When that sharp, shooting, or burning nerve pain suddenly flares up, your first thought is getting it to stop. Right now. The good news is you don't have to just wait it out. There are simple, effective first-aid steps you can take at home to dial down the intensity and get some immediate control.
Finding Immediate Nerve Pain Relief At Home

Before you can see a specialist for a full diagnosis, knowing how to manage a sudden attack at home is crucial. Think of these strategies as your first-response toolkit for nerve pain, whether you're right here in Chicago Ridge or in nearby Illinois communities like Oak Lawn and Palos Hills.
These aren't cures, but they can provide significant temporary relief. The goal is simple: calm the irritated nerve and interrupt the pain signals screaming at your brain.
To make it easy to remember, here's a quick rundown of what you can do the moment pain strikes.
At-Home Strategies For Immediate Nerve Pain Relief
| Technique | How It Works | Best For |
|---|---|---|
| Cold Therapy | Constricts blood vessels, numbs the area, and reduces inflammation that may be compressing a nerve. | Acute, sudden pain like a new sciatica flare-up or post-injury nerve irritation. Use for 15-20 minutes at a time. |
| Heat Therapy | Increases blood flow and relaxes tight muscles that might be pinching or irritating a nearby nerve. | Chronic, persistent, or achy nerve pain and muscle stiffness. A warm bath or heating pad can soothe the area. |
| Gentle Movement | Prevents stiffness and can help decompress a nerve by changing your body's position. | Pain caused by nerve compression, like a pinched nerve in the neck or sciatica from a bad posture. |
| Proper Hydration | Ensures nerves have the fluid needed to transmit electrical signals correctly and supports overall system function. | All types of nerve pain, as dehydration can worsen symptoms. A foundational step that supports all other efforts. |
These accessible methods can bridge the gap between the start of a flare-up and getting professional medical care, giving you a way to regain some control.
Temperature Therapy For Quick Comfort
One of the most reliable tools in your home kit is temperature therapy. For a brand-new or acute injury, like a sciatica attack after lifting something heavy, a cold pack is your best friend. Wrap it in a thin towel and apply it for 15-20 minutes. The cold helps reduce the swelling that’s likely squeezing the nerve.
On the other hand, for more persistent, achy nerve pain, a warm compress or a hot bath can work wonders. The heat helps relax the tight, spasming muscles that are often culprits in nerve irritation, increasing blood flow to the area and bringing a sense of soothing relief.
A good rule of thumb is to use cold for the first 48 hours of an acute injury to minimize swelling, and then switch to heat to ease muscle stiffness. But always listen to your body—use what feels best.
Gentle Movement And Positional Changes
When a nerve is angry, your instinct might be to freeze and not move a muscle. Sometimes, that actually makes things worse by increasing stiffness. Instead, try gentle, careful movement.
If sciatica is the problem, simply lying on your back with your knees bent can take pressure off the nerve in your lower back. For a pinched nerve in the neck, a slow, gentle neck tilt held for 15-30 seconds might offer relief. The key is to move slowly and stop immediately if the pain gets sharp or more intense.
These small postural adjustments can make a world of difference for our patients dealing with nerve pain across Illinois communities like Palos Heights and Worth.
Hydration And Its Role In Nerve Function
It sounds almost too simple to be true, but your nervous system runs on water. Nerves need to be properly hydrated to send electrical signals efficiently. When you're dehydrated, that communication can get fuzzy, sometimes making neuropathic symptoms feel even worse.
Making sure you drink enough water throughout the day is a foundational habit. It creates an internal environment where your nerves can function at their best, supporting every other treatment you're trying—from these home remedies to the advanced medical care we provide in Illinois communities like Orland Park and Bridgeview.
When you’ve exhausted the at-home remedies and that relentless nerve pain is still disrupting your life, it’s a clear signal that the irritated nerves need a more direct approach. For many of our patients across Illinois, from Evergreen Park to Orland Park, this is when medications become the right next step.
The goal isn't just to cover up the pain. It's to calm the source: the nerves themselves.
Think of a misfiring nerve like a faulty car alarm—it’s sending loud, frantic signals even when there’s no danger. The right medications work to recalibrate this system, essentially turning down the volume and restoring quiet.
