If you're reading this, there's a good chance your pain is no longer a small annoyance. It's the ache in your low back when you get out of the car in Oak Lawn. It's the leg pain that shoots down to your calf when you stand too long in Orland Park. It's the neck or back pain that keeps you from sleeping comfortably, walking the grocery aisles, or getting through a workday without stopping to sit down.
That kind of pain often means a spinal nerve is irritated, inflamed, or under pressure. A simple way to think about it is this. If a garden hose gets pinched, water doesn't flow normally. In the spine, when a disc bulges or a tight space narrows around a nerve, the nerve gets crowded and inflamed. Once that happens, the nerve can keep sending pain signals even with light movement.
Many patients ask the same question in the exam room. How epidural injection works? The short answer is that it places medication directly into the area around the irritated spinal nerves, where it can calm inflammation and reduce pain more precisely than a pill that has to travel through your whole body first.
For people in Palos Hills, Palos Heights, Worth, Bridgeview, Hickory Hills, Alsip, Burbank, Evergreen Park, and nearby Illinois communities, that targeted approach matters. You want relief that helps you move, sleep, and function. You also want a plan that doesn't rely only on stronger and stronger pain medicine.
Introduction Why Your Spinal Pain Needs a Targeted Solution
Spinal pain becomes disruptive when it starts running your schedule. You stop bending normally. You brace before getting out of bed. You map your errands around where you can sit. Many people in the Chicago Ridge area live with this for months before they hear a clear explanation of what's hurting.
The problem is often not just "back pain." It's nerve pain caused by swelling and irritation near the spine. A herniated disc can push into nearby tissue. Spinal stenosis can narrow the passageway where nerves travel. Either way, the nerve becomes angry, and angry nerves are noisy.
Why pills sometimes aren't enough
Oral medication can help some people, but it isn't always the best tool when one irritated nerve root is doing most of the damage. That's because the medication spreads through the entire bloodstream instead of concentrating at the trouble spot.
An epidural injection is different. It targets the epidural space, the area around the spinal nerves just outside the covering of the spinal cord. That makes it a focused treatment for focused pain.
The goal isn't to mask pain blindly. The goal is to calm the exact area that's driving it.
What patients are really looking for
Most patients don't come in asking for a procedure. They come in asking for a life back. They want to walk the dog without limping. Sit through dinner. Drive without burning leg pain. Sleep through the night.
A carefully selected epidural injection can be part of that plan because it addresses the inflammation where it starts. For the right patient, it's a non-opioid, image-guided treatment designed to reduce pain enough to restore function.
Common reasons patients ask about epidural injections include:
- Radiating leg pain: Pain that starts in the low back or buttock and travels down the leg often points to nerve root irritation.
- Neck pain with arm symptoms: Tingling, numbness, or pain into the shoulder or arm can come from an inflamed nerve in the cervical spine.
- Pain that stalls recovery: Some people are willing to stay active, but their pain is too strong to let them participate consistently in rehab or normal daily movement.
Understanding the Source of Your Pain The Epidural Space
Pain that shoots into the arm or leg usually starts closer to the spine than people expect.
The epidural space is the area around the spinal nerves, just outside the protective covering of the spinal cord and nerve roots. When a disc bulges, a bone spur narrows the opening, or nearby tissues become irritated, that small space can become crowded and inflamed. In many patients, especially those dealing with sciatica or cervical radicular pain, that irritated nerve root is what drives the burning, tingling, numbness, or electric pain felt farther down the limb.
