Pain that stays locked into one small area can wear you down in a very specific way. Maybe it's burning on the top of your foot after surgery. Maybe it's sharp groin pain after a hernia repair. Maybe your leg feels normal in one spot and unbearable in another, and nothing you've tried has matched how precise your pain feels.
That’s where many people get frustrated with standard pain treatments. If the pain is highly localized, broad treatments can feel too broad. Medications may dull everything without really calming the exact nerve pathway causing the problem. Injections can help, but sometimes the relief fades or never fully covers the painful zone.
When people ask, “How does DRG work?”, they’re usually asking something deeper. They want to know why one advanced therapy might succeed when other options haven’t. They want to know what the path looks like from the first visit to actual daily relief. And they want an explanation that sounds human, not technical.
A Targeted Solution for Hard-to-Treat Chronic Pain
I often think about the patient whose pain is so focused that they can point to it with one finger. Not their whole back. Not their whole leg. One patch of foot. One side of the knee. One corner of the groin. Those are the cases where people often say, “How can something this small disrupt my whole life so much?”
That’s the kind of pain pattern that makes people avoid shoes, stairs, driving, errands, and sleep. It can follow surgery, an injury, or a nerve problem that never settled down the way it should have. In many patients, the issue isn’t that the body part is still being harmed. The issue is that the nerve pathway keeps sounding the alarm.
DRG stimulation is designed for that kind of problem. It’s a form of neuromodulation that targets the dorsal root ganglion, a key structure involved in processing sensory signals from a specific area of the body. Instead of trying to blanket a wide region, DRG stimulation aims at a more exact pain pathway.
When broad treatments feel too broad
Some chronic pain is widespread and diffuse. Some isn’t. If your pain lives in a narrow, stubborn area, precision matters.
Common examples include:
- Post-surgical nerve pain: Pain that lingers after a foot, ankle, knee, groin, or hernia procedure.
- CRPS and causalgia: Severe nerve-related pain that may feel burning, stabbing, or exquisitely sensitive.
- Localized neuropathic pain: Tingling, electric, or hypersensitive pain limited to one region.
The more focal the pain pattern, the more important it is to match the treatment to that pattern.
For the right person, DRG stimulation offers a different kind of conversation. It isn’t just, “How do we reduce pain overall?” It becomes, “How do we calm the exact nerve relay involved in your pain?”
That shift can matter a great deal for people trying to move away from repeated flare cycles and toward steadier, opioid-sparing care.
Understanding the Source of Your Pain The Dorsal Root Ganglion
To understand DRG stimulation, it helps to start with the structure itself.
The dorsal root ganglion, or DRG, houses the cell bodies of primary sensory neurons and acts as a critical checkpoint for sensory signals such as pain, touch, and temperature before those signals move to the spinal cord and brain, as described in this National Library of Medicine review of DRG anatomy and function. That sentence is accurate, but for most patients it still sounds abstract.
A better way to think about it is this. The DRG works like a fire alarm control panel for a specific body region. Signals come in from the body. The panel sorts them. Then it helps determine how those signals move forward.
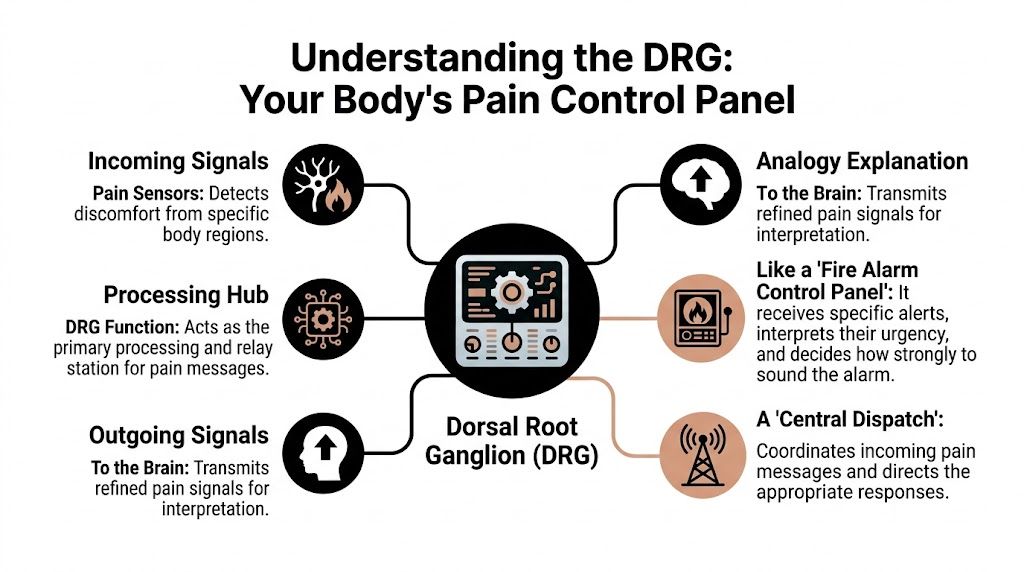
Why the DRG matters in chronic pain
In acute pain, that system is useful. If you step on something sharp, you want the alarm to fire.
