Botox usually starts working in 3 to 5 days, and the full effect is typically seen in 10 to 14 days. That timeline applies to both cosmetic use and medical treatment for chronic migraine and cervical dystonia.
If you're dealing with frequent headaches, neck tightness, or painful muscle spasms, that waiting period can feel longer than it sounds. Patients from Oak Lawn, Palos Hills, Palos Heights, Worth, Bridgeview, Hickory Hills, Alsip, Burbank, Evergreen Park, and Orland Park, Illinois often ask the same question in a very practical way: when will I feel a difference?
The short answer helps, but it doesn't tell you what those first two weeks really feel like. In pain management, expectation-setting matters. Botox is not a rescue treatment that flips symptoms off the same day. It's a targeted neuromodulator that works gradually, and the best results come when patients understand the timeline, follow post-procedure instructions carefully, and use it as one part of a broader opioid-sparing care plan.
Your Guide to the Botox Timeline for Pain Relief
A patient from Oak Lawn comes in after another week built around migraine days. A patient from Palos Hills describes neck pulling and spasm that make driving, working, and sleeping harder than they should be. In both cases, the first question is practical. How long will Botox take to help?
For pain treatment, the usual expectation is a gradual response over the first two weeks. Early changes often show up within several days, and the fuller benefit is commonly judged closer to the two-week mark. That timeline matters because Botox is usually one part of a plan for chronic migraine or cervical dystonia, not the only treatment on the calendar.
In practice, I tell patients to expect progression, not a sudden flip. You may notice less muscle tightness first. You may find that a headache trigger is less intense, or that neck posturing starts to ease before pain fully settles. Small changes count.
Clinical expectation: Botox follows a biologic timeline. It does not act like a same-day rescue treatment.
That point helps patients avoid two common mistakes. The first is deciding too early that the treatment did not work. The second is stacking other changes too quickly and making it hard to tell what is helping. In an opioid-sparing pain plan, timing matters. We often coordinate Botox with physical therapy, home exercise, trigger management, medication review, and, when appropriate, other targeted procedures so each part of care supports the next step instead of competing with it.
That is especially relevant for patients in Chicago Ridge and nearby Illinois communities who are trying to keep work, family responsibilities, and follow-up visits manageable. If Botox is being used for chronic migraine, we may track headache frequency and intensity over the next couple of weeks rather than judging the result by the first few days. If it is being used for cervical dystonia, we look for changes in muscle pull, posture, range of motion, and pain interference with daily activity.
A few expectations keep the process clear:
- Watch for gradual change: Relief usually builds over days.
- Judge the result at the right time: A follow-up window after the settling period gives a more accurate read.
- Use Botox as one part of care: It often works best alongside rehab, activity modification, and other non-opioid treatments chosen for the pain pattern being treated.
Patients generally do better when they know what the first two weeks are supposed to look like. That knowledge reduces unnecessary worry and helps us make better decisions about the rest of the treatment plan.
The Science Behind the Wait Why Botox Is Not Instant

Botox doesn't fail when it doesn't work instantly. It's doing exactly what it's supposed to do.
The medication has to reach the nerve endings involved in muscle contraction, enter those nerve cells, and then gradually interfere with the signaling machinery that releases acetylcholine. Botox's delayed onset is tied to this molecular process. It must be absorbed by nerve cells and cleave SNARE complexes before it can stop acetylcholine release at the neuromuscular junction, as described in Healthline's explanation of how Botox takes effect.
Why the effect builds over time
A simple way to think about it is a light switch with a delay in the wiring. The injection is the start of the process, not the finish line. The medication binds early, but the visible and physical result takes longer because the body still has to use up acetylcholine that's already available in the system.
That is why some people notice early softening or relaxation first, then a steadier and more complete effect later.
Why this matters for pain patients
For cosmetic patients, the delayed effect shows up as smoother movement or softer lines. For pain patients, it may show up as less spasm, less muscle pull, fewer trigger points aggravated by contraction, or a calmer pattern of headache generation.
