For targeted joint or spine injections in the Chicago area, stem cell treatment typically falls in the $3,000 to $9,000 range. That’s the honest starting point, but the cost ultimately depends on what problem is being treated, how the cells are prepared, how many areas need treatment, and whether this is a self-pay, personal injury, or workers’ compensation case in Illinois.
If you're in Oak Lawn, Orland Park, Palos Hills, Palos Heights, Worth, Bridgeview, Hickory Hills, Alsip, Burbank, or Evergreen Park, you’ve probably seen wildly different prices online and wondered whether any of them apply to your situation. That confusion is understandable. Stem cell therapy for pain is one of the most searched regenerative treatments, but many articles skip the practical questions patients ask in clinic.
People usually aren’t asking out of curiosity. They’re asking because they’ve already tried medications, therapy, injections, or surgery consults, and they want to know whether a regenerative option is realistic for their back, knee, hip, neck, or joint pain. They also want to know whether “how much stem cell?” means one procedure, a series of injections, or a treatment plan that includes other pain interventions.
The Real Cost of Stem Cell Therapy for Pain Relief

A patient from Oak Lawn or Orland Park might come in with knee arthritis, lumbar facet pain, or persistent pain after an injury and say, “I keep hearing about stem cells. What does it cost?” That’s the right question, but it only makes sense when tied to the actual pain generator.
A targeted regenerative injection for pain isn’t a generic product sitting on a shelf. It’s a procedure. The final price reflects the evaluation, harvesting when applicable, processing, imaging guidance, sterile technique, and accurate placement into the structure that’s causing pain.
Why price quotes vary so much
The biggest mistake patients make is comparing one online number to another without knowing whether they describe the same treatment. A single knee treatment is different from treating multiple joints. A focused spine procedure is different from a broad systemic infusion. A plan for degenerative joint pain is also different from a plan for post-surgical inflammation or complex injury recovery.
That’s why broad internet claims often create more confusion than clarity. A more useful starting point is the condition itself. If you’re still sorting out whether your pain is coming from the spine, joints, nerves, or surrounding soft tissue, reviewing the clinic’s pain conditions commonly evaluated and treated gives context for which diagnoses may even be appropriate for regenerative care.
Practical rule: If someone gives you a stem cell price before identifying the pain source, that quote may not be meaningful.
Why interest has grown
Regenerative medicine is no longer a fringe topic. The global stem cell therapy market is projected to grow from USD 321 million in 2026 to USD 1,290 million by 2035, a projected CAGR of 16.7%, according to Roots Analysis market projections for stem cell therapy. That growth reflects rising interest in chronic conditions such as osteoarthritis and degenerative disc disease.
Growth in interest doesn’t mean every patient is a candidate, and it doesn’t mean every clinic applies the same standards. It does mean more adults in the south and southwest suburbs of Chicago are asking whether stem cell therapy belongs in an opioid-sparing pain plan.
What patients should expect from a real conversation
A useful consultation usually answers four practical questions:
- What structure is being treated: Knee joint, lumbar facet joints, sacroiliac joint, tendon, or another pain source.
- Why regenerative treatment is being considered: Usually because the goal is to improve pain and function while avoiding repeated short-term fixes.
- How the procedure would be done: Including image guidance and whether the cells are autologous or donor-derived.
- How payment works: Self-pay is common, but personal injury and workers’ compensation need separate review.
If those pieces aren’t clear, the number alone won’t help much.
Four Key Factors That Determine Your Treatment Cost
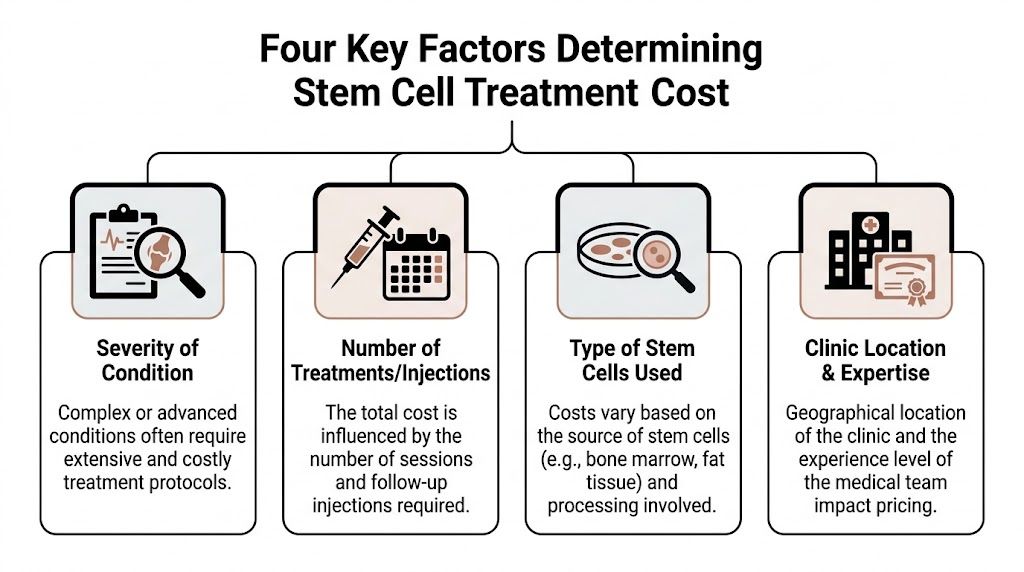
Think of stem cell pricing as a stack of building blocks. Patients often focus on the final number, but clinicians know that number is built from several decisions made before the procedure ever starts.
