If you're in Oak Lawn, Orland Park, Palos Heights, Bridgeview, Worth, Evergreen Park, Hickory Hills, Alsip, Burbank, or Palos Hills, this question usually comes up after the same frustrating pattern. You had a steroid injection. It helped. You slept better, walked easier, sat longer, or made it through work without constantly shifting in your chair. Then the pain returned, and now you're wondering whether another injection is smart, risky, or both.
That’s a reasonable concern.
“How many steroid injections?” sounds like a simple numbers question, but it usually isn’t. The safer answer depends on where the injection goes, what steroid is used, how long the last one helped, and what your broader pain plan looks like over years, not just this month. A patient with lumbar radiculopathy, a patient with knee arthritis, and a patient with shoulder pain before surgery should not all get the same answer.
As an interventional pain specialist, I want patients to think about injections the right way. A steroid shot can reduce inflammation and create a window for better movement and recovery. It does not usually cure the underlying structural problem. If you keep repeating injections without asking whether they are still meaningfully helping, you can end up chasing temporary relief instead of building a durable plan.
That matters in pain management. The goal is not to collect procedures. The goal is to restore function, protect tissue, and avoid leaning on opioids or excessive interventions when a more thoughtful strategy would serve you better.
Your Guide to Steroid Injections in the Chicago Area
A common scenario goes like this. Someone from Worth or Bridgeview gets an epidural steroid injection for leg pain from a disc problem. The first shot settles the pain enough to drive, work, and sleep again. A few months later, the pain starts creeping back, and the next question is immediate: “Can I just get another one?”
Sometimes the answer is yes. Sometimes the better answer is not yet. Sometimes the right answer is no, because the first injection did too little, wore off too fast, or points us toward a different pain generator altogether.
The question behind the question
When patients ask how many steroid injections they can have, they’re usually asking several things at once:
- Safety: Am I damaging anything by repeating this?
- Timing: How close together can these be?
- Effectiveness: If the first one helped only briefly, is another one worth it?
- Long-term planning: What happens if I’m dealing with back, neck, or joint pain for years?
Those are the right questions.
Practical rule: A good injection plan is never just about the next shot. It’s about what repeated steroid exposure means for your body over time.
That’s especially important for adults dealing with chronic spine and joint conditions in the southwest suburbs. Many people are still working, caring for family, trying to stay independent, or recovering from prior injuries and surgeries. They don’t want vague reassurance. They want a clear answer that respects both pain relief and long-term safety.
What patients often get wrong
The biggest mistake is assuming that if one injection helped, repeating the same injection over and over must be the best strategy. It isn’t.
The second mistake is assuming there’s a universal lifetime number that applies to everyone. There isn’t. Some body areas have tighter practical limits than others, and your medical history changes the calculation.
A useful discussion about steroid injections should cover three things at once:
| What matters | Why it matters | What it changes |
|---|---|---|
| Body area | Spine, shoulder, knee, and small joints tolerate repeated steroid exposure differently | Frequency and spacing |
| Patient factors | Diabetes, bone health, prior surgery, age, and healing capacity affect safety | Steroid choice and repeat decisions |
| Response to prior injection | Duration and quality of relief tell us whether the treatment is still worthwhile | Whether to repeat, modify, or stop |
If you’ve been asking yourself how many steroid injections you can safely receive, don’t reduce that decision to a single number. The number matters, but the reasoning matters more.
Understanding the Basic Rule for Steroid Injection Frequency
A patient from Oak Lawn gets good relief after an epidural, starts walking better, sleeping better, and asks the next question at the follow-up. “How many of these can I have?”
The short answer is that many clinicians use a general ceiling of a few steroid injections per year in the same region, and they usually space them out over time, as noted in this review of steroid injection frequency guidance. That rule is a starting point. It is not a treatment plan.

What matters more is whether the injection meaningfully improved function. If you can stand longer, drive with less pain, return to work, or sleep through the night, a repeat injection may still have value later. If relief lasted only a few days or barely changed anything, repeating the same steroid injection on autopilot is usually poor medicine.
