If you're dealing with chronic migraine or painful neck spasms, you already know how quickly pain can take over a normal week. Plans get canceled. Sleep becomes unreliable. Work, driving, exercise, and even simple family time start revolving around what your head or neck will allow that day.
Many patients across the south Chicago suburbs, including Oak Lawn, Palos Hills, Palos Heights, Worth, Bridgeview, Hickory Hills, Alsip, Burbank, Evergreen Park, Orland Park, and the Chicago Ridge area, are looking for something more targeted than another pill. They want relief that makes medical sense, fits into a long-term plan, and doesn't depend on opioids.
Finding Relief When Chronic Pain Takes Over
Botox often surprises people because they know the name from cosmetic medicine. In pain management, though, Botox is a medical treatment with a very different purpose. It can help calm overactive muscle activity and reduce pain signaling in carefully selected conditions, especially chronic migraine and cervical dystonia.
That distinction matters. This isn't about softening forehead lines. It's about reducing the burden of a neurological or muscular condition that keeps interrupting your life.
For chronic migraine, Botox is FDA-approved and used on a scheduled basis by trained medical professionals. For cervical dystonia, it helps weaken muscles that are contracting too forcefully or too often. In both settings, the goal is the same. Lower the intensity of the problem at its source so you can function better day to day.
Why patients ask about Botox now
People usually reach this question after more basic options haven't done enough. Sometimes oral medications cause side effects. Sometimes they help only part of the way. Sometimes the problem keeps returning and the cycle of pain, missed activities, and rescue medication becomes its own burden.
A few practical reasons Botox becomes part of the conversation:
- It targets the problem locally rather than trying to affect the whole body.
- It fits opioid-sparing care for patients who want alternatives to habit-forming pain treatment.
- It has a defined treatment rhythm for ongoing conditions, which helps with planning and follow-up.
- It serves different pain conditions differently, which is why proper diagnosis matters.
Many patients feel better once they understand that therapeutic Botox isn't a beauty treatment repurposed on a whim. It's a focused medical tool used for specific diagnoses.
The Science Behind How Botox Calms Nerves
If your neck keeps pulling to one side or headache pain keeps returning despite medication, the next question is usually simple. What is this treatment doing inside the body?
The core mechanism is straightforward. Botox temporarily reduces communication between a nerve ending and the muscle or pain pathway it is driving. In practical terms, it quiets an overactive signal instead of masking symptoms throughout the whole body.