Chronic neuropathic pain is different. The alarm system may keep sending danger messages after the original injury has healed, or it may overreact to normal input like light touch, shoes, bedsheets, or walking. That’s why some patients say, “Nothing looks wrong, but it still hurts terribly.”
With DRG stimulation, the goal isn’t to remove the DRG or damage the nerve. The goal is to modulate the signal. In plain language, that means adjusting how the pain message is processed before it spreads into a larger, harder-to-control experience.
Why this is different from “the spinal cord”
Patients often hear about spinal cord stimulation and assume DRG stimulation is the same thing. They’re related, but not identical.
The spinal cord is a larger communication highway. The DRG is more like a specialized checkpoint along a specific route. If your pain is limited to a distinct area, treating the checkpoint can offer a more focused strategy than treating the broader highway.
That’s one reason DRG therapy gets attention in focal pain syndromes. The anatomy supports precision.
A simple analogy that helps
Think about an apartment building with a faulty fire alarm panel in one wing.
- Normal system: Smoke in one unit triggers the right response.
- Faulty system: The same wing keeps sounding alarms even when there’s no active fire.
- DRG stimulation: A technician recalibrates the panel so it stops overreacting and sends more appropriate alerts.
The whole building doesn’t need to be shut down. The work is focused where the false alarm is happening.
Practical rule: If your pain feels extremely localized, ask whether the pain pathway itself is localized too.
People living with nerve pain in the Chicago suburbs often don’t need a crash course in neuroanatomy. They need a clear explanation of why a focused therapy might fit a focused pain problem. If you’re trying to understand whether your symptoms line up with nerve-related conditions, a review of conditions commonly treated in interventional pain care can help frame that discussion before a consultation.
Is DRG Stimulation the Right Choice for Your Pain
Not every chronic pain problem is a DRG problem. That’s good news, because it means patient selection matters. The more carefully a therapy is matched to the pain pattern, the better the conversation tends to be.
DRG stimulation is often considered when pain is neuropathic, focal, and persistent despite more conservative care. Patients usually describe the pain as burning, electric, stabbing, tingling, or painfully sensitive to touch. The pain may be confined to the foot, ankle, knee, groin, hip, or another defined area rather than spreading broadly across the body.
Pain patterns that raise suspicion
Certain stories come up again and again in good DRG candidates.
- After surgery: The incision healed, but burning or shooting pain remained in a tightly defined area.
- After injury: A fracture, crush injury, or nerve trauma led to ongoing hypersensitivity.
- With CRPS features: The limb may feel painfully sensitive, swollen, temperature-sensitive, or difficult to trust.
One of the strongest data points we have comes from the landmark ACCURATE study. At 12 months, 81.2% of patients treated with DRG stimulation for lower-limb CRPS or causalgia achieved significant pain relief, compared with 56.7% treated with traditional spinal cord stimulation, according to the published ACCURATE trial results.
That doesn’t mean DRG is right for everyone with leg pain. It does mean this therapy has meaningful evidence in the kinds of focal neuropathic conditions where precision matters.
When DRG may be worth discussing
You may want to ask about DRG stimulation if several of these sound familiar:
- Your pain is localized: You can outline the painful area clearly.