I explain this as long-term management, not yearly quota filling.
Steroid exposure adds up over time. The local tissue matters. Your overall health matters. The specific steroid matters too, because some formulations stay in the system longer or create more blood sugar disruption than others. For a patient with diabetes in Orland Park, that changes how aggressively I repeat injections. For a patient with fragile bone health, prior surgery, or several injections already on record, it changes the conversation again.
Why spacing matters
Spacing is part safety and part decision-making.
A gap between injections gives time to see the true result of the prior treatment. It also reduces the chance of stacking steroid exposure too quickly and losing sight of whether the injection is still helping enough to justify another one. Good pain care is not just about calming inflammation today. It is about preserving options for next year and five years from now.
That is why I do not look at steroid injections as a stand-alone answer. I use them alongside other interventional pain treatment options and a broader plan to restore movement, function, and independence without leaning on opioids or excessive procedures.
What the basic rule actually means
The basic rule supports a few practical decisions:
- Use the lowest exposure that has a real clinical payoff
- Leave enough time between injections to judge the result accurately
- Repeat only when the last injection produced meaningful functional benefit
- Stop repeating the same treatment when benefit becomes weak, brief, or inconsistent
- Plan for the long term, especially in patients who may need pain care over many years
Here is the practical framework I use:
| Guiding idea | Practical meaning |
|---|---|
| A yearly limit is a ceiling, not a goal | No one should receive repeat injections just because calendar time passed |
| Relief must justify repetition | Better walking, sleeping, working, or daily activity matters more than a temporary drop in pain score |
| Steroid choice affects frequency | Some steroids and some patient profiles call for more caution |
| The plan should age well | A useful injection today should not create avoidable problems later |
Used well, steroid injections can buy time, calm a flare, and help you stay active. Used too often, they lose value and narrow future options. The right number is the number that helps you function safely, with a plan that still makes sense years from now.
