Pain changes ordinary life first.
You notice it when getting out of bed takes planning, when a short drive through Oak Lawn feels longer than it should, or when work in Palos Hills, Bridgeview, or Burbank leaves your back or neck throbbing before the day is half over. Many people do not start by looking for a specialist. They start by trying to push through, resting on weekends, taking more medication than they want to, and hoping the problem settles down.
For some, it does not.
When pain keeps returning, spreads into the leg or arm, triggers headaches, or makes walking, sleeping, and concentrating harder, it helps to know there is a middle ground between “just live with it” and major surgery. That middle ground is an interventional pain management clinic. It focuses on finding the structure that is creating pain and treating it with targeted, minimally invasive care that supports function and reduces reliance on opioids.
Your Path to Relief Starts Here
People living with ongoing pain often describe the same pattern. They miss family outings. They stop gardening. They sit through a child’s school event while counting the minutes until they can stand up again. In towns around Chicago Ridge, including Evergreen Park, Worth, Alsip, Hickory Hills, and Orland Park, that experience is common enough that many patients assume it is just part of aging or part of recovering from an old injury.
It is not something you have to accept without asking better questions.
An interventional pain management clinic looks at pain as a signal with a source. Instead of only trying to dull the sensation, the goal is to identify whether the problem is coming from an irritated nerve, an inflamed joint, spinal narrowing, a compressed vertebra, or another pain generator. That matters because the treatment changes depending on the source.
This approach has grown because patients want options that are more precise and less disruptive than long-term medication use or large operations. The global interventional pain management market is projected to grow at a 6.5% CAGR from 2025 to 2033, reflecting rising chronic pain rates and strong demand for minimally invasive, opioid-sparing treatment at specialized clinics, according to the interventional pain management market projection.
Why this approach feels different
A targeted procedure is not the same as “getting another shot.”
It usually starts with a careful exam, review of imaging, and a discussion about what pain is stopping you from doing. For one person, that may be standing long enough to cook dinner. For another, it may be sleeping through the night or returning to work after an injury.
Three ideas guide good pain care:
- Restore function: Relief matters, but so does walking farther, bending more easily, and getting back to normal routines.
- Use precision: Image guidance helps place treatment where the problem is.
- Avoid unnecessary escalation: Many patients want to reduce medication burden and delay or avoid surgery when appropriate.
Pain treatment works best when it is tied to a life goal, not just a pain score. “I want to walk the grocery store without stopping” is often a more useful target than “I want zero pain.”
For patients in the southwest suburbs of Illinois, having local access to advanced, opioid-sparing care can make the process less overwhelming. Understanding the options is often the first step toward control.
What is Interventional Pain Management
Interventional pain management is best understood as precision pain medicine.
A simple analogy helps. If your home alarm keeps going off, you can muffle the sound, or you can find the faulty wire or sensor. An interventional pain specialist works more like an electrician for the body’s signaling system. The job is to identify where the pain signal is being generated and interrupt it as accurately as possible.

How it differs from medication-only care
Oral pain medication can help some people, especially for short-term flares. But pills circulate through the whole body. They do not tell you if the problem is the facet joints, the epidural space, the sacroiliac joint, or a specific peripheral nerve.
Interventional care asks more specific questions:
- Is the pain coming from an inflamed spinal nerve?
- Is arthritis in the small joints of the spine driving the problem?
- Is spinal stenosis limiting walking tolerance?
- Is a post-surgical nerve pathway still firing after tissue has healed?
Those questions shape the treatment plan.
Why imaging matters
Most interventional procedures are performed with fluoroscopy (live X-ray) or ultrasound guidance. That imaging acts like a road map. It helps the physician guide a needle or device to the intended structure with far more precision than a blind injection.
That precision can improve both diagnosis and treatment.
For example, if a small diagnostic injection numbs a suspected pain source and your pain pattern changes in the expected way, that information helps confirm what causes the symptoms. In other words, some procedures do double duty. They can relieve pain and clarify the diagnosis.
Where it fits between conservative care and surgery
Interventional pain management is often the space between physical therapy alone and major surgery.
That does not mean it replaces everything else. A strong plan may still include exercise, rehabilitation, sleep support, posture changes, or coordination with a spine surgeon when needed. The point is to use the least invasive treatment that has a real chance of helping.