A nerve normally releases a chemical messenger called acetylcholine. That messenger crosses a very small gap and tells a muscle to contract. When that signaling becomes excessive or poorly controlled, patients can feel constant tightness, abnormal pulling, spasm, or pain that keeps flaring in the same area.
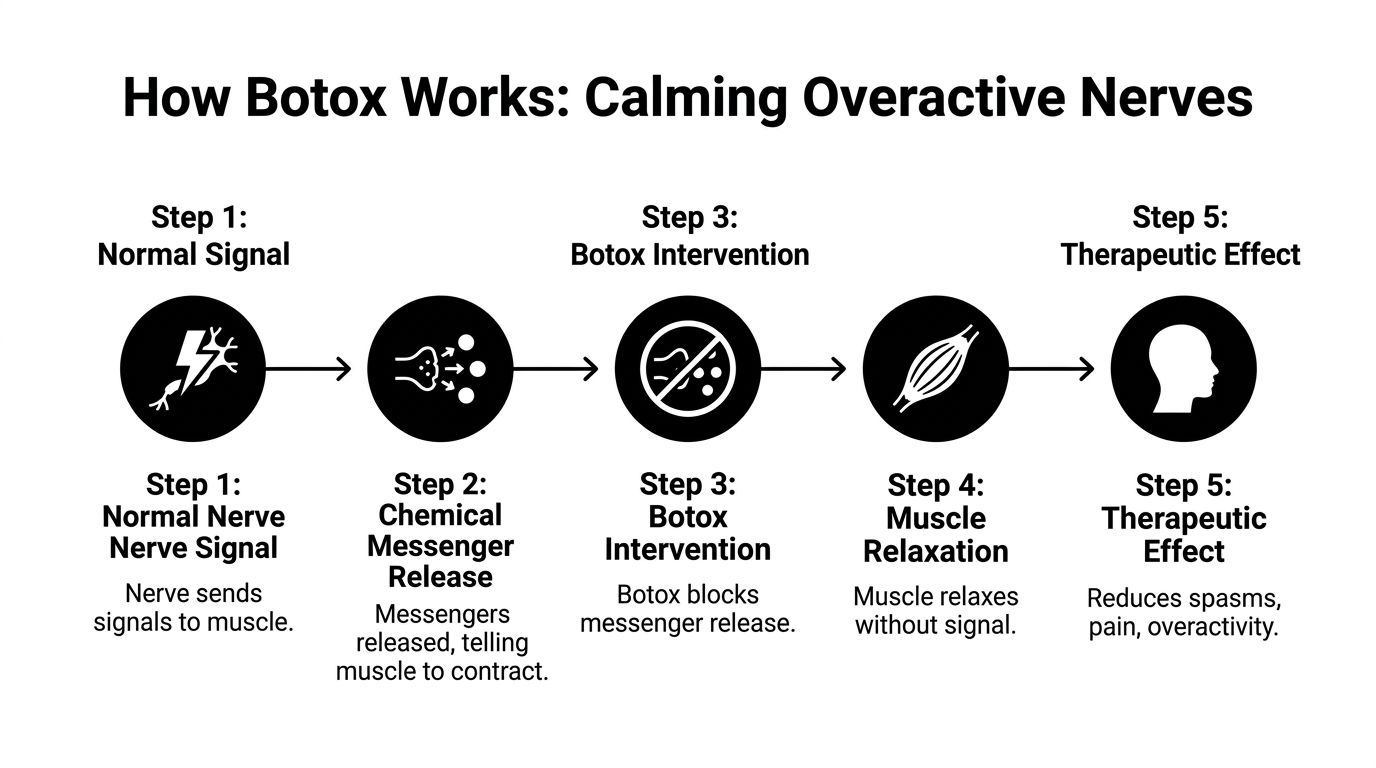
What happens at the nerve ending
After injection, botulinum toxin type A attaches to the targeted nerve ending and enters the nerve terminal. It then interferes with the release process for acetylcholine. The technical details matter less than the result. The message does not leave the nerve as effectively, so the muscle receives less of the command to tighten.
That is why patients often hear Botox described as a signal blocker. It does not burn the nerve. It does not cut anything. It does not permanently damage muscle tissue. The effect fades as the nerve rebuilds its ability to release that messenger.
At a more detailed level, Botox acts on proteins involved in vesicle docking and release. For patients, the practical takeaway is enough. Less chemical signaling means less involuntary contraction in the treated area.
Why that matters for pain care
In cervical dystonia, reducing that signal can ease the muscle overactivity that twists the neck, creates spasm, and causes deep aching fatigue.
In chronic migraine, the story is broader. Botox appears to reduce the release of certain pain-related chemicals around nerve endings, which can lower how easily pain circuits are triggered. That helps explain why some patients in Orland Park, Oak Lawn, and nearby communities consider it when they want an option that is more targeted than taking another pill every day. We often discuss it as one part of a wider plan for neurologic and musculoskeletal pain conditions we treat.
Precision matters here. The benefit depends on choosing the right muscles, the right pattern, and the right dose for the diagnosis.
What Botox does not do
A lot of anxiety comes from cosmetic language, especially the word "freeze." Medical Botox is more controlled than that.
| Concern | What actually happens |
|---|---|
| "Will it kill the nerve?" | No. The effect is temporary, and nerve signaling returns over time. |
| "Will my muscles stop working forever?" | No. The treated muscles gradually recover as the medication wears off. |
| "Will it spread through my whole body?" | Properly administered treatment is intended to act locally in the injected areas. |
There is a real trade-off. If treatment is too conservative, relief may be limited. If too much medication reaches the wrong muscle, weakness can feel awkward or functionally annoying for a period of time. That is one reason therapeutic Botox belongs in a medical pain practice, where anatomy, diagnosis, and follow-up shape the plan.
Why relief is not immediate
Botox starts its work after the injection, but patients do not usually feel the full effect right away. The nerve needs time to reduce chemical signaling, and the treated muscle or pain pathway needs time to settle down. In practice, changes often build over several days and continue to develop over the next couple of weeks.
