If your back or neck pain feels like a deep, stubborn ache instead of a sharp electric pain, you may have already noticed how confusing that can be. You hurt when you stand too long, lean back, turn to look over your shoulder, or get out of the car, yet scans and generic advice often don't fully explain why.
One common reason is facet mediated pain. This is pain coming from the small joints in the spine that guide motion and help keep the back and neck stable. It’s common, often missed, and very treatable when the diagnosis is precise.
For people in Oak Lawn, Palos Hills, Palos Heights, Worth, Bridgeview, Hickory Hills, Alsip, Burbank, Evergreen Park, Orland Park, and nearby Illinois communities around Chicago Ridge, understanding this condition can be the first real step toward moving better again, sleeping better, and relying less on opioid medication.
Your Guide to Understanding and Treating Facet Pain
Many patients describe the same pattern. The pain sits close to the spine. It’s aching, nagging, and mechanical. It often flares when they extend the back, twist, or stand in one place. It may not travel down the arm or leg in the dramatic way people expect from a pinched nerve.
That pattern matters because facet-mediated pain is a leading cause of chronic low back pain, and chronic low back pain affects a significant portion of adults globally over age 45. In patients seeking help for chronic pain, diagnostic studies confirm the facet joints are the source in 15-45% of low back cases, 34-48% of mid-back cases, and 27-67% of neck pain cases according to AAPM&R’s overview of facet-mediated pain.
Why this diagnosis gets missed
Facet pain can look ordinary on the surface. People call it “arthritis,” “a bad back,” “neck tension,” or “just getting older.” But those labels don’t tell you which structure is generating pain.
Facet pain also overlaps with other spine problems. That’s where patients get understandably frustrated. They’re told they have wear and tear, but they still don’t know what is causing the pain they feel every day.
Practical rule: If your pain is mostly in the neck, mid-back, or low back itself, and certain movements reliably trigger it, the small joints in the spine deserve a close look.
A reassuring starting point
This is not a mystery diagnosis when it’s approached carefully. A good pain evaluation looks at your symptom pattern, your movement triggers, your exam findings, and, when appropriate, targeted diagnostic blocks that test the pain source directly.
For many patients in these Illinois suburbs, the biggest relief is hearing that there’s a structured, non-opioid path forward. You don't have to guess forever, and you don't have to jump straight to major surgery to get help.
What Are Facet Joints and How Do They Cause Pain
