Understanding Pain Management: A Medical Specialty Dedicated to Your Relief
What is pain management dr refers to a physician with specialized training in evaluating, diagnosing, and treating all types of pain. These doctors—often called pain management specialists or pain medicine physicians—help people who suffer from acute, subacute, or chronic pain conditions.
Quick Answer:
A pain management doctor is a medical specialist who:
- Diagnoses the root causes of your pain through comprehensive evaluation
- Creates personalized treatment plans using multiple approaches
- Offers non-opioid therapies as first-line treatments
- Performs interventional procedures like nerve blocks and injections
- Coordinates care with other healthcare providers for comprehensive relief
- Focuses on improving your quality of life and daily function
Pain affects more than 50 million U.S. adults according to recent reports. For many people, this isn’t just a temporary discomfort—it’s a persistent condition that interferes with work, relationships, sleep, and everyday activities.
Unlike your primary care doctor who treats a wide range of health issues, a pain management specialist focuses exclusively on understanding and relieving pain. They have advanced training in pain physiology, diagnostic techniques, and a broad range of treatment options that go far beyond simply prescribing medication.
The field of pain management recognizes that chronic pain is not just a symptom—it’s often a disease process itself. This understanding has led to sophisticated, multimodal approaches that address pain from multiple angles, giving you the best chance at meaningful relief.
Whether you’re dealing with back pain, arthritis, neuropathy, or another condition, a pain management doctor can help you steer your options and find a path forward.
Decoding Pain: Understanding the Condition and the Specialty
When you’re living with pain that won’t go away, understanding what’s happening in your body can feel overwhelming. That’s where pain management comes in—a specialized medical field focused on helping people like you find relief and get back to living life on your terms.
Pain management isn’t just about masking discomfort. It’s about improving your quality of life and restoring your ability to do the things that matter most to you. Whether that’s playing with your grandchildren, returning to work, or simply sleeping through the night without waking up in agony.
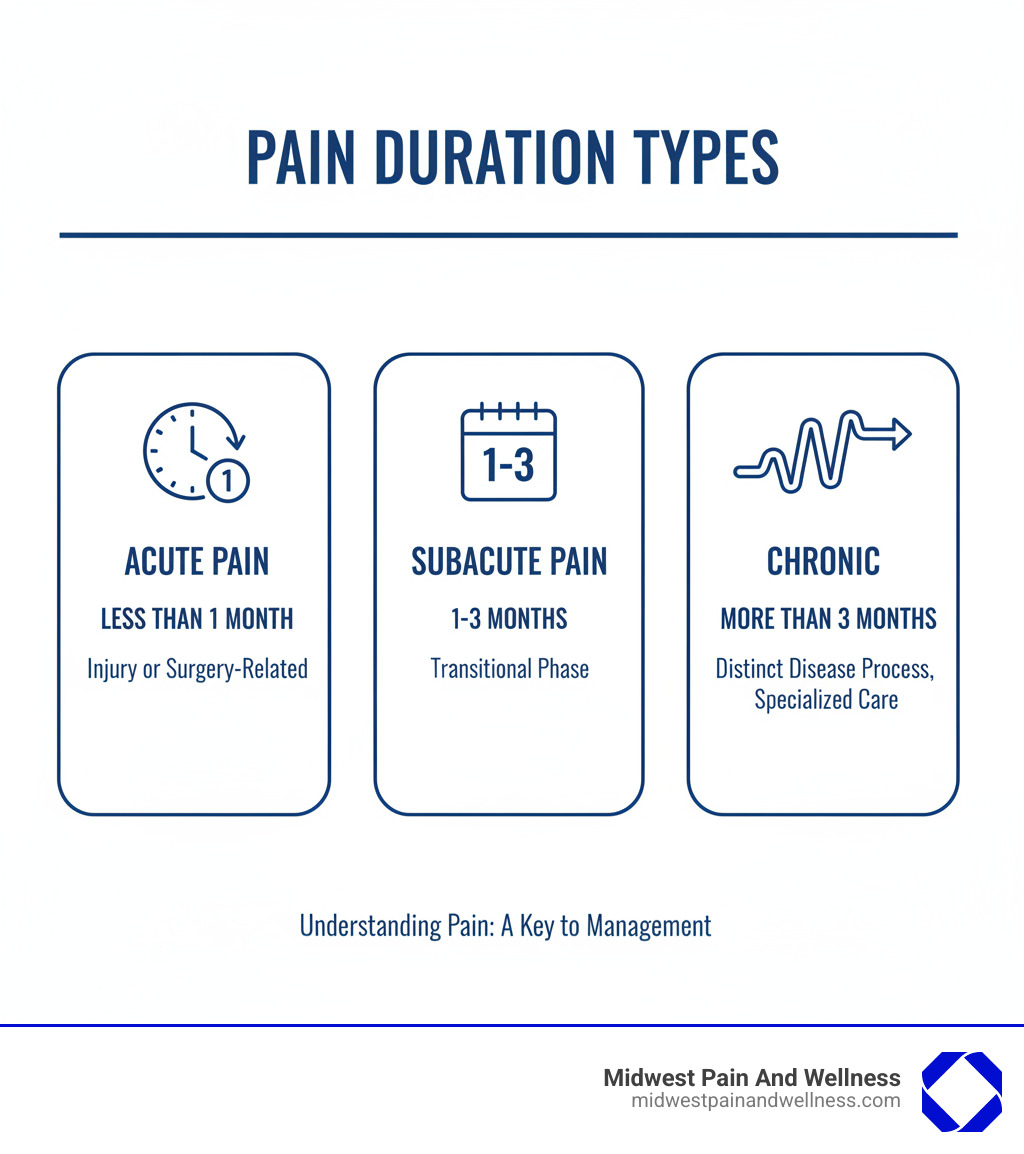
To understand what a pain management dr does, it helps to know that not all pain is created equal. Doctors categorize pain based on how long it lasts, and this distinction matters when it comes to treatment.