The larger point is simple. Botox is local, temporary, and targeted. For the right patient, that makes it a useful opioid-sparing tool, especially when oral medications have not provided enough relief or have caused side effects that are hard to tolerate.
Applying Botox for Chronic Migraine and Cervical Dystonia
The same medication can help two different conditions, but it doesn't help them in exactly the same way. That's where a lot of patient confusion starts.
With cervical dystonia, the logic is fairly direct. Certain neck muscles contract when they shouldn't, or they contract with too much force. That can pull the head into an abnormal position, create deep muscle pain, and leave the neck feeling tight, tired, and hard to control. Botox weakens the specific overactive muscles that are driving that pattern.
Why cervical dystonia responds
In dystonia, treatment isn't about relaxing every muscle in the neck. It's about identifying which muscles are overfiring and which ones are compensating. If the wrong muscles get treated, the result can be underwhelming or awkward. If the right ones are treated, patients often notice less pulling, less spasm, and better head positioning.
That selectivity is one reason therapeutic Botox belongs in a medical setting rather than a cosmetic one. The anatomy is more complex, and the goal is function, not appearance.
Why Botox helps migraine even though migraine isn't just a muscle problem
Migraine treatment is more nuanced. In chronic migraine, Botox isn't solely used to relax forehead or neck muscles. It's believed to reduce the release of pain-related neuropeptides such as CGRP and Substance P, which helps reduce neurogenic inflammation and central sensitization.
This is why a patient with head pain may still receive injections in the scalp, temples, neck, and upper shoulder region. Those sites are chosen because they relate to the pain network involved in chronic migraine, not because every painful headache starts as neck tension.
For people who meet the definition of chronic migraine, meaning 15 or more headache days per month, Botox is given every 12 weeks into 31 sites across 7 head and neck muscle areas, according to the Cleveland Clinic explanation of botulinum toxin injections for chronic migraine. The same source notes that Phase III PREEMPT trials found patients had 8.4 fewer headache days per month compared with placebo.
A common question is, "Why inject my neck for a headache?" Because chronic migraine involves pain signaling pathways that extend well beyond where you feel the pain most intensely.
What works and what doesn't
There are a few practical truths that matter here.
- Works best with the right diagnosis. Botox for chronic migraine isn't the same as Botox for occasional tension headaches.
- Works best when the pattern is mapped correctly. Cervical dystonia requires individualized muscle selection.
- Doesn't work like a rescue medication. It's preventive treatment, not something you use once a migraine has fully escalated.
- Doesn't replace good overall care. Sleep, triggers, medication review, and other interventions still matter.
Patients who want to understand whether their condition fits these uses can review common diagnoses on the clinic's conditions we treat page.
Your Botox Treatment Journey in the Chicago Ridge Area
Most patients feel less anxious once they know what the visit looks like. The process is straightforward, but it shouldn't feel rushed.

The first visit is about diagnosis, not just scheduling injections
A proper Botox evaluation starts with the story behind your symptoms. For migraine, that means the pattern of headache days, associated symptoms, what you've already tried, and whether the diagnosis is chronic migraine rather than another headache disorder. For cervical dystonia, the visit focuses on where the neck pulls, which movements trigger pain, how long the symptoms have been present, and what the exam shows.
Patients from Hickory Hills, Alsip, Oak Lawn, and nearby Illinois communities often arrive worried they'll be pushed quickly into a procedure. Good care works the opposite way. The diagnosis comes first, and candidacy follows from that.
Building a treatment plan that fits the condition
Once Botox is considered appropriate, the discussion becomes practical. Which muscles or treatment zones will be targeted? What kind of benefit is realistic? How often will treatment likely be needed? Are there reasons to combine Botox with other therapies rather than use it alone?
This is also when expectations get clarified. For example, migraine patients need to know Botox is preventive. Dystonia patients need to know the aim is improved comfort and function, not perfect symmetry or complete stillness.
A personalized treatment strategy may include Botox alongside other interventional options, which you can see reflected in the clinic's procedures we use for treatment.
What the injection visit feels like
The procedure itself is usually brief. The needle used is small, and most patients describe the sensation as a series of quick pinpricks. Some sites are more noticeable than others, especially in sensitive scalp or neck regions, but the process is generally very manageable.