Injection Limits by Body Area and Type
A patient from Oak Lawn may do very well with one lumbar epidural during a bad sciatica flare, then go a year or longer without needing another. A patient with shoulder arthritis may get short relief from an intra-articular injection, but repeated shots into the same joint can become a poor trade if the benefit keeps shrinking. The body area matters because the tissue at risk is different, the goal is different, and the long-term plan should be different too.
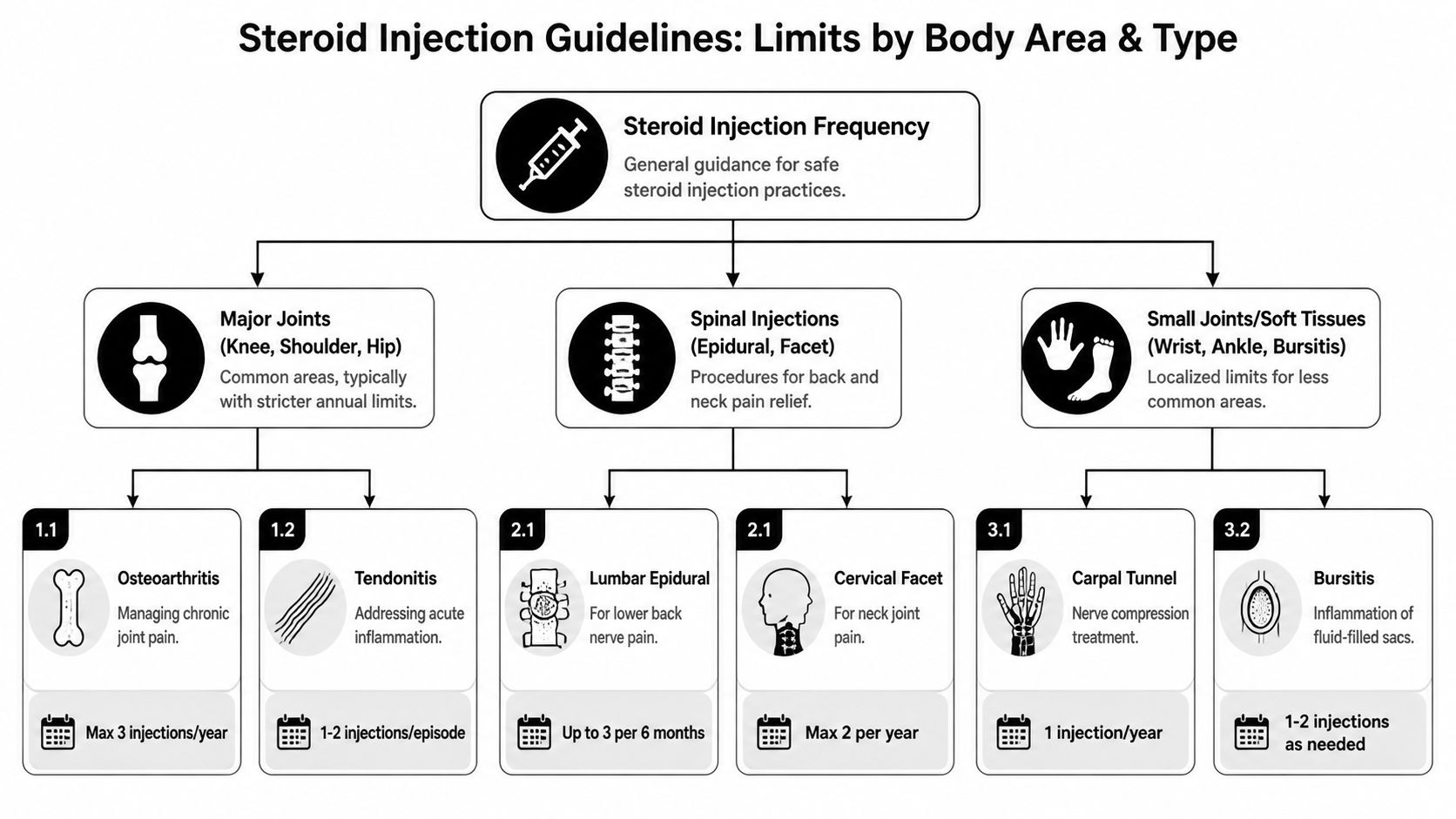
For spinal pain, joint pain, and small joint arthritis, I do not use one universal tally. I look at the specific structure being treated, how much relief the last injection gave, how long it lasted, and whether repeating it protects function or just postpones a better decision. That is how steroid use stays useful over years instead of becoming a reflex.
Patients also deserve to hear that not every procedure involves steroid. In many cases, a better next step is one of the interventional pain procedures used for treatment that targets the pain generator without adding more steroid exposure.
Epidural steroid injections for back and neck pain
An epidural steroid injection, or ESI, is usually meant to calm inflamed spinal nerve roots. The target is nerve-related arm or leg pain, not every type of neck or back pain.
For the same spinal region, many practices stay within about 3 to 4 steroid injections per year. That number is a ceiling, not a schedule. In practice, the better question is whether the injection changed daily life in a meaningful way. Better walking, sitting, driving, sleeping, or getting through work matters more than a temporary drop on a pain scale.
I repeat an ESI when three things line up:
- The first injection produced clear functional improvement
- Relief lasted long enough to justify another exposure
- The symptoms still match the same nerve-based diagnosis
I slow down or change course when the first injection gave little benefit, wore off quickly, or the pain pattern changed. At that point, more steroid in the same area often gives less return and adds exposure that may not help you over the long run.
Intra-articular joint injections
A steroid injection inside a joint follows a different logic. The issue is not only total steroid exposure. Local tissue effects matter too, especially in weight-bearing joints or joints that may eventually need surgery.
