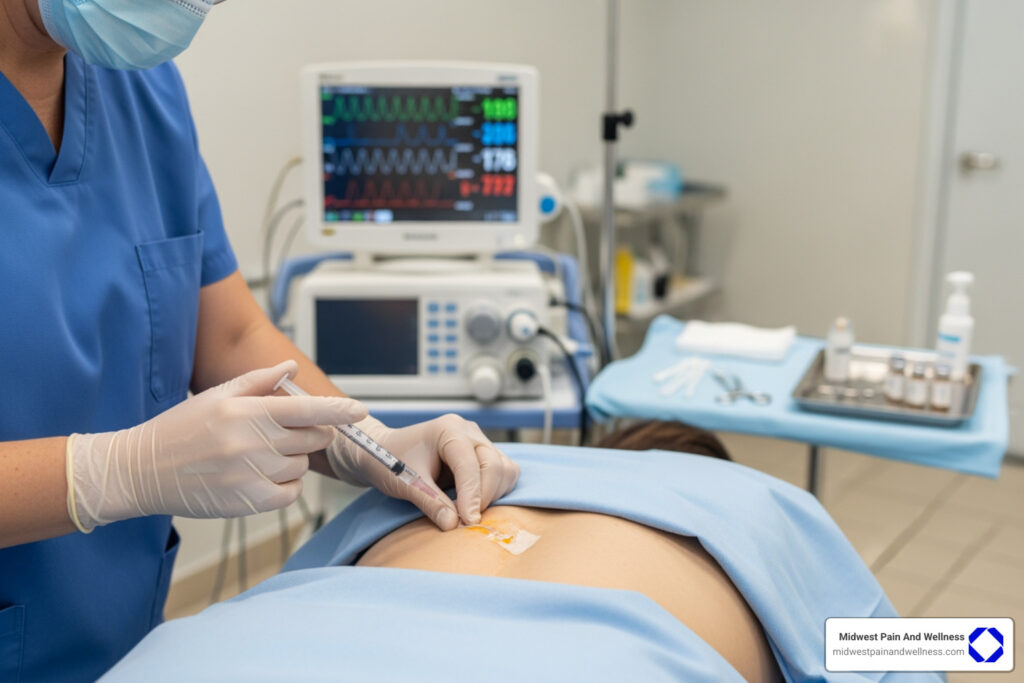
Why Chronic Pain Sufferers Are Turning to Peripheral Nerve Stimulation
Peripheral nerve stimulation (PNS) is a minimally invasive treatment that uses mild electrical pulses to block pain signals from reaching your brain, offering relief for chronic pain without surgery or opioids.
Quick Facts About PNS:
- What it does: Sends gentle electrical signals to specific nerves to interrupt pain messages
- Treatment duration: Typically a 60-day temporary procedure
- Procedure time: About 20 minutes in an outpatient setting
- Recovery: Most patients feel relief within 1-2 days
- Invasiveness: Uses a needle puncture—no surgery required
- Best for: Chronic nerve pain, post-surgical pain, CRPS, and localized pain that hasn’t responded to other treatments
Chronic pain is one of the leading causes of disability worldwide. For years, managing persistent pain meant choosing between medications with unwanted side effects or invasive surgeries. Now, advances in neuromodulation technology offer a different path.
A 44-year-old patient who developed severe nerve pain after foot surgery found themselves unable to walk or stand comfortably. After trying physical therapy and medications without lasting relief, they turned to PNS—and experienced 90-100% pain relief, regaining the ability to perform daily activities.
PNS represents a breakthrough for people who’ve struggled to find relief. Unlike permanent implants or ongoing medications, this approach targets the specific nerves causing your pain. The device uses ultrasound guidance for precise placement, and because it’s temporary, you can try it without committing to a permanent solution.
The treatment emerged in the mid-1960s, but recent innovations in wireless technology and minimally invasive techniques have made it more accessible and effective than ever. For patients seeking alternatives to opioid pain medications—which contribute to nearly 42,000 deaths annually in the U.S.—PNS offers hope without the risks of addiction or systemic side effects.
