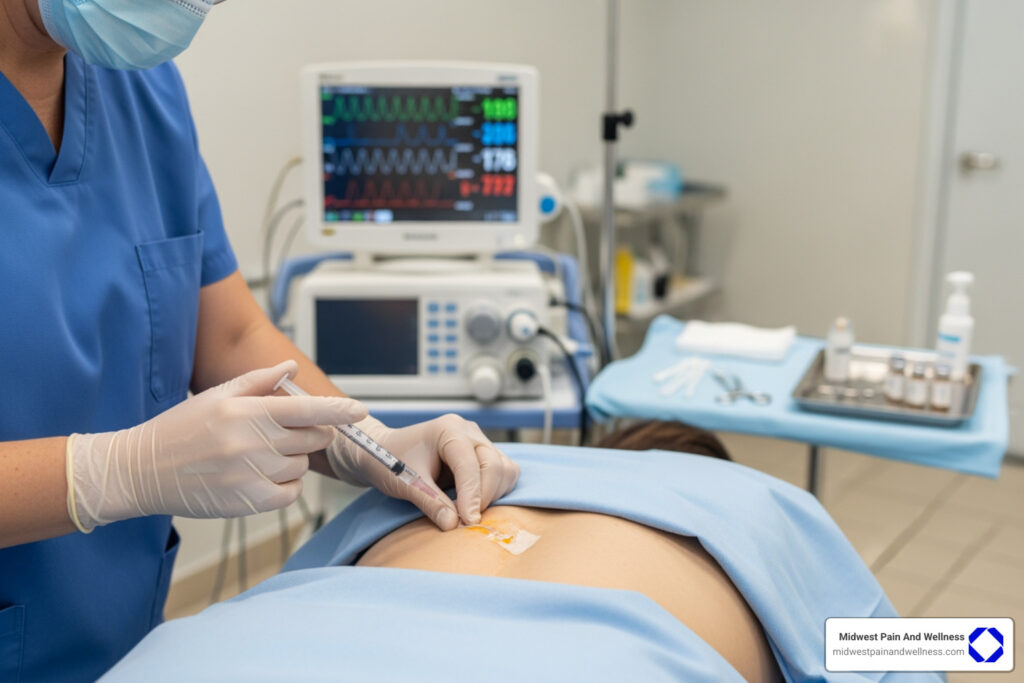
Understanding Your Options for Piriformis Syndrome Relief
Piriformis syndrome treatment ranges from simple lifestyle changes to advanced injections and, in rare cases, surgery. Most people find relief with conservative care, including physical therapy, targeted stretches, and anti-inflammatory medications. For persistent pain, corticosteroid injections provide relief for about 73% of patients, though symptoms may return. Surgery is reserved for severe cases unresponsive to other treatments after six months.
Quick Treatment Overview:
- First-line options: Rest, ice/heat therapy, NSAIDs, piriformis stretches
- Physical therapy: Targeted stretching, manual therapy, strengthening exercises
- Injections: Corticosteroid injections (~73% pain relief), botulinum toxin
- Alternative therapies: Acupuncture, dry needling, TENS therapy
- Surgery: Endoscopic release (considered only after conservative treatments fail)
Piriformis syndrome occurs when the piriformis muscle, located deep in the buttock, compresses the sciatic nerve. This causes pain, tingling, and numbness radiating down the back of the leg. The condition accounts for approximately 0.3% to 6% of all lower back pain cases but is often misdiagnosed because it mimics other issues, like sciatica from a herniated disc.
An accurate diagnosis is crucial for effective treatment. With the right approach, most people experience significant improvement, whether the pain stems from prolonged sitting, athletic overuse, or trauma. The key is finding the right combination of treatments for your specific needs.

Understanding Piriformis Syndrome: Causes, Symptoms, and Diagnosis
Before exploring treatments, it’s helpful to understand what piriformis syndrome is. The piriformis is a small, pear-shaped muscle deep in your buttock that helps rotate your leg and stabilize your hip. When it tightens, spasms, or swells, it can compress the nearby sciatic nerve—the body’s largest nerve—causing pain, tingling, and numbness.
Primary Causes and Risk Factors
Piriformis syndrome can develop gradually or appear after a specific event. Understanding the trigger helps guide an effective piriformis syndrome treatment plan.