A useful way to compare the options is this:
| Approach | Main role | Limitation |
|---|---|---|
| Medication-only care | Can reduce symptoms temporarily | May not identify or treat the pain source |
| Interventional pain care | Targets a specific structure with image-guided treatment | Works best when diagnosis and patient selection are careful |
| Surgery | Can address structural problems directly | More invasive and not always the first or best step |
Good interventional care does not chase pain everywhere at once. It tests a theory, confirms the source, and treats the structure most likely to improve function.
For many patients, that clarity is a relief in itself.
Pain Conditions We Treat in the Chicago Ridge Area
Pain rarely arrives with a neat label. A patient from Palos Heights may call it “that ache in my low back.” Someone in Worth may describe “burning down my leg.” A driver from Evergreen Park may say, “My neck pain turns into headaches by afternoon.”
Those descriptions matter. They often point toward different structures and different treatment paths.
Common pain patterns we evaluate
Several conditions commonly bring patients to an interventional pain management clinic in the Chicago Ridge area:
- Chronic low back pain: Often linked to discs, facet joints, sacroiliac joints, or spinal narrowing.
- Neck pain: May come from cervical facet joints, disc problems, muscle irritation, or nerve compression.
- Sciatica: Leg pain, tingling, or burning caused by irritation of a nerve root in the lower back.
- Spinal stenosis: Narrowing around the nerves that can trigger back and leg symptoms, especially with standing or walking.
- Facet joint arthritis: Arthritis in the small joints of the spine that can cause aching, stiffness, and pain with extension or twisting.
- Sacroiliac joint dysfunction: Pain near the beltline or buttock from irritation where the spine meets the pelvis.
- Post-surgical pain: Persistent pain after spine or joint procedures, sometimes involving scar tissue or ongoing nerve irritation.
- Chronic migraine: Recurrent headaches that interfere with work, light tolerance, sleep, and concentration.
- Cervical dystonia: Painful neck muscle contractions that can pull the head into abnormal positions.
- Complex regional pain syndrome: A severe pain condition that may include swelling, color change, temperature sensitivity, and heightened nerve response.
Common conditions and potential interventional treatments
| Condition | Potential Interventional Options |
|---|---|
| Chronic low back pain | Epidural steroid injections, medial branch blocks, radiofrequency ablation, sacroiliac joint interventions |
| Neck pain | Cervical epidural injections, facet-based procedures, targeted nerve interventions |
| Sciatica | Epidural steroid injections, selective nerve root treatments |
| Spinal stenosis | Epidural injections, minimally invasive lumbar decompression, Vertiflex evaluation |
| Facet joint arthritis | Diagnostic medial branch blocks, radiofrequency ablation |
| Sacroiliac joint dysfunction | SI joint injections and related image-guided interventions |
| Post-surgical pain | Spinal cord stimulation evaluation, targeted nerve-based treatments |
| Chronic migraine | Botox and other headache-focused interventional strategies |
| Cervical dystonia | Botox and multimodal supportive care |
| Compression fracture pain | Kyphoplasty evaluation |
Some patients have more than one pain generator at the same time. A person in Hickory Hills might have facet arthritis plus spinal stenosis. An older adult in Alsip may have a compression fracture on top of chronic degenerative changes. That is why a good evaluation matters more than a long list of services.
For a broader overview of diagnoses commonly managed in this setting, the conditions treated at Midwest Pain & Wellness page gives a useful local reference point.
When symptoms deserve a closer look
You should not assume every flare is “just muscle strain” if you notice any of these patterns:
- Pain that radiates: Symptoms travel into the arm, hand, buttock, or leg.
- Positional pain: Walking or standing worsens symptoms, but bending forward or sitting helps.
- Repeated setbacks: Relief from rest, therapy, or medication fades quickly.
- Function loss: Sleep, work duties, driving, or household tasks keep getting harder.
In plain terms, the goal is not to put a complicated name on your pain. It is to identify what is generating it so treatment can be targeted rather than guesswork.
A Closer Look at Advanced Minimally Invasive Procedures
A good procedure plan should feel logical, not mysterious. Once the pain source is narrowed down, treatment can target the structure that causes trouble, whether that is an inflamed nerve root, an arthritic joint, a narrowed spinal canal, or a muscle group sending the wrong signals. The goal stays the same across all of these options. Reduce pain enough to restore walking, sleeping, working, and rehabilitation, while relying less on opioid medication.
Radiofrequency ablation
Radiofrequency ablation, or RFA, is often used for pain coming from arthritic facet joints in the neck or low back.