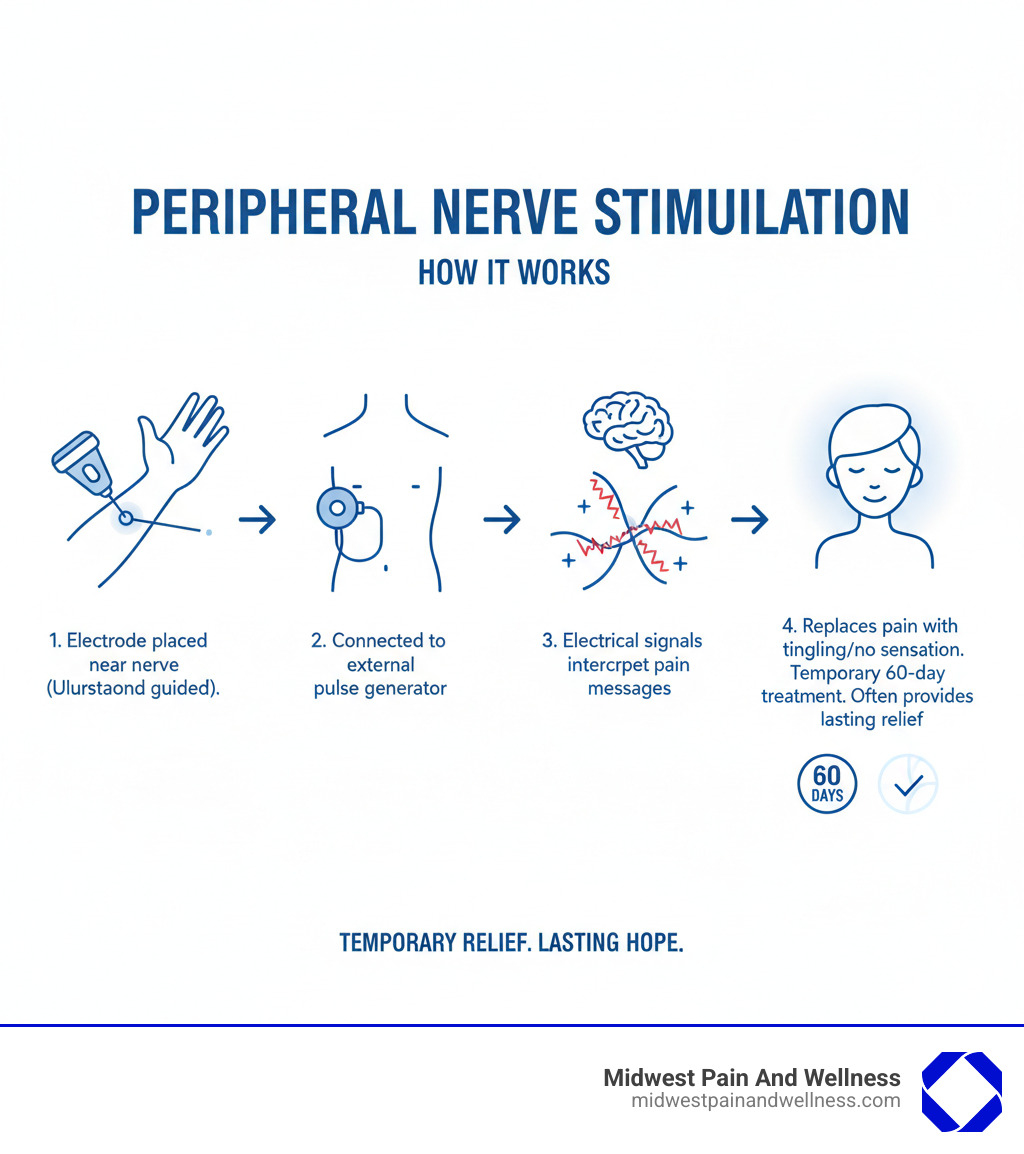
How Peripheral Nerve Stimulation Provides Targeted Pain Relief
Think of your nervous system as an elaborate alarm system. When you experience chronic pain, it’s like having a faulty alarm that won’t stop ringing—even when there’s no real emergency. Peripheral nerve stimulation works by intercepting those false alarms before they reach your brain’s control center.
Unlike treatments that mask pain with medication or require invasive surgery, PNS takes a different approach. It focuses on your peripheral nerves—the vast network of nerves branching throughout your body, outside your brain and spinal cord. By delivering gentle electrical pulses directly to these nerves, PNS modulates the pain signals right at their source.
