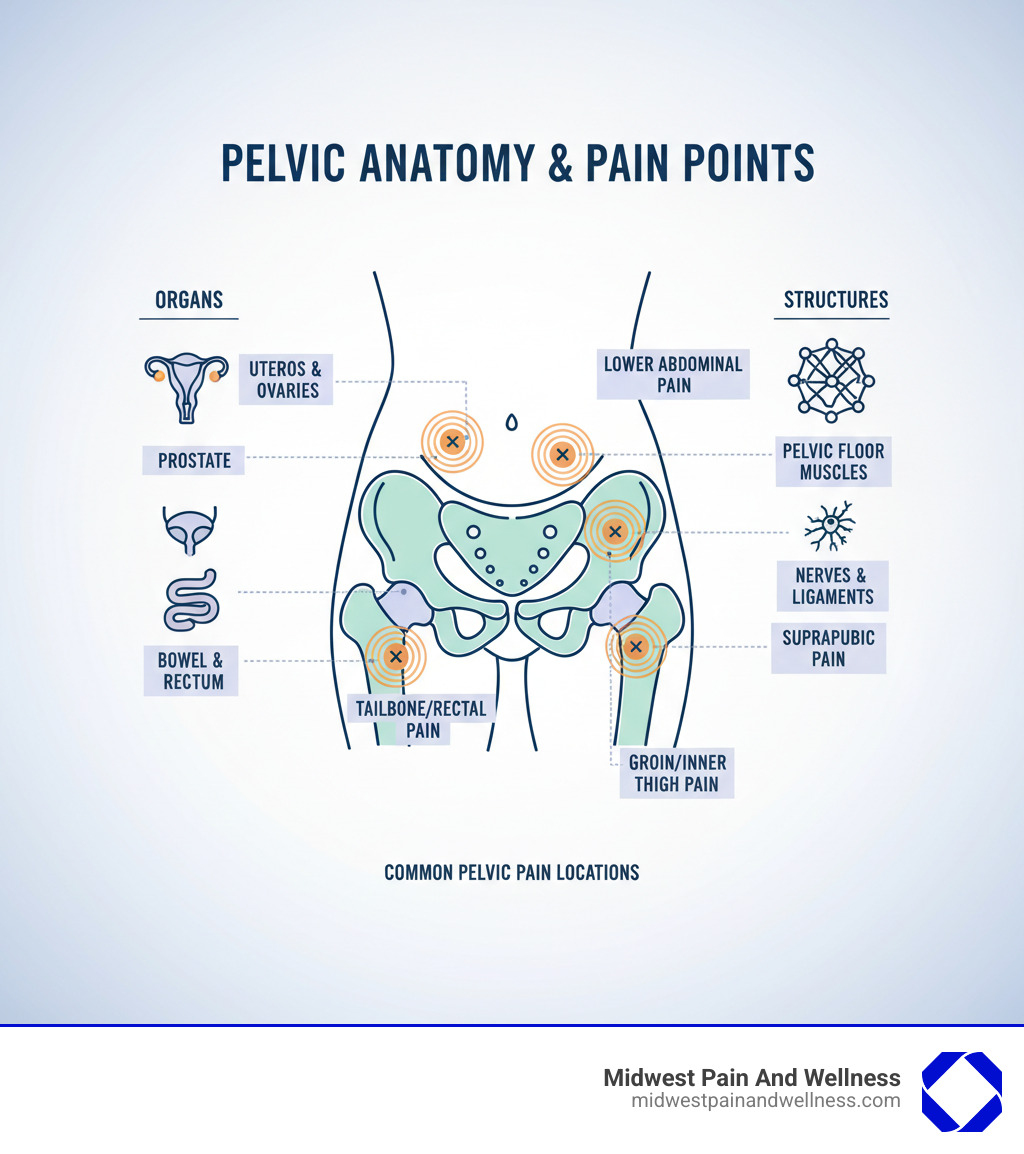
Understanding Pelvic Pain: Common Causes and Symptoms
Your pelvis contains the reproductive, urinary, digestive, and musculoskeletal systems, all connected by a web of nerves. Pain here can feel sharp, dull, burning, or like cramping, and its characteristics provide clues to its origin. Pain that changes with your menstrual cycle may suggest a gynecological issue, while discomfort during urination could point to a bladder condition.