Think of your spine as a long chain of bones that has to be both stable and flexible. Each segment has to let you bend, turn, and straighten up without collapsing under the load of everyday life.
The facet joints are part of that system. The easiest way to picture them is as small hinges on a door.
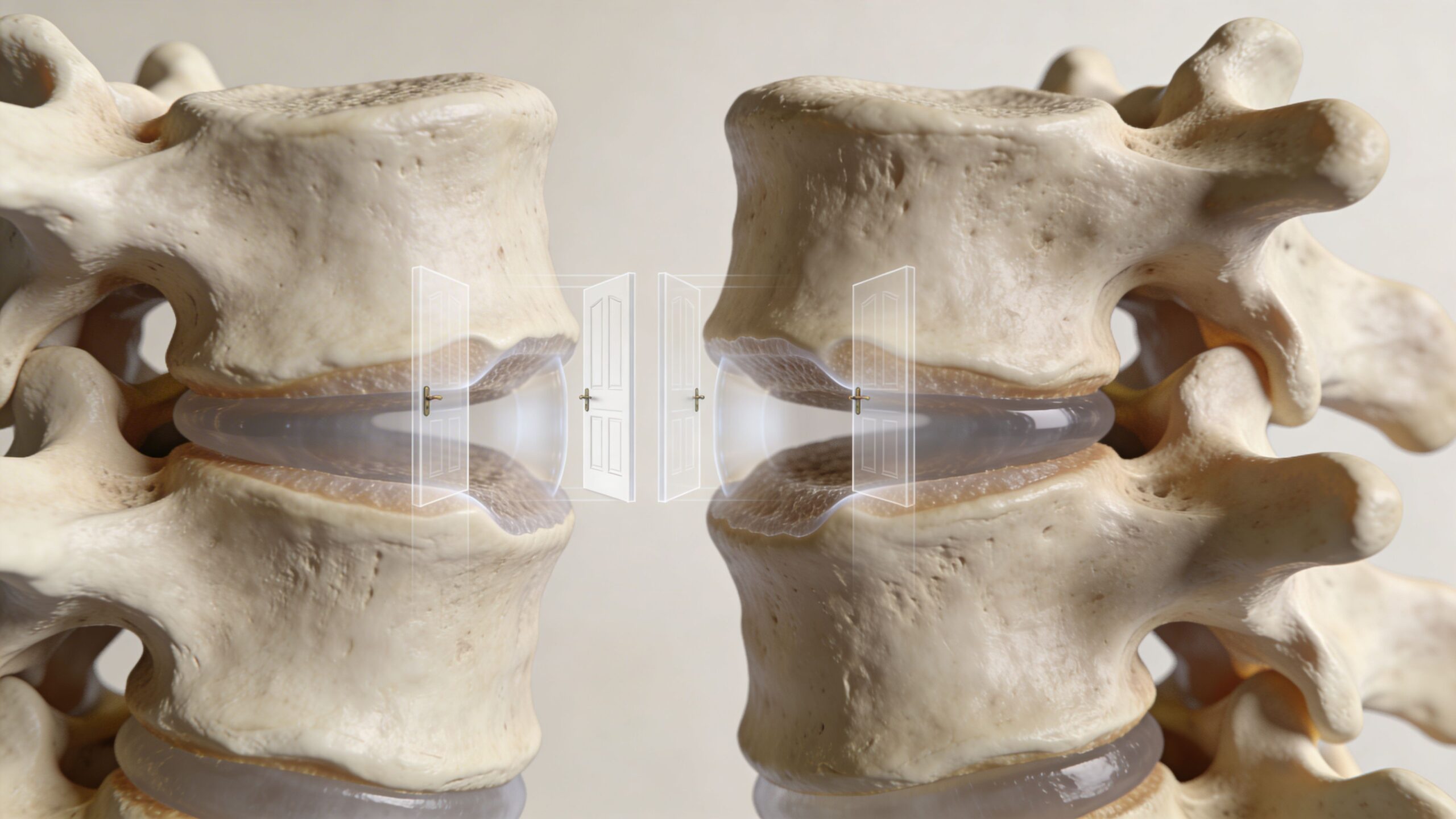
The hinge analogy
A door hinge doesn’t do the same job as the door panel. It guides motion. It keeps the movement controlled. If the hinge gets rusty, irritated, or worn, the door may still move, but it won’t move smoothly.
Facet joints work the same way.
- In the neck, they help guide turning and looking up.
- In the mid-back, they help coordinate movement around the rib cage and posture.
- In the low back, they help manage load and control bending and twisting.
These are synovial joints, which means they’re real joints with a capsule and joint surfaces. When they become irritated or degenerate, they can become a pain generator all by themselves.
What goes wrong
Facet mediated pain can arise when the joint lining becomes inflamed, the capsule gets irritated, or arthritic change alters how the joint moves. The pain signals are carried by the medial branch nerves, which supply these joints.
That detail matters because treatment targets the nerve pathway carrying the pain signal, not the large nerves that control leg or arm strength.
A few common mechanical examples help:
- Repeated extension can increase pressure on the joints.
- Twisting under load can stress the capsule.
- Age-related osteoarthritis can make the joint less forgiving.
- Prior injury can change how that spinal segment moves.
Facet pain versus disc or nerve pain
Patients often hear “back pain” as if it’s one thing. It isn’t. Different structures create different pain patterns.
| Problem source | Typical feel | Common pattern |
|---|---|---|
| Facet joint pain | Deep, dull, aching, mechanical | Worse with extension or rotation, often stays near the spine or refers in a non-radicular pattern |
| Disc or nerve root irritation | Sharp, burning, shooting, electric | More likely to travel down an arm or leg, sometimes with numbness, tingling, or weakness |
That distinction isn't perfect in every person, but it’s a very useful starting point.
If you're trying to understand other painful spine conditions that can overlap with this diagnosis, Midwest’s overview of conditions we treat gives a broader picture of common spine and nerve pain patterns.
Facet pain is a joint problem first. It often behaves like a painful hinge, not like a trapped wire.
Recognizing the Symptoms of Facet Pain
Facet mediated pain has a recognizable “signature,” although not every patient reads the textbook. Patients generally don't describe it as lightning, burning, or shocking. They describe it as stiff, deep, sore, tight, or aching.
