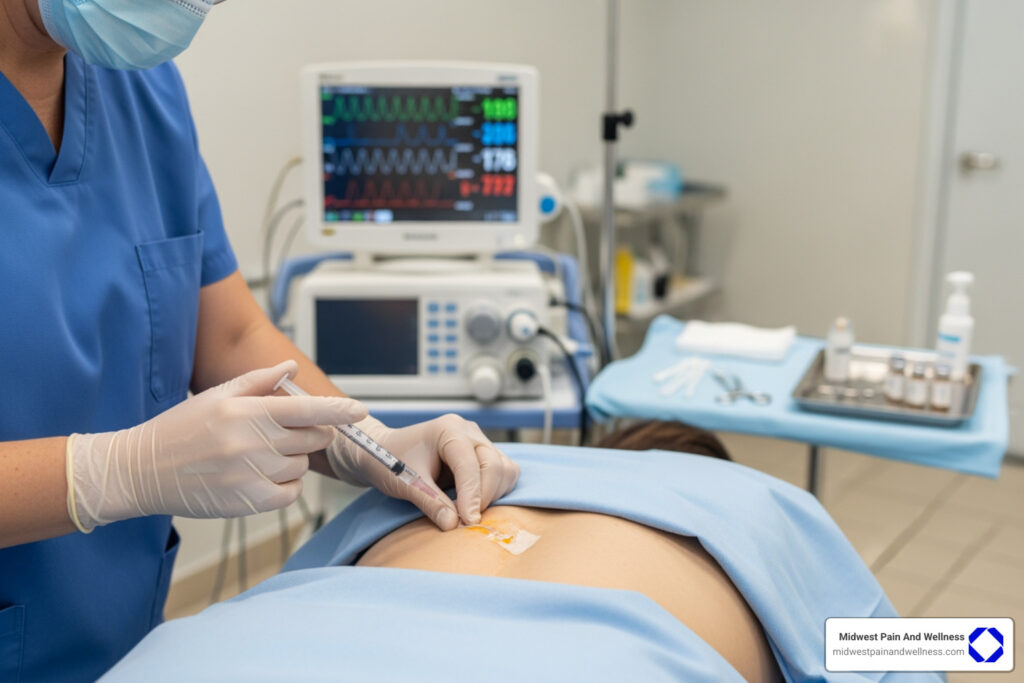
Understanding the Science Behind Platelet-Rich Plasma
How does PRP work? PRP therapy concentrates your body’s platelets and injects them into an injured area to trigger natural healing. When activated, these platelets release growth factors that drive the repair process through three distinct stages:
- Inflammatory Phase (Days 1-7): Platelets recruit immune cells and release initial growth factors.
- Proliferation Phase (Days 5-20): Growth factors stimulate the production of fibroblasts and stem cells.
- Remodeling Phase (Months 3-6): New collagen and tissue form to repair the damage.
PRP typically contains 3 to 7 times the concentration of platelets found in normal blood. This surge “jump starts” the body’s repair cascade, accelerating regeneration at the cellular level. For patients at Midwest Pain And Wellness seeking alternatives to surgery or long-term medication, PRP offers a promising regenerative approach.
As Dr. Yaw Donkoh, a double board-certified physician, I have seen how PRP helps patients find relief through minimally invasive treatments. My focus is on outcomes-based care, helping you understand how these biological therapies can restore your quality of life.
What is Platelet-Rich Plasma (PRP)?
Platelet-Rich Plasma (PRP) is a natural healing solution derived from your own blood. To understand PRP, we look at the four primary components of blood: red cells, white cells, plasma, and platelets. Plasma is the liquid vehicle, while platelets (thrombocytes) are cell fragments responsible for clotting and tissue repair. They contain “growth factors”—the body’s natural repair crew.
PRP is simply blood with a much higher concentration of these platelets. By concentrating them, we create a potent solution that accelerates healing when introduced to a damaged area. This leverages the body’s own biological mechanisms to repair tissue. For a deeper dive into the science, you can explore scientific research on PRP biology.
How does PRP work at a cellular level?
When PRP is injected, platelets undergo degranulation, releasing stored growth factors. These factors bind to receptors on target cells, signaling them to initiate repair. Key activities include:
- Cell Reproduction (Mitogenesis): Stimulating the creation of new cells to replace damaged ones.
- Tissue Regeneration: Initiating the formation of new host tissue for tendons, ligaments, and cartilage.