- The quality feels nerve-related: Burning, tingling, electric, stabbing, or touch-sensitive pain is common.
- Conservative care hasn’t been enough: Medications, therapy, or injections haven’t delivered lasting control.
- Function is shrinking: You’re avoiding walking, wearing normal shoes, driving, or sleeping comfortably.
When another option may fit better
If pain is widespread, mechanical, or driven by a different structural issue, another treatment may make more sense first. Some patients need medication adjustment, physical rehabilitation, image-guided injections, radiofrequency treatment, or another neuromodulation strategy instead.
That’s why a careful consultation matters more than internet checklists.
Good candidates usually don’t just have severe pain. They have the kind of pain that matches the therapy’s targeting strength.
For someone in Palos Hills, Bridgeview, Worth, Burbank, or Evergreen Park who has been told to “just live with it,” this is often the most important takeaway. If your pain is focal and nerve-driven, there may be a more precise option than the broad approaches you’ve already tried.
Your DRG Therapy Journey at Midwest Pain & Wellness
By the time most patients consider DRG stimulation, they’ve already been through enough uncertainty. What helps is a clear roadmap. The process usually unfolds in two stages: a trial and, if the trial goes well, a permanent implant.
The first stage matters because no one should have to guess whether a neuromodulation therapy will help. You get a chance to experience it before making a longer-term decision.
Step one: the consultation and planning
The visit starts with pattern recognition. Your physician looks at where the pain is, how it behaves, what treatments you’ve already tried, and whether the symptoms fit a focal neuropathic process. Prior surgeries, imaging, medications, and functional limits all matter.
This is also where expectations get clarified. The goal isn’t perfection. The goal is meaningful relief that improves function, tolerance for activity, and day-to-day quality of life.
Some patients are surprised that this planning stage is so detailed. It needs to be. Targeted therapy only works well when the targeting is thoughtful.
Step two: the trial period
During a DRG trial, temporary leads are placed using image guidance so the care team can test whether stimulation meaningfully reduces your pain in the intended area. Patients then go home and live real life with the system for a short trial window.
During that time, you’re not just rating pain on a scale. You’re looking for practical changes.
- Walking: Can you put more weight on the painful foot or leg?
- Clothing and shoes: Are everyday sensations less irritating?
- Sleep: Are nighttime flares less disruptive?
- Routine tasks: Can you drive, shop, or sit more comfortably?
A strong trial gives both patient and physician useful information. It tells you whether the painful region is being covered in a way that feels relevant to your life, not just interesting in a procedure room.
A good trial isn’t about chasing a perfect day. It’s about seeing whether your normal painful activities become more manageable.
Step three: moving to a permanent implant
If the trial clearly helps, the next conversation is about permanent implantation. This is typically a minor outpatient procedure in which the long-term leads are positioned and a small generator is placed under the skin.
The details vary by patient, but the overall idea is straightforward. The implanted system delivers stimulation to the target area so the nerve signals can be modulated over time. After placement, the device is programmed and adjusted based on your response.
Programming isn’t a one-time event. Fine-tuning often matters. Some people respond well right away. Others need adjustments to get the best coverage and comfort.
What recovery usually feels like
Most patients don’t describe recovery as difficult in the same way they describe recovery from a major orthopedic or abdominal surgery. Still, you’ll need to follow activity instructions carefully while the leads settle and the tissues heal.
Common themes during recovery include:
- Incision care: Keep the area clean and follow specific wound instructions.
- Movement limits early on: Bending, twisting, and heavy lifting may be restricted at first.
- Programming follow-up: Adjustments may improve comfort and targeting.
- Function tracking: Patients are encouraged to notice what daily tasks become easier.
If you’re curious about the physician behind this kind of care, you can learn more about Dr. Yaw Donkoh’s background and training.
For many patients in Orland Park, Palos Heights, Oak Lawn, Alsip, or Hickory Hills, the most reassuring part of the process is that it unfolds step by step. Nothing about it requires blind faith. The trial lets you test the concept before committing to the implant.
Comparing Your Pain Relief Options DRG vs SCS
A common source of confusion is this: people hear “stimulation” and assume every stimulator works the same way. They don’t.