Those changes don't always feel dramatic in the first few days. They often feel incremental.
Botox blocks the signal pathway gradually. Patients who know that ahead of time are less likely to mistake normal delay for treatment failure.
This is especially important in Palos Hills, Burbank, and nearby Illinois communities where many patients have already tried several treatments before considering Botox. If you've been dealing with pain for months or years, it's understandable to want immediate proof that something is finally helping. But Botox is one of those treatments where the biology rewards patience.
What doesn't work
Trying to "speed it up" doesn't help. Extra facial movement, rubbing the area, pressing on sore spots, or returning too soon for premature adjustments won't make the medication bind faster. The process unfolds on its own schedule.
The best approach is simple:
- Follow aftercare closely: That protects the injection pattern.
- Watch for gradual change: Small improvements count.
- Judge the result at the right time: Early second-guessing usually adds confusion, not clarity.
Botox Onset and Peak Timeline by Condition
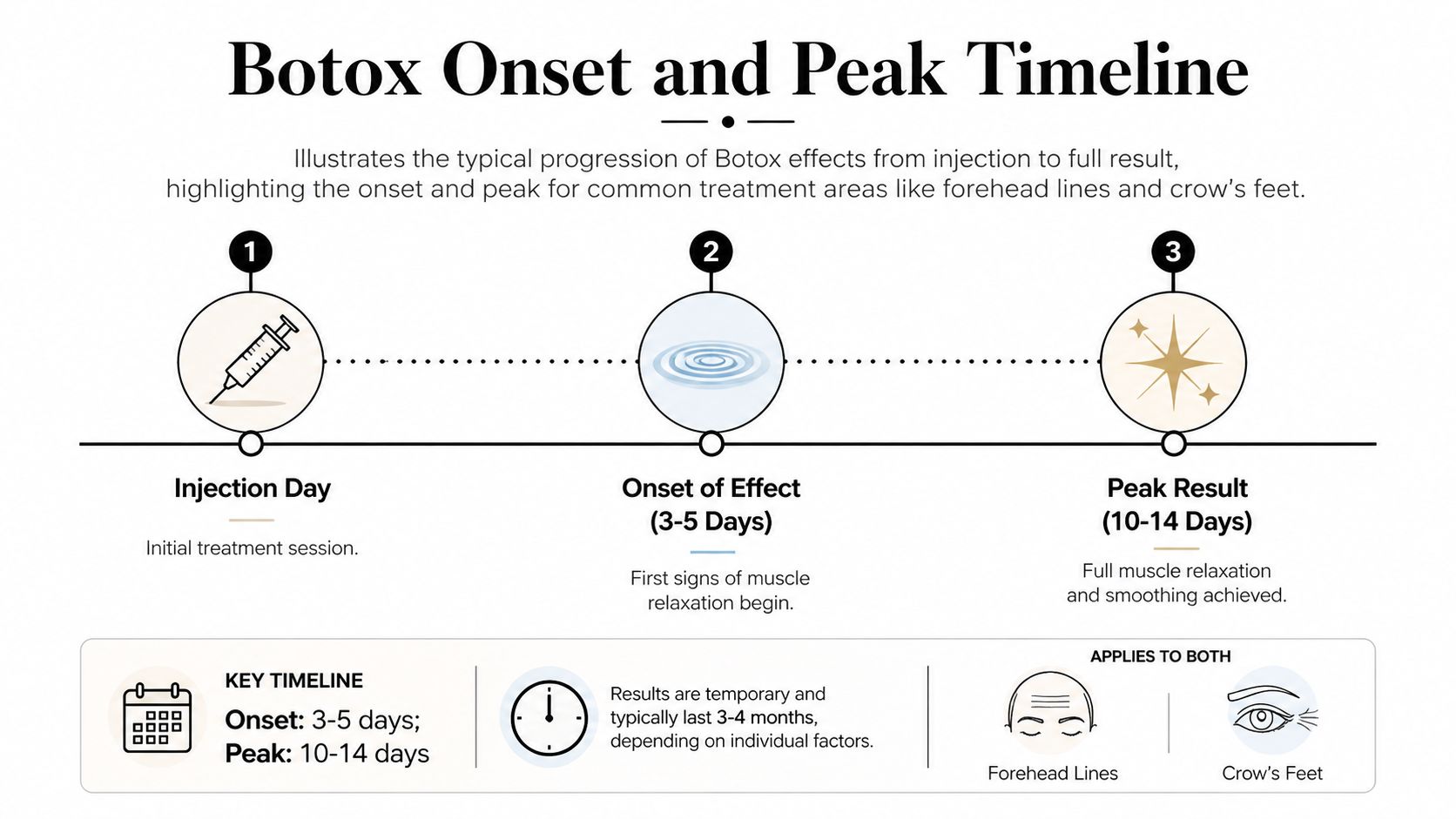
In pain medicine, the same drug timeline can feel different depending on what condition you're treating. A patient with chronic migraine may judge success by fewer headache days and less severity. A patient with cervical dystonia may notice the earliest improvement as reduced pulling, easier head positioning, or less pain with turning the neck.