Beyond Standard Pain Relievers
It’s a common frustration: over-the-counter pain relievers like ibuprofen or acetaminophen just don’t touch nerve pain. That’s because they’re designed to fight inflammation or general pain, not the complex nerve-signaling problem at the heart of neuropathy.
Instead, we focus on specific classes of prescription medications that are proven to quiet the nervous system. The two most effective categories are anticonvulsants and certain antidepressants. While originally developed for other conditions, they have become mainstays in treating nerve pain because they work on the right pathways.
Anticonvulsants: The Nerve Stabilizers
Anticonvulsants, also known as anti-seizure drugs, are often our first-line choice for calming overactive nerves. They work by slowing down the erratic electrical impulses firing off in the nerves, much like a dimmer switch tones down a bright, flickering light. For someone in Palos Heights, Illinois dealing with the constant burning of diabetic neuropathy, this can be life-changing.
Prescription medications like gabapentin and pregabalin are proven to calm these overactive nerve signals in the brain and spinal cord. In fact, clinical evidence shows these are first-line therapies. In well-managed treatment, about 50% of patients see a 30-50% reduction in their pain. For example, trials have shown pregabalin can reduce pain by up to 22% at higher doses, compared to just 8.4% with a placebo. You can explore the full study on these gabapentinoid findings to see the data for yourself.
Finding the right dose is absolutely key. At our Chicago Ridge clinic, we always “start low and go slow.” We begin with a small dose and increase it gradually, which helps minimize side effects and pinpoints the lowest effective dose needed to control your symptoms.
Antidepressants: A Dual-Action Approach
It might sound odd to use an antidepressant for pain, but certain types are incredibly effective because they work on the brain chemicals that manage both mood and pain signals. Specifically, they boost serotonin and norepinephrine, two neurotransmitters that are essential for the body's natural pain-suppressing system.
By increasing the levels of these chemicals, these medications essentially turn up the volume on your body's own ability to block pain signals before they reach the brain. This makes them especially useful for widespread nerve pain, like in fibromyalgia or pain radiating from a back injury affecting someone in Hickory Hills or Alsip, Illinois.
The classes of antidepressants we most commonly use for nerve pain are:
- Tricyclic Antidepressants (TCAs): Amitriptyline and nortriptyline are older medications but remain highly effective options for many patients.
- Serotonin-Norepinephrine Reuptake Inhibitors (SNRIs): Duloxetine and venlafaxine are newer choices that often come with fewer side effects.
A Personalized Medication Plan
There is no "one-size-fits-all" pill for nerve pain. The best medication for a patient in Burbank, Illinois with nerve pain after surgery will likely be different from what helps someone in Worth, Illinois with pain from shingles.
Our approach at Midwest Pain & Wellness is always personalized. We build your medication plan based on:
- The specific type and cause of your nerve pain
- Your overall health profile and other medical conditions
- Any other medications you’re taking to avoid interactions
- Your individual response and tolerance to the treatment
By carefully selecting and managing your medication, we can significantly reduce your pain and help you get back to your life—all while prioritizing your safety and avoiding a reliance on opioids.
