Understanding the Medical Revolution Reshaping Pain Treatment
What are advanced therapies? Advanced therapies are innovative medical treatments based on genetic material, stem cells, and tissues that offer new possibilities for healing conditions where conventional treatments have proven ineffective. These therapies encompass three main categories:
- Gene Therapy: Treatments that modify or replace faulty genes to address conditions at their genetic source
- Cell Therapy: The use of living cells, often stem cells, that have been manipulated to achieve therapeutic effects
- Tissue Engineering: Laboratory-cultivated cells or tissues designed to repair, regenerate, or replace damaged human tissue
The field of advanced therapies represents a fundamental shift in how we approach healing. Unlike traditional pharmaceuticals that manage symptoms, these treatments work at the cellular level to actually repair damaged tissue and restore function. The European Union has approved 21 advanced therapy drugs as of June 2022, with hundreds more currently in clinical trials targeting conditions from cancer to cardiovascular disease.
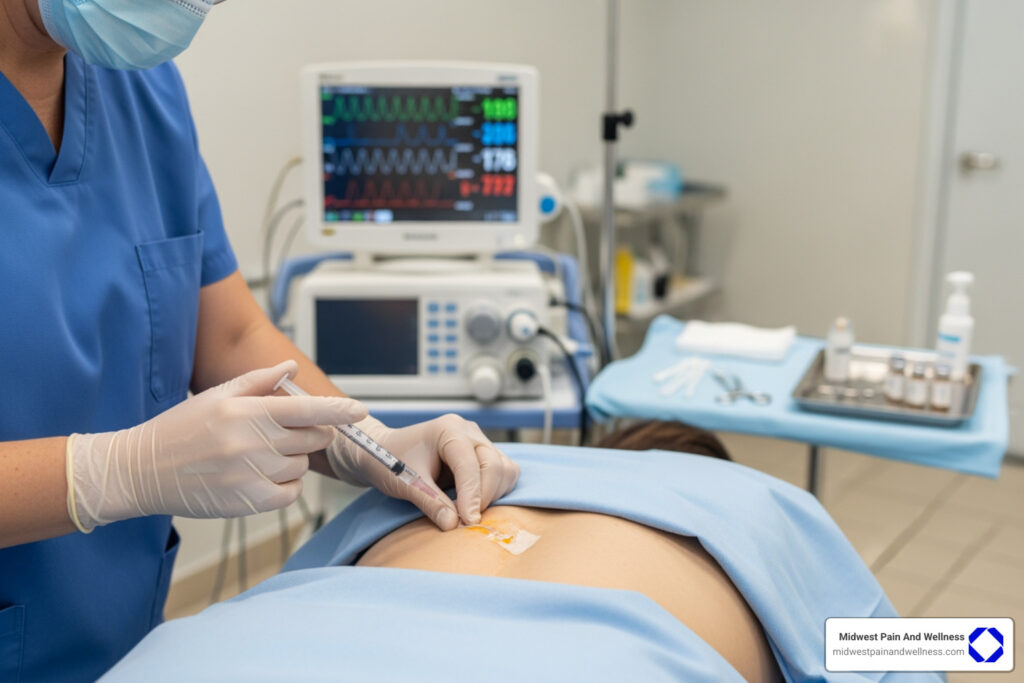
For those living with chronic pain, this matters because advanced therapies offer genuine alternatives to opioids and surgery. Rather than masking pain or cutting out damaged tissue, these treatments harness your body’s natural healing mechanisms—using stem cells as building blocks to create healthy new cells and restore damaged ones.
As Dr. Yaw Donkoh, a double board-certified physician in anesthesiology and interventional pain management, I’ve witnessed how regenerative approaches can transform outcomes for patients who’ve exhausted conventional options. Understanding what are advanced therapies is essential for anyone seeking cutting-edge, evidence-based solutions to persistent pain.

Defining the New Frontier: What are advanced therapies?
What are advanced therapies? At their core, advanced therapies represent a fast-moving, interdisciplinary field of research focused on restoring and restructuring diseased or damaged tissue and organs. These biological medicines leverage the body’s own incredible capacity for healing, moving beyond symptom management to address the root causes of illness and injury. They are often referred to as Advanced Therapy Medicinal Products (ATMPs), particularly in regulatory contexts.