A knee, shoulder, or hip injection can be very reasonable for an inflammatory flare or to help someone participate in therapy and regain motion. It becomes less appealing when repeated injections are being used to carry a joint that is mechanically failing, unstable, or steadily wearing down. Temporary relief can hide a problem that needs a different treatment path.
The shoulder is a good example. A large 2019 Arthroscopy study looked at patients undergoing rotator cuff repair and found that multiple shoulder corticosteroid injections within the year before surgery were associated with higher revision surgery risk, according to this PubMed record of the Arthroscopy study.
That does not mean one properly chosen joint injection is unsafe. It means repeated injections into the same joint deserve a longer view, especially if surgery may become part of the plan later.
Small joints and hand injections
Small joints have less margin for error. The joint space is smaller, the surrounding soft tissue is smaller, and repeated injections can reach the point of diminishing return sooner.
For hand and small joint arthritis, many specialists keep the number of corticosteroid injections limited per joint over time, as described in this Arthritis Foundation overview of hand injections. In clinic, that usually means being selective. If a thumb joint injection gives durable relief and better pinch strength, repeating it later may make sense. If the effect is brief and function keeps slipping, the plan should change.
Each joint has its own history. A thumb CMC joint, a knee, and a lumbar epidural should not be lumped into one lifetime count.
Nerve blocks and related procedures are not all the same
Patients often call everything a "shot." Medically, that is too broad to be useful.
Some injections contain steroid. Some do not. Diagnostic medial branch blocks are different from epidural steroid injections. Radiofrequency ablation is different from both. Sacroiliac procedures, peripheral nerve treatments, and some regenerative approaches follow their own rules and may reduce how often steroid is even part of the plan.
The practical question is simple. What structure is causing the pain, and what treatment addresses that structure with the least cumulative downside?
A quick comparison
| Injection type | Main target | Why limits matter |
|---|---|---|
| Epidural steroid injection | Inflamed spinal nerve roots | Repeat benefit may fall off, and cumulative steroid exposure adds up |
| Joint injection | Arthritis or joint inflammation | Local cartilage, tendon, and surgical planning all matter |
| Small joint injection | Hand or other small joints | Small tissue space and shorter runway for repeated steroid use |
| Nerve block or non-steroid procedure | Specific nerves or pain pathways | May control pain without adding steroid burden |
The safest frequency depends on more than body part alone. It depends on what tissue is being treated, what steroid is being used, and whether the injection is helping you stay active in a way that still makes sense five, ten, or twenty years from now.
How Your Personal Health Profile Affects Injection Safety
A 52-year-old patient from Orland Park and a 72-year-old patient from Oak Lawn can show up with the same scan and still leave with different injection plans. That is normal. Safe steroid use depends on the whole patient, not just the body part that hurts.

In practice, I look at four questions before recommending another steroid injection. What medical conditions are in the background? How did you respond last time? Which steroid are we considering? Are we using this injection to restore function for a meaningful stretch of time, or are we repeating it because nothing else has been organized yet?
That last point matters. A good plan for chronic pain has to work not only this month, but years from now. If you are being treated for back, neck, joint, or nerve pain, the diagnosis itself shapes the safest path, which is why the full range of conditions we treat in interventional pain management matters when deciding whether steroid should stay in the plan.
Diabetes changes the conversation
Diabetes is one of the clearest examples of why the usual injection limit is only a starting point. Steroids can raise blood sugar for a short period after an injection. For some patients, that is manageable with planning. For others, especially if control is already inconsistent, it can turn a helpful treatment into a rough few days.
Before I recommend an injection for a patient with diabetes, I want to know:
- How controlled the blood sugar has been recently
- Whether a prior steroid injection caused a significant spike
- Whether a lower systemic exposure approach makes more sense
- Whether the likely pain relief is strong enough to justify the temporary glucose disruption
A patient with brittle diabetes may still be a candidate. The treatment just has to be chosen carefully, timed appropriately, and coordinated with the physician managing the diabetes.