A typical visit has this rhythm:
- Review the plan so you know where injections are going and why.
- Mark or identify the treatment areas based on anatomy and the pattern of symptoms.
- Administer the injections carefully with attention to placement, dose distribution, and muscle balance.
- Give post-visit guidance about what to expect over the next days and weeks.
The skill isn't just in giving injections. It's in choosing the right targets and avoiding the wrong ones.
Why specialist care matters
This matters most in conditions like cervical dystonia, where one patient's neck pattern may look very different from another's. It also matters in chronic migraine, where consistent technique and accurate protocol-based treatment influence the quality of the result.
For patients coming from Burbank, Evergreen Park, Orland Park, Worth, Bridgeview, and Palos Heights, the treatment day itself is only one part of the process. The more important part is that the injections are tied to a thoughtful diagnosis and a plan for follow-up.
Understanding Treatment Timelines and Results
A patient from Orland Park or Oak Lawn may come in hoping for relief by dinner that same night, especially after months of living around migraine attacks or constant neck spasm. Botox usually does not work on that timetable.
The medication needs time to quiet the nerve signals we targeted during treatment. Some patients notice an early shift within several days. More often, the change becomes clearer over the next 1 to 2 weeks. For chronic pain conditions, I ask patients to look for a trend, not a dramatic same-day result.
What improvement usually feels like
Early benefit can be subtle.
With cervical dystonia, the first sign may be less pulling or fewer spasms before pain improves. With chronic migraine, the change is often fewer headache days, lower intensity, or attacks that are easier to recover from. That matters because Botox is a preventive treatment. Its job is to reduce the burden of pain over time and help you rely less on rescue medication, not to act like a fast-acting rescue shot.
Useful signs of progress include:
- Fewer difficult days over the course of the month
- Less severe flare-ups even if symptoms have not fully disappeared
- Better function at work, while driving, or during sleep
- Less dependence on short-term pain medication as part of an opioid-sparing plan
Those gains may sound modest on paper. In real life, they are often what allow a patient to get through a workweek, attend family events, or stop planning every day around pain.
Why repeat treatment is usually part of the plan
Botox wears off. The treated nerve endings gradually recover their signaling, so the effect is temporary and repeat injections are often needed to maintain benefit.
For many patients, that treatment interval is about every 3 to 4 months. That schedule is not a flaw in the therapy. It is part of using a reversible treatment carefully and predictably. It also gives us a chance to reassess the pattern of pain, adjust dosing or muscle targets if needed, and make sure the treatment is still earning its place in the larger care plan.
Practical rule: Judge Botox by the pattern across the full treatment cycle, not by how you feel later the same day.
Matching the timeline to the condition
| Condition | What patients often notice first | Ongoing expectation |
|---|---|---|
| Chronic migraine | Fewer or less intense headache days | Preventive benefit that usually requires repeat cycles |
| Cervical dystonia | Less pulling, less spasm, improved neck comfort | Temporary muscle relaxation that usually needs maintenance |
The patients who do best usually understand the trade-off clearly. Botox can reduce pain, spasm, and medication use, but it does so gradually and temporarily. For patients in the south Chicago suburbs who want an alternative to more pills, that can still be a very meaningful win.
Is Botox Safe and Are You a Good Candidate
If you live in Orland Park, Oak Lawn, or nearby and you are tired of building your week around pain, safety is usually the first question after effectiveness. That is the right question to ask.
Botox has a long medical history, and in pain practice it is used selectively, not casually. The safety profile is well understood when the diagnosis is correct, the injection plan matches the condition, and the treatment is done by a clinician who regularly uses it for problems like chronic migraine or cervical dystonia. For patients who want an opioid-sparing option, that experience matters.

Common trade-offs patients should know
Most side effects are temporary and limited to the treatment area. Injection-site soreness, bruising, a mild post-treatment headache, or temporary neck discomfort are all things I discuss with patients before we proceed.
The more meaningful question is whether the expected benefit justifies the local weakness Botox can sometimes cause. In the right muscle, that weakness is part of the treatment. In the wrong muscle, or at the wrong dose, it can be frustrating. A migraine patient may notice temporary heaviness in the forehead. A patient with cervical dystonia may get pain relief but also feel that certain neck movements are weaker for a period of time. Good technique lowers that risk, but it does not erase it.
