Living with daily pain changes the rhythm of everything. Getting out of bed takes planning. Driving through Chicago Ridge traffic feels longer than it used to. Grocery shopping in Oak Lawn, walking into work in Alsip, or sitting through dinner in Palos Heights can start to revolve around one question: how bad will the pain be today?
Many people who ask “How does SCS work?” are already far past the stage of trying a heating pad and hoping for the best. They’ve often been through medications, rest, injections, therapy, or even surgery, and they’re frustrated that the pain keeps coming back. They don’t want vague promises. They want to know what this treatment does, what the process feels like, and whether it’s realistic for their life in Illinois.
Reclaiming Your Life from Chronic Pain
A common story sounds like this. Someone injures their back, has a surgery, or develops nerve pain that never fully settles down. Months later, the pain is still there. It radiates into the leg, burns, stabs, or aches, and slowly starts shrinking their world.
At first, they push through it. Then they stop going on walks. They sit out family events. Sleep gets lighter. Mood gets shorter. Even when the pain isn’t the only thing in the room, it becomes the thing that shapes the room.
For many patients in Chicago Ridge and nearby communities like Bridgeview, Worth, Hickory Hills, and Orland Park, that’s the point where spinal cord stimulation enters the conversation. Spinal cord stimulation, or SCS, is a therapy that uses carefully programmed electrical impulses to change how pain signals travel before the brain experiences them as pain. It’s used in pain management, not as a shortcut, but as a thoughtful option when pain has become persistent and disruptive.
What matters most is that SCS isn’t about “covering up” pain in a simplistic way. It’s about changing the pain signaling system itself. In clinical trials, over 70% of patients experienced significant pain relief during an SCS trial, and permanent success is typically defined as at least 50% improvement in both pain and function according to clinical benchmarks for SCS trial and implant success.
That combination matters. Pain relief alone isn’t enough if you still can’t stand longer, sleep better, or get through your day with more control.