Common Causes in Women
Women face a wide range of potential causes, with 4% to 16% experiencing chronic pelvic pain.
- Endometriosis: Tissue similar to the uterine lining grows outside the uterus, causing inflammation, scarring, and severe pain, especially during periods. You can find more scientific research on endometriosis.
- Uterine Fibroids: Non-cancerous growths in the uterus that can cause pain, pressure, and heavy bleeding.
- Adenomyosis: Uterine lining tissue grows into the muscular wall of the uterus, causing heavy periods and deep, aching pain.
- Pelvic Inflammatory Disease (PID): An infection of the reproductive organs, often from an STI, that can lead to scarring and chronic pain.
- Ovarian Cysts: Most are harmless, but large, ruptured, or twisted cysts can cause sudden, severe pain.
- Menstrual Cramps (Dysmenorrhea): While mild cramping is common, severe pain can signal an underlying condition.
- Ovulation Pain (Mittelschmerz): A sharp, brief pain on one side of the lower abdomen mid-cycle.
- Pregnancy-Related Pain: Discomfort from stretching ligaments is normal, but severe or persistent pain requires evaluation.
- Ectopic Pregnancy: A medical emergency where a fertilized egg implants outside the uterus, causing severe pain and potential bleeding. Seek immediate care if suspected.
Common Causes in Men
Chronic pelvic pain affects 2% to 16% of men and can be equally disruptive.
- Prostatitis: Inflammation of the prostate gland causing pain in the perineum, groin, or lower back, often with urinary symptoms.
- Chronic Pelvic Pain Syndrome (CPPS): Ongoing pelvic pain without a bacterial infection, often linked to muscle tension and nerve issues. Read more in this information on Chronic Primary Pelvic Pain Syndrome in Men.
- Hernias: Tissue pushing through a weak spot in the abdominal wall, causing groin pain, especially with activity.
Causes Affecting All Genders
Many causes are unrelated to reproductive organs.
- Urinary Tract Infections (UTIs): Bacterial infections causing lower abdominal pain and burning during urination.
- Interstitial Cystitis (Bladder Pain Syndrome): A chronic condition causing bladder pressure, pain, and frequent urination. For more information, visit Details on Interstitial Cystitis.
- Kidney Stones: Hard deposits causing severe pain that radiates from the back to the lower abdomen.
- Irritable Bowel Syndrome (IBS): Causes cramping, bloating, and changes in bowel habits.
- Other Digestive Issues: Chronic constipation, inflammatory bowel disease (Crohn’s, ulcerative colitis), diverticulitis, and appendicitis can all cause pelvic pain. Appendicitis is a medical emergency.
- Musculoskeletal Problems: Pelvic floor muscle spasms, myofascial pain (trigger points), nerve entrapment (like pudendal neuralgia), and sacroiliac joint dysfunction can all be sources of significant pain.
When to Seek Immediate Medical Attention
Go to the emergency room or call 911 for these red flag symptoms:
- Sudden, severe, and unbearable pain
- High fever or chills
- Nausea and vomiting with severe pain
- Dizziness, fainting, or heavy bleeding
- Severe pain during pregnancy
- Inability to stand up straight
- Blood in your urine or stool
The Path to Diagnosis: How Doctors Uncover the Source of Pain
Finding the source of pelvic pain is challenging because many organ systems are located in a small area. At Midwest Pain And Wellness, we take a systematic approach to uncover the cause, as a clear diagnosis is the first step toward effective pelvic pain relief.

Your Initial Consultation
Your journey begins with an in-depth conversation. We listen to your story to understand your pain: when it started, what it feels like, and what makes it better or worse. We will review your medical, surgical, and psychological history, as past procedures or emotional stress can contribute to chronic pain. A physical examination, which may include an abdominal, pelvic, or rectal exam, helps us identify tenderness, masses, or muscle issues. We may also use simple tests like the Carnett test (tensing abdominal muscles) or the cotton-tipped applicator test to pinpoint the pain’s source. Keeping a pain journal can also reveal important patterns.