Acute pain typically lasts less than one month. It’s your body’s alarm system—sharp, immediate, and usually tied to a specific cause like a broken bone, surgery, or infection. Think of the pain you feel after spraining your ankle or having your appendix removed. As your body heals, this type of pain naturally fades.
Subacute pain hangs around for one to three months. You’re past the initial injury, and healing is happening, but your nervous system is still sending pain signals. This is a critical window where proper care can prevent pain from becoming a long-term problem.
Chronic pain is different. It persists for more than three months, and here’s what makes it particularly challenging: chronic pain is increasingly recognized as a disease in itself, not just a symptom of something else. Your nervous system has essentially gotten stuck in pain mode, even if the original injury has healed.
Chronic pain can stem from ongoing tissue damage, nerve dysfunction, inflammation, or sometimes no clear cause at all. It affects your physical abilities, your mental health, your relationships, and your overall quality of life. Research shows that current chronic pain treatments can achieve about a 30% decrease in pain scores—which might not sound like much, but for many people, it’s the difference between being bedridden and being able to function.
What conditions do pain management doctors treat?
A pain management dr has the training and expertise to tackle a wide range of pain conditions. We don’t just treat symptoms—we dig deep to find the source of your pain and build a treatment plan that addresses your specific situation.
Back pain is one of the most common reasons people seek pain management care. Whether you’re dealing with an acute muscle strain or chronic conditions like herniated discs, spinal stenosis, or degenerative disc disease, we have specialized treatments that can help. This includes pain in your lower back, mid-back, and upper back.
Neck pain often develops from poor posture (yes, looking at you, smartphone users), whiplash injuries, pinched nerves in the neck, or arthritis. When neck pain radiates down your arm or causes headaches, it’s time to see a specialist.
Arthritis comes in many forms, and we treat them all. Osteoarthritis—the wear-and-tear kind that commonly affects knees, hips, and hands—can make simple movements excruciating. Inflammatory arthritis like rheumatoid arthritis requires a different approach, and we work with your other doctors to manage the pain effectively.