Steroid selection affects how often repeat treatment is reasonable
Patients are often told that "a steroid shot is a steroid shot." That is not accurate enough to guide long-term care.
Different corticosteroids have different durations, particle characteristics, and risk profiles. In some settings, that affects how often I am willing to repeat an injection and which route I prefer. Dexamethasone, triamcinolone, and betamethasone are not interchangeable in every patient or every procedure. The safer choice may depend on the location being treated, your medical history, and how much cumulative exposure you have already had.
This is one reason I do not build a treatment plan around a fixed annual number alone. I build it around total steroid burden over time.
Age, bone health, and the long view
A younger patient with recurring pain needs a different discussion from a retired patient with osteopenia, prior fractures, or frail tissue. The question is not only how many injections are allowed this year. The question is what repeated steroid exposure means over ten, fifteen, or twenty years.
For younger patients, repeated injections can become a habit before anyone has stepped back and asked whether the diagnosis is correct or whether a non-steroid strategy would serve them better. For older patients, bone density, tendon quality, skin integrity, fall risk, and surgical planning matter more with each repeat procedure.
I want every injection to earn its place in the long-term plan.
Prior response is one of the best decision tools
The safest repeat injection is usually the one that has already shown a clear, practical benefit. I care less about whether you felt "a little better" and more about whether you functioned better.
Use prior response this way:
| Prior result | What it suggests |
|---|---|
| Clear, meaningful relief | The target was likely correct, and repeat treatment may be reasonable if function improved |
| Minimal relief | The pain generator or procedure choice may need to be reconsidered |
| Very brief relief | Steroid may not be the right long-term tool for this problem |
| Relief with side effects | The medication choice, dose, or procedure type may need to change |
If one injection helped you walk farther, sleep through the night, or get back to work for a meaningful period, that is useful information. If it gave you two days of partial relief and a week of high sugars or insomnia, that is useful information too. I do not count those outcomes the same way, and neither should your treatment plan.
A disappointing injection still helps guide care. It can prevent months or years of repeating the wrong procedure.
Previous surgery and structural problems matter
Patients with prior spine surgery, advanced arthritis, tendon injury, joint instability, or a problem that may need surgery require a more disciplined approach. Steroids reduce inflammation. They do not repair a torn tendon, reverse joint collapse, or correct mechanical instability.
That distinction changes how often repeat injections make sense. In some cases, an injection is a smart bridge while physical therapy, weight loss, surgical evaluation, or a more durable procedure is being arranged. In other cases, repeating steroid becomes a delay tactic that keeps pain temporarily quieter while function continues to decline.
The right number of injections is personal. It depends on your diagnosis, your health conditions, the steroid being used, and what kind of life you need that treatment to support over time.
The Risks of Too Many Injections and Long-Term Safety
A patient from Orland Park gets good relief from a knee or spine injection, then asks the next practical question. “How many times can I keep doing this before it becomes a problem?” That is the right question. The answer is not a simple yearly cap. It is a long-term safety decision based on what tissue is being treated, how your body handles steroid exposure, and whether each injection is still buying real function.
Overuse creates two kinds of risk. One is local. That includes skin changes, soft tissue thinning, cartilage wear, and tendon weakening near the treatment site. The other is systemic. Steroid absorbed into the bloodstream can push blood sugar up, disturb sleep, trigger flushing, and add to cumulative exposure over time.
The local risk matters more than many patients realize. Around tendons and certain joints, repeated steroid can make future treatment harder. In shoulder care, surgeons have raised concern that multiple injections before repair may leave tissue in worse shape for healing. The lesson is practical. An injection that helps you function during a flare is very different from repeating the same shot into a struggling structure year after year without changing the plan.
I also discuss the lifetime view, especially with younger patients from Oak Lawn who may be dealing with pain for decades. Medicine does not give us a clean lifetime maximum for steroid injections. That uncertainty is exactly why I use them selectively. The goal is not to see how many you can safely accumulate. The goal is to use the fewest injections necessary to keep you moving while we build a treatment plan that lasts.