The source of the cells
Some pain protocols use autologous cells, meaning the material comes from your own body, often bone marrow aspirate concentrate or adipose-derived tissue. Other protocols use donor-derived or expanded cell products intended for different goals.
Autologous treatment is often easier for patients to understand because the source is personal and the procedure is localized. It can also fit better when the main target is one joint, one tendon region, or a specific part of the spine.
Allogeneic or expanded-cell approaches are different. They may be discussed more often when the goal is broader immunomodulation rather than a strictly local orthopedic target. That difference matters because the source affects handling, logistics, and price.
The processing method
Not all processing is equivalent. Some procedures rely on same-day concentration of aspirate at the point of care. Others involve more advanced expansion and manufacturing steps.
This is one reason cheap quotes deserve scrutiny. If a clinic can’t explain how the product is prepared, how viability is assessed, or what quality controls are used, the lower price may reflect a thinner protocol rather than better value.
A lower quote isn’t always a bargain. Sometimes it means the treatment is less targeted, less documented, or less carefully processed.
The treatment protocol
Quotes for treatment often vary significantly. A single, image-guided injection into one pain generator is one procedure. Treating several structures in the same patient is another. A knee with isolated osteoarthritis differs from a patient who has lumbar facet pain, sacroiliac dysfunction, and tendon involvement around the hip.
Here’s how that usually plays out in real practice:
- Single-site treatment: Often the simplest quote because there is one target and one procedural plan.
- Multi-site treatment: Cost rises when several joints or spinal levels require distinct injections.
- Hybrid plans: Some patients don’t get a regenerative procedure alone. They may need it integrated with ablation, decompression options, or other interventional care.
That last point matters. Stem cells aren’t a replacement for every established pain procedure. In many patients, they make the most sense as part of a broader plan.
Provider and facility expertise
A regenerative procedure for pain should be treated like an interventional procedure, not like a retail add-on. For back, neck, and joint pain, precision matters. Accurate diagnosis matters first, and then accurate placement matters just as much.
A specialist’s experience affects the entire episode of care:
| Cost driver | Why it matters |
|---|---|
| Diagnostic accuracy | Treating the wrong structure is expensive even if the price looks low |
| Imaging guidance | Targeted placement improves the value of the procedure |
| Sterile technique and workflow | Quality handling affects safety and consistency |
| Integration with pain management | Some patients need regenerative care plus other interventions, not one or the other |
What doesn’t work well
Patients usually get frustrated when stem cell therapy is marketed as a cure-all. That’s not how evidence-based pain management works.
These situations deserve caution:
- Vague diagnosis: “General back pain” is not enough to justify a high-cost biologic procedure.
- No imaging guidance: For spine and joint work, blind placement is hard to defend.
- One-size-fits-all protocols: Knee arthritis, disc-related pain, and tendon injury aren’t the same problem.
- Sales language instead of medical reasoning: The recommendation should start with anatomy and function, not hype.
The right question isn’t only “How much stem cell?” It’s “How much for the right treatment, in the right place, for the right diagnosis?”
Price Ranges for Stem Cell Therapy in the Chicago Area
Patients in Oak Lawn, Palos Heights, or Bridgeview usually want a usable number, not a lecture. For common orthopedic and spine applications, there are price ranges that help frame the discussion.
According to a published review on orthopedic stem cell applications and dosing, a single stem cell injection for knee osteoarthritis in the U.S. can cost $1,500 to $9,000, while lumbar or facet joint interventions range from $3,000 to $7,000. Those figures include harvesting, processing, and the image-guided injection itself.
That’s the most practical benchmark for localized pain procedures. In the Illinois suburbs around Chicago Ridge, patients often see quotes that fit within those broad ranges, but the exact figure depends on diagnosis, number of targets, and technique.