Neuropathic pain results from damaged or malfunctioning nerves. This includes conditions like sciatica, diabetic neuropathy, post-herpetic neuralgia (the lingering pain after shingles), trigeminal neuralgia, and pain from multiple sclerosis or spinal cord injuries. Nerve pain can feel like burning, shooting, stabbing, or electric shocks. It’s notoriously difficult to treat—less than 50% of people with neuropathic pain find adequate relief with a single therapy, which is why we use comprehensive, multimodal approaches.
Fibromyalgia causes widespread musculoskeletal pain throughout your body, along with fatigue, sleep problems, and cognitive difficulties often called “fibro fog.” It’s a complex condition that requires a equally sophisticated treatment strategy.
Headaches and migraines that are persistent or severe can be debilitating. We treat chronic migraines, tension headaches, cluster headaches, and other types of head pain that interfere with your daily life.
Cancer pain can come from the cancer itself, from treatments like chemotherapy or radiation, or from associated conditions. Managing this pain is crucial for maintaining quality of life during and after cancer treatment.
Post-surgical pain sometimes persists long after the surgical site has healed. When pain becomes chronic after surgery, specialized intervention can help break the cycle.
Complex Regional Pain Syndrome (CRPS) is a chronic pain condition that typically affects an arm or leg, usually after an injury, surgery, stroke, or heart attack. The pain is often disproportionate to the original injury and requires specialized care.
Beyond these common conditions, we also manage other complex pain disorders that disrupt your daily life. Our goal is always the same: identify the source of your pain and create a treatment plan custom specifically for you.
The Specialist’s Role: What is a Pain Management Dr?
A pain management dr is a medical doctor—either an MD (Doctor of Medicine) or DO (Doctor of Osteopathic Medicine)—who has dedicated their career to understanding and treating one of the most complex challenges in medicine: pain itself. These physicians bring together specialized knowledge, advanced diagnostic skills, and a compassionate approach to help people whose lives have been disrupted by persistent pain.
What sets pain management doctors apart is their focused expertise in diagnosing the source of your pain. They don’t just treat the symptoms you’re experiencing—they work to understand what’s causing those symptoms in the first place. This might involve analyzing nerve function, evaluating structural problems in your spine, or identifying inflammation patterns that other providers might miss.
Once they’ve identified the underlying issues, pain management doctors develop comprehensive treatment plans custom specifically to your situation. These plans draw from a wide range of options, including medications, interventional procedures, physical therapies, and psychological support. The goal isn’t simply to mask your pain, but to address its root causes and help you regain function in your daily life.
A hallmark of effective pain medicine is the multidisciplinary approach. Your pain management doctor serves as the quarterback of your care team, coordinating with other specialists to ensure you receive well-rounded treatment. This might include working alongside physical therapists to improve your mobility, consulting with psychologists to address the emotional toll of chronic pain, collaborating with surgeons when needed, and maintaining close communication with your primary care physician.
This team-based strategy recognizes an important truth: pain affects every aspect of your life—physical, emotional, and social. By bringing together experts from different fields, we can address all these dimensions and give you the best chance at meaningful, lasting relief.
Pain management doctors often come from backgrounds in anesthesiology, which provides extensive training in pain physiology and interventional procedures. Others specialize in physical medicine and rehabilitation (PM&R), focusing on restoring function and quality of life. Some have training in neurology, bringing deep expertise in nerve-related pain conditions, while others come from psychiatry, with special insight into the psychological aspects of chronic pain.
At Midwest Pain And Wellness, our doctors are double board-certified, meaning they’ve achieved certification in not just one, but two medical specialties. This demonstrates an exceptional level of expertise and commitment to providing the highest quality care for complex pain conditions.
What is the training and background of a pain management doctor?
Becoming a pain management dr requires an extraordinary commitment to education and training—typically more than nine years beyond a bachelor’s degree. This extensive preparation ensures that these specialists have the knowledge and skills needed to tackle even the most challenging pain conditions.
The journey begins with medical school, where aspiring physicians spend four years mastering the fundamentals of human anatomy, physiology, pharmacology, and disease processes. They emerge with either an MD or DO degree and a broad foundation in medicine.
