Back pain often takes over slowly. First it changes how you lift a laundry basket, then how long you can sit in the car, then whether you can walk through the grocery store without planning where you might need to stop.
For many adults in the Chicago Ridge area, that pattern feels familiar. You may live in Oak Lawn, Palos Hills, Palos Heights, Worth, Bridgeview, Hickory Hills, Alsip, Burbank, Evergreen Park, or Orland Park. You may have already tried rest, stretching, a round of medication, maybe even chiropractic care or physical therapy, only to find that the pain keeps returning.
The good news is that modern chronic back pain treatment options are broader and more targeted than many patients realize. Effective care is not about chasing temporary relief. It is about identifying the specific pain generator, matching treatment intensity to the problem, and building an opioid-sparing plan that helps you move, work, sleep, and function again.
Your Life with Chronic Back Pain in Illinois
A common story starts on an ordinary Illinois morning. You carry groceries in from the car, twist slightly, and feel that familiar catch in your lower back. By the time you reach the kitchen, your muscles have tightened. Later, the drive to work feels longer than it should. By evening, even getting up from the couch takes planning.

In communities like Oak Lawn, Palos Hills, and Orland Park, people often tell the same version of this experience. They stop walking for exercise. They avoid longer drives. They turn down family outings because standing, bending, or sitting too long will cost them later. Pain starts to organize the day.
When short-term fixes stop working
Many patients have not ignored the problem. They have usually done quite a bit already.
Some have tried:
- Rest and heat: Useful for flare-ups, but often not enough when pain has become persistent.
- Over-the-counter medication: Sometimes helpful, sometimes limited by stomach, kidney, or blood pressure concerns.
- General exercise videos: Better than no movement, but not targeted to the actual source of pain.
- Passive treatments: Massage or occasional adjustments may help temporarily without changing the overall pattern.
At that point, the frustration is not just physical. It is the feeling that no one has explained why the pain keeps coming back.
Back pain is not a single diagnosis. A plan only makes sense after the pain source is narrowed down.
That is where a more specialized evaluation matters. A clinic focused on spine, nerve, and musculoskeletal pain can sort through whether the issue is disc-related, joint-related, nerve-related, SI joint-related, or a combination. If you want to understand the kinds of conditions that fall into that category, the practice’s conditions we treat page gives a useful overview.
A clearer path forward
Patients often do not need more random treatment. They need a sequence. Start with what is most likely to help. Escalate only when necessary. Keep function, safety, and durability in view.
That is the path this guide follows.
Understanding Why Your Back Pain Became Chronic
Not all back pain becomes chronic. Many episodes improve as irritated tissue settles down and normal movement returns. Chronic pain is different. The body does not “forget” the original injury.
The alarm system problem