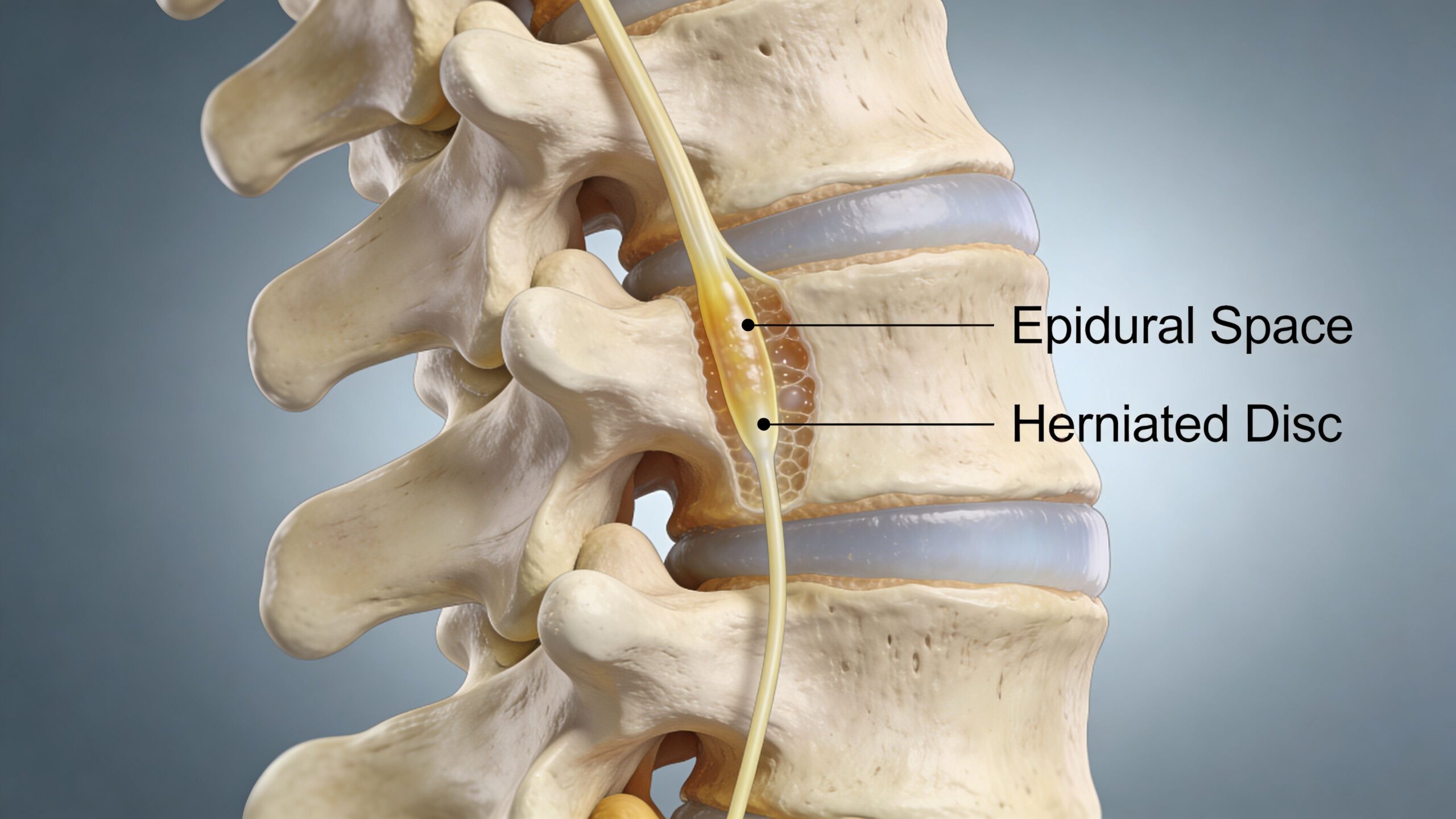
Why this space matters
The epidural space matters because it sits next to the nerves that carry signals from your spine into your shoulder, arm, buttock, leg, and foot. If one of those nerves is swollen or chemically irritated near its starting point, the brain often feels pain along the nerve's entire route, not just in the back or neck.
That is why a patient in Chicago Ridge may say, "My calf is what hurts," while the actual source is an irritated lumbar nerve root. The same pattern happens in the neck. A pinched or inflamed cervical nerve can create pain in the shoulder blade, arm, or hand even when the neck itself is only mildly sore.
What your doctor is trying to reach
During an epidural injection, the goal is to place medication into this space so it can bathe the irritated nerve root and nearby inflamed tissue. That targeted placement is one reason pain specialists use fluoroscopic guidance. Precision matters when the aim is to calm the area generating the symptoms and help you return to walking, driving, sleeping, or getting through a workday with less pain.