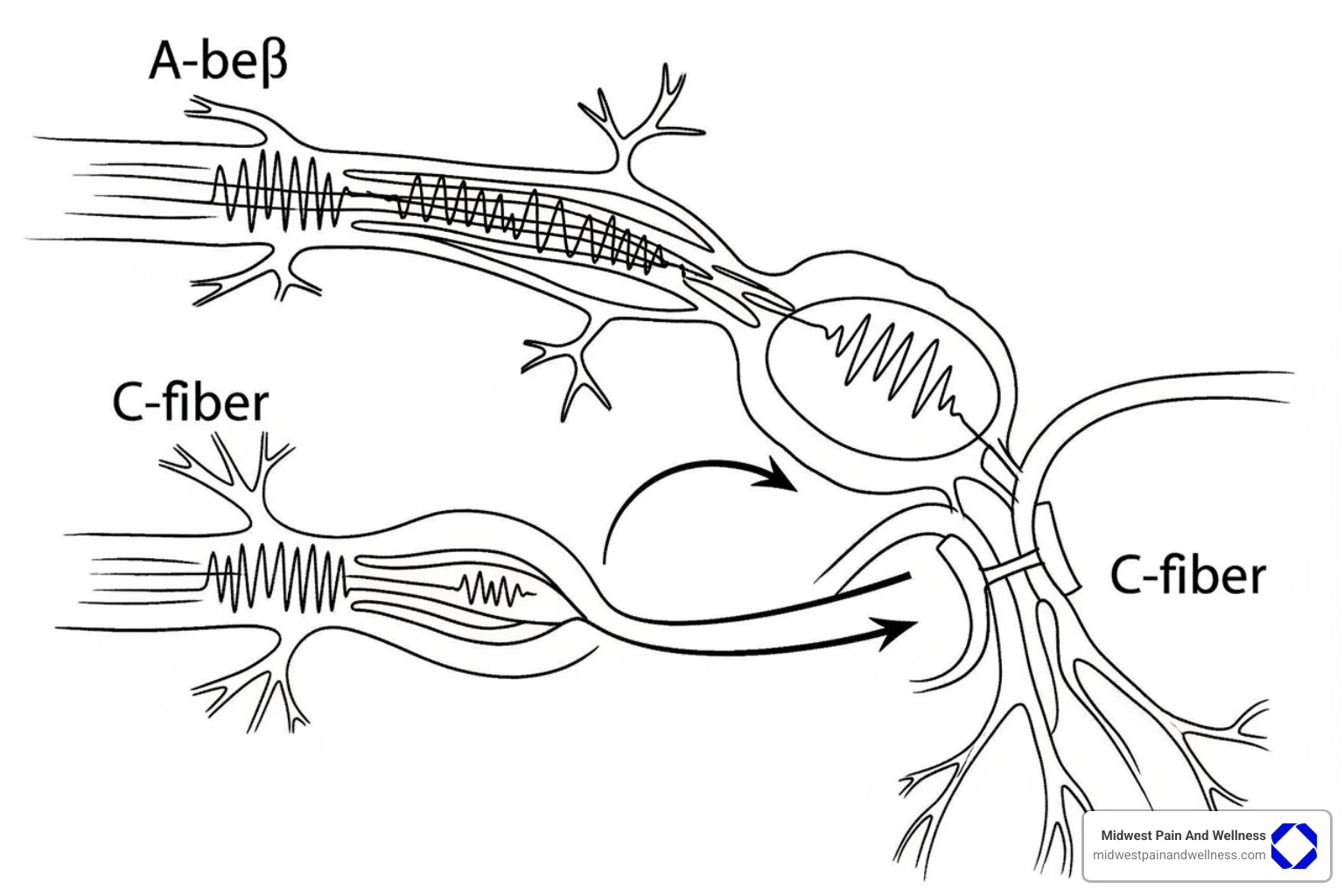
This is neuromodulation in action—using targeted electrical stimulation to change how your nerves communicate with your brain. The result? Many patients experience significant pain reduction without the need for ongoing medications or permanent implants.
The Science Behind How PNS Works
The magic of peripheral nerve stimulation lies in something called the Gate Control Theory of pain. Researchers Wall and Melzack introduced this concept back in 1965, and it remains the foundation for understanding how electrical nerve stimulation works today.