The purpose of these therapies is to regenerate, repair, or replace compromised cells or tissue, offering new hope for conditions where traditional treatments fall short. This involves a blend of cutting-edge biotechnology, including the strategic use of stem cells, which act as the body’s essential building blocks. The field is constantly evolving, with significant scientific research dedicated to understanding and classifying these complex interventions, as highlighted in various studies, including this Scientific research on ATMP classification.
For those interested in exploring these innovative treatment options further, particularly in pain management, we offer More info about regenerative therapy at Midwest Pain And Wellness.
What are advanced therapies in the context of gene modification?
When we talk about advanced therapies in the context of gene modification, we’re primarily referring to gene therapy. This approach aims to treat conditions caused by faulty genes by inserting a correct copy of a mutated gene directly into a patient’s cells or by compensating for its altered function. The process often involves using specialized “vectors,” such as modified viruses, to deliver the new genetic material into the target cells.
The goal is to correct the underlying genetic defect, effectively “rewriting” the instructions within the cells to produce healthy proteins or perform their proper functions. This can include DNA repair mechanisms, where specific genetic sequences are edited to fix errors. Gene therapy holds immense promise for a range of inherited and acquired diseases, moving beyond just managing symptoms to offering potential cures by addressing the fundamental genetic blueprint.
What are advanced therapies doing to change chronic pain management?
For us at Midwest Pain And Wellness, advanced therapies are fundamentally reshaping chronic pain management by offering powerful, opioid-free relief and promoting long-term healing. Traditional pain management often relies on medications that mask pain or invasive surgeries that alter anatomy, sometimes without addressing the underlying tissue damage or dysfunction.
Advanced therapies, particularly those involving cell-based and regenerative approaches, work differently. They focus on an interventional approach that harnesses the body’s innate healing capabilities. Instead of just blocking pain signals, these therapies aim to repair damaged nerves, joints, tendons, and discs. By regenerating injured tissues, they can restore function and significantly reduce pain, leading to more sustainable and comprehensive relief. This aligns perfectly with our philosophy of creating custom care plans that prioritize long-term healing and improving our patients’ quality of life. For a deeper dive into our approach to managing persistent discomfort, you can find More info about chronic pain treatment.
The Core Pillars: Gene, Cell, and Tissue Engineering
The definition of advanced therapies is rooted in three distinct yet often overlapping categories: gene therapy, cell therapy, and tissue engineering. These are the fundamental “pillars” upon which this new era of medicine is built. In regions like the European Union, these categories are formally defined under regulations such as the Archived EU Regulation 1394/2007, which helps classify Advanced Therapy Medicinal Products (ATMPs). While regulatory specifics vary globally, the core scientific concepts remain consistent.
Let’s break down each pillar:
| Category | Primary Mechanism | Key Components / Focus | Examples |
|---|---|---|---|
| Gene Therapy | Modifying or introducing genetic material | DNA, RNA, viral/non-viral vectors | Correcting faulty genes, producing therapeutic proteins |
| Cell Therapy | Using live cells (often somatic or stem cells) | Autologous/allogeneic cells, manipulated cells | Immunotherapy (e.g., CAR T-cells), regenerative injections |
| Tissue Engineering | Creating or cultivating cells/tissues outside the body | Scaffolds, biomaterials, lab-grown cells/tissues | Lab-grown cartilage, artificial skin, organ repair |
Somatic Cell Therapy Medicinal Products
Somatic cell therapy medicinal products (sCTMPs) involve the use of live somatic cells that have been substantially altered through manipulation to achieve a therapeutic, diagnostic, or preventive effect. These cells can be derived from the patient themselves (autologous), from another human donor (allogeneic), or even from an animal (xenogeneic).
The “manipulation” is key here; it goes beyond simple handling and significantly changes the cells’ biological characteristics, physiological functions, or structural properties. The aim is for these cells to exert their effect through metabolic, pharmacological, or immunological means. A prominent example of cell therapy is immunotherapy, such as CAR T-cell therapy for cancer, where a patient’s own immune cells are genetically modified in the lab to better target and destroy cancer cells. At Midwest Pain And Wellness, we also explore various More info about cell-based options for pain relief, leveraging the body’s natural healing processes.