That’s why many people live with it for a long time before anyone names it accurately.
Common patterns in the low back and neck
In the low back, facet pain often sits on one or both sides of the spine. It may spread into the buttock, hip area, or upper thigh, but it usually doesn't behave like classic sciatica.
In the neck, patients often notice pain while looking up, turning to reverse the car, or holding the head in one position for too long. The discomfort may spread into the upper shoulder or between the shoulder blades.
Typical clues include:
- Pain with leaning back because extension increases contact pressure at the facet joints
- Pain with twisting such as rolling over in bed or turning to reach
- Morning stiffness or end-of-day ache after prolonged posture
- Localized tenderness close to the spine
- No clear nerve deficit such as obvious arm or leg weakness from a pinched root
Referred pain can be misleading
Facet pain can travel, but it tends to travel in predictable, non-radicular patterns. That means the pain is referred from the joint, not caused by a compressed nerve root.
Classic studies on cervical facet pain found that irritation at C3/4 can refer pain to the suboccipital region, C5/6 can cause pain in the scapular or shoulder area, and C6/7 can create an interscapular ache, as described by ASRA’s review of facet joint pain.
Patients often get confused here. They assume shoulder blade pain must be a shoulder injury, or headache-like pain must be “just stress.” Sometimes a neck facet joint is the source.
What facet pain usually is not
Facet pain usually does not look like this:
- Electric pain racing below the knee or down the arm
- Progressive numbness
- Clear muscle weakness
- Loss of reflexes
- A classic pinched-nerve picture
That doesn't mean someone can't have more than one issue at the same time. They can. But when the story is mostly axial pain, movement-provoked pain, and aching referral, facet joints move higher on the list.
If your pain is worse when you arch, twist, or stand, and less like a shock down the limb, the problem may be coming from the joints that guide spinal motion.
A plain-language self-check
Patients often find this simple checklist helpful:
- “It hurts when I straighten up.” That points toward extension-sensitive structures like facets.
- “It stays in my neck or back.” Localized pain is common with facet problems.
- “It goes to my shoulder blade or buttock, not all the way down.” Referred pain can do that.
- “My arm or leg strength feels normal.” That leans away from major nerve root compression.
None of that replaces an exam, but it helps make the condition easier to recognize.
How We Accurately Diagnose Facet Mediated Pain
A lot of patients from Oak Lawn, Orland Park, and nearby suburbs come in with the same reasonable question: “If this joint is the problem, why didn’t my scan settle it?”
The short answer is that facet pain is diagnosed more like a mechanical problem than a picture-reading problem. A door hinge can look worn and still swing smoothly. Another hinge can look only mildly aged but pinch every time the door opens. Facet joints work the same way. We have to match what you feel, how your spine moves, and how the joint’s nerve supply responds to a focused test.
Why scans don't tell the whole story
MRI and CT scans can be helpful, but they do not prove which structure is causing pain. Many adults have facet arthritis on imaging and feel little or nothing from it. Others have pain that behaves exactly like an irritated facet joint even though the scan looks less dramatic than expected.
That is why we do not rely on imaging alone.
Instead, we build the diagnosis in layers. Your story comes first. Then we examine how your spine behaves under load and movement. Imaging helps us rule in or rule out other causes, and a diagnostic injection helps confirm whether the painful hinge is the source.
The office evaluation
A careful visit usually starts with a few very practical questions:
- Where is the pain centered?
- Which movements set it off?
- Does it stay local, or does it refer into the shoulder blade, buttock, or upper thigh?
- Are there signs that suggest a nerve problem, such as numbness, weakness, or balance trouble?
The physical exam adds another piece. Facet joints often hurt when they are compressed by extension and rotation, so those movements can reproduce a familiar pattern. We also check strength, sensation, and reflexes. If those are intact, the picture leans more toward a joint source than a pinched nerve.
No single exam finding makes the diagnosis by itself. The value comes from the pattern.
The most useful confirmation test
The clearest way to test suspected facet pain is with diagnostic medial branch blocks. These are small injections placed under fluoroscopic guidance near the tiny nerves that carry pain signals from the facet joints.
Patients sometimes worry that this means a big procedure. It is a very focused test.
The goal is simple: temporarily numb the nerve serving the suspected joint and see whether your usual pain drops in a meaningful, clearly trackable way. If the hinge stops sending pain while the numbing medicine is working, that gives us much better evidence that we found the right structure.