- Stimulating Reparative Cells: Activating mesenchymal stem cells to differentiate into fibroblasts (collagen producers) or chondrocytes (cartilage cells).
The role of platelet concentration
The effectiveness of PRP is linked to platelet density. While normal blood has a baseline level, PRP amplifies this by 300% to 700%. At Midwest Pain And Wellness in Chicago Ridge, we aim for at least a 7x concentration for optimal results. This high density ensures a robust release of healing compounds, leading to quicker growth of new bone and soft tissue.
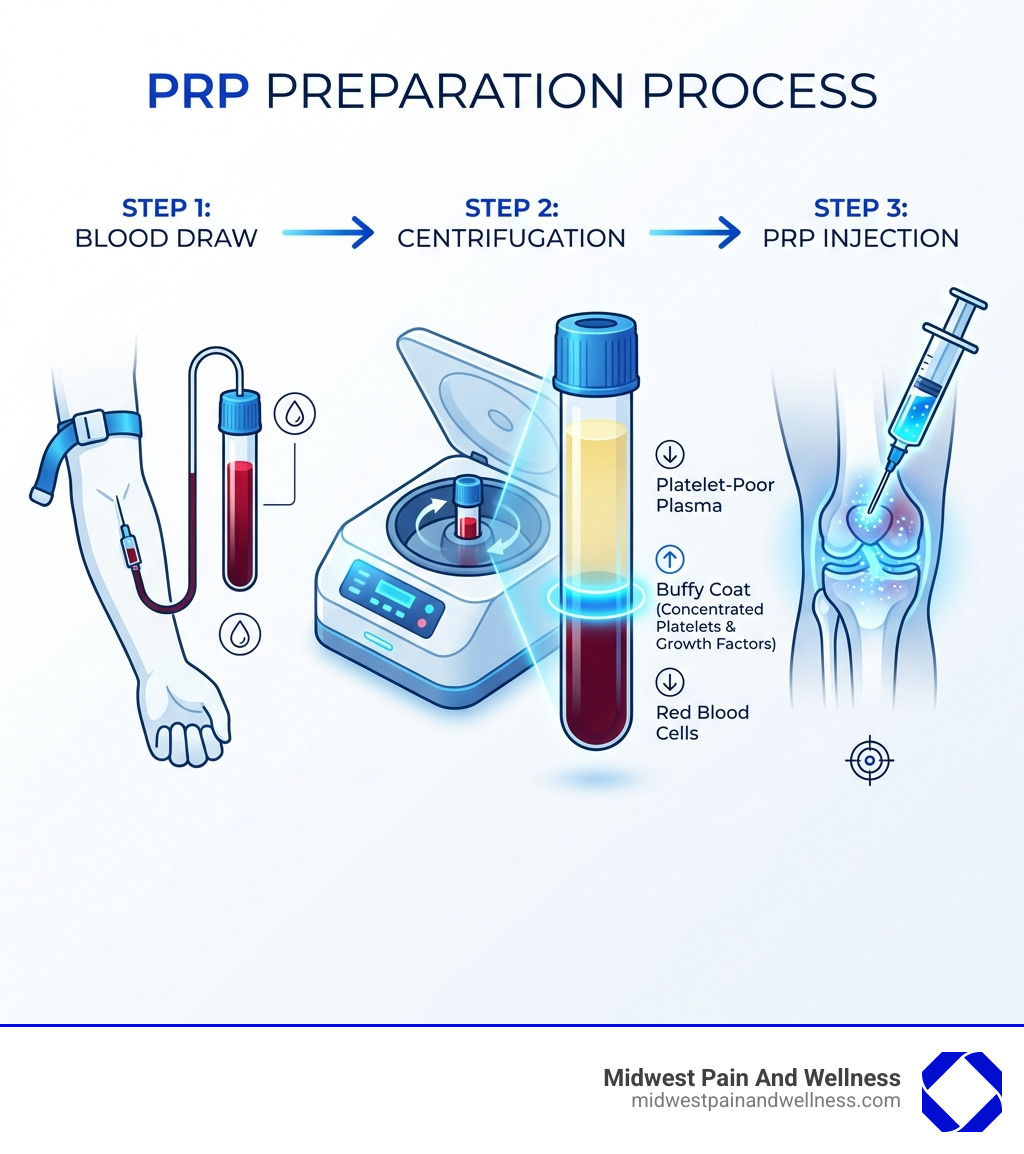
The Step-by-Step Process: How is PRP Prepared?