SCS works best when the goal is not perfection. The goal is meaningful relief, better function, and getting parts of your life back.
How SCS Works to Modulate Pain Signals
SCS works by changing how pain signals are processed before the brain experiences them as pain.
Pain starts in the body, travels through nerves to the spinal cord, and then continues upward to the brain. With spinal cord stimulation, thin leads placed in the epidural space deliver mild electrical pulses near the spinal cord. Those pulses influence the pain pathways, which can reduce how intense or intrusive the pain feels.
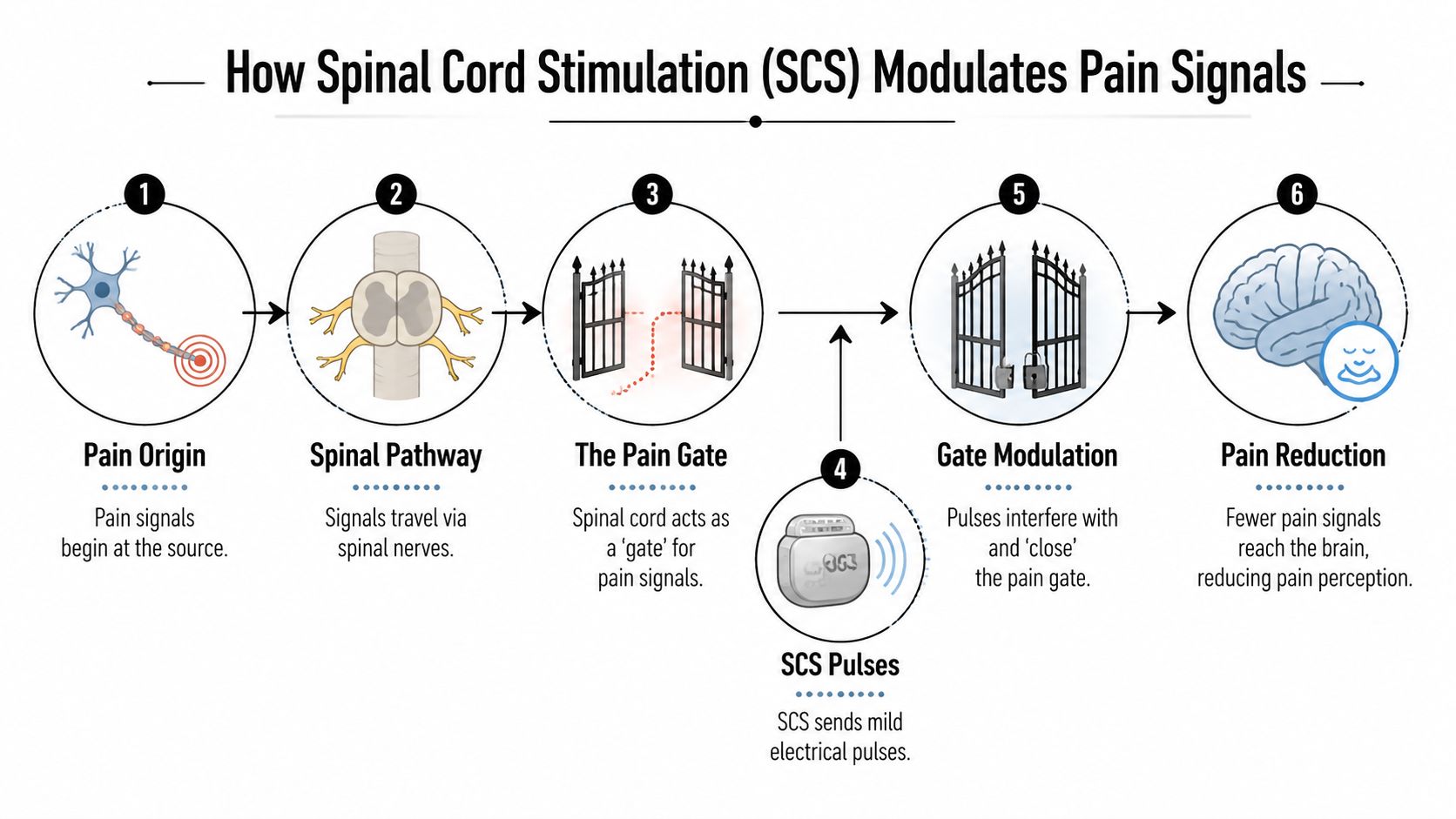
The gate control idea
One of the main ways clinicians explain SCS is with the gate control theory of pain. The spinal cord acts like a relay station. Pain signals arriving from the body have to pass through that relay before the brain interprets them. Stimulation can interfere with that transmission, which helps quiet the signal reaching the brain.
In more technical terms, SCS delivers electrical impulses through epidural leads to the dorsal columns, where it can activate large-diameter A-beta fibers and inhibit pain signal transmission. The Cleveland Clinic overview of spinal cord stimulators describes this process in patient-friendly terms.
The device changes how the nervous system handles pain signals coming from the underlying condition.
That point matters in clinic conversations. Patients in Chicago Ridge often ask whether SCS is fixing the disc problem, scar tissue, or nerve injury itself. Usually, the answer is no. The goal is to reduce the abnormal pain signaling that continues after the original issue has become chronic, especially when the nervous system has become overly reactive.
What the system includes
An SCS system has three basic parts:
- Leads placed near the spinal cord to deliver stimulation
- A pulse generator that powers the system
- A patient controller or remote that lets you adjust settings within the range your physician programs
Some systems produce a tingling sensation called paresthesia. Others are designed to work without that feeling. Neither approach is automatically better for every patient. The right choice depends on the pain pattern, where the pain is located, how your body responds during the trial, and how much day-to-day control you want over the settings.