- Muscle Spasm: Overuse, injury, or prolonged sitting can cause the piriformis to contract and stay tight, putting pressure on the sciatic nerve.
- Overuse from Repetitive Motion: Athletes, especially runners and cyclists, are at higher risk due to repetitive movements that can inflame or enlarge the muscle.
- Trauma or Injury: A fall, car accident, or direct blow to the buttock can cause swelling or scar tissue that irritates the nerve.
- Anatomical Variations: In about 15-20% of people, the sciatic nerve passes through the piriformis muscle instead of beneath it, increasing the risk of compression.
- Prolonged Sitting: Constant pressure from sitting at a desk or driving can irritate the piriformis and sciatic nerve. Carrying a thick wallet in a back pocket (“wallet neuritis”) can have the same effect.
- Other Factors: Improper lifting techniques, poor spinal alignment, leg-length discrepancies, and foot problems can also contribute by altering your gait and mechanics.
Research shows that piriformis syndrome is often overlooked because it mimics other conditions. An accurate diagnosis is the first step toward relief. You can read more about these diagnostic challenges in scientific research.
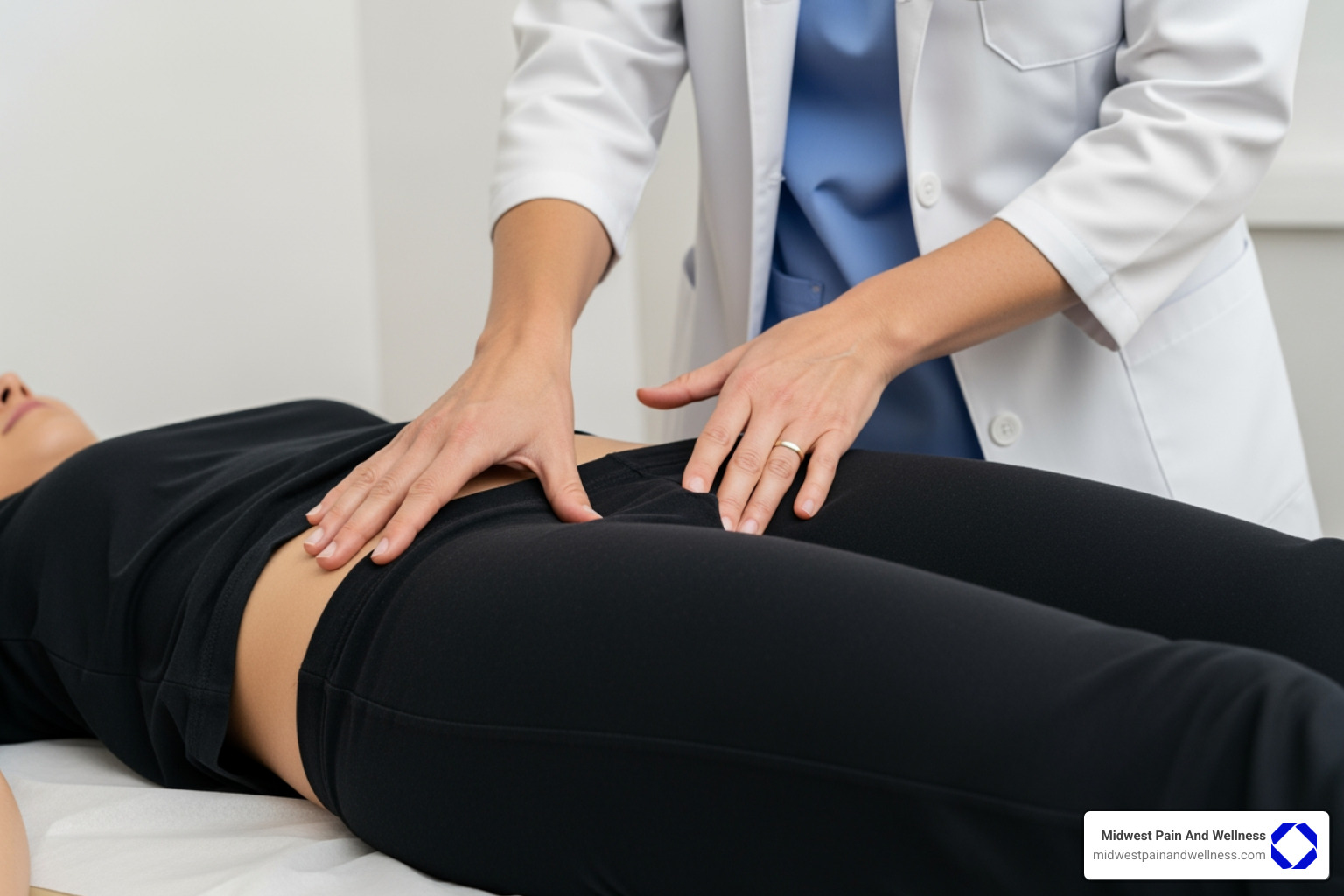
How is Piriformis Syndrome Diagnosed?