Next comes residency training, which lasts approximately four years. During residency, physicians focus intensively on a specific medical specialty. For future pain management doctors, this is often anesthesiology, where they gain deep experience with pain physiology, advanced pharmacology, and the procedures used to block pain signals. Some complete residencies in physical medicine and rehabilitation, learning to restore function and treat musculoskeletal conditions. Others train in neurology, specializing in disorders of the nervous system, or psychiatry, focusing on the mind-body connection in pain.
After completing residency, physicians who want to specialize in pain management pursue an additional year of fellowship training. This fellowship is devoted entirely to the evaluation, diagnosis, and treatment of all types of pain. During this intensive year, doctors gain hands-on experience with advanced diagnostic techniques, specialized interventional procedures like nerve blocks and spinal injections, and complex medication management strategies. They learn to treat everything from common back pain to rare conditions like Complex Regional Pain Syndrome.
Following fellowship, pain management doctors pursue board certification in Pain Medicine. This subspecialty certification demonstrates that a physician has met rigorous standards of expertise and passed comprehensive examinations. At Midwest Pain And Wellness, our doctors are double board-certified, having achieved certification in both their primary specialty and pain medicine—a distinction that reflects exceptional dedication to their field.
The learning doesn’t stop there. Because pain management is a rapidly evolving field, dedicated pain doctors engage in ongoing education throughout their careers. They attend conferences, review the latest research, and continually refine their techniques to ensure they’re offering the most current and effective treatments available.
What should I expect during my first visit to a pain management specialist?
Your first appointment with a pain management dr is an important opportunity for us to understand your unique situation and begin developing a plan to help you feel better. We know that chronic pain can be frustrating and exhausting, so we’ve designed this visit to be thorough yet comfortable.
We’ll start by taking a comprehensive medical history. This means discussing your past medical conditions, any surgeries you’ve had, previous injuries, and other health issues that might be relevant. We’re looking for clues about what might be contributing to your pain, and sometimes the answer lies in understanding your overall health picture.
Next, we’ll dive into a detailed pain history. This is where you get to tell your story. We’ll ask about the location of your pain—exactly where you feel it and whether it radiates to other areas. We’ll want to know about the quality of your pain: Is it sharp or dull? Burning or aching? Throbbing or constant? These descriptions help us understand what type of pain you’re experiencing.
We’ll ask you to rate your pain intensity on a scale from 0 to 10, where 0 means no pain at all and 10 is the worst pain you can imagine. We’ll also discuss when the pain started, whether it’s constant or comes and goes, what makes it worse, and what provides relief. Understanding what aggravates and alleviates your pain gives us valuable insights.
It’s important that we know about any previous treatments you’ve tried—medications, injections, physical therapy, chiropractic care, or anything else. We want to understand what worked, what didn’t, and any side effects you experienced. This helps us avoid repeating approaches that haven’t helped and build on strategies that have shown promise.
Perhaps most importantly, we’ll discuss how pain affects your daily life. Can you sleep through the night? Are you able to work? Have you had to give up activities you love? How has pain impacted your relationships and your mood? These questions help us understand what matters most to you and what improvements would make the biggest difference.
During the physical examination, we’ll assess the area where you’re experiencing pain, but we’ll also look at your posture, observe how you move, test your reflexes, and check your sensation. Sometimes the source of pain isn’t exactly where you feel it, and a thorough physical exam can reveal important clues.
Please bring any imaging and test results you have—X-rays, MRI scans, CT scans, or nerve conduction studies. We’ll review these together to help confirm or refine our diagnostic understanding. If you haven’t had recent imaging, we may recommend additional tests.
We’ll also talk about your goals for treatment. What does success look like to you? Is it getting back to work? Playing with your grandchildren? Sleeping through the night? Reducing your pain enough to exercise? Your goals become our goals, and they guide every decision we make about your care.
Finally, we’ll discuss realistic expectations. While we’re committed to helping you feel significantly better, we also believe in honesty. Current chronic pain treatments typically aim for about a 30% decrease in pain scores, though many patients experience even greater relief. For us, success isn’t just about numbers on a pain scale—it’s about helping you reclaim your life and the activities that matter to you.