Picture a gate in your spinal cord that can swing open or closed. When it’s open, pain signals flood through to your brain. When it’s closed, those signals get blocked. PNS essentially helps close that gate.
Here’s what happens in your body: Pain signals typically travel along small, slow nerve fibers called C-fibers. These are the troublemakers sending distress signals to your brain. When a PNS device delivers mild electrical pulses to the affected nerve, it activates larger, faster nerve fibers called A-beta fibers. These larger fibers essentially rush ahead and close the gate in your spinal cord, preventing the slower pain signals from getting through.
The tingling sensation some patients feel—called paresthesia—was once considered essential for pain relief. Older systems aimed to create this gentle buzzing feeling that would “replace” the pain sensation. But modern PNS technology has evolved. Today’s sub-perception systems can block pain signals without creating any noticeable sensation at all. You get the relief without feeling the device working, which many patients find more comfortable and natural.
The science goes even deeper than the Gate Control Theory. Recent scientific research on PNS neurophysiological mechanisms shows that peripheral nerve stimulation also activates pathways to your brainstem, triggering your body’s natural pain-fighting systems. These include the noradrenergic, cholinergic, serotonergic, and dopaminergic systems—complex networks that influence not just pain perception, but also mood and cognitive function.
When PNS stimulates certain nerves, like the trigeminal or occipital nerves, it can activate the locus coeruleus—a small region in your brainstem involved in attention, arousal, and pain control. This means PNS doesn’t just block pain signals; it engages your body’s own mechanisms for managing pain more effectively.
Conditions Treated with Peripheral Nerve Stimulation
Peripheral nerve stimulation shines brightest for localized chronic pain—situations where we can identify specific nerves causing your discomfort. If you’ve tried conservative treatments without lasting success, PNS might offer the breakthrough you’ve been seeking.
The treatment has proven particularly effective for chronic neuropathic pain, where nerve damage causes burning, tingling, shooting, or stabbing sensations that can feel relentless. Research also shows that PNS successfully treats acute post-surgical pain, helping patients recover with minimal need for opioid medications.
For people living with post-amputation pain—whether phantom limb sensations or residual limb discomfort—PNS can provide meaningful relief. The same holds true for Complex Regional Pain Syndrome (CRPS), a challenging condition that causes severe pain, swelling, and skin changes, typically in an arm or leg.
The versatility of PNS extends to shoulder pain from conditions like subacromial impingement, chronic low back pain involving specific peripheral nerves in the lumbar region, knee pain following joint replacement, and foot pain from nerve injuries or diabetic neuropathy.
What makes PNS unique is its precision. We can target the exact nerve transmitting your pain signals, creating a truly personalized treatment. The occipital nerves help us address headaches and occipital neuralgia. The trigeminal nerves become targets for facial pain syndromes. The deep peroneal nerve treats foot pain, while genicular nerves address knee discomfort.
For upper extremity issues, we might focus on the median, ulnar, or radial nerves. Groin pain and meralgia paresthetica respond to stimulation of the ilioinguinal, iliohypogastric, or lateral femoral cutaneous nerves. Low back and buttock pain often improves when we target the cluneal nerves, while pudendal nerves help with pelvic pain.
Lower extremity neuropathies may benefit from targeting the femoral, sciatic, or obturator nerves. More widespread arm or leg pain might require addressing the brachial or lumbar plexus. We can even treat chest wall pain through intercostal nerves, sacroiliac joint pain through specific joint nerves, chronic low back pain via medial branches of the dorsal ramus, and post-stroke facial pain by targeting the gasserian ganglion.
This comprehensive approach means that wherever your pain originates, there’s likely a way to address it with targeted nerve stimulation. At Midwest Pain And Wellness, we carefully evaluate which nerves are involved in your specific condition, then create a customized treatment plan designed for your unique situation.
The PNS Procedure: A Patient’s Guide
Walking into a medical procedure can feel intimidating, especially when you’re dealing with chronic pain and hoping this will finally be the answer. At Midwest Pain And Wellness, we understand those feelings completely. That’s why we make sure you know exactly what to expect every step of the way during your peripheral nerve stimulation journey.