Using Topical Treatments and Gentle Exercises
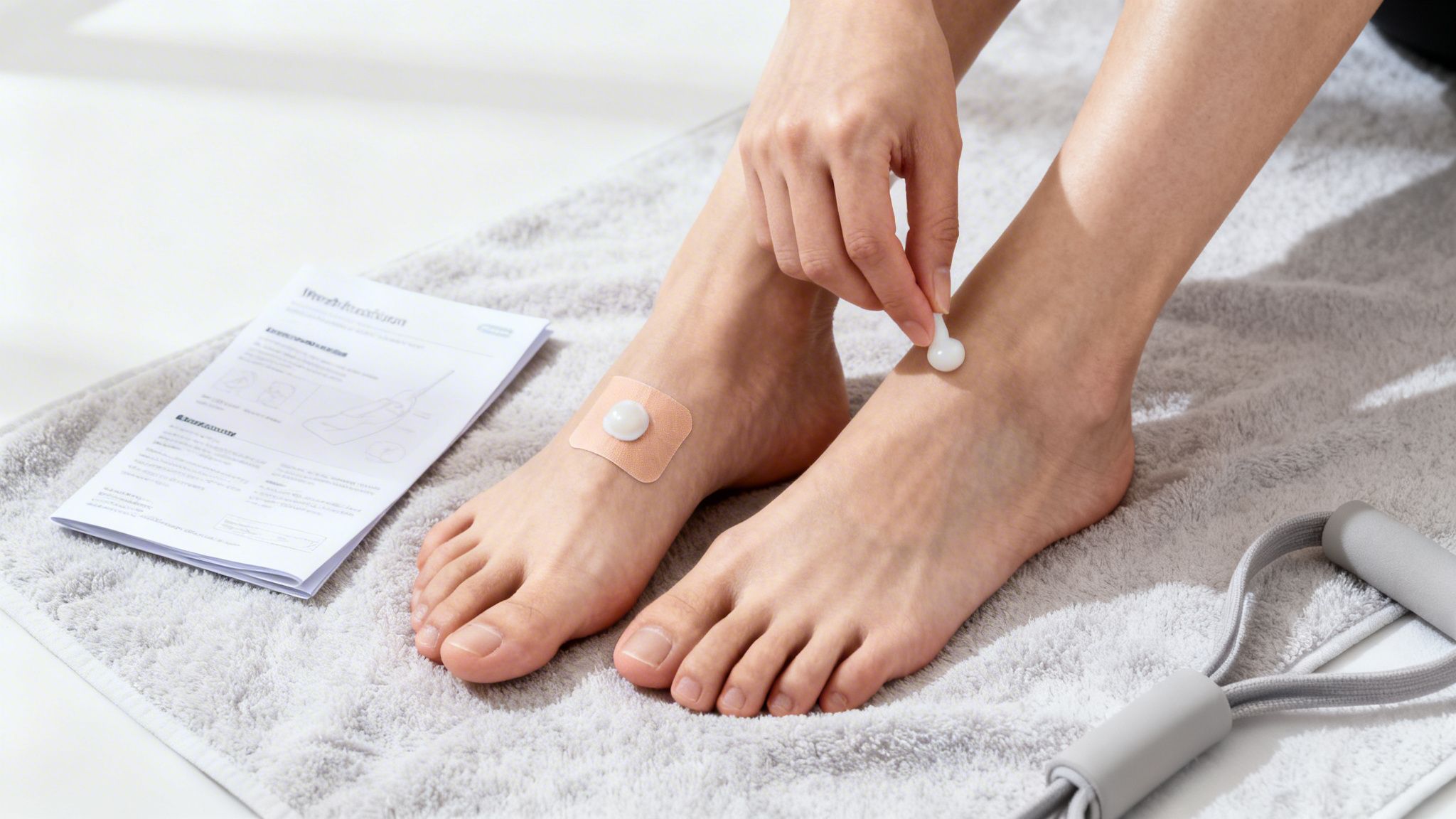
When nerve pain is concentrated in one specific spot—like the burning in your feet from neuropathy or a sharp sting along a scar—systemic medications can sometimes feel like overkill. Why treat your whole body for a problem in one area?
A much better alternative is to go straight to the source with topical treatments. This is a huge advantage: they work right where you hurt, with minimal absorption into the rest of your body. For our patients in Oak Lawn or Palos Hills, Illinois, that means getting relief without the systemic side effects that can come with pills.
Targeted Topical Solutions for Nerve Pain
When your pain is localized, topicals are your first line of defense. The two most common and effective options we rely on are lidocaine and capsaicin. They both target pain, but they get there in very different ways.
Lidocaine, which comes in patches or creams, is a local anesthetic. It works by temporarily numbing the overactive nerve endings in your skin, preventing them from screaming pain signals at your brain. Think of it as a temporary "off switch" for the local pain receptors.
A patient of ours in Palos Heights, Illinois recovering from shingles used a lidocaine patch right over the area where the rash had been. It gave her hours of relief from that lingering nerve pain, known as postherpetic neuralgia, finally allowing her to wear clothing and sleep comfortably.
Capsaicin, on the other hand, is more of a long-term strategy. Derived from chili peppers, it initially causes a warming or burning sensation where you apply it. But with repeated use, it actually desensitizes the nerve endings, depleting them of the chemical they use to transmit pain signals.