Chronic migraine
For chronic migraine, Botox is a medical treatment with established clinical use. In the PREEMPT trials, Botox reduced headache days by 50%, as summarized in this discussion of Botox timing and therapeutic outcomes.
What patients often need to hear is this: the injection series may begin acting on schedule, but the way migraine relief is perceived can still feel gradual. Some people first notice that attacks are less intense. Others say the headaches still happen but feel less punishing. Some don't appreciate the benefit until they compare the next few weeks to what life looked like before treatment.
Cervical dystonia
With cervical dystonia, the treatment target is different. Here, the goal is to reduce involuntary muscle contraction and the pain that comes with abnormal neck posture or repetitive spasm. The same source notes that the HEADWAY trials showed a -4.7 point improvement on the TWSTRS pain and disability scale at 6 weeks, which fits with the expected pattern that Botox reaches peak effect around the two-week window and then continues to support symptom control over time.
For patients, the practical sign isn't a stopwatch. It's function. Turning the head may feel less restricted. Constant muscular guarding may ease. Sleep may improve because the neck isn't pulling as forcefully.
A simple comparison
| Condition | What you may notice first | When patients often start noticing change | When peak effect is expected |
|---|---|---|---|
| Chronic migraine | Less tension contribution, less intensity, fewer severe flares | Early changes may begin within the usual Botox onset window | 10 to 14 days |
| Cervical dystonia | Less pulling, reduced spasm, easier neck movement | Often within the first several days to week | 10 to 14 days |
The condition matters, but the core timing still holds.
For a broader look at headache, neck, spine, and nerve issues commonly managed in interventional practice, patients can review conditions we treat.
What to watch for after treatment
A useful way to track progress is to look at function instead of waiting for a dramatic single moment.
- Migraine patients: Pay attention to headache frequency, intensity, rescue medication use, and how often pain disrupts work or sleep.
- Cervical dystonia patients: Notice posture, range of motion, muscle tightness, and whether pain becomes less constant.
- Both groups: Keep notes rather than relying on memory. Symptom patterns are easier to judge when they're written down.
Don't evaluate Botox by asking, "Do I feel completely different today?" Evaluate it by asking, "Is the pattern improving over the next two weeks?"
That approach leads to better decisions and fewer false alarms.
Factors That Can Influence Your Botox Results

Botox has a typical timeline, but it isn't identical for every patient. Some notice clear change on the earlier side. Others need more time. A smaller group doesn't respond as expected and needs troubleshooting.
According to this review discussing delayed or absent Botox response, up to 10 to 15% of patients may have a delayed or absent response. Reasons can include strong muscles, higher metabolism, or anti-Botox antibodies. In repeat users, those antibodies occur in 1 to 5%, and the issue can be more relevant in higher-dose therapeutic protocols.
Common reasons the timeline varies
Some variation is straightforward and not concerning.
- Muscle strength: Stronger target muscles may take longer to relax fully.