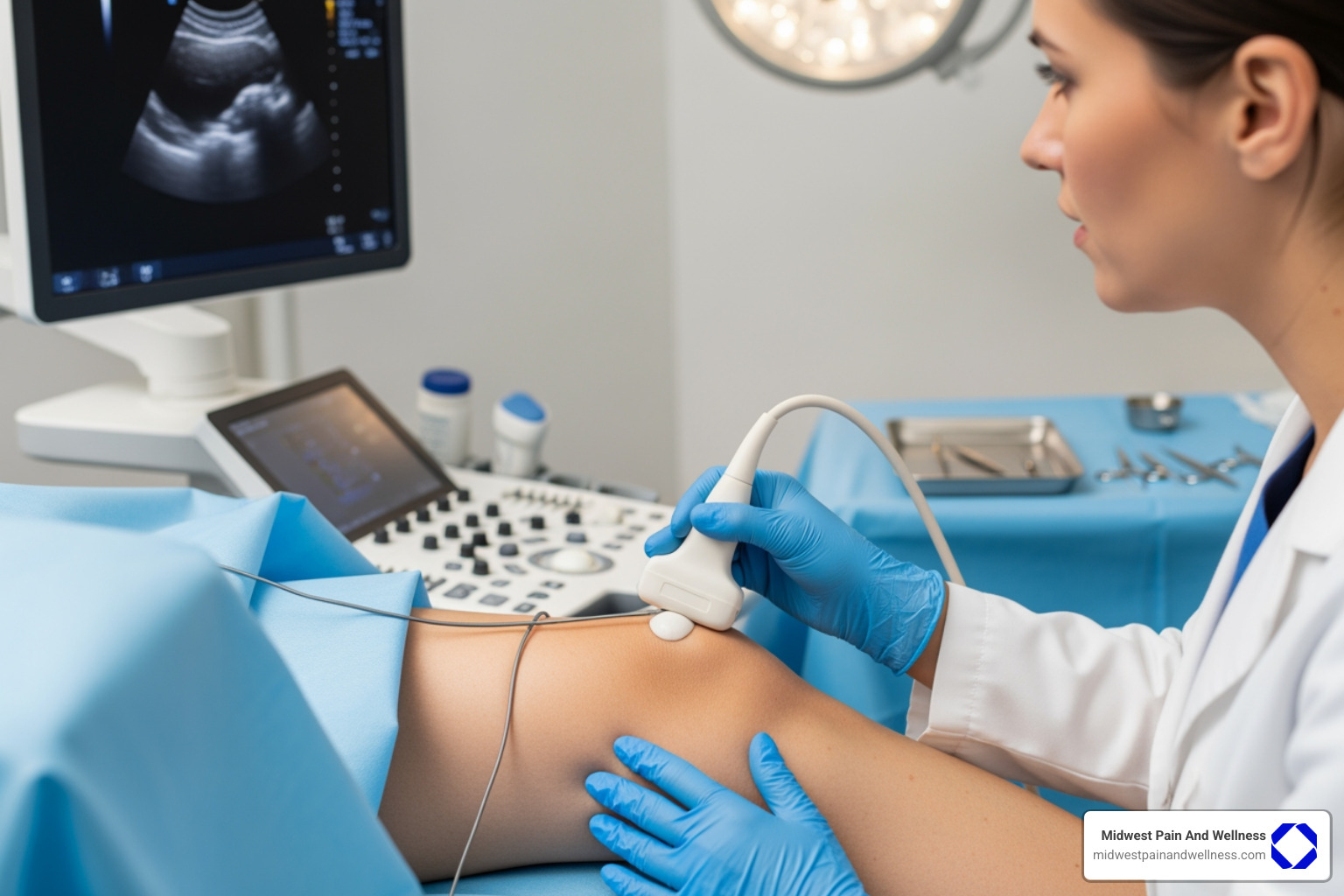
Are You an Ideal Candidate for PNS?
The truth is, PNS isn’t right for everyone—but when it’s the right fit, the results can be remarkable. Our double board-certified doctors take time to evaluate each patient carefully, looking at your complete pain story before recommending this treatment.
The best candidates for peripheral nerve stimulation typically share a few common experiences. You’ve probably already tried what we call conservative treatments—things like physical therapy, medications, and nerve blocks with local anesthetic and steroid injections. These approaches might have helped temporarily, but the relief didn’t last. If a nerve block gave you a few hours or days of blessed relief before the pain came roaring back, that’s actually a good sign that PNS might work for you.