DRG stimulation and traditional spinal cord stimulation (SCS) are both neuromodulation therapies, but they’re built for different pain patterns. In simple terms, DRG tends to shine when pain is highly localized. SCS is often used for broader pain distributions.
The key anatomical advantage was described clearly in the neurosurgical literature: because the DRG is specific to a particular dermatome, stimulation can be mapped closely to the painful area without affecting surrounding regions, as explained in this Neurosurgical Atlas review of DRG stimulation.
Why precision changes the decision
If your pain covers a wide territory, broader coverage may be useful. But if your pain is concentrated in a place that’s historically harder to treat, such as the foot or groin, precision can be the difference between “somewhat better” and “that’s the spot.”
That doesn’t make DRG universally better. It makes it better suited to certain maps of pain.
DRG Stimulation vs. Traditional SCS at a Glance
| Feature | DRG Stimulation | Traditional SCS |
|---|---|---|
| Primary targeting style | Focused targeting of a specific pain pathway | Broader targeting across larger pain regions |
| Best fit | Focal neuropathic pain, including hard-to-treat small areas | More diffuse or widespread pain patterns |
| Coverage feel | More precise and localized | Broader field of coverage |
| Useful body regions | Often helpful for areas such as foot, groin, knee, or other discrete zones | Often considered for larger back and leg pain distributions |
| Programming goal | Match stimulation closely to one painful region | Cover a larger pain territory |
| Clinical decision point | Strong option when pain can be mapped tightly | Strong option when pain is less localized |
How this compares with other interventional options
Patients also ask how DRG compares with nerve blocks or other injections. That’s a fair question.
Injections can be excellent diagnostic or therapeutic tools. They may reduce inflammation, calm irritated nerves, or help confirm a pain generator. But they’re usually not designed to provide the same kind of ongoing neuromodulation that an implanted DRG system can provide for the right candidate.
A practical way to think about the options:
- Injections and blocks: Often useful earlier in care or as part of a broader plan.
- Radiofrequency procedures: Can help certain pain generators, depending on anatomy and diagnosis.
- Traditional SCS: Often considered for broader pain fields.
- DRG stimulation: Often considered when the pain is localized and nerve-driven.
If you want to see the range of interventional approaches that may be considered alongside neuromodulation, this overview of pain procedures used in treatment is a helpful reference.
The best device isn’t the newest one or the most talked about one. It’s the one that matches the way your pain is distributed.
That’s why the question isn’t a simple “DRG or SCS?” The better question is, “Which treatment fits the geography of my pain?”
Life After DRG Implantation Outcomes and Success
The part patients care about most is simple. What does life feel like after implantation if the therapy works?
The answer usually isn’t dramatic in a movie-script sense. It’s more practical. A person notices they can wear a shoe longer. Walk farther through the grocery store. Stand in the kitchen without bracing mentally for the next electric jolt. Sit through a family event and pay attention to the people there instead of the pain signal in one part of the body.

What durable improvement can look like
Long-term results matter because temporary excitement is not enough. In one major follow-up study, over 70% of patients who received a permanent DRG implant maintained at least a 50% reduction in pain at 36 months, with many also reporting better physical function and quality of life, according to this long-term Journal of Pain follow-up study30788-X/fulltext).
That kind of durability is important for people who have already cycled through short-lived treatments. It suggests that, for the right candidate, DRG stimulation can become part of a stable long-term plan rather than a temporary experiment.
The day-to-day reality of living with the device
Eventually, individuals stop thinking about the implant every hour of the day. It becomes something they manage, not something that manages them.
Daily life may include:
- Device awareness early on: At first, you’ll notice the implant site and the fact that a system is there.
- Programming adjustments: Fine-tuning may improve comfort and precision over time.
- Charging or maintenance habits: Depending on the system, you may need to follow a simple routine.
- Follow-up visits: These help make sure the settings still match your symptoms and goals.
A more meaningful measure than a pain score
Pain scores matter, but function matters just as much. For many patients, success sounds like this:
- “I can walk into the store without dreading the parking lot.”
- “I can let a bedsheet touch my foot again.”
- “I can garden, cook, or play with my grandchildren without that one area taking over the day.”
Those changes may sound small to someone who hasn’t lived with focal neuropathic pain. They don’t feel small when your life has been organized around avoiding pain triggers.