These treatments are a low-risk, effective way to tackle pain right where it hurts. Studies show that even low-dose capsaicin can make a real difference for peripheral neuropathic pain. You can discover more insights about these topical treatments and how they compare.
Pairing Treatment with Therapeutic Movement
Applying a cream or patch is an excellent first step, but pairing it with gentle, therapeutic movement can make a world of difference. When nerves are irritated, keeping them completely still can just lead to more stiffness and pain. The right kind of movement, however, improves blood flow, nourishes the nerves, and helps them slide and glide more freely.
This dual approach gives our patients in Illinois communities from Worth to Bridgeview a powerful, non-invasive way to manage their pain and reclaim function.
Nerve Gliding for Better Mobility
One of the most effective techniques we teach is nerve gliding, sometimes called nerve flossing. This isn't aggressive stretching; it's a series of specific, controlled movements designed to gently mobilize an irritated nerve through its pathway. The goal is to free up any spots where it might be getting compressed or stuck.
For someone in Hickory Hills or Alsip, Illinois struggling with carpal tunnel, specific nerve gliding exercises for the median nerve can significantly reduce that tingling and numbness. Likewise, a patient with sciatica can perform gentle leg movements to help the sciatic nerve move more smoothly through the tissues in the hip and leg.
These are slow and deliberate movements.
- For Carpal Tunnel: Extend your arm in front of you with your palm facing up. Gently bend your wrist back as if signaling "stop," hold for a moment, then straighten it. Repeat slowly and smoothly.
- For Sciatica: Lie on your back and bring one knee toward your chest. Slowly straighten and bend that leg, feeling a gentle "flossing" sensation down the back of your thigh.
By combining a topical treatment to quiet the initial pain with these gentle exercises, movement becomes much more tolerable. This creates a positive cycle of relief and improved function for people in Burbank, Evergreen Park, and Orland Park, Illinois, helping you take back control from your pain.
When the usual approaches like home remedies, medications, and physical therapy just aren't cutting it, it’s easy to feel defeated. But for those of us dealing with stubborn, life-altering nerve pain, this is where advanced interventional treatments can make all the difference.
These aren't major surgeries. They are minimally invasive procedures, often done right in our office, that let us target the precise source of your pain with incredible accuracy.
For many of our patients in Illinois, from Hickory Hills to Bridgeview, the thought of a "procedure" can be a little scary. But the reality is that these treatments require very little downtime and can offer profound, long-lasting relief. The goal isn't to just mask the pain—it's to interrupt the pain signals right at the source.
Nerve Blocks for Diagnosis and Relief
One of the most important tools we use is the nerve block. This is a targeted injection containing a local anesthetic (to numb the area) and an anti-inflammatory steroid, delivered directly to the nerve that we suspect is causing the problem.
A nerve block does two critical jobs at once:
- It’s a diagnostic tool. If the injection brings immediate, significant relief, we’ve confirmed that we’ve found the right nerve. This is priceless information that helps us build a long-term treatment plan for patients from Alsip to Burbank, Illinois.
- It provides therapeutic relief. The anesthetic offers fast-acting comfort, while the steroid gets to work reducing inflammation. This can bring relief that lasts for weeks or even months.
For someone in Evergreen Park, Illinois with searing pain shooting down their leg, a targeted nerve block can both confirm which spinal nerve is compressed and give them an immediate break from the agony.
A nerve block is key because it answers the crucial question—"Where is the pain coming from?"—while providing a welcome window of relief. This often makes physical therapy much more effective because you can finally move with less pain.
Radiofrequency Ablation for Long-Term Control
Once a nerve block has successfully pinpointed the problem nerve, we can look at a longer-lasting solution: radiofrequency ablation (RFA). This procedure is the next step up, designed to provide relief for many months, sometimes even a year or more.
During an RFA, we use a specialized needle to send a gentle radiofrequency current to the nerve. This creates a tiny lesion that disrupts the nerve’s ability to send pain signals to your brain. It’s like putting a misbehaving nerve into "sleep mode."
Think of a patient in Palos Hills, Illinois with chronic neck pain from arthritis in their facet joints. RFA can quiet the nerves that send those pain signals, giving them back the ability to turn their head without that familiar wince. You can read more about the variety of procedures we use for treatment and how they are customized for different conditions.