That approach changes the conversation.
A 68-year-old with severe knee arthritis waiting for surgery has a different risk-benefit profile than a 42-year-old with recurring tendon pain, diabetes, and many active working years ahead. The steroid type matters. The dose matters. The body area matters. Your health conditions matter. Safe frequency is never just a number copied from a handout.
Here is the standard I use in practice:
A repeat injection should clear four tests before it makes sense.
- The first injection improved function in a meaningful way. Less pain alone is not enough if you still cannot walk, sleep, work, or participate in therapy better.
- The benefit lasted long enough to justify more steroid exposure. A few days of mild relief usually does not earn a repeat.
- The target is still correct. If the diagnosis has changed, repeating the same procedure is poor medicine.
- There is a larger plan beyond another shot. That may include rehab, weight loss, bracing, regenerative options, radiofrequency treatment, surgical evaluation, or another non-opioid strategy.
What does not age well is habitual steroid use. I see this in patients who have been getting the same injection on a schedule for years because it is familiar and temporarily helpful. Over time, the returns often shrink while the downside grows. Blood sugars become harder to control. Tissue quality becomes a concern. The underlying arthritis, stenosis, or tendon damage continues to progress.
That is why long-term pain care should be managed like a lifecycle, not a series of isolated flare visits. Each injection needs a reason. Each repeat needs a measurable benefit. Each year of treatment should move you toward better function with less reliance on steroid, not quiet acceptance of the same short-term fix.
If your current pattern of injections is starting to feel automatic, schedule a pain management evaluation to review your long-term injection strategy. A careful plan protects future options while treating the pain you have right now.
Your Comprehensive Pain Strategy at Midwest Pain & Wellness
A steroid injection should be viewed as one tool, not the whole toolbox. It can put out the inflammatory fire. That window may let you move better, sleep better, tolerate rehab better, and avoid an opioid-centered path. But if that’s all you do, the benefit often remains temporary.
The stronger approach is multimodal and diagnosis-driven.
What a durable plan usually includes
When pain is persistent, the right strategy often combines several layers:
- Precise diagnosis first: Not all back pain is disc pain. Not all shoulder pain is joint pain. The structure causing symptoms has to be identified accurately.
- Targeted procedures when indicated: Epidural steroid injections, medial branch blocks, sacroiliac interventions, and other image-guided treatments can reduce pain in the right setting.
- Non-opioid progression: If the issue is facet-mediated pain, radiofrequency ablation may be more durable than repeating steroid indefinitely.
- Advanced options for selected patients: Peripheral nerve stimulation, spinal cord stimulation, MILD, Vertiflex Superion, kyphoplasty, PRP, cell-based therapies, and Botox all have different roles depending on the condition.
- Care coordination: Good pain care often requires communication with surgeons, primary care physicians, chiropractors, and rehab clinicians.
Why this matters more than another shot
The practical mistake many patients make is asking, “Can I get another injection?” before asking, “What is the long-term plan if this pain keeps coming back?”
That second question is the one that protects you.
If an injection gives enough relief to help you function while another treatment addresses the more durable problem, that’s smart use. If the same injection is being repeated because no one has built a broader strategy, that’s when care becomes reactive.
A thorough plan aims to do four things at once:
| Goal | Why it matters |
|---|---|
| Reduce pain | You need symptom control to live and function |
| Preserve tissue | Short-term relief should not create avoidable long-term damage |
| Improve function | Walking, working, sleeping, and caring for yourself matter more than a pain score alone |
| Limit opioid reliance | Chronic pain deserves better than escalating medication dependence |
A long-horizon way to think about treatment
For many adults in the Chicago Ridge area and surrounding suburbs, pain management is not a two-week problem. It may be a condition that needs steady, thoughtful care over years. That changes the standard.
A long-horizon pain plan asks:
- Is this injection buying real function?
- Is there a more durable procedure for this pain generator?