- Metabolism: Some people process medications differently and notice a different onset pattern.
- Condition severity: A heavily overactive muscle group often doesn't feel the same as a mild problem responding to treatment.
- Treatment history: Repeat treatments may feel more predictable than a first experience.
When a weak response needs attention
A delayed result is one thing. No meaningful result after the expected settling period is another.
That doesn't automatically mean Botox "doesn't work" for you. It may mean the injection pattern needs refinement, the target muscles need reassessment, the dose needs adjustment, or a different neurotoxin should be considered. The same review notes that switching to Xeomin can be a reasonable troubleshooting option because it has lower immunogenicity.
What helps most: careful reassessment, not rushing to conclusions and not repeating injections too early without a plan.
What patients can do well
Patients can't control every biologic variable, but they can avoid sabotaging a good treatment.
A few practical points matter:
- Give it enough time. Judging too early is the most common mistake.
- Follow positioning instructions after treatment. Technique and aftercare affect predictability.
- Report what changed and what didn't. Specific feedback is much more useful than "it sort of worked."
- Track symptom patterns. For migraine, note headache burden. For dystonia, note spasm intensity and neck function.
If you're in Worth, Hickory Hills, or nearby Illinois communities and your response seems slower than expected, the right next step is medical review, not frustration. Botox is precise treatment. Precision includes adjusting the plan when the first pass isn't enough.
What to Expect After Your Botox Injections in Chicago Ridge

You leave the office in Chicago Ridge after Botox for chronic migraine or cervical dystonia and feel about the same. That is the usual course. The first day is mainly about protecting the injection sites and avoiding anything that could make placement less predictable.
Patients often expect to feel a change right away. In pain practice, I set expectations differently. Injection day is usually quiet. Relief, if Botox is the right fit, develops later as the medication starts reducing the abnormal muscle signaling that contributes to headache patterns or neck spasm.
What the first day usually looks like
Mild soreness, small raised areas, pinpoint redness, or a bruised feeling at a few injection sites can happen. These short-lived effects are common after needle-based treatment and do not tell us yet whether the medication will help your pain.
For patients being treated as part of an opioid-sparing plan, the early goal is simple. Get through the day comfortably, follow aftercare instructions, and keep the rest of your migraine or dystonia plan on track. That may include your current medications, physical therapy, sleep work, or other procedures used for treatment if Botox is only one part of care.
Aftercare that matters
- Stay upright for several hours after treatment: Avoid lying flat right away.
- Do not rub or massage the treated areas: Pressure can shift medication away from the intended muscles.
- Skip hard exercise and excessive heat that day: Heavy exertion, hot yoga, saunas, and anything that causes intense flushing can increase irritation around fresh injection sites.
- Use a light touch: Washing your face or scalp is fine. Aggressive pressure is not.
- Resume normal routine carefully: Desk work, light errands, and gentle activity are usually fine unless your clinician gave different instructions.
Simple steps make a difference.
When to contact your clinician
Call if you develop swelling that seems out of proportion, trouble swallowing, new muscle weakness outside the treated area, or any reaction that feels concerning rather than mildly annoying. Patients treated for cervical dystonia should be especially attentive to swallowing changes or head drop. Patients treated for migraine should let us know if they develop symptoms that are different from their usual headache pattern.
A second reason to check in is practical. If the post-treatment period is harder than expected, we may need to adjust the next session's dose, injection sites, or the broader pain plan.
For patients in Oak Lawn, Palos Hills, Evergreen Park, Bridgeview, and nearby Illinois communities, the first day after Botox is usually uneventful. The useful question is not whether you feel different that afternoon. The useful question is whether your symptoms begin to shift over the next several days and weeks in a way that supports steadier, lower-risk pain control.
Planning Your Treatment Journey for Lasting Relief
You have your first round of Botox, the first few weeks go well, and then the practical question comes up. When should the next treatment be planned so relief does not wear off all at once?