A useful analogy is a home alarm that becomes too sensitive. At first, it goes off for a specific intruder. Later, it starts reacting to wind, vibration, or a harmless bump against the door. Pain can work the same way.
An injury or strain may start the process. Then inflammation lingers, muscles tighten, sleep worsens, and movement becomes guarded. Over time, the nervous system can become more reactive. That does not mean the pain is imaginary. It means the system that detects danger is now amplifying it.
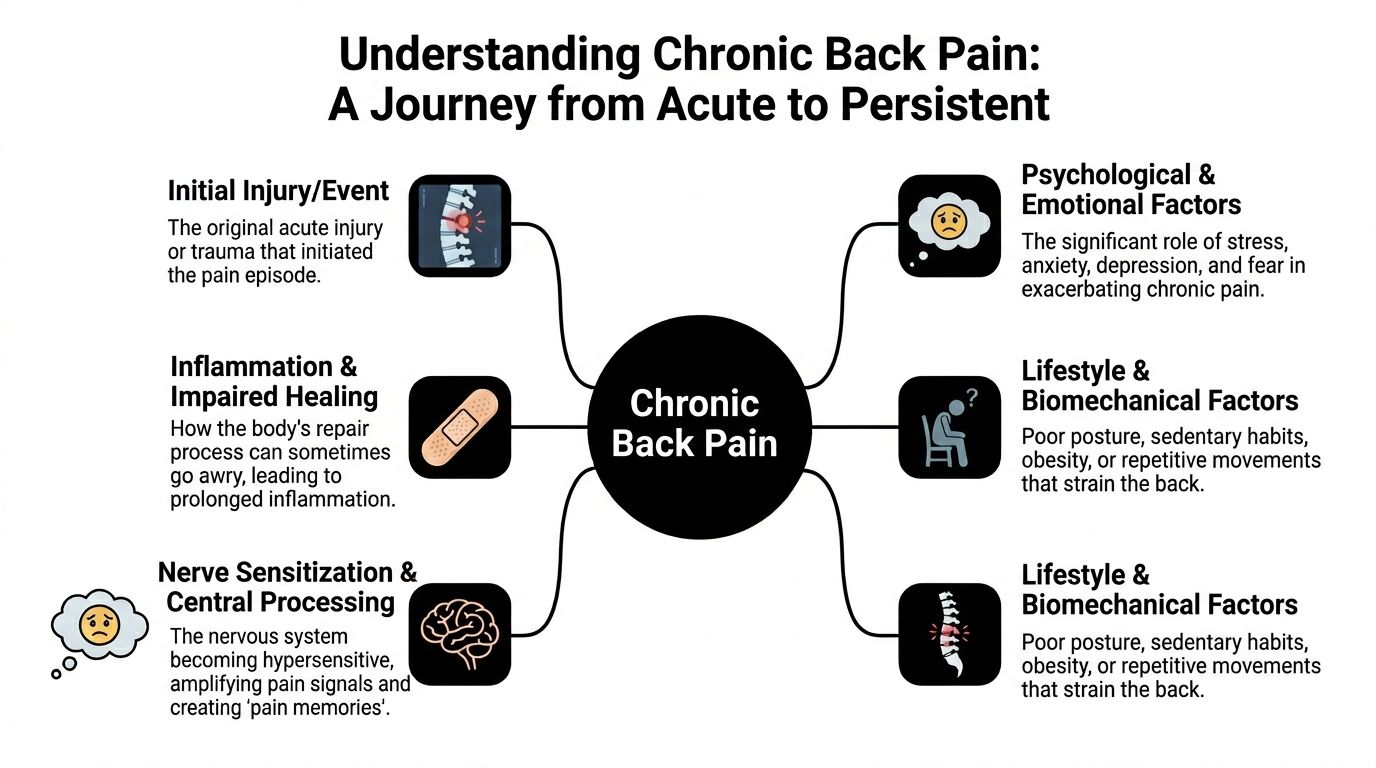
Chronic low back pain is a major public health problem. The WHO identifies low back pain as the leading cause of disability worldwide, and it affects roughly 1 in 4 Americans. The same review also notes that an NIH study found early, appropriate care can reduce work absences and help prevent progression from acute to chronic pain, as summarized by the AAFP review on chronic low back pain.
The main pain generators
“Back pain” is only a symptom label. The actual source may come from several different structures.
Discs
The intervertebral discs act as cushions between the vertebrae. With degeneration, a disc can lose water content, become less resilient, and sometimes trigger deep, aching pain with sitting, bending, or lifting. Some disc problems also irritate nearby nerves.
Facet joints
These are the small joints at the back of the spine. They can become arthritic and inflamed. Facet pain often shows up with standing, twisting, arching backward, or getting out of a chair after sitting.
Sacroiliac joint
The SI joint sits where the spine and pelvis meet. It can mimic low back pain, buttock pain, or even pain that feels like sciatica. Patients often point to one side near the belt line.
Spinal nerves
When a disc bulges, a joint enlarges, or a narrowed spinal canal crowds the nerves, pain may travel into the buttock or leg. Tingling, numbness, burning, or weakness suggest nerve involvement more than a simple muscle strain.
Why diagnosis matters more than labels
The same phrase, “my lower back hurts,” can describe very different problems. One patient needs movement retraining and core stabilization. Another needs treatment aimed at inflamed facet joints. Another has vertebrogenic pain from the endplates inside the vertebrae. Another has spinal stenosis and does better when leaning forward.
That is why successful care starts with pattern recognition:
- Where the pain sits
- What movements trigger it
- Whether it travels down the leg
- What imaging does or does not show
- How the exam behaves in clinic
Good pain treatment is targeted treatment. If the diagnosis is too broad, the results usually are too.
The Starting Point Conservative Care and Pain Management
The first phase of treatment is often the most misunderstood. Patients sometimes think conservative care is just a box to check before more intensive treatment begins. In practice, it is a central part of long-term success.
What the evidence supports
A landmark review published in 2025 found that for chronic low back pain, only about 1 in 10 common non-interventional treatments had moderate-certainty evidence of effectiveness. Among the options that showed benefit were exercise, spinal manipulative therapy, and certain antidepressants, according to the NeuRA summary of the BMJ Evidence Based Medicine review.