Estimated 2026 self-pay costs in Illinois
| Therapy Type | Source | Typical Price Range (per treatment) | Commonly Used For |
|---|---|---|---|
| Stem cell injection for knee osteoarthritis | Usually autologous cell-based orthopedic preparation | $1,500 to $9,000 | Knee osteoarthritis |
| Stem cell injection for lumbar or facet pain | Usually autologous cell-based orthopedic preparation | $3,000 to $7,000 | Lumbar pain, facet-related pain |
| PRP | Platelet-rich plasma from your own blood | Varies by clinic and protocol | Tendon pain, mild joint degeneration, adjunctive use |
The PRP row is intentionally qualitative here because pricing varies by clinic and no verified Illinois-specific PRP number was provided. That doesn’t make PRP less useful. It means patients should ask for a written quote tied to the exact target being treated.
What the quoted price usually includes
A proper quote for a localized stem cell procedure generally includes more than the injection itself. It often bundles:
- Procedure planning: Review of imaging, exam findings, and candidacy.
- Harvesting and processing: When using your own cells, this is part of the procedural cost.
- Image guidance: Important for spine, sacroiliac, and many joint interventions.
- Delivery into the target: The actual injection is the final step, not the whole service.
Why one patient pays more than another
A patient with one painful knee may have a fairly straightforward procedural quote. A patient from Hickory Hills with lumbar pain involving more than one structure may need a more complex plan. The same applies when pain overlaps with prior surgery, injury claims, or multiple degenerative areas.
If a quote seems unusually low, ask what’s excluded. The missing piece is often imaging guidance, harvesting, or follow-up planning.
Another practical issue is that many online ads discuss “stem cells” as if all products and protocols are interchangeable. They aren’t. Local orthopedic injections and systemic infusions serve different goals, and patients shouldn’t compare those prices as if they’re the same treatment.
Will Insurance or Workers Comp Cover Stem Cell Therapy

Many Illinois patients get blindsided. They assume the hard part is choosing whether to do the treatment. Often the harder part is figuring out who pays for it.
For pain management indications, most stem cell treatments are still handled cautiously by insurers. In practical terms, that means many plans view these procedures as investigational for orthopedic or spine pain, even when the clinical reasoning is sensible.
Why standard insurance often says no
Commercial insurance and Medicare tend to prefer established billing pathways. Procedures like epidural steroid injections, radiofrequency ablation, medial branch blocks, and certain decompression procedures have clearer coverage structures. Regenerative treatments for pain usually do not.
That doesn’t mean a treatment lacks logic or that it can’t help the right patient. It means coverage rules haven’t kept up with patient interest. When patients hear “not covered,” they often assume “not legitimate.” Those are not the same thing.
Workers’ compensation in Illinois is different
The more nuanced conversation happens in Illinois workers’ compensation and some personal injury cases. A verified summary of the current gap in online information notes that stem cell treatment is often classified as experimental, yet Illinois workers’ comp may approve it on a case-by-case basis when it is part of a multimodal treatment plan, with approval rates for interventional pain described as as low as 20 to 30% in the cited discussion from Start Stem Cells on stem cell therapy cost and workers’ comp questions.
That’s not a promise of coverage. It is a reminder that the answer is not always a flat no.
Here’s what usually strengthens the case:
- Clear diagnosis: The file should identify the pain generator, not just list chronic pain.
- Prior conservative care: Documentation matters when showing why another option is being considered.
- Multimodal planning: Requests are stronger when the regenerative procedure is part of an organized pain strategy rather than a standalone elective add-on.
- Functional goals: It helps when the request ties treatment to return of mobility, tolerance for work activity, or better day-to-day function.
The strongest workers’ comp requests read like medical plans, not wish lists.
Personal injury and lien-based cases
Some patients from Alsip, Burbank, or Evergreen Park are not dealing with workers’ comp at all. They may be in a personal injury case, or they may be delaying a decision while legal and medical documentation develops.
In those settings, the practical questions include whether the treatment is being considered now, whether a less costly step is more appropriate first, and whether the medical record supports why a regenerative option belongs in the plan at all. That’s why records, imaging, prior procedure response, and exam findings matter so much.
What patients should ask the office
Before assuming you must self-pay, ask direct questions:
- Will you submit documentation for review if this is workers’ comp?
- Is the treatment being recommended alone, or as part of a broader pain plan?
- What chart notes and imaging support medical necessity?
- If coverage is denied, what self-pay costs would apply?
Insurance conversations can feel frustrating, but clarity early on saves time and disappointment.
PRP vs Stem Cells Understanding Your Options
Patients often use these terms as if they mean the same thing. They don’t. Both fall under regenerative medicine, but they do different jobs and fit different clinical situations.