Neurostimulation: A Pacemaker for Pain
For the most severe and complex cases of chronic nerve pain, neurostimulation offers a truly innovative solution. The most common type is a spinal cord stimulator (SCS), which works by masking pain signals before they ever reach your brain.
The procedure involves placing small, soft wires near the spinal cord. These wires deliver tiny electrical pulses that you can't even feel. The pulses replace the sensation of pain with a gentle tingling or, in many cases, no sensation at all. You control the device with a small remote, adjusting the stimulation as you need to.
So, who is a good candidate? Imagine a patient in Worth, Illinois who has already had back surgery but still lives with constant nerve pain radiating into their legs (a condition called post-laminectomy syndrome). When other treatments have failed, an SCS can be life-changing.
The best part is that you get to "test drive" the therapy first. We place temporary leads for a trial period of several days so you can see exactly how much relief it provides in your daily life. We only move forward with the long-term implant if the trial is a clear success. This process gives patients in Orland Park, Illinois and beyond real hope when they thought they had run out of options.
Lifestyle Changes That Support Long-Term Nerve Health
Medical treatments are a powerful part of managing nerve pain, but what you do every day is just as critical. Lasting relief comes from building a lifestyle that actively supports your nervous system, not works against it.
Your daily choices can either fuel the inflammation that irritates nerves or create an environment where they can finally start to heal. For our patients in Alsip, Burbank, and Evergreen Park, Illinois, these foundational habits are what make their medical treatments so much more effective.
Adopt an Anti-Inflammatory Diet
The food you eat is one of the most powerful tools you have. A typical diet high in processed foods can drive up inflammation, making nerve pain worse. Shifting to an anti-inflammatory diet helps calm that response from the inside out.
Focus on bringing more of these nerve-supporting foods into your routine:
- Omega-3 Fatty Acids: Found in fatty fish like salmon and mackerel, plus flaxseeds and walnuts. Omega-3s are proven to help reduce inflammation body-wide.
- Antioxidant-Rich Produce: Berries, leafy greens like spinach and kale, and other brightly colored vegetables are loaded with antioxidants that help protect nerve cells from ongoing damage.
- Foods High in B Vitamins: Vitamins B1, B6, and B12 are absolutely essential for nerve health. Good sources include lean meats, eggs, and fortified whole grains.
Even simple swaps—choosing salmon over red meat, or a side of steamed broccoli instead of fries—can make a real difference in your body’s ability to repair and maintain nerve function. You can discover more about the conditions we treat where these dietary shifts are a key part of the plan.
The Importance of Managing Stress
Stress is a major amplifier of all types of pain. When you're stressed, your body is flooded with hormones like cortisol, which increases inflammation and makes your nerves far more sensitive to pain signals.
For anyone living with chronic nerve pain in Palos Hills or Worth, Illinois, stress management isn't a luxury—it’s a core part of the treatment plan. Consistently calming your nervous system can directly lower the volume on pain signals.
- Mindful Breathing: Take a few moments each day to focus on slow, deep breaths. Inhaling for four counts and exhaling for six helps activate your body's "rest and digest" system, promoting calm.
- Gentle Movement: Activities like yoga and tai chi are fantastic. They combine deliberate movement with focused breathing, which helps release both physical tension and mental chatter.
- Mindfulness Practice: Even 5-10 minutes a day using a guided meditation app can help you create distance from the pain-anxiety cycle, giving you more control over your life.
Why Quitting Smoking and Limiting Alcohol Is Non-Negotiable
We have to be direct about this: if you're serious about finding relief from nerve pain, smoking and excessive alcohol use are two habits that must be addressed. They are incredibly destructive to your nervous system.
Smoking constricts your blood vessels, which chokes off the supply of oxygen and nutrients to your nerves—especially the delicate ones in your hands and feet. This starves them of what they need to function and directly worsens conditions like peripheral neuropathy.
Heavy alcohol use is directly toxic to nerve tissue. It also depletes your body of the very B vitamins that are vital for nerve repair. For anyone in Orland Park or Hickory Hills, Illinois who wants lasting relief, continuing these habits is like trying to put out a fire while pouring gasoline on it.
This decision tree helps visualize how we approach care when pain persists after initial conservative treatments.