Patients often ask why we treat the spine when the pain is felt lower down. The answer is simple. The nerve functions like an electrical line. If the line is irritated near its origin, the signal can be felt anywhere downstream.
What can irritate the epidural space
Several common spine problems can inflame this area:
- Disc herniation: Disc material can press on or irritate a nearby nerve root.
- Spinal stenosis: Age-related narrowing can crowd the nerves and trigger inflammation.
- Degenerative changes: Arthritic joints, thickened ligaments, and related wear can reduce the room available for the nerve.
- Post-injury or post-surgical irritation: Some patients develop persistent nerve inflammation even after the original injury has started to heal.
In our Chicago-area practice, that anatomy guides treatment decisions. If your exam, symptom pattern, and imaging all point to a specific irritated nerve, an epidural injection can fit into an opioid-sparing plan focused on function, not just short-term pain scores.
Clinical takeaway: The epidural space is the area around the spinal nerves where inflammation often triggers radiating pain, which is why carefully guided treatment is directed there.
The Dual-Action Mechanism How an Epidural Injection Works Biologically
A patient in our Chicago Ridge clinic might say, "My leg pain starts in my back, shoots past my knee, and makes a simple trip to Mariano's feel like too much." In that situation, the goal of an epidural steroid injection is straightforward. We place medication near the irritated spinal nerve so it can calm the process causing the pain.
The treatment works in two phases. A local anesthetic can quiet the nerve soon after the injection. A corticosteroid then works over the next several days to reduce inflammation around that nerve root.
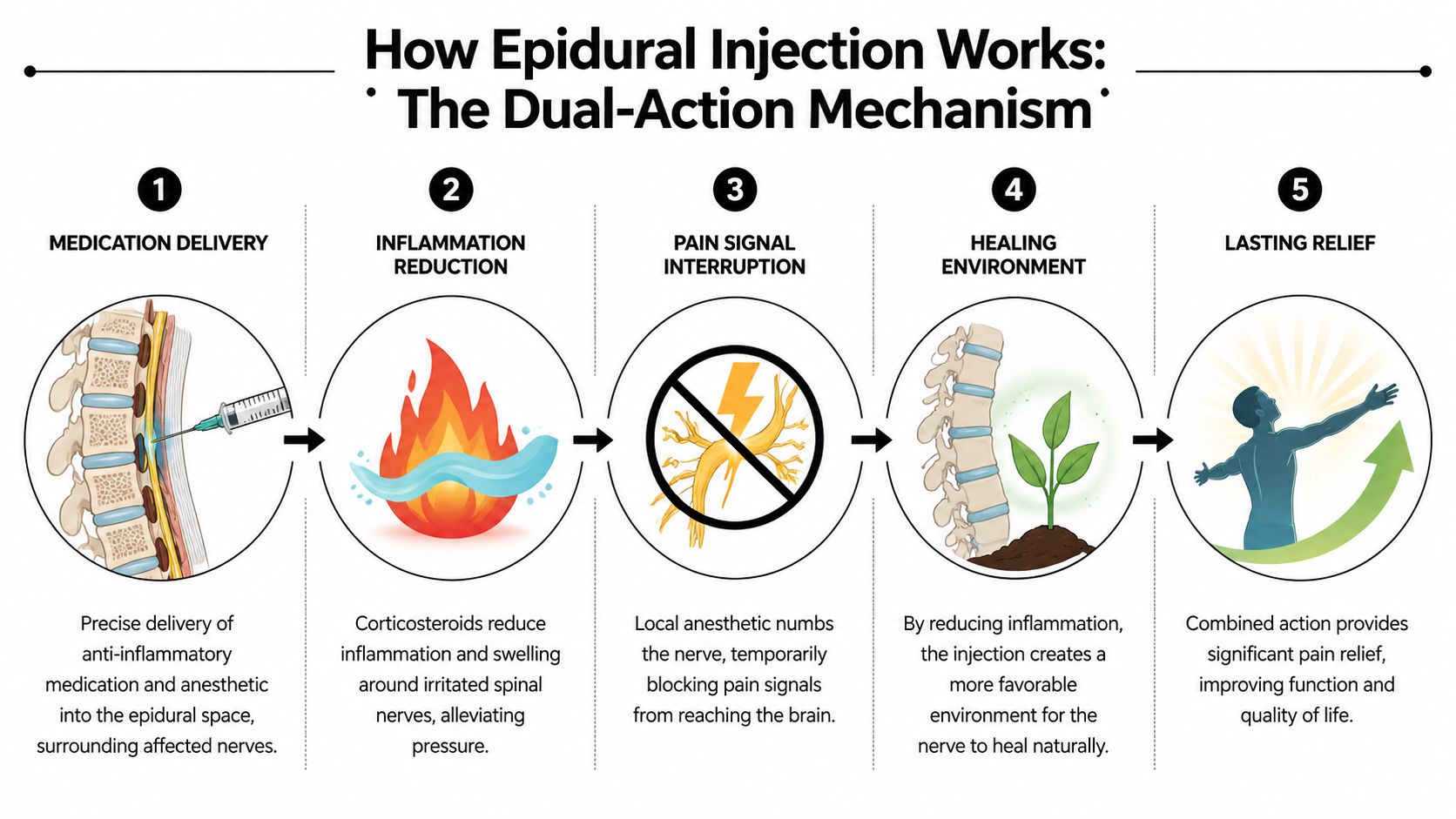
The numbing medicine works first
The local anesthetic, often lidocaine or a similar medication, temporarily slows the nerve's ability to send pain signals. It works like turning down the volume on an overactive alarm. The irritated nerve is still there, but it becomes less likely to keep firing so intensely.
That early numbing effect can also give your doctor useful information. If your usual pain eases for a short time after the injection, it supports the idea that the treated nerve is part of the problem.
The steroid calms the inflammatory irritation
The steroid addresses the deeper issue. An irritated nerve root is often swollen and chemically inflamed, especially with conditions like a disc herniation or stenosis. Corticosteroids reduce that inflammatory activity, which can lower swelling and make the nerve less sensitive.
Patients do not need to memorize the chemistry. The practical point is easier to grasp. A calmer nerve usually hurts less with standing, walking, bending, coughing, or getting in and out of the car.