Why programming matters
SCS is not a one-setting therapy. We can adjust pulse width, amplitude, frequency, and which contacts are active. That is one reason the trial matters so much. It helps identify whether your pain responds to stimulation at all, and it gives us early information about which programming style fits your symptoms.
Different systems use different stimulation strategies, including traditional low-frequency patterns and high-frequency therapy. Published studies on high-frequency SCS have shown meaningful pain relief for some patients with chronic back and leg pain, including people with failed back surgery syndrome, as reported in research on 10 kHz spinal cord stimulation published in PubMed.
In practice, programming is where the science meets the daily reality of living with pain. A setting that helps while lying down may not be the one that works best for walking through a grocery store, riding in a car, or sleeping through the night. That is why follow-up adjustments are part of the treatment, not a sign that something has gone wrong.
What patients usually notice
Patients usually describe SCS as making pain less dominant.
The pain may feel less sharp, less constant, or less disruptive during ordinary activities. Some notice they can sit longer, stand with less flare-up, or sleep with fewer interruptions. Others notice the biggest change is that the pain stops commanding their attention every minute of the day.
That is the practical value of SCS. It can calm an overactive pain pathway enough to give you more room to function, while still requiring thoughtful programming, realistic goals, and ongoing follow-up over time.
The SCS Trial and Implantation Journey
You come in after years of back or leg pain, and the first question is usually simple: “How do I know this is worth doing?” The trial answers that in a practical way. It lets you feel the therapy in day-to-day life before anyone commits to a permanent implant.

The trial is a real-world test
During the trial, temporary leads are placed into the epidural space through a needle, usually with local anesthesia and light sedation. Those leads connect to an external generator that you wear outside the body. Patients then go home and use the system during a short trial period, often about a week, as described by Johns Hopkins Medicine’s overview of spinal cord stimulator placement.
The reason for the trial is straightforward. Pain relief in a procedure room does not tell me enough. I want to know whether stimulation helps you stand at the kitchen counter, ride in the car, sleep longer, or walk through a grocery store with less flare.
What to watch for during the trial
A useful trial includes testing the activities your pain usually limits, rather than only recording pain scores while resting.
Patients often pay attention to changes such as:
- Walking farther before pain forces a stop
- Sitting or standing with fewer flare-ups
- Sleeping more consistently because pain interrupts less often
- Using less rescue medication if relief allows it
- Handling normal routines with less effort and less fear of a bad pain day
Many clinics use pain relief of about 50% along with better function as a common benchmark for considering a permanent implant, according to MedlinePlus information on spinal cord stimulation.
What can affect trial results
The trial also helps clarify fit. If the painful area is not covered well, the settings need adjustment, or the pain pattern does not respond the way we hoped, that usually becomes clear during this stage.
There are real trade-offs. Temporary leads can move. Coverage may feel strong one day and less consistent the next, especially with certain body positions. That does not always mean SCS has failed. It often means the trial is doing its job by showing us how your body responds in real conditions.
Practical rule: A successful trial improves daily function you care about.
What happens if the trial helps
If the trial gives meaningful relief and improves function, the next step is permanent implantation. Long-term leads are placed, and the pulse generator is implanted under the skin, usually in the upper buttock or abdomen. This is commonly done as an outpatient procedure.
Patients are often relieved to hear what this procedure is and what it is not. It is still surgery, and it deserves careful planning. At the same time, it is different from open spine surgery. There is no fusion, no large spinal hardware, and no cutting away of bone or disc to create the pain-relief effect.
The evaluation before permanent implantation
Good SCS care starts before the trial and continues after the implant. At our clinic in the Chicago Ridge area, that means looking closely at the diagnosis, imaging, prior procedures, medication history, goals, and daily function. We also review whether SCS fits better than other options listed in our interventional pain treatment procedures.
That step matters because SCS is not a shortcut. It works best when the pain pattern, the device, and the patient’s goals line up clearly. Patients who do well over time usually understand each phase of the process, know what improvement would count as meaningful in their own life, and expect follow-up visits for programming and long-term management.