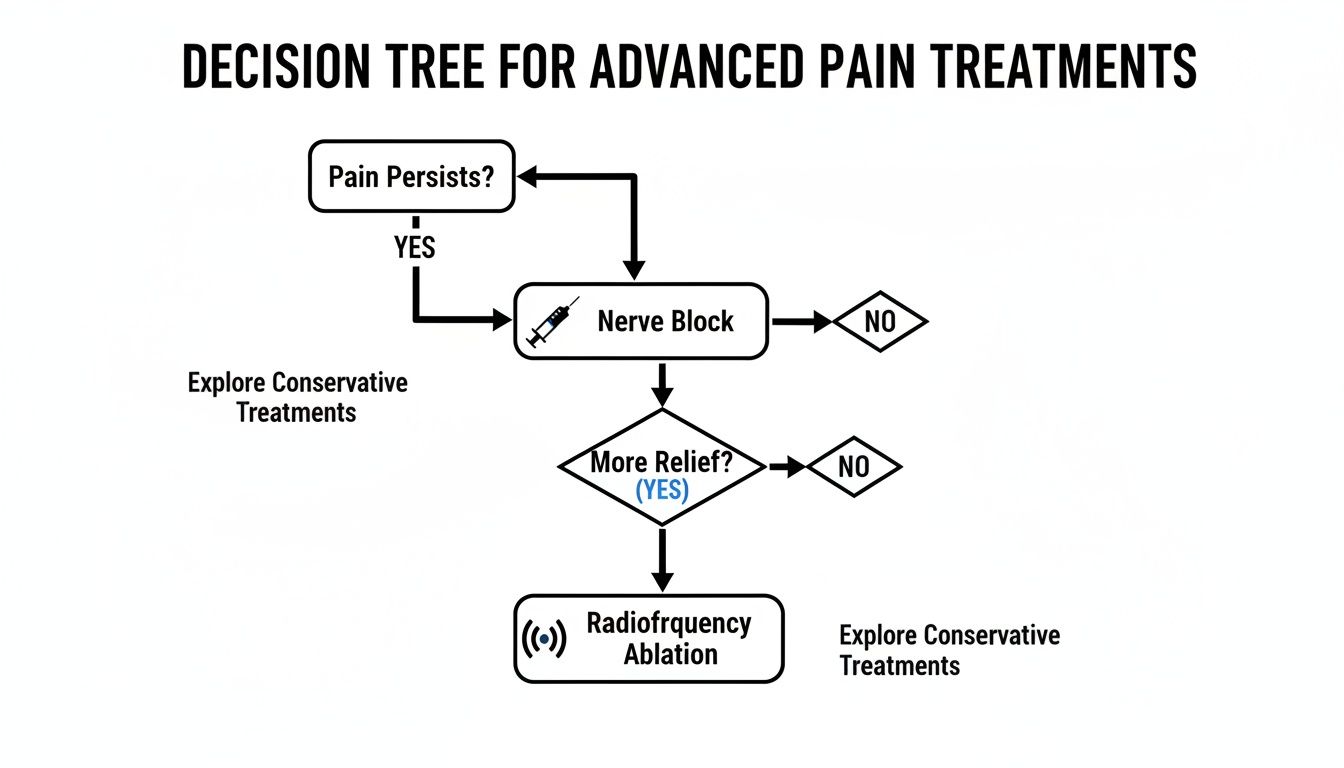
As you can see, if initial therapies don't provide enough relief, a diagnostic nerve block is often the next logical step. If that's successful, it can open the door to a longer-lasting solution like radiofrequency ablation.
When to See a Pain Specialist in Illinois
It’s a question we hear all the time: "Is my nerve pain bad enough to see a specialist?" It's natural to hope the pain will just fade on its own. But toughing it out can sometimes make the problem more stubborn and relief harder to find.
Knowing when to get an expert opinion is one of the most important steps you can take. If you’re in Orland Park, Illinois, or a nearby community, recognizing the signs can make all the difference. Your primary doctor is always the right place to start, but a pain specialist brings a different level of expertise, focusing entirely on finding and treating the root cause of your pain.
Signs It's Time for Expert Care
So, when does manageable discomfort become a problem that needs a specialist? Certain symptoms are clear red flags that your nerve is under serious stress and it’s time to escalate your care.