This is why relief may not be immediate. The anesthetic may help first. The steroid often needs time to settle the area down.
Why the exact location matters
Medication works best when it reaches the painful nerve's neighborhood. That is why pain specialists use imaging to guide placement instead of relying on feel alone. A few millimeters can matter in the spine.
If one nerve on one side is inflamed, the injection should be directed to that level and that side. Good targeting improves the chance that the medicine will spread where it is needed and supports an opioid-sparing plan centered on function.
What happens after the medication is placed
Here is the biological sequence in simple terms:
- The medication is delivered into the epidural space near the irritated nerve.
- The local anesthetic starts quieting pain signaling in the short term.
- The steroid begins reducing inflammatory chemicals and nerve swelling over time.
- The nerve becomes less reactive with movement and daily activity.
- Pain may ease enough for better walking, sleeping, exercise, and physical therapy participation.
That last step matters more than many people realize. Relief is not only about comfort. It can create a window where you can move more normally, strengthen supportive muscles, and get back to the routines that matter in daily life across the Chicago suburbs.
What people mean by "breaking the pain cycle"
Pain can keep feeding itself. When a nerve is inflamed, movement hurts. Then you start guarding, nearby muscles tighten, sleep gets worse, and the whole area becomes more sensitive. Over time, even simple tasks can feel bigger than they should.
An epidural injection can interrupt that pattern by lowering the irritation at the source. The spine's structure may still have age-related wear, a bulging disc, or narrowing. The injection helps create better conditions for the nerve to settle down so rehabilitation and daily activity become more manageable.
A successful epidural injection is targeted anti-inflammatory care designed to calm an irritated spinal nerve and help you function with less reliance on opioid medication.
Where this mechanism is most relevant
This biology is most useful when symptoms match an inflamed spinal nerve pattern, including:
- Sciatica from a lumbar disc herniation
- Leg pain from foraminal or spinal narrowing
- Arm pain from cervical nerve root irritation
- Some cases of back or neck pain where inflammation is clearly part of the picture
The main idea is simple. An epidural steroid injection helps reduce nerve inflammation and quiet pain signaling so the affected nerve has a chance to recover and you can return to a more active life with less pain.