Why two blocks matter
One block can be helpful, but two blocks improve accuracy. That matters because local anesthetic can occasionally spread to nearby tissues, and some patients can feel temporary relief for reasons unrelated to the facet joint itself.
Using two carefully interpreted medial branch blocks lowers the chance of calling the wrong structure the pain generator. In plain terms, it helps us avoid treating the wrong hinge.
That is especially important if your goal is lasting relief without opioids. A precise diagnosis gives us a much better chance of choosing a treatment that fits the mechanics of your pain instead of masking symptoms for a short time.
Clinical focus: Good pain care identifies which structure is producing the pain, then matches treatment to that structure.
What patients usually want to know
Here is the process in plain language:
- You describe the pain pattern and what movements trigger it.
- We examine how your neck or back moves and whether the pattern fits an irritated facet joint.
- We review imaging without over-calling it.
- Fluoroscopy-guided medial branch blocks test the joint’s nerve supply directly.
- If the response is clear and reproducible, the diagnosis becomes much more reliable.
This step-by-step approach helps patients avoid guesswork. It also gives people who want to stay active, keep working, care for family, and reduce reliance on opioid medication a more direct path toward the right treatment.
Your Personalized Treatment Plan at Midwest Pain & Wellness
Once we know the painful structure is a facet joint, the plan becomes more specific. Instead of treating “back pain” or “neck pain” as one broad problem, we treat the irritated hinge and the movement patterns around it.
The goal is simple. Reduce pain enough for you to move better, stay active, sleep more comfortably, and rely less on opioid medication.
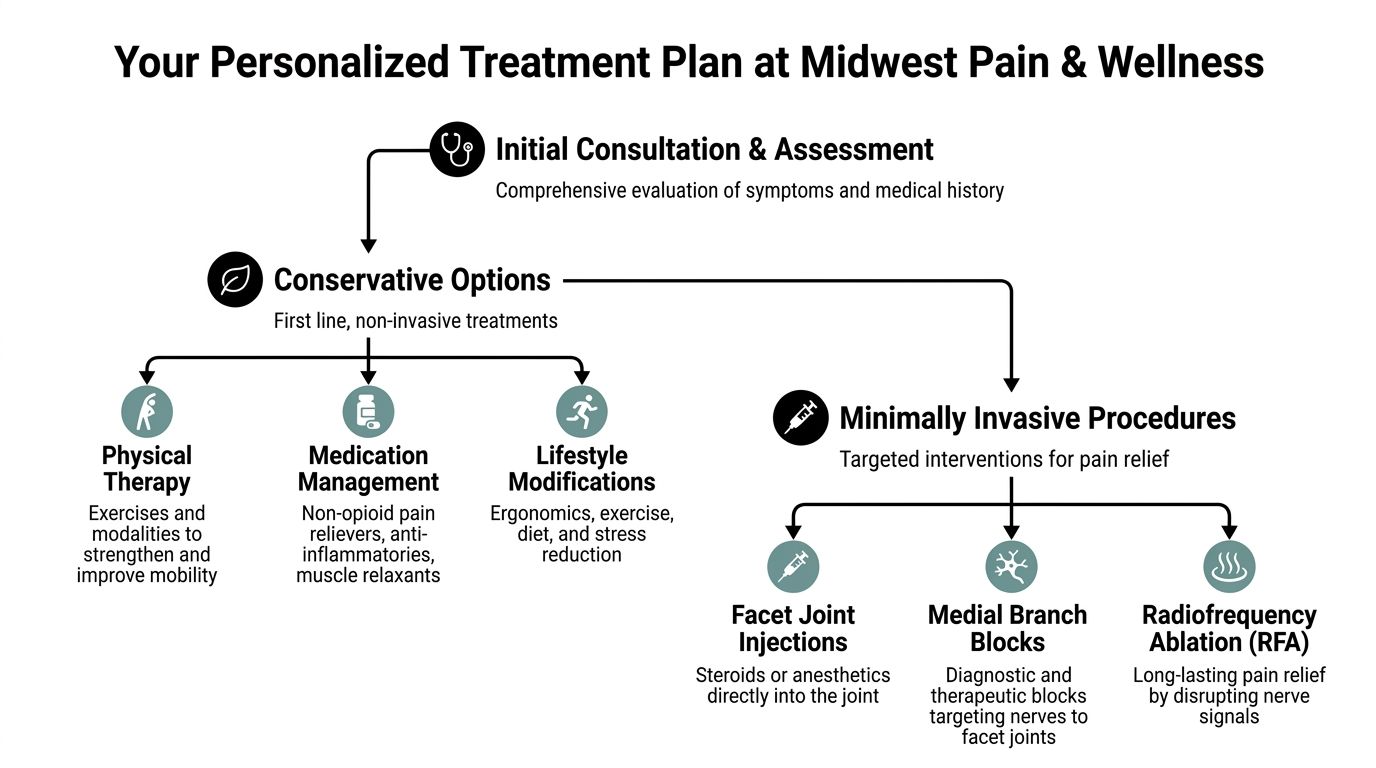
First-line care that supports the painful joint
A sore hinge affects the whole door. It may stick, swing unevenly, or make the frame work harder. A painful facet joint does something similar in the spine. Muscles tighten to protect the area, nearby segments take on extra stress, and ordinary movements start to feel unreliable.