To help you prepare for your first visit, the AHRQ guide on preparing for appointments offers helpful tips on organizing your medical information and questions. Coming prepared helps us make the most of our time together and get you started on the path to relief as quickly as possible.
Crafting Your Relief: A Tour of Pain Management Treatments
When you walk into Midwest Pain And Wellness, you’re not getting a one-size-fits-all prescription. We take the time to truly understand your pain and design a treatment plan that’s as unique as you are. This is what we call a multimodal approach—combining different therapies and techniques to give you the best possible outcome.
Think of it like this: if you’re trying to move a heavy piece of furniture, pushing from just one angle might not work. But when you push, lift, and slide all at once, suddenly it moves. Pain management works the same way. By addressing your pain from multiple directions simultaneously, we can often achieve relief that a single treatment alone couldn’t deliver.

Our treatment plans are goal-oriented, meaning we start by asking what matters most to you. Maybe it’s being able to play with your grandchildren again, returning to your favorite hobby, sleeping through the night, or simply getting back to work. Whatever your goals are, they become the target we’re aiming for together.
Research shows that even a 30% decrease in pain scores can dramatically improve your daily functioning and quality of life. That might not sound like complete elimination, but for many people, it’s the difference between being stuck on the couch and reclaiming the activities they love.
Here’s how the different treatment categories work together:
| Treatment Category | Description | Examples |
|---|---|---|
| Medications | Pharmaceutical options to reduce pain signals, inflammation, and nerve sensitivity | Non-opioid pain relievers, anti-inflammatory drugs, nerve pain medications, muscle relaxants |
| Interventional Procedures | Targeted procedures that deliver relief directly to the pain source | Nerve blocks, epidural injections, radiofrequency ablation, trigger point injections |
| Therapies | Physical and psychological approaches that restore function and change pain perception | Physical therapy, occupational therapy, Cognitive Behavioral Therapy (CBT), biofeedback |
As a pain management dr, we’re constantly evaluating what’s working and what needs adjustment. Your treatment plan isn’t set in stone—it evolves as you heal and as we learn more about what helps your specific condition. This individualized care is at the heart of everything we do at Midwest Pain And Wellness.
What are the various treatment approaches used by a pain management dr?
The beauty of modern pain management is that we have an extensive toolkit at our disposal. At Midwest Pain And Wellness, our double board-certified doctors draw from multiple treatment categories to create your personalized plan.
Medications form one important component, but we emphasize non-opioid options as first-line treatments. These include anti-inflammatory medications, nerve pain medications like gabapentin or duloxetine, muscle relaxants, and topical treatments. Each medication targets pain through different mechanisms, which is why combining them strategically often works better than relying on just one.
Interventional procedures are where pain management specialists truly shine. These are minimally invasive techniques that target the exact source of your pain. Examples include epidural steroid injections for back and leg pain, nerve blocks that interrupt pain signals, radiofrequency ablation that provides longer-lasting relief by carefully treating specific nerves, and trigger point injections for muscle pain. These procedures are performed with precision, often using imaging guidance to ensure accuracy.
Physical therapy and rehabilitation help restore strength, flexibility, and function. Your body often compensates for pain in ways that create new problems, and physical therapy retrains your movement patterns while building resilience. Occupational therapy helps you adapt daily activities to reduce strain and pain.
Psychological support addresses the emotional and mental aspects of chronic pain. Cognitive Behavioral Therapy (CBT) teaches practical skills for managing pain-related stress, anxiety, and depression. Biofeedback helps you gain awareness and control over physical responses to pain.
Complementary therapies round out our approach. These include massage therapy, acupuncture, mindfulness techniques, and relaxation training. While these aren’t typically standalone solutions, they can significantly improve the effectiveness of other treatments.
For more detailed information on treatment options, the American Society of Regional Anesthesia and Pain Medicine provides additional resources on treatment options for chronic pain.
What is the role of non-opioid therapies in pain management?