Who Can Benefit from an Epidural Steroid Injection
In clinic, a common Chicago Ridge conversation sounds like this: “My back hurts, but the worst part is the pain shooting into my leg when I stand or walk.” That detail matters. Epidural steroid injections help specific patterns of spinal pain, especially when a nerve is irritated and the symptoms travel along that nerve’s path.
The best candidate is not defined by pain alone. We look for a match between three things: your symptoms, your physical exam, and your imaging. When those line up, an injection can place anti-inflammatory medication close to the problem area instead of treating pain in a broad, nonspecific way. That targeted approach fits our opioid-sparing philosophy at Midwest Pain & Wellness. The goal is simple: help you move better, sleep better, and stay active in daily life across the Chicago suburbs.
Common conditions that may respond well
Epidural steroid injections are often considered for:
- Lumbar disc herniation with sciatica, where pain starts in the low back or buttock and runs down the leg
- Foraminal or spinal stenosis, where narrowing around the nerve can trigger leg pain, heaviness, or burning with standing and walking
- Cervical radiculopathy, where a pinched nerve in the neck sends pain, tingling, or numbness into the shoulder, arm, or hand
- Some cases of axial back pain, if the history and exam suggest inflammation is a meaningful part of the problem
One evidence summary reported that outcomes vary by diagnosis. Patients with sciatica from disc herniation, foraminal stenosis, and some forms of axial back pain may all improve after epidural treatment, but the degree and duration of relief differ from one condition to another and from one person to the next review of epidural injection outcomes.
That variation is normal. A swollen nerve from a fresh disc herniation behaves differently than a nerve irritated by long-standing narrowing, scar tissue, or arthritis. The injection is most useful when your pain pattern tells us inflammation is a real driver of symptoms.
Signs your pain pattern may be a good fit
A good candidate often describes pain in a way that sounds familiar to spine specialists:
- "My pain shoots down one arm or one leg."
- "Standing or walking brings on the symptoms."
- "Coughing, sneezing, or certain positions make the pain flare."
- "The numbness or tingling follows a clear path."
That last point can be confusing. Back pain that stays only in the center of the low back is sometimes less responsive to an epidural than pain that radiates outward along a nerve. In simple terms, a traveling pain pattern gives us a clearer target.
Why careful selection matters
An epidural is not a generic fix for every sore back. It is a targeted treatment for the right diagnosis.
If your MRI shows one level, but your symptoms point to another, we pause and sort that out first. If your pain may be coming more from a joint, muscle, or sacroiliac problem than from an irritated nerve, a different treatment may make more sense. That is why a careful consultation matters more than the procedure name itself.
| Approach | Best general use | Why a specialist may choose it |
|---|---|---|
| Transforaminal | A specific irritated nerve root on one side | Most targeted delivery near the exiting nerve |
| Interlaminar | Wider or central spread of medication | Helpful when symptoms are less confined to one side |
| Caudal | Lower access through the sacral canal | Sometimes useful when anatomy or prior surgery changes the usual path |
Prior surgery, the shape of your spinal anatomy, the location of narrowing, and how your symptoms travel all influence whether an epidural is a reasonable option. If you want to see the wider range of spine and nerve conditions we evaluate for interventional pain treatment, that overview can help you understand where an epidural fits and where another treatment may be a better match.
The main question is not whether epidural injections help people in general. The key question is whether your symptoms, exam, and imaging point to a treatable source that an epidural can reach.
Injection Techniques Your Doctor May Choose
A patient in Chicago Ridge may come in saying, "My back hurts." But the pattern matters. Pain that shoots down one leg after getting out of the car at the Metra station is different from pain spread across the low back after a long day on your feet. That is why the injection route is chosen with care. Your doctor is matching the path of the medicine to the path of your pain.