That is why treatment often begins with measures that calm the joint and improve the way the area moves.
Conservative care may include:
- Targeted physical therapy to improve mobility, reduce muscle guarding, and build support around the involved spinal segment
- Activity modification to reduce repeated extension, twisting, or long periods in one position that keep irritating the joint
- Non-opioid medication strategies when appropriate, especially when inflammation or muscle spasm is adding to the problem
- Ergonomic changes for driving, desk work, lifting, and sleep position
This phase is not about asking you to tolerate pain. It is about reducing mechanical stress on the joint so rehab has a fair chance to work.
Injections and nerve treatments each have a different job
Many patients in Oak Lawn, Orland Park, and nearby Illinois suburbs come in hearing the word “injection” as if it describes one treatment. In spine care, that word covers several very different tools. The difference matters because each one answers a different question.
| Option | Main role | What it helps answer or do |
|---|---|---|
| Facet or related anti-inflammatory injection | Reduce joint irritation | May settle a painful flare so daily activity and therapy are more tolerable |
| Medial branch block | Confirm the pain source, sometimes with brief relief | Tests whether the small nerves serving the facet joint match your pain pattern |
| Radiofrequency ablation | Provide longer relief after the diagnosis is confirmed | Interrupts pain signaling from the medial branch nerve |
For patients comparing options, Midwest Pain & Wellness outlines procedures we use for treatment such as medial branch blocks and radiofrequency-based care for spine pain.
Why radiofrequency ablation can help
Radiofrequency ablation, or RFA, is often the next step after the diagnosis is clearly established.
The hinge analogy still applies here. The facet joint is the sore hinge. The medial branch nerve is the small wire carrying the hinge’s complaint to the brain. RFA places controlled heat on that wire so it stops sending the same pain signal for a period of time.
Patients are often relieved to hear what RFA does not do. It does not fuse the spine. It does not remove bone or disc tissue. It does not create medication dependence.
It is a targeted, image-guided treatment meant to quiet a confirmed pain pathway.
Who tends to benefit most
The patients who usually do best are the ones whose full picture lines up. That includes a pain pattern that fits facet pain, exam findings that support it, and clearly positive diagnostic blocks before any longer-acting procedure is chosen.
Common features include:
- Pain patterns consistent with facet joint pain
- Clear relief from dual diagnostic medial branch blocks
- Pain increased by extension or rotation
- No stronger competing source, such as dominant radicular pain, taking over the picture
Good selection matters because precision matters. If you treat the wrong hinge, even a well-performed procedure will disappoint.
What an opioid-sparing plan looks like in real life
For many patients, the treatment path is easier to understand when it is laid out plainly:
Define the pain pattern
We sort out whether your symptoms behave more like facet pain, nerve root pain, disc-related pain, or a combination.Calm what can be calmed
Physical therapy, movement changes, and non-opioid medication options help reduce strain on the joint and improve function.Use procedures with a purpose
Some injections are meant to reduce inflammation. Medial branch blocks are meant to confirm the source. RFA is considered only after the target is shown to be correct.Build on the relief
When pain decreases, patients can walk more normally, tolerate exercise better, and return to work, driving, or household tasks with less guarding.Reassess if symptoms return
The treated nerve can recover over time, so some patients need follow-up and, in selected cases, repeat treatment.