Don't ignore these signs:
- Persistent Pain: The pain has stuck around for more than a few weeks without improving, despite at-home care or over-the-counter medications.
- Severe Intensity: Your pain is intense enough to disrupt daily life—interfering with work, walking, or getting a full night's sleep.
- New Muscle Weakness: You’re noticing clumsiness, a "foot drop," or weakness in your arms or legs. This suggests the nerve controlling those muscles is in trouble.
- Spreading Numbness or Tingling: The numb or tingling sensation is progressing or moving into new areas.
- Standard Care Isn't Working: The treatments from your primary doctor aren't providing meaningful relief.
If this sounds like what you're going through, it's a clear signal to see a pain specialist. For our neighbors in Palos Heights, Worth, and Bridgeview, Illinois, an early and accurate diagnosis is the key to preventing long-term nerve damage and finally getting relief.
An interventional pain physician is a medical doctor who specializes in diagnosing and treating pain right at the source. Instead of just managing symptoms with pills, they use targeted, minimally invasive procedures to interrupt pain signals and reduce inflammation directly—often avoiding major surgery or a reliance on opioids.
What an Interventional Pain Physician Can Do
When you see a specialist like Dr. Donkoh, the approach is different. The first step is getting to a precise diagnosis. For patients in Hickory Hills and Alsip, Illinois, this might involve advanced diagnostics to find out exactly which nerve is causing the problem and why.
We work closely with your whole care team—your primary doctor, chiropractor, or surgeon—to build a cohesive plan. You can learn about Dr. Donkoh's patient-centered philosophy and see how this coordinated approach works.
From there, we create a personalized plan that goes way beyond medication. For a patient in Burbank, Illinois with leg pain that radiates, this might mean a diagnostic nerve block to confirm the source of the pain. For someone in Evergreen Park, Illinois with chronic nerve pain related to their back, we might explore advanced options like radiofrequency ablation. Our goal is to find the most direct and effective path to get you back to living your life.
Frequently Asked Questions About Nerve Pain Relief
It’s normal to have a lot of questions when you’re dealing with nerve pain. As specialists serving communities from Oak Lawn to Palos Hills, Illinois, we hear the same concerns from our patients every day. Here are some straightforward answers to help you understand your options.
Can Nerve Damage Be Reversed?
This is a big one. While very severe nerve damage can be permanent, that isn't the whole story. Your peripheral nerves actually have a remarkable, natural ability to regenerate. Many of our treatments are designed to create the perfect conditions for that healing to happen.
Even when damage can’t be completely reversed, our goal is to significantly reduce your symptoms and give you your life back. For our patients in Palos Heights and Worth, Illinois, this means finding a way to live comfortably and stay active, even if some of the underlying damage remains.
How Long Do Nerve Pain Treatments Take to Work?
The timeline for relief really depends on the treatment we choose together. There’s no single answer.
- Topical Treatments: Medicated creams and patches often provide relief within minutes to a few hours.
- Oral Medications: Some medications, like gabapentin, need a few weeks to build up in your system to reach their full, pain-relieving effect. It’s a gradual process.
- Interventional Procedures: A diagnostic nerve block can offer immediate, though temporary, relief. More advanced treatments like radiofrequency ablation (RFA) can be a true game-changer for people in Bridgeview and Hickory Hills, Illinois, with relief that builds over a few weeks but can last for many months.
Is Surgery My Only Option for Severe Nerve Pain?
Absolutely not. In fact, surgery is almost always the last resort for nerve pain, not the first step. The entire field of interventional pain management is dedicated to highly effective, minimally invasive treatments that can manage even severe pain without major surgery.
It’s a huge relief for our patients in Alsip, Burbank, Evergreen Park, and Orland Park, Illinois to learn that procedures like nerve blocks, RFA, and spinal cord stimulation are designed to provide powerful, lasting relief without the risks and long recovery that come with a major operation.
Our focus is always on finding the least invasive and most effective solution for your specific pain.
If nerve pain is holding you back, it's time to explore your options. At Midwest Pain & Wellness, we create personalized, opioid-sparing treatment plans for lasting relief. Learn more about our approach and book your consultation by visiting us at https://midwestpainandwellness.com.