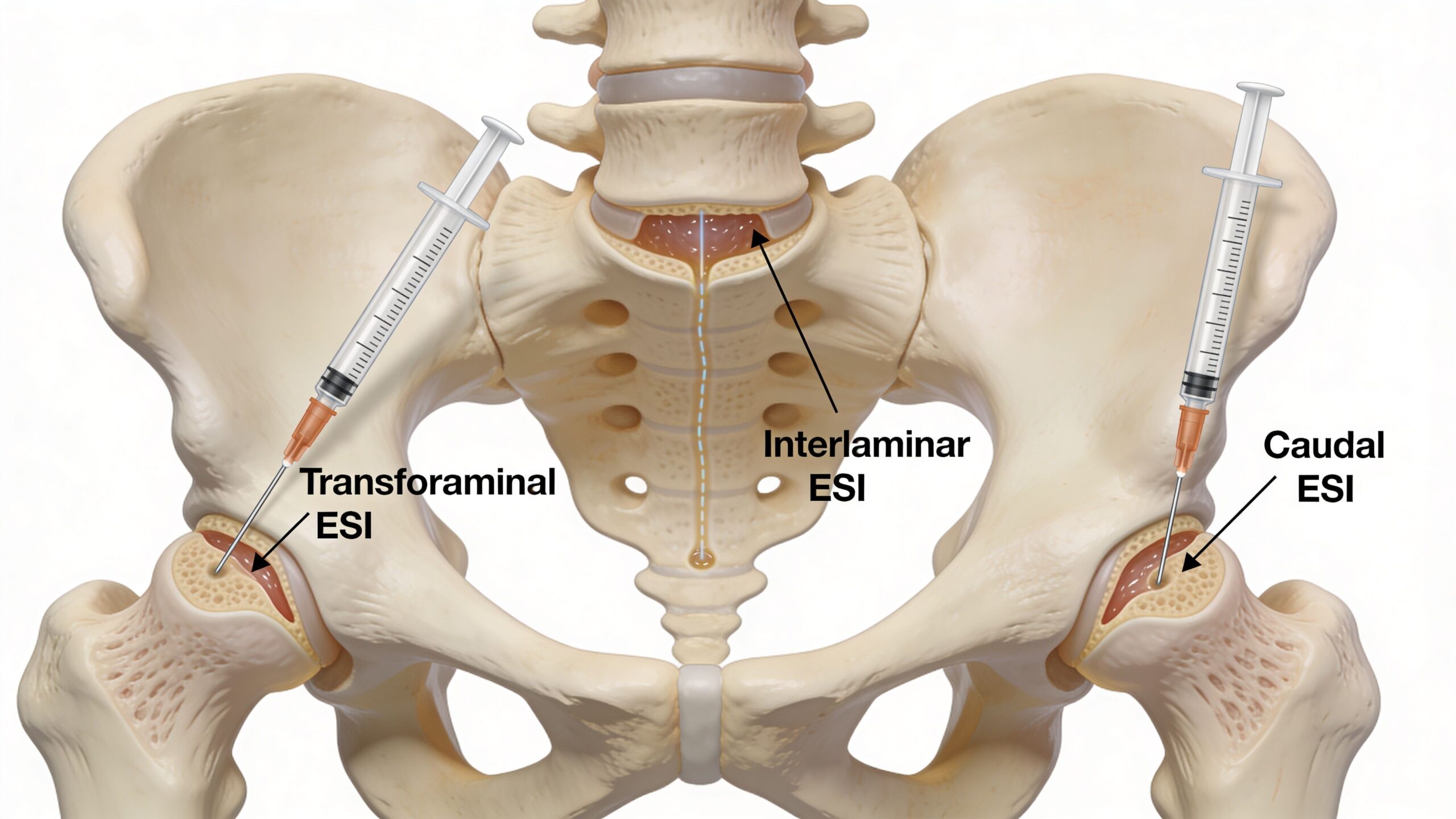
Transforaminal approach
A transforaminal epidural places medication near a specific nerve root as it leaves the spine. It is often chosen when symptoms follow one clear nerve pattern, such as one-sided sciatica from a disc herniation.
RadiologyInfo's epidural overview notes that transforaminal injections can provide superior short-term pain relief up to 6 months in 60% to 70% of lumbar radiculopathy cases, compared with 40% to 50% for caudal injections. That result fits the anatomy. When the irritated nerve is the main pain generator, placing medication closer to that nerve can make the treatment more precise.
For someone whose leg pain starts after ten minutes of walking around Lake Katherine or makes it hard to get through nine holes at a local course, that precision can matter.