The point of a personalized plan is not temporary numbness. It is giving you enough pain control to use your body again with more confidence and less dependence on opioids.
Finding Lasting Relief and Restoring Your Life
Facet mediated pain is treatable, but it helps to set the right expectation from the start. Most patients aren't looking for a miracle phrase on a scan. They want to garden, work, drive, sleep, exercise, and get through the day without planning every movement around pain.
That’s the right goal.
Lasting relief often means durable control, not a once-and-done cure. If you respond well to radiofrequency ablation, the pain relief can last for a meaningful stretch of time, and then the nerve may gradually regenerate. If symptoms return in the same pattern, the condition can be reassessed and treatment can be repeated when appropriate.
What matters most is what that relief allows you to do. When pain drops, patients can move more normally. They can stick with therapy. They can tolerate walking, housework, and errands with less hesitation. They often sleep better because they aren’t waking every time they roll or extend.
For many people in Hickory Hills, Alsip, Burbank, Evergreen Park, Orland Park, and the surrounding Illinois communities, that’s the difference between merely “coping” and regaining part of life.
If your pain fits the pattern described in this guide, a formal evaluation is the next sensible step. You can request a visit through Midwest Pain & Wellness appointments to find out whether facet joints are part of the problem and whether image-guided, opioid-sparing treatment makes sense for you.
A clear diagnosis changes everything. It turns vague back or neck pain into a specific problem with a specific plan.
Frequently Asked Questions About Facet Pain
Is facet pain just another word for arthritis
Not exactly. Arthritis can be one cause of facet mediated pain, but the terms aren’t identical.
Facet pain means the facet joint is acting as the pain generator. Sometimes that happens because of osteoarthritis. Other times the problem includes irritation of the joint capsule, mechanical overload, or post-injury change in how the segment moves.
Can facet pain cause pain away from the spine
Yes. It can refer pain, which is why it can be confusing.
In the neck, the pain may spread into the base of the skull, shoulder area, or between the shoulder blades. In the low back, it may spread into the buttock or hip region. That referred pain is different from classic nerve-root pain that shoots down a limb with numbness or weakness.
If my MRI shows degeneration, does that prove the facets are the problem
No. Imaging can show age-related changes that are not causing symptoms.
That’s why a good diagnosis uses the whole picture, especially your symptom pattern, exam findings, and targeted diagnostic blocks when needed.
Are medial branch blocks treatment or testing
Primarily, they are diagnostic testing. They temporarily numb the tiny nerves that carry pain from the facet joints.
If your usual pain improves in the expected way, that strongly suggests the joint is the source. The blocks may give short-term relief, but their biggest value is helping choose the right next step.
Will I need surgery for facet mediated pain
Not necessarily. Many patients with confirmed facet pain are managed without surgery.
When dual diagnostic blocks clearly identify the joint as the pain source, radiofrequency ablation is often used to provide longer-lasting relief without fusion surgery and without ongoing opioid dependence.
What is recovery like after a medial branch block or RFA
These are commonly outpatient, image-guided procedures. Most patients are able to return to light routine activity quickly, though individual instructions vary.
The important point is that recovery is usually far easier than recovery from surgery. Patients should still follow post-procedure guidance closely and pay attention to how their pain pattern changes afterward.
Can the pain come back after RFA
Yes. The treated medial branch nerve can regenerate over time.
That doesn't mean the procedure failed. It means the pain pathway can reconnect. If the same pain pattern returns and the clinical picture still fits, repeat evaluation can determine whether another treatment cycle is appropriate.
I live in Worth or Bridgeview. How does scheduling and insurance usually work
The practical first step is to schedule an evaluation and bring any prior imaging reports, procedure history, medication list, and details about when the pain occurs. The clinic can then review your history, discuss likely next steps, and help clarify logistics such as insurance, workers’ compensation, or personal injury documentation based on your situation.
How do I know when it's time to get evaluated
Consider getting checked when the pain has become persistent, limits walking, driving, sleep, work, exercise, or daily chores, or keeps returning despite rest and basic care. You should also seek prompt medical attention if pain is accompanied by concerning neurologic symptoms such as progressive weakness, significant numbness, or other urgent changes.
If you're dealing with stubborn neck or back pain in Chicago Ridge or nearby Illinois communities, Midwest Pain & Wellness offers evaluation and interventional pain management options focused on identifying the source of pain and supporting function with opioid-sparing care.