Tissue Engineered Products
Tissue engineered products (TEPs) are designed to repair, regenerate, or replace human tissue. These products contain or consist of engineered cells or tissues that have been constructed or cultivated in a laboratory setting. They often involve a combination of cells, biomaterials (like scaffolds that provide structural support), and biologically active molecules.
The goal is to grow functional tissue outside the body that can then be implanted to replace damaged tissue. Examples include lab-grown cartilage for joint repair, artificial skin for burn victims, or even more complex structures aimed at regenerating organs. The engineered cells or tissues are either not intended for the same essential function in the recipient as in the donor, or they have undergone substantial manipulation to improve their regenerative capabilities.
How Advanced Therapies Work: The Role of Stem Cells
At the heart of many advanced therapies, particularly in regenerative medicine, lies the incredible power of stem cells. These are naturally occurring cells in our bodies that possess a remarkable ability: they can divide and produce a range of different cell types. Think of them as the body’s ultimate building blocks, capable of becoming specialized cells like bone, muscle, nerve, or cartilage, and playing a crucial role in growth, development, and repair after injury.
This unique capacity is precisely how advanced therapies leverage stem cells. They are used to kick-start the body’s regenerative process, creating new, healthy cells and restoring damaged ones. While some cells in our body, like skin cells, are constantly self-healing without intervention, others, such as those in organs and connective tissues, often need assistance. Advanced therapies provide this assistance by introducing or stimulating stem cells to repair or replace compromised tissue.
For pain management, this means we can use stem cells to target areas of chronic damage—whether it’s a worn-out joint, a degenerated disc, or injured ligaments—and encourage the body to heal itself more effectively. This regenerative potential offers a stark contrast to treatments that merely manage symptoms. For example, therapies like More info about amniotic fluid injections use the rich regenerative properties of the amniotic fluid to support natural healing processes.
Stem cells as Advanced Therapy Medicinal Products (ATMPs)
Stem cells are categorized as Advanced Therapy Medicinal Products (ATMPs) when they undergo “substantial manipulation” or are used for a “different essential function” than their original biological role. This distinction is crucial for regulatory bodies, as it dictates the level of oversight and approval required. Basic manipulations like cutting, grinding, shaping, or simple freezing usually don’t qualify a product as an ATMP. However, if the cells are cultured extensively, genetically modified, or combined with non-cellular components in a way that significantly alters their biological characteristics, they enter the ATMP classification.
The development of stem cell-based ATMPs requires meticulous attention to manufacturing consistency and reproducibility. Regulatory bodies, such as the European Medicines Agency (EMA) in the EU and the Food and Drug Administration (FDA) in the United States, closely scrutinize these aspects. They emphasize that pre-clinical and clinical testing must thoroughly account for the unique properties of these cells, adequately studying potential risks—like unintended tumor development or immune rejection—and balancing them against the anticipated patient benefits. This rigorous process ensures that these innovative treatments are both safe and effective before they can reach patients.
Navigating the Regulatory Landscape for ATMPs
The regulatory landscape for Advanced Therapy Medicinal Products (ATMPs) is a complex and evolving domain, distinct from that of traditional pharmaceuticals. These innovative treatments, by their very nature, present unique challenges for regulators worldwide.
In regions like the European Union, a comprehensive framework has been established, notably with EU Regulation No. 1394/2007, which regulates the development and marketing authorization of ATMPs. The European Medicines Agency (EMA) has a dedicated Committee for Advanced Therapies (CAT) that plays a central role in assessing these products, evaluating their risk/benefit profile, and providing scientific advice. You can learn more about this body at the Official EMA Committee for Advanced Therapies. This framework aims to ensure patient safety while fostering innovation and market access within Europe.