Here is the simple version. Small nerves carry pain signals from those joints to the brain. RFA uses controlled heat to interrupt those signals. It does not reverse arthritis. It reduces the volume of a pain message that keeps firing long after the joint has become irritated.
A 2017 review on interventional pain techniques in the National Library of Medicine noted that radiofrequency ablation can provide months of relief for carefully selected patients, and that spinal cord stimulation also shows better long-term results when screening is done thoughtfully. That point matters in real life. The right procedure depends less on the name of the treatment and more on whether your pain pattern, exam, and imaging all line up.
RFA usually follows diagnostic medial branch blocks. Those temporary numbing injections work like a test run. If the block briefly relieves the expected pain, that gives your physician better evidence that RFA is targeting the correct nerve pathway.
Spinal cord stimulation
Spinal cord stimulation, or SCS, is used for certain cases of persistent nerve pain, including some patients with post-surgical spine pain or ongoing leg pain after other treatments.
SCS changes how pain signals are processed before they fully register as pain. A useful comparison is a traffic controller redirecting a crowded intersection. The goal is not to remove a disc bulge or repair a worn joint. The goal is to change abnormal pain signaling so daily function improves.
One of the most patient-friendly parts of SCS is the trial phase. Before any permanent implant is considered, the patient tests the therapy for a short period. That helps answer the question that matters most. Does it help you stand longer, sleep better, or get through the day with less medication?
Epidural steroid injections
An epidural steroid injection places anti-inflammatory medication near an irritated spinal nerve.
This is commonly used when pain travels from the neck or low back into an arm or leg, such as sciatica or cervical radicular pain. If a disc bulge or narrowing is inflaming a nerve root, reducing that inflammation can create a better window for movement and therapy.
Patients in the Chicago area often hear mixed advice about epidurals, especially after an urgent care visit, ER visit, or workers' compensation evaluation. The key point is: An epidural does not push a disc back into place. It calms inflammation around the nerve so the body has a better chance to move, heal, and tolerate rehabilitation.
Medial branch blocks and joint-specific injections
Some procedures answer a diagnostic question before they serve as a treatment.
A medial branch block targets the tiny nerves that serve the facet joints. A sacroiliac joint injection helps determine whether pain near the beltline or buttock is coming from the SI joint rather than the lumbar discs or hip. These injections are useful because spine pain can overlap. The place you feel pain is not always the structure creating it.
That is one reason precise, image-guided injections matter. They help avoid guessing. They also help patients and insurers understand why the next step is being recommended.
Minimally invasive lumbar decompression
MILD, short for minimally invasive lumbar decompression, is used for selected patients with lumbar spinal stenosis.
Stenosis means the space around the spinal nerves has become too tight. Many patients describe a very specific pattern. Standing or walking brings on back or leg pain, but leaning forward over a shopping cart gives relief. MILD removes a small amount of tissue contributing to that crowding through a tissue-sparing approach.
For older adults who want to walk farther without jumping straight to major surgery, this can be a meaningful middle ground.
Vertiflex Superion
Vertiflex Superion is another option for carefully selected patients with lumbar spinal stenosis. It acts as a spacer that helps maintain room for the nerves in certain positions, especially standing and walking.
A simple way to picture it is a doorstop that keeps a narrowing space from closing down as much. It is not appropriate for every anatomy pattern, which is why imaging review and symptom matching come first.
Kyphoplasty
When a vertebral compression fracture causes significant back pain, kyphoplasty may be considered.
The procedure is meant to stabilize the fractured vertebra and reduce pain related to collapse. This often comes up in older adults with osteoporosis who develop sudden, severe back pain after what seemed like a small twist, bump, or lift. In that setting, “back strain” is not always the full story.
PRP and regenerative options
Platelet-rich plasma, or PRP, is a regenerative treatment used in selected cases involving certain joints, soft tissues, or chronic pain patterns. Its purpose differs from steroid treatment. Steroids mainly reduce inflammation. PRP is intended to support healing responses in the tissue itself.
Patients should ask practical questions early. Is the diagnosis a good match for PRP? What level of improvement is realistic? Will insurance cover any part of it? In the Chicago Ridge and Orland Park area, that financial piece often affects timing and treatment choice more than clinic websites admit.
Botox for chronic migraine and cervical dystonia
Many patients know Botox from cosmetic medicine, but pain specialists use it for very different reasons.