At Midwest Pain And Wellness, non-opioid therapies are our first-line approach. This isn’t just a trend—it’s based on solid evidence showing that these treatments can be just as effective as opioids for many types of pain, without the serious risks.
The national conversation around opioids has changed dramatically in recent years, and for good reason. While opioids have a place in specific situations, they’re not the answer for most chronic pain conditions. Non-opioid approaches address pain through different pathways and actually help your body heal and adapt, rather than just masking symptoms.
Physical therapy is one of the most powerful non-opioid tools we have. A skilled physical therapist can identify movement problems, strengthen supporting muscles, and teach you techniques that reduce pain during daily activities. The benefits extend far beyond the therapy sessions themselves—you’re learning skills you’ll use for life.
Occupational therapy focuses on adapting your environment and activities to minimize pain triggers. This might mean ergonomic changes at your workstation, techniques for household tasks, or strategies for pacing activities throughout your day.
Cognitive Behavioral Therapy (CBT) has strong scientific support for chronic pain management. It doesn’t mean your pain is “all in your head”—rather, CBT teaches you practical skills for managing the very real ways that pain affects your thoughts, emotions, and behaviors. Many patients find this empowering.
The CDC provides comprehensive information on non-opioid therapies that patients and families find helpful.
Massage therapy offers more than just relaxation. Regular therapeutic massage can reduce muscle tension, improve circulation, and decrease pain intensity. Research from Cleveland Clinic highlights the benefits of massage for various pain conditions.
Mindfulness and meditation techniques help you change your relationship with pain. Instead of fighting against discomfort, you learn to observe it without judgment, which often reduces its intensity and emotional impact. Cleveland Clinic also offers practical guidance on mindfulness techniques that complement medical treatment.
By starting with these approaches, we can often achieve significant relief while avoiding the risks associated with long-term opioid use. And when these therapies are combined—physical therapy plus cognitive strategies plus appropriate medications—the results are often better than any single treatment alone.
What are the risks and benefits associated with different pain management treatments, including opioids?
Transparency matters. As your pain management dr, we believe you deserve to understand both the potential benefits and risks of any treatment we recommend. This is called shared decision-making, and it’s central to how we practice at Midwest Pain And Wellness.
Every treatment involves a risk-benefit analysis. A treatment that works wonderfully for one person might not be right for another, depending on their specific condition, medical history, and personal circumstances. Our job is to present the options clearly so you can make informed choices about your care.
Let’s talk honestly about opioids. These medications can provide significant pain relief for certain acute situations—after surgery, for instance, or for cancer-related pain. However, for chronic non-cancer pain, the risks often outweigh the benefits.
The risks of long-term opioid use are serious and well-documented. Addiction is a real concern—opioids change brain chemistry in ways that can lead to dependence, even when taken as prescribed. Tolerance develops over time, meaning you need higher doses to achieve the same effect. Common side effects include constipation, drowsiness, mental fog, and hormonal changes. More seriously, opioids can slow breathing, and overdose is a genuine risk.
The numbers are sobering: approximately 8.5 million people reported misusing prescription pain medications in a recent year. This isn’t about moral failing—it reflects the powerful nature of these drugs and why we need to be so careful with them.
When opioids are necessary, we prescribe them cautiously, with clear goals, regular monitoring, and a plan for tapering off when appropriate. The CDC offers helpful guidelines on opioid therapy that inform our prescribing practices.
Non-opioid medications have their own considerations. Anti-inflammatory drugs can affect your stomach, kidneys, or cardiovascular system with long-term use. Nerve pain medications might cause dizziness or drowsiness initially. We monitor these carefully and adjust as needed.
Interventional procedures carry small risks like infection, bleeding, or temporary increased pain at the injection site. However, these procedures are generally very safe when performed by experienced specialists using proper techniques. The potential benefits—targeted, often long-lasting relief—frequently outweigh these minimal risks.
The key is having open conversations about what you’re comfortable with, what your priorities are, and what makes sense for your specific situation. We’re here to guide you through these decisions, not to make them for you.