Preparing PRP is a precise process involving a routine blood draw of 30 to 60 milliliters. Because the blood is autologous (your own), there is no risk of rejection. The sample is placed in a centrifuge to separate components based on density.
How does PRP work to concentrate platelets?
The centrifuge spins the blood to create three layers:
- Platelet-Poor Plasma (PPP): The lightest top layer.
- Buffy Coat: The middle layer rich in platelets and white blood cells.
- Red Blood Cells: The heaviest layer at the bottom.
At Midwest Pain And Wellness, we often use a “double-spin” technique. This further refines the buffy coat, maximizing platelet count while removing unnecessary red cells. This ensures the final solution is packed with the highest possible concentration of healing factors.
Activation of the PRP solution
In some cases, PRP is “activated” just before injection to trigger immediate growth factor release. This can be done using Calcium Chloride or Autologous Human Thrombin. However, platelets also activate naturally upon contact with collagen in the injured tissue. Your clinician will determine the best method based on your specific needs and safety.
The Biological Mechanism: How Does PRP Work?
Injecting PRP jump-starts the body’s natural repair process by delivering a high concentration of growth factors directly to the injury. This initiates a complex healing cascade. For a detailed overview, you can refer to a review of PRP mechanism of action.
Key growth factors include:
- PDGF: Stimulates cell division and new blood vessel formation.
- TGF-β: Promotes long-term healing and bone modeling.
- VEGF: Essential for angiogenesis (new blood vessel growth).
- EGF: Stimulates cell proliferation and differentiation.
The Three Phases of Healing
- Inflammatory Phase (Days 1-7): The initial response where platelets recruit immune cells. This may cause temporary minor discomfort or swelling, which are signs that healing has begun.
- Proliferation Phase (Days 5-20): Growth factors stimulate fibroblasts and stem cells to rebuild damaged tissue.
- Remodeling Phase (Months 3-6+): New collagen matures and strengthens, restoring function and providing long-term relief.
Stimulating New Cell Production
PRP acts as a biological signal for the body’s regenerative machinery. It specifically promotes the activity of:
- Fibroblasts: Responsible for collagen synthesis in tendons and ligaments.
- Mesenchymal Stem Cells: Versatile cells that can become bone, cartilage, or muscle cells.
- Chondrocytes: Essential for maintaining and repairing articular cartilage in joints.
Angiogenesis and Blood Vessel Formation
PRP promotes angiogenesis via VEGF. New blood vessels improve nutrient delivery and waste removal at the injury site, ensuring that regenerating tissues have the oxygen and support needed to thrive.
Clinical Applications and Healing Potential
PRP therapy is highly effective for many musculoskeletal conditions because it delivers a concentrated dose of your body’s own signaling proteins directly to tissue that has become irritated, strained, or slow to heal. At Midwest Pain And Wellness in Chicago Ridge, our goal is to reduce pain while improving function, using regenerative options when appropriate and combining them with a complete, outcomes-based plan.
At Midwest Pain And Wellness in Chicago Ridge, we use PRP for:
- Chronic Tendinopathy: Tennis elbow, Achilles tendinitis, and patellar tendinopathy.
- Osteoarthritis: Reducing pain and stiffness in mild to moderate knee arthritis.
- Acute Injuries: Sprains and muscle pulls.
- Post-Surgical Healing: Accelerating recovery after ligament or tendon repairs.
PRP is not an instant numbing medication. Instead, it works with your body’s timeline. Many patients notice that pain and stiffness gradually improve as the proliferation and remodeling phases progress. Because every case is different, your clinician will consider the specific tissue involved (tendon vs. joint cartilage), the chronicity of the injury, and your activity goals when recommending PRP.
Comparison: PRP vs. Cortisone Injections
Unlike cortisone, which primarily reduces inflammation and can weaken tissue when repeated, PRP is designed to support healing and strengthen the area over time. This is one reason PRP is often considered for chronic tendon problems or joint degeneration where tissue quality matters.
| Feature | PRP Therapy | Cortisone Injections |
|---|---|---|
| Primary Goal | Tissue regeneration and healing | Inflammation and pain reduction |
| Long-term Effect | Strengthens tissue | May weaken tissue over time |
| Onset of Relief | Gradual (weeks to months) | Rapid (days) |
| Duration | Often 1-2 years or more | Temporary (weeks to months) |
A practical way to think about the difference is that cortisone can be helpful when rapid symptom control is needed, while PRP may be better suited for patients who want a longer-term, restorative strategy. Your provider will also consider factors like your medical history, the number of prior steroid injections, and imaging findings.