There is no single definitive test for piriformis syndrome. It is a “diagnosis of exclusion,” meaning other potential causes for your symptoms must be ruled out first. This is why working with experienced pain management specialists at Midwest Pain And Wellness is so important.
The diagnostic process includes:
- Patient History: We discuss your symptoms, when they started, what they feel like, and what activities make them better or worse.
- Physical Examination: We perform specific “provocative tests” to reproduce your symptoms. The FAIR test (Flexion, Adduction, and Internal Rotation) and the Beatty maneuver are common tests that, if positive, strongly indicate piriformis involvement.
- Excluding Other Conditions: We must rule out issues like a herniated disc, spinal stenosis, or hip bursitis. Imaging is key for this step.
- Imaging Scans: An MRI helps visualize soft tissues and rule out spinal issues, while a CT scan details bone structures. Ultrasound provides real-time images of the muscle and nerve, and is especially useful for guiding injections.
- Advanced Diagnostics: Magnetic Resonance Neurography (MRN) offers specialized views of nerve inflammation. Electrodiagnostic tests (like EMG) assess nerve function to pinpoint the location of compression.
A thorough diagnosis ensures your piriformis syndrome treatment plan addresses the true source of your pain.
Piriformis Syndrome vs. Sciatica: What’s the Difference?
Many patients ask if they have piriformis syndrome or sciatica. Both involve sciatic nerve irritation, but the location of the problem is different.
True sciatica (lumbar radiculopathy) originates in the lower spine, where nerve roots are compressed by a herniated disc, spinal stenosis, or arthritis. The pain often starts in the lower back and radiates down the leg, worsened by bending, twisting, or coughing.
Piriformis syndrome involves nerve compression in the buttock, where the piriformis muscle squeezes the sciatic nerve. The pain is typically felt deep in the buttock and is aggravated by prolonged sitting, climbing stairs, or hip rotation.
Healthcare professionals may use the broader term “deep gluteal syndrome” to describe any non-spinal sciatic nerve entrapment in this region. Misdiagnosis is common, leading to ineffective treatment. A comprehensive evaluation is essential to differentiate these conditions and target the actual source of pain.
| Feature | Piriformis Syndrome | Lumbar Radiculopathy (Sciatica) |
|---|---|---|
| Primary Cause | Compression of the sciatic nerve by the piriformis muscle | Compression of sciatic nerve roots in the lumbar spine |
| Source of Pain | Deep in the buttock | Lower back, radiating down the leg to the foot |
| Where Compression Occurs | Outside the spinal canal (in the gluteal region) | Inside or near the spinal canal |
| What Makes It Worse | Prolonged sitting, climbing stairs, hip rotation movements | Bending, twisting, coughing, sneezing, prolonged standing |
| Imaging Findings | MRI/CT often normal; may show piriformis muscle changes | MRI/CT typically shows disc herniation or spinal stenosis |
| Diagnosis Approach | Often diagnosis of exclusion; part of deep gluteal syndrome | Confirmed by imaging showing spinal pathology |
Understanding these differences is the foundation of effective piriformis syndrome treatment.
Conservative and Non-Surgical Piriformis Syndrome Treatment
Most people with piriformis syndrome find significant relief without surgery. At Midwest Pain And Wellness, we prioritize conservative, opioid-free approaches that target the root cause of your pain. Our multi-modal strategy combines proven therapies into a customized plan to provide lasting relief.