Relief is important. Regaining trust in your body is often even more meaningful.
Recovery of confidence
One of the quiet victories after successful DRG therapy is confidence. Patients often start by testing the painful area carefully. Then they do a little more. A longer walk. A social outing. A household task they’ve been dodging.
That progression matters. It’s how pain stops dictating every decision.
For older adults in Oak Lawn, Orland Park, Evergreen Park, Palos Hills, and nearby Illinois communities, the goal isn’t to become someone else. It’s to get back to ordinary life with less fear, less guarding, and more room to move.
Patient Questions About DRG Therapy Answered
Patients usually ask practical questions before they ask technical ones. That makes sense. You’re trying to decide whether this is worth a call, a visit, and a real discussion.
Do I need a referral to ask about DRG stimulation
Sometimes yes, sometimes no. It often depends on your insurance plan, not just the clinic. Some plans allow self-referral for specialty evaluation, while others want a referral from a primary care physician or another treating doctor.
If you’re in Oak Lawn, Palos Heights, Worth, Bridgeview, Hickory Hills, Alsip, Burbank, Evergreen Park, or Orland Park, the easiest next step is usually to call and ask what your specific plan requires.
Is DRG stimulation covered by Medicare or insurance
Coverage depends on medical necessity, diagnosis, prior treatment history, and your individual plan. Many patients want a simple yes or no, but coverage decisions are rarely that simple.
A clinic team can usually help review benefits, authorization requirements, and what documentation may be needed before moving forward.
What happens if the trial doesn’t help
That information is still useful. A trial is designed to answer a question before permanent implantation. If it doesn’t provide meaningful relief, you typically don’t move to the long-term implant.
That doesn’t mean you’ve failed treatment. It means you’ve learned something important about what your pain responds to, and your physician can use that information to reconsider other options.
Will I feel the stimulation all the time
Experiences vary by patient and device settings. Some people are very aware of the stimulation early on, while others notice it less as programming is refined and they adapt to the therapy.
The important point is that programming can be adjusted. If the settings don’t feel right, that’s part of the follow-up conversation.
Are there activities I’ll need to avoid
There are usually temporary restrictions after lead placement and implantation so the system can heal properly. Your physician will give you specific guidance about movement, lifting, bending, twisting, and wound care.
Longer term, the goal is to expand safe activity, not shrink it. But every patient’s instructions should be individualized.
How is DRG different from the hospital billing term DRG
This is a very understandable point of confusion. In healthcare, “DRG” can also refer to Diagnosis-Related Groups, a hospital payment classification system.
That billing DRG system was developed in the late 1960s at Yale University and later became foundational in modern reimbursement, with hospitals assigning inpatient admissions to one of more than 700 DRG codes, as described in this overview of Diagnosis-Related Groups in healthcare reimbursement.
In pain treatment, though, DRG stimulation refers to the dorsal root ganglion, the nerve structure discussed earlier in this article. Same abbreviation. Very different meaning.
Can DRG therapy help me get off opioids
The goal of interventional pain care is often to improve pain control and function in a way that supports less reliance on opioid medication when appropriate. But medication changes should be individualized and supervised.
For some patients, improved control creates room to reduce medication burden. For others, the plan involves a broader combination of therapies.
What’s the best next step if I think I’m a candidate
Bring your story in a structured way. That helps more than trying to sound medical.
Useful things to share include:
- Where the pain is: Show the exact area if you can.
- What it feels like: Burning, tingling, stabbing, electric, numb, or hypersensitive.
- What you’ve tried: Medications, injections, surgery, therapy, or other procedures.
- What the pain is stopping you from doing: Walking, driving, sleeping, working, or daily tasks.
The clearer your pattern, the easier it is for a pain specialist to judge whether DRG stimulation fits.
If you’re living with chronic nerve pain in Chicago Ridge, Oak Lawn, Palos Hills, Palos Heights, Worth, Bridgeview, Hickory Hills, Alsip, Burbank, Evergreen Park, or Orland Park, Midwest Pain & Wellness can help you explore whether advanced, opioid-sparing interventional care such as DRG stimulation fits your pain pattern and goals.