For chronic migraine, Botox can reduce the frequency and intensity of headaches in selected patients. For cervical dystonia, it can relax overactive neck muscles that are causing pain and abnormal pulling. These treatments show how interventional pain care extends beyond the low back and into neurologic and muscle-based pain conditions that can seriously limit daily life.
How to judge whether a procedure makes sense
Patients usually do best when three questions are answered in plain language:
- What is being targeted? A nerve, joint, epidural space, muscle group, or narrowed area around the spine.
- Why does it fit your symptoms? The treatment should match your pain pattern, exam findings, and imaging.
- What would count as success? Better walking tolerance, easier sleep, fewer flares, improved physical therapy participation, or less reliance on opioid medication.
If you want a local overview of the types of interventions offered in a physician-directed practice, the procedures used for treatment at Midwest Pain & Wellness page lists the main options.
The best procedure is the one that matches the pain generator and the function you want back, whether that means returning to work, handling a workers' compensation recovery plan, or getting through a grocery trip without having to stop halfway.
Your Patient Journey From Evaluation to Lasting Relief
A first visit to an interventional pain management clinic often feels easier once you know the sequence. Most patients do better when the process is predictable.
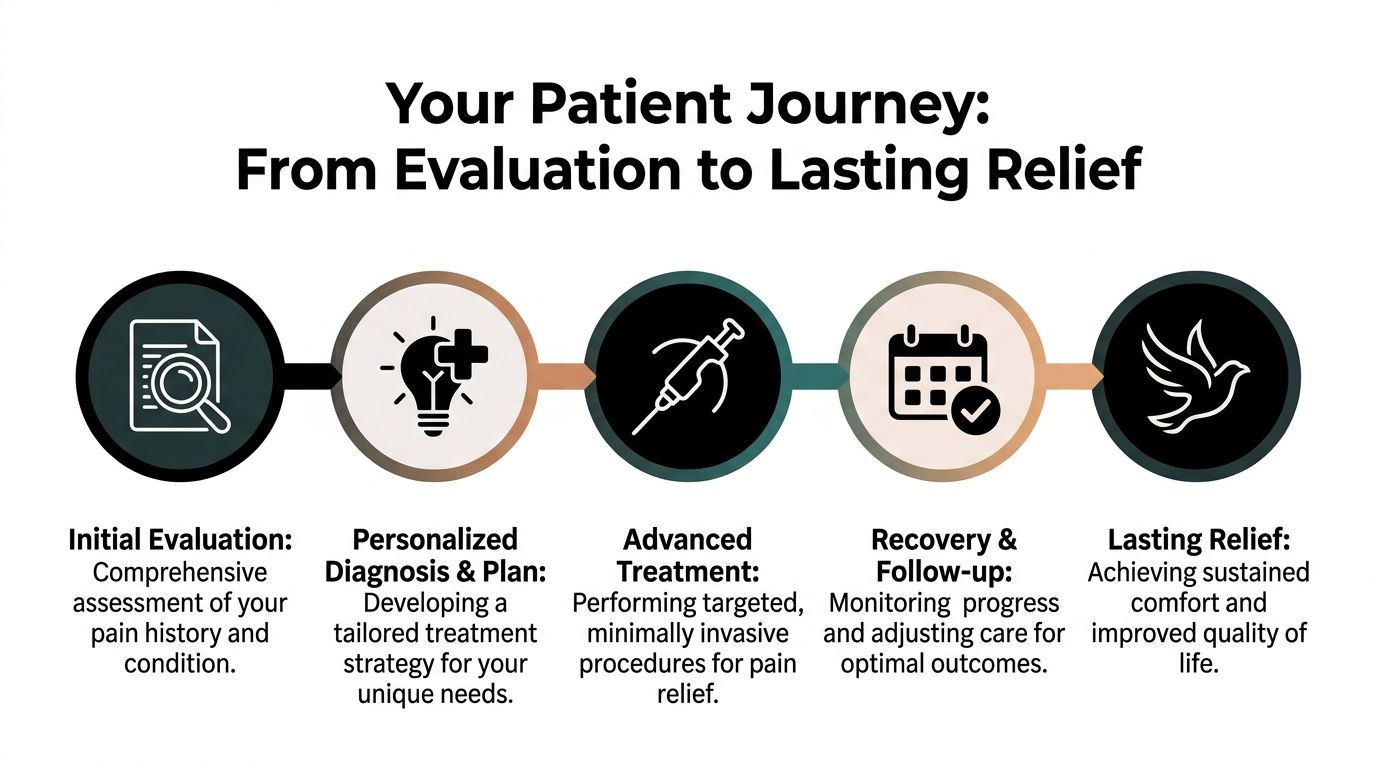
Step one is listening carefully
The evaluation usually begins with your story, not a procedure.