Lifestyle Modifications
Simple changes in your daily routine can make a big impact:
- Activity Modification: Take frequent breaks from prolonged sitting (every 20-30 minutes) to stand, walk, or stretch.
- Avoid “Wallet Neuritis”: Move your wallet from your back pocket to a front pocket or jacket to prevent uneven pressure on the piriformis muscle.
- Balanced Rest: During acute flare-ups, rest from aggravating activities for up to 48 hours. Avoid prolonged inactivity, which can weaken muscles.
- Proper Posture and Lifting: Maintain good posture while sitting and standing. When lifting, bend your knees and keep your back straight.
- Warm-ups and Footwear: Always warm up before exercise. If you have a leg-length discrepancy or foot issues, supportive shoes or orthotics can help.
- Ice and Heat Therapy: Use ice packs for acute pain to reduce inflammation and heat packs to relax tight muscles.
Physical Therapy and Stretches
Physical therapy is a cornerstone of effective piriformis syndrome treatment. A therapist will create a personalized program to stretch the piriformis, strengthen surrounding muscles, and correct biomechanical imbalances.
- Piriformis Stretches: Key stretches include the supine knee-to-chest stretch, the seated piriformis stretch, and standing variations. Each stretch should be held for 20-30 seconds without sharp pain.
- Strengthening Exercises: Strengthening the hip abductors and gluteal muscles helps stabilize the pelvis and reduces strain on the piriformis.
- Range of Motion and Manual Therapy: Exercises to improve hip mobility, combined with hands-on techniques like soft-tissue massage and myofascial release, can relax tight muscles and provide immediate relief.
- Osteopathic Manipulative Treatment (OMT): Our osteopathic physicians use OMT to address musculoskeletal imbalances throughout the body, helping to relieve pain and restore function. Learn more in A guide to Osteopathic Manipulative Treatment.
Medications and Injections for Piriformis Syndrome Treatment
When other conservative measures aren’t enough, medications and injections can help manage pain and inflammation.
- Oral Medications: Over-the-counter NSAIDs (ibuprofen, naproxen) can reduce pain and inflammation. For persistent muscle spasms, prescription muscle relaxants may be used. Nerve-related pain can sometimes be managed with anticonvulsant medications. We prioritize opioid-free strategies for long-term wellness.
- Corticosteroid Injections: For severe pain, an injection of corticosteroid and local anesthetic directly into the piriformis muscle can be effective. Research shows about 73% of patients experience significant pain relief. However, relief can be temporary, with about 50% of patients reporting pain recurrence after five weeks. Injections are best used to enable more effective participation in physical therapy.
- Advanced Injections: Local anesthetic injections can break the pain-spasm cycle. Another technique, sciatic perineural hydrodissection, uses fluid to free the nerve from surrounding tissue. One study showed 84% of patients had immediate pain relief from this method. We use ultrasound guidance for precise placement.
Alternative Therapies for Pain Relief
Our multi-modal approach to piriformis syndrome treatment may include alternative therapies to complement traditional methods.
- Acupuncture: This ancient practice involves inserting thin needles into specific points to reduce muscle spasm and pain.
- Ultrasound-Guided Dry Needling: Thin needles are inserted into painful trigger points within the piriformis muscle to stimulate relaxation and healing, with ultrasound ensuring precision.
- TENS Therapy: A TENS (Transcutaneous Electrical Nerve Stimulation) unit uses a low-voltage electrical current to block pain signals and stimulate endorphin release.
- Botox Injections: Botulinum toxin can be injected into the piriformis muscle to temporarily paralyze it, forcing it to relax and relieving pressure on the sciatic nerve. Effects typically last several months.
- Regenerative Therapies: Prolotherapy involves injecting a mild irritant solution to promote tissue regeneration and strengthen weakened ligaments. Platelet-Rich Plasma (PRP) therapy uses a concentration of your own blood platelets to stimulate tissue repair in chronically injured areas.
Surgical Options for Refractory Piriformis Syndrome
Surgery is a last resort for piriformis syndrome, considered only after other treatments have failed. At Midwest Pain And Wellness, we exhaust all conservative options before recommending a surgical procedure.
Surgery is typically reserved for patients with debilitating pain that has persisted for at least six months despite comprehensive non-surgical care. The primary goal is to decompress the sciatic nerve by relieving pressure from the piriformis muscle.