Diagnostic Tests and Procedures
To confirm a diagnosis or rule out certain conditions, we may recommend additional tests.
- Lab Tests: Blood tests check for infection or inflammation, while a urinalysis can detect a UTI. STI screening and a pregnancy test are also common.
- Imaging Studies: A pelvic ultrasound is often the first step to visualize organs like the uterus and ovaries. An MRI provides more detailed images of soft tissues, useful for identifying endometriosis or nerve problems, while a CT scan is helpful for examining the bowel and urinary tract. You can find more information at the Mayo Clinic’s resource page.
- Minimally Invasive Exploration: If imaging is inconclusive, a laparoscopy (a tiny camera inserted into the abdomen) can directly view pelvic organs to diagnose conditions like endometriosis. A hysteroscopy examines the inside of the uterus, and a cystoscopy looks inside the bladder.
A Spectrum of Solutions for Pelvic Pain Relief
Effective pelvic pain relief rarely comes from a single solution. At Midwest Pain And Wellness, we use a comprehensive, multi-modal approach, creating a custom care plan that combines different therapies to address the root cause of your pain. Our goal is to find long-term relief without relying on opioids.

Home Remedies and Lifestyle Changes for Pelvic Pain Relief
Simple strategies can provide significant comfort and work well alongside medical treatments.
- Heat Therapy: A heating pad or warm bath can relax cramping muscles and increase blood flow, providing immediate relief.
- Gentle Movement: Activities like walking, swimming, or light stretching release endorphins (natural painkillers) and improve circulation without straining your pelvis.
- Stress Reduction: Since stress amplifies pain, practices like meditation, mindfulness, and deep breathing can calm your nervous system and break the pain-stress cycle.
- Diet and Posture: An anti-inflammatory diet rich in fruits, vegetables, and lean proteins can reduce systemic inflammation. Improving your posture can also reduce strain on pelvic muscles. For some, weight management can relieve pressure on pelvic structures.
You can learn more about our holistic approach to wellness at More about our approach to wellness.
The Role of Medications
Medications can be a key part of your relief plan, and we prioritize effective, opioid-free solutions.
- Over-the-counter pain relievers: NSAIDs like ibuprofen (Advil) reduce inflammation, while acetaminophen (Tylenol) can ease pain.
- Hormonal Treatments: For pain related to the menstrual cycle, birth control pills, GnRH injections, or progestin-releasing IUDs can be very effective.
- Other Medications: Muscle relaxants can help with pelvic floor spasms. Certain antidepressants are also excellent for chronic pain as they alter how the brain processes pain signals, offering a non-addictive alternative for relief.
How Pelvic Floor Physical Therapy Can Help
Pelvic floor physical therapy (PFPT) is a cornerstone treatment for many types of pelvic pain. The pelvic floor is a group of muscles supporting your pelvic organs, and when they are too tight or weak, they can cause significant pain. A specialized therapist uses techniques to address these issues.
- Manual Therapy: Techniques like myofascial release apply gentle, sustained pressure to release tension in tight muscles and connective tissues.
- Biofeedback: This helps you see what your pelvic floor muscles are doing in real-time, teaching you how to properly contract and, more importantly, relax them.
- Therapeutic Exercise: Your therapist will guide you through specific strengthening or relaxation exercises custom to your needs.
- Trigger Point Therapy: This involves releasing painful “knots” in the pelvic floor muscles to provide relief.
PFPT aims to restore proper muscle function, which can improve pain as well as bladder, bowel, and sexual function.
Managing Chronic Pain: Advanced Treatments and Long-Term Wellness
Living with chronic pelvic pain can rewire your nervous system, a process called central sensitization. This makes your body overly sensitive to pain, creating a cycle where pain persists even after an initial injury has healed. Addressing chronic pain requires a long-term strategy that retrains this brain-pain connection.