In the United States, where Midwest Pain And Wellness operates, the Food and Drug Administration (FDA) takes a similar rigorous approach to regenerative medicine therapies (RMTs), which include cell therapies, therapeutic tissue engineering products, and human cell and tissue products. The FDA defines RMTs in section 506(g)(8) of the Food Drug & Cosmetic Act. To accelerate the development and review of certain promising RMTs, the 21st Century Cures Act established the Regenerative Medicine Advanced Therapy (RMAT) designation. This designation is designed to facilitate faster access for patients to therapies that address unmet medical needs.
While the specific classifications and approval pathways may differ between regulatory bodies like the EMA and FDA, the overarching goal remains the same: to ensure that advanced therapies are safe, effective, and of high quality before they reach patients. This often involves processes for marketing authorization, and in some cases, provisions like “hospital exemption” for products prepared on a non-routine basis for individual patients within a hospital setting, reflecting the bespoke nature of some of these treatments. It’s clear that global inconsistencies exist, but the trend is towards increasingly sophisticated oversight for these breakthrough medicines.
Challenges in regulating ATMPs vs. traditional pharmaceuticals
Regulating ATMPs presents unique complexities that set them apart from traditional pharmaceuticals. Unlike conventional drugs, which are typically chemical compounds manufactured in large, standardized batches, ATMPs often involve living cells or genetic material, making their production and standardization far more intricate.
One significant challenge is the “industrial process” aspect. Many ATMPs start with patient-specific cells, leading to small batch sizes or even “custom-made” products custom to an individual. This makes traditional large-scale manufacturing quality control and reproducibility difficult. The inherent variability of biological starting materials and the complex manufacturing processes require specialized Good Manufacturing Practice (GMP) guidelines.
Another complexity lies in the need for long-term follow-up. Because ATMPs often aim for durable or even curative effects by modifying cells or genes, their long-term safety and efficacy need extensive monitoring, sometimes for many years after administration. This contrasts with many traditional drugs where effects are more immediate and reversible. The risk-benefit assessment for ATMPs must consider these long-term implications, including potential for immune rejection or unintended cellular changes. These unique characteristics necessitate specialized clinical trial methodologies, often involving smaller patient cohorts and adaptive designs, which can be challenging to align with conventional regulatory expectations.
The Current Landscape and Future of Advanced Therapies
The field of advanced therapies is experiencing exponential growth, reflecting its immense potential to transform medicine. Data from a comprehensive review up to June 2015 identified 939 clinical trials investigating ATMPs globally, with a striking 85% still ongoing. This indicates a robust and active development pipeline. The majority of these trials are in the early stages (Phase I, I/II: 64.3%), illustrating the exploratory nature of much of the current research, though a significant portion (Phase II, II/III: 27.9%, Phase III: 6.9%) are progressing towards pivotal studies.
Looking at the breakdown by category, somatic cell therapies lead the pack, accounting for 53.6% of trials, followed by tissue-engineered products (22.8%) and gene therapies (22.4%). Combined products are less common at 1.2%. These statistics underscore the diverse approaches being explored within advanced therapies.
These trials target a wide array of diseases. Cancer is a primary focus (24.8%), reflecting the impact of immunotherapies and gene therapies in oncology. Cardiovascular diseases (19.4%), musculoskeletal conditions (10.5%), immune system and inflammation disorders (11.5%), and neurology (9.1%) also represent significant areas of investigation. The consistent growth in ATMP clinical trials over the past 15 years—from 34 trials in 1999–2003 to 572 in 2011–2015—signals a burgeoning field with profound implications for future healthcare. For a deeper understanding of the current and future outlook, you can refer to this Scientific study on ATMP perspectives.
Future perspectives on healthcare impact
The future of advanced therapies holds immense promise, with the potential to offer curative solutions for severe chronic conditions that currently have limited treatment options. This curative potential could lead to significant long-term health benefits for patients and, paradoxically, could also pose substantial challenges for healthcare budgets.
ATMPs often come with high development costs due to their complexity, specialized manufacturing, and the need for extensive long-term follow-up. This translates into high anticipated prices, sometimes reaching hundreds of thousands or even millions of dollars per patient, as seen with early gene therapies like Glybera or cell therapies like Provenge. These pricing strategies, while reflecting the innovation and potential for a cure, can strain the sustainability of national health insurance systems.