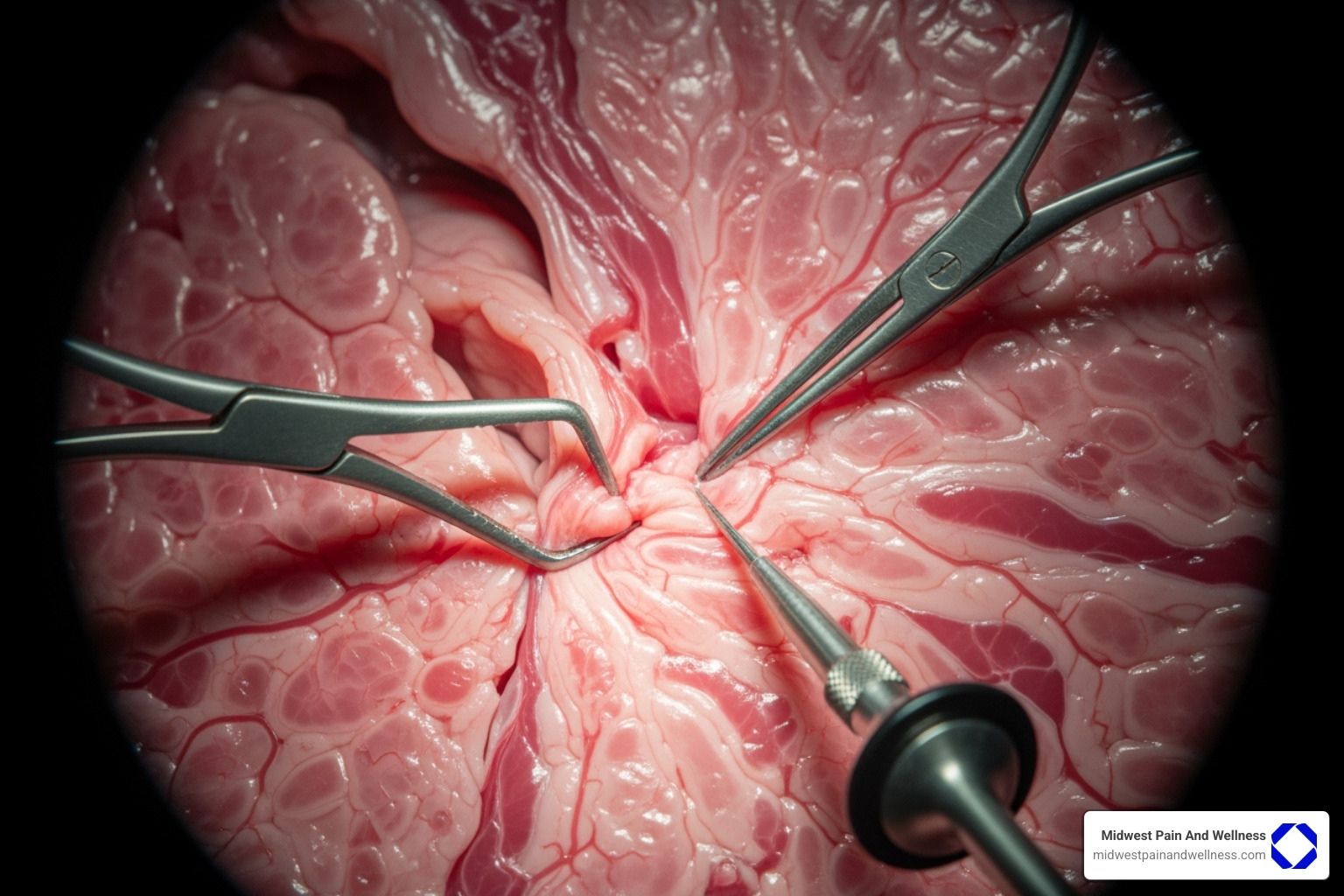
Surgical Piriformis Syndrome Treatment Approaches
Several surgical techniques can address piriformis syndrome:
- Open Piriformis Tendon Release: This traditional approach involves a larger incision to directly view and release the piriformis tendon, reducing tension on the sciatic nerve.
- Endoscopic Piriformis Release: This modern, minimally invasive technique uses a camera and small incisions for a precise release of the muscle. Research shows endoscopic release has a high success rate and lower complication rates than open surgery.