That question matters in pain management. For chronic migraine and cervical dystonia, Botox works best as part of a broader opioid-sparing plan that may also include physical therapy, home exercise, sleep work, medication review, and targeted procedures when needed. The goal is not only temporary symptom relief. The goal is steadier function with fewer bad stretches between visits.
In practice, the benefit from Botox is temporary. The exact duration varies by condition, dose, injection pattern, and individual response, but patients usually do better when we plan ahead instead of waiting for symptoms to return at full intensity.
Why consistency matters
Chronic migraine and cervical dystonia tend to build back gradually. Patients often notice more headache days creeping in, tighter neck muscles, worse head position, poorer sleep, or a drop in daily tolerance before they feel completely back to baseline. If treatment is delayed until that point, the next cycle can feel harder than it needed to be.
I encourage patients to watch for the pattern, not a single bad day. That is especially helpful for residents of Oak Lawn, Palos Hills, Chicago Ridge, and nearby communities who are balancing work, family, and long commutes and need their treatment plan to be realistic.
How Botox fits into a broader pain plan
Botox is rarely the whole answer. It is one treatment within an interventional pain strategy built around the actual pain generator.
For migraine, that may mean combining Botox with trigger management, non-opioid medications, and careful follow-up on headache frequency and function. For cervical dystonia, it often means pairing injections with movement work, posture correction, and reassessment of which muscles are driving pain and abnormal pull. Good planning keeps each part of care working in the same direction.
A few habits make long-term treatment more effective:
- Book follow-up before relief fades too far: Scheduling early is often easier than trying to get in once symptoms flare.
- Track function, not just pain: Fewer migraine days, less rescue medication use, better neck rotation, and better sleep are useful markers.
- Note when benefit starts and when it tapers: That helps guide the timing of the next session.
- Coordinate other treatments: Therapy, procedures, and medication changes should fit the Botox cycle when possible.
Patients do best when the plan is adjusted over time. If the first cycle helps but does not last long enough, or if one symptom improves more than another, the next treatment can often be refined. Dose, muscle selection, and timing all matter.
If you want to build a treatment schedule that fits your condition and daily life, you can request a visit through our Botox consultation and appointment page.
Frequently Asked Questions About the Botox Timeline
Does the first Botox treatment take longer to work?
Sometimes it can feel that way, especially because first-time patients don't always know what subtle improvement feels like. The more reliable approach is to judge the first treatment at the expected assessment window and track symptoms carefully rather than relying on memory.
If I don't feel much at first, should I assume it didn't work?
No. Early underwhelming results are common because Botox develops gradually. Pain relief can also be less obvious than cosmetic change because you're measuring symptoms and function, not just appearance.
Can I make Botox work faster?
No. You can't rush the biologic process once the injections are placed. The best thing you can do is follow aftercare instructions and let the medication work on schedule.
What if I see no result after two weeks?
That's the point to contact your treating clinician for review. A poor response may reflect the target muscle pattern, dose, technique, or your individual biology. It doesn't always mean Botox is the wrong treatment, but it does mean the next step should be guided by a medical assessment.
If there is no clear benefit after the expected window, the answer is follow-up, not guesswork.
Is the timeline different for pain relief than for cosmetic Botox?
The core mechanism is the same. The difference is how patients perceive success. Cosmetic patients often watch for visible muscle softening. Pain patients may notice improvement through fewer headaches, less neck pulling, better sleep, or easier daily function.
How should I track my response?
Keep it simple and specific.
- For migraine: Write down headache days, severity, and rescue medication use.
- For cervical dystonia: Note pulling, spasm intensity, turning limits, and pain with activity.
- For both: Record changes over the first two weeks and then over the following months.
That record helps your clinician decide whether to continue the same plan or adjust it.
If you're looking for evidence-based, opioid-sparing treatment for chronic migraine, cervical dystonia, or other persistent pain conditions in Chicago Ridge and nearby Illinois communities, Midwest Pain & Wellness offers personalized care led by a double board-certified interventional pain specialist. Schedule a consultation to find out whether Botox fits your treatment plan and what timeline to expect for meaningful relief.