Your pain also needs to follow a specific pattern. PNS works best when we can trace your discomfort to a particular peripheral nerve or nerve pathway. This is often neuropathic pain—that burning, shooting, or electric sensation that comes from nerve injury, post-surgical complications, or certain types of headaches. It’s the kind of pain that has a clear location and path, not a vague, all-over ache.
We’ll also look at your overall health picture. While a full psychological evaluation isn’t typically needed for temporary PNS devices, we do want to make sure there aren’t major psychological or psychiatric factors that might affect your recovery. We’re also checking for anything that would make the procedure unsafe, like allergies to the device components, bleeding disorders, or infections near where we’d place the lead.
Perhaps most importantly, we want to make sure you have realistic expectations. PNS can significantly reduce pain and improve your quality of life, but we’ll be honest with you about what it can and can’t do. Our comprehensive evaluation includes reviewing your medical history, performing a physical exam, and looking at any imaging studies to paint a complete picture of your condition.
The Implantation Process for Peripheral Nerve Stimulation
Here’s the good news: getting a PNS device is nothing like major surgery. The entire procedure is minimally invasive and happens right in our outpatient clinic. Most patients are surprised by how straightforward it is.
On the day of your procedure, we’ll start by numbing the area where the lead will be placed with local anesthesia. You’ll be awake or lightly sedated during the procedure, and that’s actually helpful—we need you to tell us what you’re feeling so we can position the electrode perfectly. Think of it as a collaboration between you and your doctor.
We use ultrasound imaging to see exactly where we’re going. This technology lets us identify your target nerve with precision and guide the electrode placement safely. Dr. Richard W. Rosenquist and other pain specialists have demonstrated how ultrasound guidance allows us to direct the stimulating needle right to nerves like the deep peroneal nerve, making the whole process much more accurate.
The actual placement happens through a needle puncture—not an incision. We insert a thin, wire-like electrode through this tiny opening and position it carefully next to the peripheral nerve that’s causing your pain. The whole process typically takes about 20 minutes, though it might feel longer when you’re lying there hoping for relief.
Once the electrode is in place, we’ll do a test run. We’ll turn on the stimulation and ask you to describe what you feel. Does it cover the painful area? Is the intensity right? This real-time feedback lets us make small adjustments to ensure the stimulation targets your pain effectively.
After we’ve confirmed optimal placement, we secure the lead with a sterile dressing and sometimes suture it to nearby tissue to keep it from shifting. The lead then connects to a small external pulse generator—about the size of a pager or small phone—that you’ll wear on your body for the treatment period.
No extensive incisions. No permanent hardware buried deep in your body. Just a targeted, reversible treatment that gets right to work.
Recovery and Aftercare
One of the most exciting aspects of peripheral nerve stimulation is how quickly many patients feel relief. We’re not talking weeks or months—some people notice significant improvement within a day or two.
Right after the procedure, the insertion site might feel a bit tender, similar to a minor bruise. That’s completely normal and should fade quickly. Before you head home, we’ll check your stimulation settings and make sure your bandage is secure and comfortable.
You’ll leave with a controller or a smartphone app that puts you in charge of the stimulation intensity. We’ll teach you how to use it, and you can adjust it as needed throughout the day. The external wires need to be kept safe—we’ll provide a sleeve to tuck them away and prevent any accidental tugging or dislodgement.
Life with the device requires a few precautions. The external components aren’t waterproof, so showering requires either removing the device or using the protective sleeve we provide. You’ll also want to avoid swimming or soaking in a pool or bath while the device is in place.
We don’t just send you home and wish you luck. Follow-up care is built into the process. You’ll come back within a week or two so we can check how the insertion site is healing and see how you’re responding to the treatment. We’ll have another appointment around the one or two-month mark to fine-tune your settings and make sure you’re getting the best possible pain relief.
After the 60-day treatment cycle, removing the lead is simple and happens right in our office. Here’s something remarkable: many patients continue experiencing pain relief long after the device comes out. That sustained relief often opens doors that pain had closed—returning to physical therapy, getting back to gardening, or simply being able to walk through a grocery store without wincing.
Throughout your recovery, our team at Midwest Pain And Wellness stays connected with you, adjusting your treatment as needed and celebrating the small victories that add up to a better quality of life.