That is why careful muscle selection and dosing matter so much.
Who may not be a good candidate
Some patients should avoid Botox, and others need a more cautious workup first. Reasons to pause or reconsider treatment include:
- Allergy concerns related to the product or its ingredients
- Active skin infection near the planned injection sites
- Certain neuromuscular disorders such as myasthenia gravis or ALS
- Pregnancy or breastfeeding, depending on the clinical situation and risk discussion
- Diagnostic uncertainty, especially if the symptoms may reflect a different headache disorder, muscle problem, or neurologic condition
A thorough evaluation is a sign of good care, not hesitation. If your clinician asks detailed questions about your headache pattern, prior treatment response, swallowing issues, muscle weakness, or other neurologic symptoms, that is part of making treatment safer and more useful.
The best candidate profile
The strongest candidates are adults with a clear diagnosis, realistic goals, and a reason to reduce reliance on daily or as-needed medication. In pain medicine, that often means someone with chronic migraine or cervical dystonia who has not done well enough with standard treatment, cannot tolerate it, or wants an option that does not affect the whole body the way many pills do.
Clear targets matter. So do expectations. Botox can be a strong tool for reducing pain days, spasm, and medication burden, but it is not a cure-all, and it should not be offered as a cosmetic-style add-on for a complex pain problem.
Botox is safest and most useful when the diagnosis is clear, the target is specific, and the treatment plan is built around function. The right question is not, "Can I get Botox?" The better question is, "Does Botox fit my diagnosis, my goals, and the rest of my care plan?"
Integrating Botox into a Comprehensive Pain Care Plan
Botox is powerful, but it isn't a stand-alone answer for every patient. The best results usually come when it fits into a broader pain strategy designed around the actual problem.
For chronic migraine, that may mean pairing Botox with trigger review, sleep and stress counseling, medication management, and careful tracking of headache patterns. For cervical dystonia, the plan may also include movement training, targeted rehabilitation, and other interventions that improve function while the treated muscles are less overactive.
Why multimodal care matters
Pain conditions rarely have one driver. A migraine patient may also have neck pain, poor sleep, medication overuse, or another headache contributor. A dystonia patient may have guarding, deconditioning, and secondary pain from months or years of abnormal movement.
That is why Botox should be viewed as one tool among several, not as a magic fix.
A thoughtful plan often includes:
- Accurate diagnosis first so treatment matches the condition
- Functional goals such as fewer missed workdays, better sleep, or easier neck rotation
- Follow-up and reassessment to decide whether the response is strong enough to continue
- Alternative options when needed if Botox doesn't deliver enough benefit on its own
Where Botox fits in opioid-sparing care
One of Botox's practical advantages is that it can reduce symptom burden without asking the whole body to tolerate another daily medication. That makes it especially appealing for people trying to avoid escalation of pain pills or simplify a medication regimen that already feels heavy.
The most useful mindset is this. Botox doesn't have to do everything to be worth doing. If it lowers the volume of pain, reduces flares, and improves function enough to let the rest of the care plan work better, that's meaningful progress.
Take the Next Step Toward Fewer Pain Days
Botox works by temporarily calming overactive nerve signaling. In pain medicine, that targeted effect can make a real difference for people living with chronic migraine or cervical dystonia. It isn't cosmetic medicine dressed up as pain care. It's a focused medical treatment used for specific conditions.
The biggest benefits come from matching the treatment to the right diagnosis, the right anatomy, and the right expectations. Botox doesn't work as an instant rescue option, and it doesn't replace a full pain care strategy. What it can do is reduce the intensity of the cycle, lower symptom burden, and create room for better day-to-day function without relying on opioids.
If you're in Chicago Ridge, Orland Park, Palos Heights, Oak Lawn, Palos Hills, Worth, Bridgeview, Hickory Hills, Alsip, Burbank, Evergreen Park, or nearby Illinois communities, a careful evaluation is the best next step. You can request a visit through the clinic's online appointment page.
Midwest Pain & Wellness provides compassionate, evidence-based care for people living with chronic pain, including chronic migraine and cervical dystonia. If you're ready to find out whether Botox belongs in your treatment plan, schedule a consultation with Midwest Pain & Wellness.