What outcomes can you realistically expect?
Results vary by condition and severity, but common goals include:
- Less pain with activity: such as walking, climbing stairs, gripping, or returning to sport.
- Improved mobility and endurance: reduced stiffness and improved tolerance for daily tasks.
- Better tissue resilience: especially in tendons and ligaments that are repeatedly stressed.
In many cases, PRP is most effective when paired with a structured rehab plan. Targeted physical therapy can progressively load the healing tissue (for example, eccentric tendon exercises), helping translate biological healing into real-world strength and stability.
Soft Tissue and Bone Regeneration
PRP can improve tissue strength by up to 40% compared to natural healing. In dentistry and oral surgery, it is used to improve bone grafts and speed recovery after extractions.
In orthopedic and sports medicine settings, PRP is often chosen because tendons and ligaments have limited blood supply, which can make them slow to recover. By enhancing local growth factor signaling and supporting collagen production, PRP may help these tissues heal more effectively. For joint conditions like knee osteoarthritis, PRP is generally used to decrease pain and improve function in mild to moderate cases, with benefits that may last longer than short-acting anti-inflammatory options for some patients.
Cosmetic and Specialized Uses
PRP is also used for hair loss (male pattern baldness) to stimulate follicles and in facial rejuvenation to improve skin texture through collagen stimulation.
For patients considering PRP for hair or skin concerns, it is still the same core concept: concentrating platelets to deliver growth factors that signal repair and regeneration. Treatment plans can differ depending on goals, and your clinician can help you understand what is realistic based on current evidence and your individual situation.
Frequently Asked Questions about PRP Therapy
Is PRP therapy safe?
Yes. Because PRP uses your own blood, the risk of allergic reaction or disease transmission is virtually zero. Common side effects include temporary soreness or swelling at the injection site.
That said, PRP is still a medical procedure. Safety depends on appropriate patient selection, sterile technique, and proper imaging guidance when indicated. We screen patients for blood disorders or anticoagulation therapy to ensure they are suitable candidates.
Who is a good candidate (and who should be cautious)?
PRP may be a good option if you have a tendon, ligament, or joint problem that has not improved with conservative care and you want to avoid surgery or long-term medication when possible.
You may need extra caution or a different approach if you:
- Have a known platelet or bleeding disorder
- Are taking medications that significantly affect clotting (your prescribing clinician may need to advise on whether adjustments are safe)
- Have an active infection or significant systemic illness
Your provider will review your medical history to decide whether PRP is appropriate and safe.
How long does it take to see results?
While the healing cascade starts immediately, visible results usually take a few weeks. Full tissue remodeling typically occurs over 3 to 6 months. The benefits can last a year or longer as the body continues to repair itself.
It is also normal to have a short period of increased soreness after the injection, especially in the first several days, as the inflammatory phase begins.
How many treatments are typically required?
Most musculoskeletal conditions require 1 to 2 injections spaced 8 weeks apart. For hair loss, a series of 3 monthly treatments is common.
If symptoms are severe or the tissue is significantly degenerated, your clinician may discuss whether additional injections could be helpful, or whether another interventional option or referral is more appropriate.
What should you do after a PRP injection?
Aftercare varies by the body part treated, but general guidance often includes:
- Activity modification: avoid high-impact or heavy loading of the treated area early on
- Rehab planning: begin or continue a structured physical therapy program when recommended
- Follow-up: reassessment helps confirm progress and refine your plan
We often recommend physical therapy alongside PRP to maximize the functional recovery of the treated area, especially for tendon and joint conditions where strength and mechanics strongly influence outcomes.
Conclusion
Understanding how does PRP work highlights a shift toward regenerative medicine that uses your own biology to heal. By concentrating platelets, PRP provides a targeted boost to the body’s repair mechanisms, from collagen synthesis to new blood vessel growth.
At Midwest Pain And Wellness, Dr. Yaw Donkoh and our team provide opioid-free, interventional care custom to your needs. If you are in Chicago Ridge and looking for long-term relief from chronic pain or injuries, PRP therapy offers a minimally invasive path to recovery. Contact us today to explore your regenerative future.