Types of Spinal Cord Stimulation Systems
Not all spinal cord stimulators feel the same. That surprises many patients. They assume SCS is one device with one sensation, but modern systems can work in different ways.

Traditional tonic stimulation
Traditional tonic stimulation is the older style many people have heard about. It usually creates paresthesia, which patients often describe as a gentle tingling, buzzing, or humming sensation in the area where they usually feel pain.
For some people, that sensation is reassuring because it tells them the therapy is working. For others, it can be distracting, especially if body position changes the way it feels.
Newer paresthesia-free options
Modern systems have expanded beyond tonic stimulation. SCS technology now includes high-frequency, subthreshold, and burst models, allowing different programmable therapy options, as noted in this overview of evolving SCS technology and FDA clearance pathways.
These newer forms of stimulation often work without a tingling sensation. That can be a better fit for patients who want relief without feeling the device during daily activities.
How the choice is made
Choosing a system isn’t about picking the newest label. It’s about matching the technology to the patient.
A few practical considerations usually shape that discussion:
- Pain pattern: Nerve pain in the leg may behave differently than broader back pain.
- Sensitivity to sensation: Some patients like paresthesia coverage. Others don’t.
- Daily routine: Work demands, driving, sleep, and movement patterns all matter.
- Programming flexibility: Some systems offer more options for fine-tuning than others.
A good device match depends less on marketing language and more on how your pain behaves in daily life.
A realistic note about innovation
Rapid innovation in SCS is good for patients because it expands options. It also means patients should ask clear questions. What type of waveform is being considered? Will you feel it? How easily can it be adjusted? What happens if your pain changes?
Those are better questions than asking which stimulator is “the best.” In pain management, the better device is the one that fits the anatomy, pain distribution, and functional goals of the person using it.
Who Is a Good Candidate for Spinal Cord Stimulation
SCS is usually considered when pain has become chronic, conservative treatment hasn’t been enough, and the pain pattern suggests a nerve-related component rather than a simple muscle strain or short-term flare.
The strongest candidates often have pain that’s persistent, disruptive, and resistant to standard treatment, but still follows a pattern that neuromodulation can address. Many have already tried medication management, targeted injections, rehab-based care, or prior surgery.
Pain patterns that often fit SCS
Candidates often fall into groups like these:
- Post-surgical nerve pain: People who still have significant back or leg pain after spine surgery.
- Complex regional pain syndrome: Patients with severe, often burning pain that can be difficult to treat with simpler measures.
- Chronic neuropathic pain: Burning, shooting, electrical, or radiating pain in the limbs or trunk.
- Opioid-sparing goals: People who want to reduce dependence on long-term pain medication while improving function.
For readers in Palos Hills, Worth, Bridgeview, Burbank, and Evergreen Park, the key question isn’t whether the pain is “bad enough.” The better question is whether the pain has stayed long enough, resisted enough treatment, and interfered enough with life that a neuromodulation evaluation makes sense.
Who may not be an ideal fit
SCS is not a blanket solution. It may be a poor fit when expectations are unrealistic, when the pain type doesn’t match what stimulation tends to help, or when another treatment target is more obvious.
A few examples include:
- Pain without a clear nerve-related pattern
- Untreated medical or psychological issues that interfere with treatment
- A desire for complete and immediate elimination of all pain
- Situations where another procedure addresses the root problem more directly
That last point matters. Sometimes the best next step isn’t a stimulator. It may be a decompression procedure, a joint-based intervention, a nerve block strategy, or another part of a broader pain plan. Patients exploring the conditions commonly treated in interventional pain management often find that candidacy depends on diagnosis more than on pain severity alone.
The mindset that helps most
The best candidates usually have two things. They have pain that matches the therapy, and they’re willing to participate in the process. That means giving clear feedback during the trial, attending follow-ups, and treating SCS as an active therapy rather than a passive fix.