Evaluating PNS: Benefits, Risks, and Alternatives
At Midwest Pain And Wellness, we believe in empowering our patients with all the information they need to make informed decisions about their pain management journey. Understanding both the advantages and potential drawbacks of peripheral nerve stimulation—and how it compares to other options—helps you choose the path that’s right for you.

Key Benefits of PNS Therapy
Peripheral nerve stimulation offers a compelling array of advantages, particularly for individuals who have exhausted other treatment avenues or are seeking non-opioid solutions. For many patients, PNS can provide substantial relief—often reporting 90-100% pain reduction. This can translate to a dramatic improvement in daily function and quality of life, allowing you to return to activities you thought were lost to pain.
One of the most significant benefits is the decreased need for opioids. In the face of the ongoing opioid crisis, PNS stands out as a non-pharmacological alternative. Research suggests that peripheral nerve stimulators can successfully treat post-operative and acute pain with minimal need for opioid pain medications. This is a crucial benefit, helping patients avoid the side effects and risks associated with long-term opioid use—including the very real danger of addiction.
By reducing pain, PNS enables patients to participate more actively in physical therapy and daily activities. This leads to improved physical function, increased mobility, and overall functional improvement. Imagine being able to garden again, play with your grandchildren, or simply walk through a grocery store without constant discomfort.
The procedure itself is minimally invasive and reversible. Unlike traditional surgery, it involves only a needle puncture. Furthermore, temporary PNS devices are fully removable, offering a trial period without the commitment of a permanent implant. This reversibility provides peace of mind—you can try the treatment and see how it works for your specific situation.
PNS also provides targeted relief by directly addressing the specific peripheral nerve causing pain. This precision is a major advantage over systemic medications that affect your entire body. The field of PNS is rapidly evolving, with advancements in indications, targets, and device designs expanding the opportunities for patients to find relief. A systematic literature review of PNS therapies highlights the growing body of evidence supporting its efficacy.
Potential Risks and Complications
While peripheral nerve stimulation is generally considered safe and low-risk, it’s important to be aware of potential complications, as with any medical procedure. Infections may occur in about 4 to 10% of cases. Our team uses stringent sterilizing techniques and precautions to minimize this risk. If an infection does occur, it may require antibiotic therapy, lead removal, or both.
The thin electrode lead could potentially migrate from its original position, break, or be misplaced during the initial procedure. This might reduce effectiveness or require repositioning. Some patients may experience skin irritation or dermatitis at the exit site for the external wires. While rare, some individuals may find the electrical sensations uncomfortable or intolerable, even with adjustable settings—this is called stimulation intolerance.
There’s a small risk of bleeding or hematoma (a collection of blood) at the insertion site, especially for patients on blood-thinning medications. We’ll discuss any such medications with you prior to the procedure. Long-term nerve damage is a very rare but serious complication. Our use of ultrasound guidance and careful technique significantly reduces this risk. Although rare, the device or its components could also malfunction.
We carefully discuss all potential risks and benefits with our patients, ensuring informed consent and a clear understanding of the procedure.
How PNS Compares to Other Pain Treatments
Understanding how peripheral nerve stimulation fits into the broader landscape of pain management can help you decide if it’s the right choice for you. PNS targets specific peripheral nerves—like those in your foot, elbow, or head—using a temporary system that lasts about 60 days. The procedure is minimally invasive, involving only percutaneous lead placement through a needle puncture.
Spinal cord stimulation (SCS), by contrast, targets the spinal cord itself at different levels—lumbar, thoracic, or cervical. It’s a permanent system that requires more moderate surgical implantation. While both use electrical stimulation to manage pain, SCS addresses pain at a different point in the nervous system and involves a longer-term commitment.
Nerve blocks offer another approach, providing short-term diagnostic or therapeutic relief lasting just hours to days. These injections target specific nerves, individual muscles, or groups of nerves, and they’re minimally invasive like PNS. However, their brief duration makes them better suited for diagnosis or temporary relief rather than long-term management.
Oral medications, including opioids, anti-inflammatories, and nerve pain medications, work throughout your entire body systemically. While they can be effective, they often come with side effects and, in the case of opioids, carry risks of dependency and addiction. Unlike PNS, which provides localized relief, medications affect your whole system—and they require ongoing use to maintain their effect.
Each approach has its place in comprehensive pain management. At Midwest Pain And Wellness, our double board-certified doctors work with you to determine which treatment—or combination of treatments—will provide the best long-term relief for your specific situation.