The challenge lies in balancing the desire for patient access to these life-changing treatments with the economic realities of healthcare funding. Payers are increasingly demanding robust clinical evidence, including long-term data, to justify these high costs. This may lead to new reimbursement models, such as outcomes-based agreements or installment payments. Advanced therapies are ready to fundamentally reshape healthcare, requiring innovative solutions not just in science, but also in how we finance and deliver these transformative treatments. The goal is to ensure that their profound impact on patient outcomes is matched by accessible and sustainable integration into our healthcare systems.
Frequently Asked Questions about Advanced Therapies
What are the potential benefits and risks for patients?
Advanced therapies offer numerous potential benefits, including the possibility of life-changing cures for previously untreatable conditions, significant improvements in quality of life, and the potential to halt or reverse disease progression. For many patients, these therapies represent a last resort and a guide of hope. They can target the root causes of disease, leading to durable and long-lasting effects that go beyond symptom management.
However, like all medical treatments, advanced therapies also carry risks. Because they involve manipulating genes or cells, there are concerns about potential unintended side effects. These can include off-target gene activation, immune rejection (where the body attacks the introduced cells or genetic material), or, in rare cases, the uncontrolled growth of cells, leading to tumor development. Ensuring manufacturing consistency and reproducibility is also critical to minimize variability and potential safety issues. The rigorous regulatory review processes are designed to thoroughly assess these risks against the potential clinical efficacy, ensuring that the benefits outweigh the potential harms for patients.
How many advanced therapies are currently approved?
The number of approved advanced therapies is steadily growing, but it’s important to differentiate between approvals in different regions. As of June 30, 2022, the European Union had approved 21 advanced therapy drugs, though only 14 of these had marketing authorization, meaning they were cleared for sale. These approvals include groundbreaking treatments for rare genetic conditions and certain cancers.
Globally, the landscape of ATMP development is vast and rapidly expanding. Our research identified 939 clinical trials investigating ATMPs, with the number consistently growing over the past 15 years. This reflects a dynamic field with a strong pipeline of innovative treatments in various stages of development. While the number of fully approved therapies may seem modest compared to traditional drugs, the pace of innovation and the focus on rare diseases and conditions with high unmet needs are significant.
Who sponsors the majority of advanced therapy research?
Interestingly, the majority of advanced therapy research is sponsored by non-commercial entities, particularly in the earlier phases of development. Our data shows that 73.2% of ATMP trials were sponsored by non-commercial organizations, such as universities, medical centers, and research institutes. These institutions often drive the foundational science and early-stage clinical investigations for these complex therapies.
However, as ATMPs progress to later stages of clinical development, especially Phase III, there’s a shift towards commercial sponsorship. While only 20% of Phase I and I/II trials had commercial sponsors, this figure rises to 53.8% for Phase III trials. This transition reflects the substantial financial investment required for large-scale clinical trials, manufacturing infrastructure, and the complex process of bringing a product to market. Commercial sponsors typically step in when the potential for successful treatment and eventual commercialization becomes clearer, taking on the significant costs and risks associated with late-stage development and regulatory approval.
Conclusion
What are advanced therapies? They are a guide of hope in modern medicine, offering innovative solutions that move beyond symptom management to target the root causes of disease and injury. From gene editing to cellular regeneration and tissue reconstruction, these therapies are fundamentally changing how we approach healing, particularly for chronic and previously untreatable conditions.
At Midwest Pain And Wellness, we are dedicated to staying at the forefront of these advancements, integrating cutting-edge, opioid-free pain management strategies into our practice in Chicago Ridge, Illinois. Our double board-certified doctors use a multi-modal, interventional approach, collaborating with other practitioners to create custom care plans for long-term pain relief. We believe in using the body’s natural healing mechanisms, and advanced therapies are a crucial part of this philosophy.
If you’re seeking innovative solutions for persistent pain and want to explore how advanced therapies might fit into your personalized treatment plan, we invite you to learn more about the More info about conditions we treat at our clinic. We are committed to guiding you through the possibilities and helping you achieve lasting relief and improved quality of life.