That finding matters. It tells patients two things at once. First, not every commonly recommended therapy is likely to help. Second, conservative care still matters when it is evidence-based and well matched to the diagnosis.
Targeted exercise is different from generic exercise
A handout of random stretches is not the same as a directed rehabilitation plan. The point is not to “strengthen your back” in a vague sense. The point is to improve support, mechanics, and tolerance in the structures experiencing strain.
A focused therapy program may work on:
- Core control: Helping the trunk stabilize during sitting, lifting, and transfers.
- Hip mobility: Reducing excess load on the lumbar spine.
- Gluteal strength: Improving how force travels through the pelvis.
- Walking tolerance: Especially useful when deconditioning has become part of the pain cycle.
- Fear-free movement: Rebuilding confidence after months of guarding and avoidance.
For one patient, the main issue is repeated flexion during lifting. For another, it is stiffness and pain with extension. The exercises should reflect that difference.
Medication can support function without becoming the whole plan
Non-opioid medication has a role, but it works best when used strategically.
For some patients, NSAIDs can reduce inflammatory pain enough to make therapy and daily movement more productive. In other cases, medication aimed at nerve sensitivity or mood-related pain amplification can help settle the system enough for rehabilitation to work better.
Trade-offs are important:
- NSAIDs may help, but some patients cannot take them safely because of kidney disease, stomach ulcer risk, bleeding concerns, or cardiovascular issues.
- Neuropathic pain medications may help nerve-related symptoms, but sedation or dizziness can limit use.
- Muscle relaxants may sound appealing for spasms, but they are not always useful long term.
The goal is not to stack prescriptions. It is to use the least medication needed to improve participation in recovery.
Conservative care also includes behavior change
Pain often narrows life. People sit more because walking hurts. Then they lose tolerance. They sleep poorly, then become more sensitive to pain the next day. Stress rises, and muscle tension follows.
A practical conservative plan usually includes:
- Pacing activity instead of boom-and-bust cycles
- Improving sleep habits
- Breaking up prolonged sitting
- Using body mechanics that reduce repeated irritation
- Treating related conditions that add to the burden
Neck tension, headaches, poor sleep, and anxiety around movement can all reinforce pain behavior. Sometimes addressing associated issues changes the back pain picture more than patients expect.
When conservative care is enough, and when it is not
Some patients improve steadily once the diagnosis is clarified and treatment becomes specific. Others get partial benefit, but pain still blocks work, exercise, or daily function.
That does not mean conservative care failed. It may mean the pain generator needs something more targeted. A patient with facet-mediated pain may need diagnostic blocks. A patient with spinal stenosis may need decompression-focused treatment. A patient with vertebrogenic pain may not improve until the basivertebral nerve is addressed.
At Midwest Pain & Wellness, conservative care is often combined with image-guided procedures, rehabilitation, and follow-up adjustments so the plan can evolve rather than stall.
The best conservative plan is active, not passive. It helps you build capacity while reducing the drivers of pain.
Targeted Relief with Interventional Pain Procedures
When exercise, medication, and time do not produce enough progress, interventional pain procedures can help identify and treat the source more directly. The logic is similar to an electrician tracing a short circuit. Before fixing the wiring, you need to know exactly where the problem is.
Diagnostic blocks answer a key question
Some injections are not mainly about long-term relief. They are about precision.
Medial branch blocks
These target the small nerves that carry pain from the facet joints. If a patient’s pain pattern and exam suggest facet arthritis, a medial branch block can help confirm whether those joints are driving the pain.
SI joint injections
Low back and buttock pain can come from the sacroiliac joint and masquerade as disc or nerve pain. A properly placed injection can clarify whether the SI joint is the culprit.
The value of a diagnostic procedure is that it reduces guessing. If a block helps in the expected way, the next step becomes more rational.
Therapeutic injections calm inflammation at the source
Other injections are used to reduce irritation in a defined area.
A few examples:
- Epidural steroid injections may help when inflamed spinal nerves are contributing to leg pain.
- Facet joint injections may be used in selected situations when joint inflammation is the issue.
- SI joint injections can serve both a diagnostic and therapeutic role.
These are not magic shots. Their usefulness depends on the diagnosis, timing, and clinical goal. For some patients, the main benefit is enough pain reduction to restart physical therapy and walking. For others, the relief is brief and mainly confirms the next treatment step.