Interventional Options for Lasting Pelvic Pain Relief
When other therapies aren’t enough, Midwest Pain And Wellness offers advanced, opioid-free interventional procedures that target the source of your pain.
- Trigger Point Injections: An anesthetic is injected into tight muscle knots (trigger points) to release tension and break the pain cycle.
- Nerve Blocks: Anesthetic is injected near specific nerves to block pain signals. These can be diagnostic (to identify the source) or therapeutic (for longer-term relief).
- Botulinum Toxin (Botox) Injections: Injected into spastic pelvic floor muscles, Botox can provide relaxation and pain relief for several months.
- Neuromodulation: For severe, persistent pain, spinal cord stimulation uses a small implanted device to send mild electrical pulses that block pain signals from reaching the brain.
- Radiofrequency Ablation: This procedure uses heat to create a lesion on a nerve, preventing it from sending pain signals for a year or more.
Find more details on our specific procedures at Details on our Treatment Procedures.
The Connection Between Pelvic Pain and Mental Health
Chronic pain and mental health are deeply linked. Pain can lead to depression and anxiety, while these conditions can, in turn, amplify pain. A history of trauma is also strongly associated with chronic pelvic pain. That’s why psychological support is an essential part of comprehensive pain management. Therapies like Cognitive Behavioral Therapy (CBT), mindfulness, and talk therapy can help you develop coping strategies, change negative thought patterns, and process the emotional impact of living with pain.
Long-Term Implications of Untreated Pain
Ignoring chronic pelvic pain can have serious consequences. It can decrease your quality of life, harm work and relationships, allow underlying conditions to worsen, and lead to the development of chronic pain syndromes like central sensitization. Proactive, comprehensive care is crucial to avoid these outcomes and manage pain effectively for the long haul. Our philosophy emphasizes early intervention to improve your quality of life. More info about our treatment philosophy.
Frequently Asked Questions about Pelvic Pain
We hear these questions often from our patients in Chicago Ridge. Here are some straightforward answers to common concerns.
How do I know if my pelvic pain is serious?
Sudden, sharp, or severe pain should never be ignored, especially if you also have a fever, vomiting, or heavy bleeding. These are red flags that could signal an emergency like appendicitis or an ectopic pregnancy. However, any chronic pain that disrupts your daily life is also serious enough to warrant a medical evaluation. A doctor can rule out dangerous conditions and help you find a path to pelvic pain relief.
Can pelvic pain be cured completely?
The answer depends on the cause. If your pain is from a treatable issue like a UTI or a specific ovarian cyst, a cure is often possible. For chronic conditions like endometriosis or interstitial cystitis, a complete “cure” may not be realistic. However, the goal shifts to effective management. With the right combination of treatments, we can achieve significant, long-lasting pain reduction that allows you to live a full, active life.
Is it normal to have some pelvic pain during pregnancy?
Yes, mild aches and pains are a normal part of pregnancy as your body changes. However, you should always contact your doctor for any sharp, severe, or persistent pain, or pain accompanied by bleeding, regular contractions, fever, or fluid leakage. These could be signs of a complication that requires immediate medical attention. It’s always better to be cautious and get checked out.
Conclusion
Living with pelvic pain can be isolating, but it’s crucial to remember that pelvic pain relief is achievable. The path to feeling better begins with understanding that your pain is complex, often stemming from a combination of reproductive, urinary, digestive, or musculoskeletal issues. You do not have to accept discomfort as your new normal.
At Midwest Pain And Wellness in Chicago Ridge, Illinois, we believe in personalized, multi-modal care. Our double board-certified specialists create custom, opioid-free treatment plans that target the root causes of your pain. By collaborating with physical therapists and other practitioners, we address the whole person, not just the symptoms.
Whether you need help with lifestyle adjustments, specialized therapies, or advanced interventional procedures, we are here to guide you. You’ve already taken the first step by educating yourself. Now, let us help you take the next one toward reclaiming your comfort and quality of life.
Ready to explore your options? Learn more about the conditions we treat and the comprehensive solutions we offer: Learn about the Conditions We Treat.