Interlaminar approach
An interlaminar epidural enters from a more central path between the bony structures of the spine. The medication can spread across a broader area inside the epidural space.
This approach may make sense when symptoms are more diffuse, when both sides are involved, or when the doctor wants coverage across a wider region rather than one exact exit point. It is less like aiming at one doorway and more like placing medicine into the hallway where several irritated structures may be affected.
That can be a good fit for a patient whose goal is simpler daily movement. Standing at your kitchen counter, walking the aisles at Mariano's, or getting through a workday in the southwest suburbs without repeated pain flares.
Caudal approach
A caudal epidural reaches the epidural space through the sacral opening at the base of the spine. It works like entering the same canal from below.
This route is often helpful when prior surgery, scar tissue, or the shape of the anatomy makes another path less practical. It is usually less targeted than a transforaminal injection, but in the right patient it can still deliver medication where it needs to go.
That can be a smart option for someone focused on getting back to a steady routine, such as climbing stairs more comfortably, tolerating a longer commute, or keeping up with family activities on the weekend.
What the visit usually feels like
The names sound technical. The experience is usually calm and organized.
- Before the procedure: Your doctor reviews symptoms, medications, allergies, and imaging so the plan matches your diagnosis.
- During positioning: You are placed in a way that gives safe access to the treatment area, and the skin is cleaned carefully.
- During the injection: Local anesthetic numbs the skin first. Imaging guidance helps place the needle accurately.
- Right after: You are observed briefly and sent home with clear instructions about soreness, activity, and when to call.
Patients who want to review other image-guided procedures used for treatment at Midwest Pain & Wellness can see how each option is matched to a specific pain pattern.
The best technique is the one that fits your anatomy, your symptoms, and your goal of getting back to an active life with less reliance on opioid medication.
Your Epidural Injection Journey at Our Chicago Ridge Clinic
For many people, anxiety comes less from the injection itself and more from not knowing what the day will be like. When the process is explained clearly, most patients feel far more at ease.

Before procedure day
The visit starts with diagnosis, not rushing. Your doctor reviews where the pain starts, where it travels, what makes it worse, and what treatments you've already tried. Imaging is matched to your symptoms because an MRI finding alone doesn't always explain pain.
Medication review matters too. Blood thinners, diabetes medications, recent illness, and allergies may affect planning. This is also when patients ask practical questions about work, driving, and recovery.
For more about the physician behind this kind of evaluation, patients can review Dr. Donkoh's background and training.
During the injection
Most patients are surprised by how controlled the environment feels. The skin is cleaned, the area is numbed, and imaging guidance is used to help direct the needle accurately. The point is precision and safety, not speed for its own sake.
You may feel pressure during parts of the procedure. Some patients feel a brief reproduction of their usual pain when medication reaches the irritated area. That can be normal and short-lived.
Right after the procedure
Afterward, you'll spend a short period in recovery so the team can make sure you're feeling stable before discharge. The immediate numbness from local anesthetic can make the area feel different before the steroid has had time to do its anti-inflammatory work.
Most patients are told what level of soreness to expect, what activities to limit for the day, and what symptoms should prompt a call. Good pain care includes instructions, not just injections.
Balanced expectations matter
An epidural steroid injection can help significantly, but it isn't a guarantee and it isn't meant for every pain pattern. Good candidates are selected carefully because the treatment works best when the symptoms, anatomy, and injection route all line up.
That balanced approach is one of the reasons patients often feel more comfortable deciding whether an epidural makes sense for them.
Benefits Risks and Realistic Outcomes of ESIs
A good epidural steroid injection does not just aim to lower a pain score. It aims to give you enough breathing room to live more normally again. For many patients in Chicago Ridge and the surrounding suburbs, that means getting through a grocery run, sitting through a work shift, or walking through Chicago Ridge Mall without the familiar pull of leg pain forcing an early stop.
Relief can begin within days, though some patients notice the full anti-inflammatory effect closer to one to two weeks. The bigger point is function. If pain settles down enough for you to sleep, move better, and return to physical therapy, the injection has done something meaningful.
Benefits patients often notice
Success usually shows up in ordinary moments.