A pain specialist wants to know where the pain starts, where it travels, what makes it worse, what time of day it flares, what treatments you have already tried, and which activities you have lost. If you say, “I can sit fine, but I cannot walk two aisles in the grocery store,” that clue matters. If you say, “Turning my head gives me a stabbing pain into my shoulder,” that matters too.
The exam adds another layer. Range of motion, tenderness patterns, strength, sensation, reflexes, and gait can all help narrow the possibilities.
Diagnosis often happens in stages
Some pain problems are clear from history, exam, and imaging together. Others require a stepwise approach.
A physician may review prior MRI or X-ray studies, request additional imaging if needed, or use a diagnostic block to test whether a specific structure is the likely source. That is one reason interventional pain care can feel more logical than trial-and-error medication changes. It often uses small, focused steps to confirm the target before moving to a longer-acting treatment.
The treatment plan is usually multimodal
A thoughtful plan is rarely just “get an injection and wait.”
It may include:
- Targeted procedure: Such as an epidural injection, SI joint injection, medial branch block, or RFA.
- Rehabilitation support: Physical therapy, home exercise, gait support, or postural work.
- Medication review: Looking for ways to simplify or reduce medicines when safe and appropriate.
- Care coordination: Communication with primary care, rehab teams, surgeons, or case managers. Pain changes movement patterns, and if your pain eases but you never rebuild strength or mechanics, the improvement may not last as well as it could.
What procedure day is usually like
For many in-office procedures, the visit is shorter and less dramatic than patients fear.
You check in, review the plan, confirm the target area, and the physician uses imaging guidance to perform the treatment. Some soreness afterward is common depending on the procedure. Relief may be immediate, delayed, or gradual, depending on what was done and why.
A diagnostic block may work quickly but briefly. A steroid-based injection may take time as inflammation settles. An RFA procedure may involve post-procedure soreness before longer-term improvement develops.
Follow-up is where the plan gets refined
The best follow-up question is not, “Did it help?”
A better question is, “What can you do now that you could not do before?” That answer helps determine next steps. Some patients move on to therapy more effectively after pain settles. Others need a second-stage treatment after a diagnostic response clarifies the source.
Bring a short list to follow-up visits. Note what activity improved, what still triggers pain, and whether sleep, walking, driving, or work changed. That information helps fine-tune care.
Relief becomes more durable when the diagnosis is specific, the treatment is matched carefully, and follow-up turns early progress into regained function.
Navigating Insurance and Workers Compensation in Illinois
You may finally have a clear treatment plan, then hit the part patients rarely expect. Approval rules, claim numbers, medical records, and phone calls can slow everything down.
Prior authorization is one reason. A 2025 ASIPP report noted that 68% of interventional procedures face initial prior authorization denials, as referenced in a Clearway Pain Solutions article on prior authorization barriers in pain care. That does not mean the treatment is wrong for you. It often means the insurer wants the chart to tell the story in a very specific order.

Why prior authorization feels so frustrating
Insurance review works a bit like turning in paperwork for a building permit. You may know the repair is needed, but approval can still stall if one form, note, or image is missing.
For pain procedures, insurers often ask for office notes, imaging, physical therapy records, medication history, and proof that earlier treatment steps were tried first. They may also want documentation showing how pain limits walking, sleep, work, or daily tasks. That last part matters because interventional pain care is meant to restore function, not only lower a pain score for a few hours.
A clinic familiar with this process can help present the record clearly and explain medical necessity in the language insurers expect. That kind of administrative follow-through can shorten delays.
Workers compensation in Illinois adds another layer
Work injury cases often move on two tracks at once. One track is medical. The other is administrative.
If your pain began after lifting at work, repetitive use, a fall, or another job-related injury, your care may involve an employer report, a claim adjuster, work-status updates, outside records, and separate authorization rules. Patients across Chicago Ridge, Oak Lawn, Worth, Bridgeview, and nearby suburbs often discover that the biggest question is not only, "What treatment do I need?" It is also, "Who still needs what document before care can proceed?"
That is why experience matters. A physician who treats pain and understands how these cases are documented can help keep the plan organized. You can learn more about Dr. Donkoh’s background in patient-centered pain care if you want a sense of how that clinical oversight fits into the process.