Benefits and Realistic Outcomes of SCS Therapy
A good result with SCS shows up in daily life. Patients tell me they can stand long enough to cook, sit through a car ride to downtown Chicago, sleep with fewer wake-ups, or get through a workday with less backup from medication. Those changes matter more than chasing a perfect number on a pain scale.
That is why we judge success by function as much as pain relief. During the trial, the question is straightforward. Did the stimulation help enough to make real activities easier, safer, or more predictable? The answer often becomes clear in ordinary moments, not in the procedure room.
What SCS can do well
SCS can help reduce chronic nerve-related pain that has stayed stuck despite medication, therapy, injections, or prior surgery. For the right patient, the benefits can include:
- Meaningful pain relief: Enough improvement to change what the day looks like
- Better function: More tolerance for walking, sitting, standing, driving, and household tasks
- Less medication reliance: Some patients are able to reduce the amount of rescue medication they need
- Adjustability: Settings can be changed over time as pain patterns and activity levels change
- Reversibility: The system can be revised or removed if it is no longer helping
There are also settings where SCS may support goals beyond routine pain control. In carefully selected patients with chronic limb-threatening ischemia, the International Neuromodulation Society review of spinal cord stimulation for ischemic pain describes limb salvage as one of the potential benefits in addition to pain reduction.
Realistic outcomes matter more than perfect outcomes
Patients do best when expectations match what the therapy is designed to do. SCS does not erase every structural problem in the spine, and it does not help every pain pattern equally well. It is a tool for modulation. In plain terms, it changes how pain signals are processed so the nervous system is less overwhelming to live with.
A successful outcome usually means more capacity and less fear. It may mean walking farther, missing fewer family events, tolerating the grocery store, or returning to part-time work. Some patients get dramatic relief. Others get moderate relief that still feels meaningful because it gives them back independence.
SCS vs Other Chronic Pain Treatments
| Factor | Spinal Cord Stimulation (SCS) | Long-Term Opioid Therapy | Major Spine Surgery |
|---|---|---|---|
| Invasiveness | Minimally invasive, staged with a trial first | Non-procedural, but systemic exposure over time | More invasive, anatomy-changing procedure |
| Reversibility | Adjustable and removable | Medication can be changed, but long-term dependence can be hard to unwind | Usually not easily reversible |
| Customization | Device settings can be programmed and reprogrammed | Dose changes are possible, but not targeted to a pain pathway | Limited after the procedure is completed |
| Best use case | Chronic refractory pain with a neuropathic component | Short-term or selective pain control in some patients | Structural problems that clearly require surgery |
| Main limitation | Not every pain pattern responds | Side effects, tolerance, and function may remain limited | Recovery burden and surgical risk |
This comparison matters because every option involves trade-offs. Opioids may help some patients, but side effects and long-term dependence can limit function. Surgery can be the right answer when there is a clear structural target, but it carries recovery demands and does not guarantee relief from chronic nerve pain. SCS sits in the middle. It is more involved than taking a pill and less anatomy-changing than major surgery.
For patients in Chicago Ridge and nearby communities, I find that the most satisfied people are usually the ones who measure progress in specific goals. They want to sleep in bed instead of a recliner, walk the dog, attend church, drive to appointments with less dread, or get back to work with fewer flare-ups. A collection of patient stories about chronic pain treatment outcomes can help set that expectation in a grounded way.
The clearest way to say it is this. A strong SCS outcome means you can do more of your life with less interruption from pain.
Life After SCS Implantation and Long-Term Care
The first relief many patients feel after implantation isn’t physical. It’s mental. They realize there’s now a tool they can adjust and work with, instead of waiting for pain to flare.

Early recovery and adjustment
Right after implantation, the focus is healing and protecting lead position. Patients are usually advised to be careful with bending, twisting, stretching, and abrupt movements while the system settles in. The reason is straightforward. Good lead position is part of good pain coverage.