- Are we using steroid too often because the diagnosis is incomplete?
- How do we keep treatment sustainable over time?
If you answer those questions accurately, the role of steroid injections becomes clearer. They are valuable. They just work best inside a broader opioid-sparing strategy.
When you're ready to have that kind of conversation, it helps to request an evaluation rather than another automatic repeat procedure. You can start that process through the appointment page for Midwest Pain & Wellness.
Frequently Asked Questions About Steroid Injections
A common office conversation goes like this: a patient from Oak Lawn gets good relief from one knee or back injection, then asks whether repeating it every few months is the plan for years. The honest answer is that frequency depends on more than a simple yearly cap. I look at the body area, the steroid used, how much function you gained, and whether your health profile makes repeated steroid exposure riskier over time.
Is the 3 to 4 limit per joint or for my whole body
In practice, that rule is usually discussed per treated area. A knee, shoulder, spine region, or sacroiliac joint may each have their own practical limit.
Total steroid exposure still matters. If you are getting injections in several areas, I factor in the cumulative burden, especially if you have diabetes, osteoporosis risk, glaucoma, immune concerns, or a history of steroid side effects.
What if my injection barely helped
A poor response is a reason to reconsider the diagnosis or the treatment plan.
If relief lasted only a few days, or never clearly improved walking, sleeping, working, or daily activity, repeating the same injection often gives you more steroid without much return. In that setting, I want to know whether the pain source was identified correctly, whether the problem has changed, or whether another treatment would fit better.
If one injection worked, should I keep getting them forever
Only if the pattern still makes medical sense.
An injection that gives durable relief and helps you stay active can be used selectively. An injection that works for shorter and shorter periods, or has to be repeated on a tight schedule just to keep you afloat, usually signals a need to adjust course. Over a long treatment horizon, the question is not just whether it helped once. The question is whether it remains a good trade-off for the tissue involved and for your future options.
Is there a safe lifetime maximum
There is no universally accepted lifetime maximum.
That is one reason I do not build pain care one calendar year at a time, especially for younger adults or patients dealing with chronic spine, joint, or nerve pain. If you may need treatment for many years, every injection should fit into a longer plan that protects function and limits avoidable steroid exposure.
Do different steroids affect how often I can get injections
Yes. Steroid choice matters.
Some steroids are longer-acting, some are more soluble, and some are more likely to affect blood sugar or create concerns in certain tissues. The dose matters too. Two injections are not automatically equivalent just because both included steroid. Safer timing depends on what was injected, where it was placed, and why it was chosen.
Can I still get steroid injections if I have diabetes
Often, yes. The plan just needs more care.
Steroids can raise blood sugar for a period after the injection, so I consider your diabetes control, the urgency of the procedure, the steroid type, and how you will monitor glucose afterward. For some patients in Orland Park or Oak Lawn, that means adjusting timing and setting expectations clearly before we proceed.
Are injections the same as nerve blocks or ablation
No. They serve different purposes.
Some procedures use steroid to calm inflammation. Some use local anesthetic mainly to confirm the pain generator. Radiofrequency ablation does not rely on steroid in the same way and may offer a longer window of relief for the right diagnosis. That distinction matters if the goal is to reduce repeat steroid exposure over the next several years.
What about workers’ compensation or injury cases in Illinois
These cases often require tighter documentation and clearer proof of functional benefit.
The standard should still stay the same. Match the procedure to the diagnosis, document what improved, and avoid repeating injections that are not changing your activity level or quality of life in a meaningful way.
If you’re dealing with recurring back, neck, joint, or nerve pain in Oak Lawn, Orland Park, Palos Hills, Palos Heights, Worth, Bridgeview, Hickory Hills, Alsip, Burbank, Evergreen Park, or nearby Illinois communities, Midwest Pain & Wellness can help you build a smarter plan. The goal is to identify the pain source, use injections carefully when they make sense, and protect your long-term function without relying on opioids or unnecessary repeat procedures.