Questions to ask before procedure day
Good billing conversations protect your treatment timeline. Ask early, while there is still time to correct paperwork.
- What insurance or claim information is already on file
- Does this procedure need prior authorization
- What records are still missing
- Are there likely out-of-pocket costs
- If approval is delayed or denied, what happens next
- For workers comp cases, who receives the treatment note and work-status update
Midwest Pain & Wellness states that it works with workers' compensation and personal injury cases as part of its pain management services. That practical support matters in the Chicago area, where treatment can be delayed by paperwork even when the medical plan is sound.
The goal is simple. Keep care moving so you can return to daily activity, work, and function with less pain and less reliance on opioids.
Why Choose Midwest Pain & Wellness Near Orland Park
A common Chicago-area pain story goes like this. You have already tried rest, medication, maybe therapy, and you still cannot sit through work, sleep comfortably, or get through a grocery trip without paying for it later. At that point, the clinic you choose needs to do more than offer procedures. It needs to give you a clear diagnosis, a realistic plan, and follow-up that helps you function better without building your life around opioids.
Access also matters. The field has been strained in recent years. A 28.9% drop in interventional pain management use from 2019 to 2022 was reported in a 2023 retrospective review from Advocate Health on interventional pain trends and workforce strain. When fewer patients are receiving these services, a physician-led clinic close to home can make a real difference in how quickly evaluation, treatment planning, and follow-up come together.
Patients in and around Orland Park usually ask practical questions first, and for good reason. Pain treatment works like building a map before starting a trip. If the pain source is not identified carefully, even a technically well-done procedure can miss the target.
Here is what many local patients want to know:
- Will the doctor pinpoint the likely pain generator, not just list symptoms
- Is there a plan focused on function, mobility, and daily activity instead of long-term opioid reliance
- Can the clinic coordinate care with imaging centers, surgeons, primary care, or therapy when needed
- Is the location close enough that follow-up visits and repeat procedures are realistic
That last point matters more than many clinic websites admit. Interventional pain care often happens in stages. A diagnostic injection may answer one question. A follow-up visit may refine the diagnosis. A later procedure may provide longer relief. If the office is too far away, patients often delay the very visits that help turn short-term pain reduction into better walking, sleeping, working, and rehab progress.
Physician leadership helps at each step. A board-certified interventional pain specialist is trained to match the story, physical exam, and imaging to the right target, much like tracing a flickering circuit back to the exact wire causing the problem. For patients comparing options nearby, Dr. Donkoh’s training in anesthesiology and interventional pain management explains why that background matters. It supports careful procedural diagnosis, image-guided treatment, and opioid-sparing care designed to restore function.
For many families near Orland Park, the right choice is the clinic that combines technical skill with day-to-day practicality. Midwest Pain & Wellness stands out when that is what you need. Clear communication, local access, and physician-led decision-making can make treatment feel less confusing and more achievable.
Frequently Asked Questions
Do I need a referral to visit an interventional pain management clinic
Sometimes yes, sometimes no. It depends on your insurance plan. Some plans allow direct scheduling with a specialist, while others require a referral from primary care or another physician. If you are unsure, call your insurer and the clinic before booking.
Will I get a procedure on my first visit
Usually, the first visit focuses on evaluation, records, imaging review, and diagnosis. Some patients need another step, such as a diagnostic block or authorization review, before a procedure is scheduled.
How fast do these treatments work
It depends on the procedure. A diagnostic injection may change symptoms quickly. Other treatments can take longer, especially when the goal is reducing inflammation or calming irritated nerves over time.
Are these treatments a substitute for physical therapy
Not always. In many cases, procedures and therapy work best together. A well-timed intervention can reduce pain enough for you to move better, strengthen safely, and get more from rehabilitation.
Can interventional pain care help after surgery
Yes, in some cases. Persistent pain after surgery may come from ongoing nerve irritation, scar-related changes, inflammation, or a different pain generator than expected. A careful evaluation can help determine whether targeted treatment is appropriate.
What should I bring to my first appointment
Bring imaging reports if you have them, a medication list, records of prior treatments, workers compensation or injury claim information if relevant, and a short summary of what activities pain is limiting most right now.
If chronic pain is interfering with work, sleep, walking, or time with family, Midwest Pain & Wellness offers physician-led evaluation and interventional care in the Chicago Ridge area, with treatment options focused on restoring function and reducing reliance on opioids.