The first programming session is often just the beginning. Most patients need adjustments over time. That’s normal, not a sign that something is wrong. The body changes with activity, posture, inflammation, and healing, so the programming may need to change too.
Using the remote in real life
One of the most practical strengths of modern SCS is patient control. Advanced systems allow patients to adjust stimulation for different activities through remote programming apps, and in major markets this personalized control has been associated with return-to-work rates of 80% and meaningful functional improvement in Boston Scientific’s SCS handbook.
That doesn’t mean every patient returns to work or uses the same settings. It means personalization matters.
Typical day-to-day uses include:
- Lower settings for rest
- Different programs for walking or standing
- Adjustments for sitting in the car
- Changes when pain shifts location or intensity
Rechargeable and non-rechargeable systems
Some devices require regular charging. Others don’t, but the battery eventually needs replacement. Neither option is automatically better. Rechargeable systems may suit patients who want longer battery longevity and don’t mind a charging routine. Non-rechargeable systems may feel simpler to some patients.
The right choice depends on how much energy the programming requires, how the patient feels about device maintenance, and how they live day to day.
Problems that can happen
SCS is generally well tolerated, but long-term care means staying honest about possible complications. Leads can move. The stimulation pattern can stop matching the pain area. The implant site can become uncomfortable. Infection is a risk with any implanted device.
Most of these issues are manageable when addressed early. The key is follow-up, not avoidance.
If the stimulation stops fitting your pain pattern, don’t assume the therapy has failed. Sometimes the programming needs to change. Sometimes the hardware needs to be checked.
Why follow-up matters
The best long-term SCS outcomes usually come from active management. Pain changes. Activity changes. Weight, posture, work demands, and other treatments can all influence how the stimulator feels and performs.
That’s why SCS should be viewed as an ongoing therapy, not a one-time event. The implant matters, but so do the follow-up visits, the programming decisions, and the patient’s ability to say clearly what’s working and what isn’t.
Frequently Asked Questions About SCS
Can I have an MRI with an SCS implant
Sometimes, yes. It depends on the specific device and its MRI-conditional status. This should be reviewed before implantation, not after. If MRI access matters for your future care, bring that up early.
Will I feel the stimulation all the time
Not necessarily. Some systems create a mild tingling sensation. Others use paresthesia-free programming, so you may not feel the stimulation even when it’s helping.
Will airport security or screening systems be an issue
Implanted devices can create practical questions during travel and security screening. Patients typically receive device information they can carry with them. Travel is very doable, but it’s smart to plan ahead and follow the device-specific guidance.
Does the trial hurt
Most patients tolerate it well. The trial is designed to answer a practical question with the least commitment possible: does this therapy help enough in real life to justify implantation?
Is SCS only for people who already had back surgery
No. It’s often discussed in post-surgical pain, but candidacy depends more on the pain pattern, duration, prior treatment response, and overall evaluation than on surgery history alone.
Does SCS cure chronic pain
No. It treats chronic pain by modulating pain signaling. For the right patient, that can be life-changing, but it’s better understood as durable management than as a cure.
What if it works at first and then seems less effective
That can happen for different reasons. Programming may need adjustment. The pain pattern may have changed. Lead position may need to be checked. A drop in benefit doesn’t automatically mean the therapy is over.
Is this a good option for people in the Chicago Ridge area
For many adults in Chicago Ridge, Oak Lawn, Palos Hills, Palos Heights, Worth, Bridgeview, Hickory Hills, Alsip, Burbank, Evergreen Park, and Orland Park who have persistent nerve-related pain, SCS is worth evaluating. The right next step is a careful pain consultation, not a guess.
If chronic pain has narrowed your life and you’re wondering whether spinal cord stimulation could help, schedule a consultation with Midwest Pain & Wellness. A thorough evaluation can clarify whether SCS fits your pain pattern, goals, and long-term treatment plan in Illinois.