- Sciatic Neurolysis: Performed alone or with a tendon release, this procedure involves carefully removing scar tissue or adhesions from around the sciatic nerve to free it from impingement.
Potential Complications and Prognosis
As with any surgery, risks include nerve damage, infection, and bleeding (hematoma). These are uncommon with modern techniques.
Outcomes for carefully selected patients are positive. One study on piriformis release with sciatic neurolysis found that 11 of 14 patients achieved excellent outcomes, with 4 reporting good results.
Recovery requires commitment, typically involving several months of physical therapy to regain strength and function. Rehabilitation is as crucial as the surgery itself for a successful outcome.
Frequently Asked Questions about Piriformis Syndrome Treatment
Living with piriformis syndrome raises many questions. Here are answers to the most common concerns we hear from patients at Midwest Pain And Wellness.
How long does it take to recover from piriformis syndrome?
Recovery time varies depending on the severity of your condition and your chosen treatment plan.
- With conservative treatment like physical therapy and lifestyle changes, most people see improvement within a few weeks to a few months. Consistency is key to preventing symptoms from returning.
- After injections, relief is often faster but may be temporary. The average duration of relief from local anesthetic and steroid injections is about 5.3 weeks. Injections can serve as a bridge to allow for more effective physical therapy.
- Surgical recovery is the longest, requiring several months of dedicated physical therapy to restore strength and function.
Recovery is not always a straight line, but with a consistent piriformis syndrome treatment plan, improvement is achievable.
Can piriformis syndrome go away on its own?
In some mild cases, yes. Spontaneous resolution can occur if the aggravating factor is quickly identified and removed. A study of 65 patients found that 41 had complete resolution either spontaneously or with basic conservative care within 35 days.
However, most people require an active approach. Waiting for the pain to disappear often fails to address the underlying muscle imbalances or lifestyle factors, leading to recurring flare-ups. Committing to a comprehensive treatment plan is the most reliable path to lasting relief.
What should I avoid if I have piriformis syndrome?
Avoiding certain activities and habits is crucial for managing piriformis syndrome and preventing setbacks.
- Prolonged Sitting: This is a primary aggravator. Stand, walk, or stretch every 20-30 minutes to reduce pressure on the piriformis muscle.
- Sitting on a Wallet: Carrying a thick wallet in your back pocket creates direct pressure on the muscle and nerve. This habit, known as “wallet neuritis,” is a common cause of symptoms. Move your wallet to a front pocket.
- High-Impact Activities: Temporarily scale back activities like long-distance running or jumping. Consider lower-impact alternatives like swimming or cycling during recovery.
- Repetitive Leg Movements: Be mindful of exercises that involve external hip rotation or moving your leg away from your body against resistance, as these directly stress the piriformis.
- Improper Lifting: Always lift with your knees, not your back, to avoid straining your gluteal muscles.
- Personal Pain Triggers: Pay attention to any activity that consistently worsens your pain, such as climbing stairs or certain yoga poses, and modify or avoid them as you heal.
Your Path to Relief from Piriformis Syndrome
Living with piriformis syndrome can be frustrating, but you don’t have to steer it alone. At Midwest Pain And Wellness, we are here to help you find a path to lasting relief.
We believe in a thoughtful, step-by-step piriformis syndrome treatment plan custom to your needs. Our progression is:
- Conservative Care: We start with lifestyle modifications, physical therapy, and anti-inflammatory medications.
- Targeted Injections: If needed, we use precise, image-guided injections to reduce inflammation and pain.
- Advanced Therapies: We may integrate acupuncture, dry needling, or botulinum toxin injections for additional support.
- Surgical Referral: Surgery is a final option, considered only after at least six months of comprehensive conservative treatment have not provided relief.
An accurate diagnosis is the foundation of effective treatment. Because piriformis syndrome often mimics other conditions, our double board-certified doctors perform a thorough evaluation to ensure we are treating the right problem. Our commitment is to comprehensive, opioid-free pain management. We use a multi-modal, interventional approach, collaborating with other specialists to create a custom care plan focused on your long-term wellness.
Located in Chicago Ridge, Illinois, we are dedicated to helping you reclaim your quality of life. Let us help you get back to the activities you love, without pain.