Common benefits may include:
- More comfortable walking and standing: You may be able to get through errands, stand in the kitchen longer, or enjoy a local park trail with fewer stops from back or leg pain.
- Better sleep: Calmer nerve irritation often means fewer nighttime wake-ups and less tossing to find a tolerable position.
- More productive physical therapy: Lower pain levels can make stretching, core work, and guided exercise more realistic.
- Less reliance on medication: A targeted injection may reduce the need for increasing doses of oral pain medicine, which fits an opioid-sparing treatment plan.
- More confidence with daily life: School drop-offs, commuting, housework, and social plans often feel more manageable when pain is not dominating every decision.
The injection is best understood as a window of opportunity. If inflammation quiets down, you and your doctor can use that window to restore strength, improve movement, and help you stay active in a way that lasts.
Risks and Side Effects to Discuss
Every procedure carries some risk. With an epidural injection, side effects can include temporary soreness, a short-term increase in pain, flushing, headache, or temporary numbness, depending on the injection site and medications used.
Serious complications are uncommon, but they still deserve a clear discussion in plain language. Your physician should explain how your anatomy, medical history, blood thinner use, diabetes status, and imaging findings affect the risk profile for you personally.
That conversation matters because the right question is not merely, "Can this help?" The better question is, "Do the likely benefits outweigh the risks for my specific pain pattern and goals?"
What matters most: A realistic outcome is meaningful pain relief that helps you function better. It may mean finishing a shopping trip, sleeping through the night more often, or getting back to exercise without relying more heavily on pain pills.
Three practical questions patients should ask
What exact diagnosis are you treating?
The explanation should connect your symptoms, exam findings, and imaging in a way that makes sense.What does success look like for me?
A useful answer should include real-life goals such as driving more comfortably, returning to work tasks, or walking farther with less leg pain.If the injection helps, what is the next step?
The best plans use pain relief as a chance to build progress through exercise, rehab, and other treatments that support longer-term improvement.
Frequently Asked Questions About Epidural Injections
Will the injection hurt
Most patients feel more pressure than pain. The skin is usually numbed first with local anesthetic, which helps with the initial part of the procedure. During the injection itself, you may notice pressure or a brief zing if the medicine reaches an already irritated nerve.
The experience is usually short. What tends to help most is knowing that unusual sensations during placement are often temporary and expected. If you're anxious, tell your doctor beforehand so the team can guide you through it calmly.
How many injections will I need
There isn't one fixed number that fits everyone. Some patients respond well after one injection. Others may need a short series, depending on how long symptoms have been present, how severe the inflammation is, and how much relief the first injection provides.
The more important question is not "How many can I get?" but "What changed after the first one?" If pain drops, walking improves, and daily function returns, that information guides whether another injection is worthwhile.
Can I drive myself home after the procedure
You should follow the instructions given by your treating physician. In many cases, patients are asked to arrange a driver, especially if there may be temporary numbness, weakness, or medication effects that could make driving unsafe right afterward.
Even if you feel fairly normal, it's smart to plan conservatively. A ride home removes stress and lets you focus on how your body responds over the next several hours.
How quickly will I know if it worked
You may notice early changes from the numbing medicine soon after the procedure, but the steroid effect usually takes longer. Some people feel improvement within days. Others need more time before the anti-inflammatory effect becomes noticeable.
A temporary return of pain after the numbing medicine wears off doesn't necessarily mean the injection failed. That's one reason follow-up matters.
Is an epidural injection a cure
Usually, no. It's better understood as a targeted treatment tool. For some patients, it provides enough relief that the pain settles for a long period. For others, it creates a window to move better, exercise more comfortably, and avoid surgery or stronger medication.
That doesn't make it a lesser treatment. It makes it part of a broader, evidence-based pain plan.
If back, neck, arm, or leg pain is limiting your life in Chicago Ridge, Oak Lawn, Palos Hills, Palos Heights, Worth, Bridgeview, Hickory Hills, Alsip, Burbank, Evergreen Park, or Orland Park, Midwest Pain & Wellness offers image-guided, opioid-sparing care led by a double board-certified interventional pain specialist. If you'd like a careful evaluation and a treatment plan built around function, diagnosis, and realistic relief, scheduling a consultation is a good next step.