Radiofrequency ablation offers longer relief for the right patient
Radiofrequency ablation, or RFA, uses heat generated by radiofrequency energy to interrupt pain transmission in targeted nerves. It does not remove arthritis or reverse degeneration. It reduces the nerve’s ability to keep sending the same pain signal.
For facet-mediated pain, RFA is often considered after diagnostic medial branch blocks suggest the correct target. It is more durable than repeating short-lived diagnostic injections.
A related but distinct procedure is basivertebral nerve ablation for vertebrogenic pain. This is designed for a specific group of patients whose MRI shows Modic type 1 or 2 changes, which suggest inflammatory endplate-related pain inside the vertebral body.
Clinical trials of basivertebral nerve ablation showed a 25.95-point reduction in the Oswestry Disability Index at 5 years, indicating substantial functional improvement, with low complication rates, as reported in the published review of basivertebral nerve ablation evidence.
Matching procedure to pain generator
Many treatment journeys go off track at this point. A patient with facet pain gets repeated epidurals. A patient with vertebrogenic pain is sent only to generalized therapy. A patient with SI joint dysfunction is told the MRI looks “not that bad,” even though imaging may not highlight the problem clearly.
A more useful way to think about interventional care is by target.
| Pain pattern | Common target | Possible interventional approach |
|---|---|---|
| Pain worse with extension and twisting | Facet joints | Medial branch blocks, then RFA if appropriate |
| Pain into buttock or leg with nerve irritation | Epidural space and inflamed nerve root | Epidural injection |
| One-sided pain near belt line | SI joint | SI joint injection |
| Deep midline low back pain with Modic changes | Basivertebral nerve | Basivertebral nerve ablation |
Patients who want to understand the range of image-guided options can review the clinic’s procedures we use for treatment for examples of how these interventions are applied.
Procedures work best when they are used as part of a plan, not as isolated events repeated on autopilot.
Real trade-offs to consider
Interventional treatment is appealing because it is targeted and minimally invasive, but it still requires judgment.
Questions that matter include:
- Is this procedure diagnostic, therapeutic, or both
- Is the likely benefit short-term or longer-term
- Will it help the patient return to activity
- Does the history fit the target
- Has imaging been correlated with symptoms, not just read in isolation
The right injection or ablation can move treatment forward. The wrong one can consume time, money, and hope.
Advanced Solutions for Lasting Pain Control
Some patients do everything expected of them and still hurt. They complete therapy, try medications carefully, undergo targeted injections, and continue to struggle with leg pain, post-surgical pain, spinal stenosis, or persistent low back pain that limits walking and standing. That is where advanced options enter the discussion.

Neuromodulation changes the pain signal
Spinal cord stimulation, or SCS, is often described as a pain pacemaker. Small electrical leads are placed near the spinal cord to alter how pain signals are processed before they reach the brain in the usual way.
This approach is not trying to widen a narrowed space or remove a structural problem. It is changing signal transmission.
That makes SCS especially relevant for patients with:
- persistent pain after spine surgery
- chronic radicular pain
- neuropathic leg pain
- refractory back and leg symptoms when other options have not held
A key practical advantage is the trial period. Patients can test whether stimulation meaningfully improves function before committing to permanent implantation.
A 2025 review in Pain Medicine reported that SCS provides over 50% pain reduction in 60 to 70% of carefully selected patients at 5 years post-implant, according to the summary available from Main Line Spine’s discussion of non-surgical chronic back pain treatments.
Minimally invasive decompression fixes a mechanical problem
If neuromodulation changes signaling, decompression changes anatomy. The target here is not the pain message itself. It is the crowding that keeps producing the message.
Patients with lumbar spinal stenosis often describe a classic pattern. Standing and walking trigger back and leg discomfort. Leaning forward, sitting, or using a shopping cart improves symptoms. The issue is space.
For those patients, procedures such as MILD or Vertiflex Superion may be considered in the right clinical setting. These approaches are designed to create more room for neural structures with less tissue disruption than traditional open surgery.
Side-by-side decision making
| If the main problem is | The treatment logic | Examples |
|---|---|---|
| Abnormal pain signaling despite prior care | Modify the signal | Spinal cord stimulation |
| Nerve crowding from stenosis | Create more space | MILD, Vertiflex |
| Compression fracture pain | Stabilize the bone | Kyphoplasty |
| Persistent focal pain after surgery or injury | Reassess target and consider device-based or minimally invasive options | Neuromodulation or selected interventions |
Who tends to benefit from advanced care
These options are usually considered when one or more of the following are true:
- Pain remains function-limiting despite appropriate conservative care
- The diagnosis is specific enough to justify escalation
- The patient wants to avoid long-term opioid dependence
- Prior surgery did not fully solve the pain problem
- A less invasive approach may be preferable to another major operation
In older adults in Worth, Bridgeview, and Hickory Hills, this conversation often centers on walking tolerance and independence. In post-surgical or workers’ compensation cases, the focus may be returning to work capacity and reducing ongoing medication reliance.
Advanced treatment should solve a defined problem. It should not be offered just because simpler treatment took time.
Exploring Regenerative Medicine for Back Pain
Some patients ask a different question. Not “What blocks pain?” but “What might help tissue recover?” That is where regenerative medicine becomes part of the conversation.
What PRP is trying to do
Platelet-rich plasma, or PRP, uses a concentrated portion of your own blood that contains platelets and growth factors. The goal is to deliver those biologically active components to an injured or degenerative area in hopes of supporting repair.
In musculoskeletal care, PRP is more commonly discussed for tendons, ligaments, and certain joints than for every category of spinal pain. That distinction matters. Back pain can come from discs, endplates, facet joints, SI joints, muscles, ligaments, or nerves. A regenerative approach only makes sense if the suspected tissue target is one where healing biology is relevant.
Where regenerative treatment may fit
A thoughtful use of PRP may be considered when:
- the pain source appears related to soft tissue or joint structures
- the patient wants to explore non-surgical options
- conventional treatment has provided incomplete relief
- the expected goal is improved function, not an instant cure
For some people, regenerative care fits best as an adjunct. It may be paired with rehabilitation, movement correction, and other measures rather than replacing them.
Why expectations need to stay grounded
Regenerative medicine attracts interest because it is forward-looking. It also attracts overstatement.
A responsible discussion includes the limits:
- Not all back pain is a regenerative medicine problem
- Not all patients are good candidates
- Technique and diagnosis matter
- Recovery is not immediate
- Evidence varies by condition and target tissue
Cell-based therapies generate even more interest, but for many spine applications they remain investigational. Patients should hear that clearly. Newer does not automatically mean better, and “natural” does not mean proven.
A practical way to think about it
Regenerative medicine belongs in the larger framework of chronic back pain treatment options. It is not a replacement for diagnosis. It is not a substitute for decompression when severe stenosis is the driver. It is not the first choice for every arthritic or disc-related complaint.
It can, however, be a reasonable option for selected patients who want a restorative strategy and understand both the potential and the uncertainty. The right role is selective, informed, and integrated with the rest of the treatment plan.
Your Next Step to Back Pain Relief in the Chicago Area
Most patients do not need more scattered care. They need one coordinated plan built around the actual diagnosis.
That plan may begin with focused rehabilitation and non-opioid medication. It may progress to diagnostic blocks if the pain source is unclear. It may include radiofrequency ablation, epidural treatment, neuromodulation, minimally invasive decompression, or selected regenerative options if those better fit the problem. The sequence matters as much as the treatment itself.
What a good evaluation should answer
A meaningful consultation should clarify:
- What structure is most likely causing the pain
- Whether the pain is mainly mechanical, inflammatory, neuropathic, vertebrogenic, or mixed
- Which treatments are worth trying first
- Which options are unlikely to help and should be avoided
- How to improve function without defaulting to opioids
For patients in Oak Lawn, Palos Hills, Alsip, Burbank, Palos Heights, Worth, Bridgeview, Hickory Hills, Evergreen Park, and Orland Park, local access matters too. Travel is harder when sitting in a car is painful. Follow-up is more realistic when care is close to home.
The right goal
Pain relief matters, but function is the ultimate endpoint. Can you shop without bracing for the aftermath. Can you sit through work. Can you sleep, walk, climb stairs, and return to family routines without constantly calculating the cost.
That kind of improvement usually comes from matching the treatment to the pain generator and adjusting as the response becomes clear. If you are ready to start that process, you can request an evaluation through the clinic’s appointment page.
A careful diagnosis can save months of frustration. It can also help you stop chasing treatments that were never likely to address your type of pain in the first place.
If chronic back pain is limiting your life in the Chicago Ridge area, Midwest Pain & Wellness offers evaluation and opioid-sparing treatment planning for adults in Oak Lawn, Palos Hills, Palos Heights, Worth, Bridgeview, Hickory Hills, Alsip, Burbank, Evergreen Park, Orland Park, and nearby Illinois communities. Schedule a consultation to identify the pain source and build a personalized path forward.