A simple way to think about it is this. PRP is more like delivering a concentrated set of signaling materials from your own blood. Stem cell-based orthopedic treatment is more like delivering a biologic cellular product intended for a broader reparative and anti-inflammatory effect in a selected target.
What PRP usually fits best
PRP is often discussed when the goal is to help tendon problems, mild joint degeneration, or soft tissue irritation where a lower-complexity biologic option may make sense. It can also be considered when a patient wants to start with a less involved regenerative approach before moving to a more advanced procedure.
PRP tends to be easier for patients to understand because the blood draw, processing, and reinjection are conceptually straightforward. It’s still a procedure, and it still needs appropriate diagnosis and placement.
When stem cell-based treatment enters the conversation
Stem cell-based treatment comes up more often when a patient has more substantial degenerative change, a joint problem that hasn’t responded to simpler measures, or a spinal or orthopedic issue where the treating physician believes a cell-based option may be more appropriate than PRP alone.
Treatment goals change the protocol. A discussion of stem cell therapy protocols for arthritis and systemic inflammation notes that local site injections often use 50 to 200 million cells, while some IV protocols for systemic inflammation can use over 300 million cells. That distinction matters because a targeted pain procedure is not the same as a systemic infusion.
Why a pain specialist may choose one over the other
The decision usually comes down to anatomy, severity, and treatment goals. A patient can review the broader range of interventional procedures used in comprehensive pain treatment and see that regenerative care is only one part of the toolbox.
A clinician may lean toward PRP when:
- The pathology is more tendon-dominant
- The problem is earlier-stage degeneration
- A less complex autologous option is preferred first
A clinician may discuss stem cell-based treatment when:
- The target is a more significant joint or spinal pain generator
- The goal is a stronger localized biologic approach
- Prior treatment has not produced durable relief
The best regenerative option is the one that matches the diagnosis. The most expensive option is not automatically the best option.
What doesn’t help patients
What causes confusion is marketing that treats every regenerative product as interchangeable. It also doesn’t help when clinics push IV therapy for a problem that is clearly local, such as one knee or one facet region. For pain medicine, the matching of treatment to structure is what matters most.
Questions to Ask Your Doctor Before Choosing Therapy

A good consultation should leave you with more clarity, not more confusion. If you’re comparing options in Palos Hills, Worth, or Evergreen Park, the smartest move is to bring specific questions and write down the answers.
One of the most important quality checks is whether the clinic can explain dose and viability in a meaningful way. In orthopedic applications, optimal results depend heavily on the number of viable cells injected, typically targeting 1 to 5 million mesenchymal stem cells per kilogram of body weight, as described in the earlier-cited orthopedic literature. For patients, that translates into a simple rule: ask how the provider measures cell count and viability rather than accepting vague language about “high quality” cells.
Questions that protect you
Use these in any consultation:
- What exactly are you treating? Ask the doctor to name the structure, not just the symptom.
- What type of biologic are you recommending? PRP, bone marrow aspirate concentrate, adipose-derived product, or another protocol should be clearly explained.
- How do you place the treatment? For spine and joint pain, ask whether image guidance is used.
- How do you assess cell quality? A provider should be able to discuss counting, viability, and handling in practical terms.
- What is the backup plan if this doesn’t help enough? The answer should include next steps, not a shrug.
Questions about expectations
Many disappointments come from unrealistic expectations rather than bad intent. Ask these early:
| Question | Why it matters |
|---|---|
| What level of improvement is realistic for my condition? | Helps separate hope from hype |
| How long should I wait before judging the result? | Regenerative treatments are not instant numbing procedures |
| What rehab or activity changes matter afterward? | Recovery and loading often affect outcome |
| Would another interventional option fit me better? | Sometimes ablation, decompression, or targeted injection is the better choice |
Ask your doctor to explain why this procedure fits your anatomy better than PRP, steroid injection, ablation, or watchful waiting.
Red flags worth noticing
If a clinic can’t answer basic technical questions, be careful. That includes not identifying the pain source, not discussing imaging guidance, or avoiding direct answers about candidacy.
A reputable pain practice should also be comfortable telling you when stem cell therapy is not the best next step. Sometimes the right move is a different intervention, further imaging review, or a less costly treatment first.
Get a Personalized Treatment Plan at Midwest Pain & Wellness
The right answer to “How much stem cell?” is never just a number. In Illinois pain care, the cost depends on the diagnosis, the treatment target, the biologic being used, the complexity of the procedure, and whether there’s any pathway for workers’ compensation or case-based review.
That’s why a real evaluation matters. A patient from Orland Park may need a focused knee plan. A patient from Oak Lawn may have spine-generated pain that fits a different interventional approach. Another patient from Palos Heights or Bridgeview may be better served by PRP, radiofrequency ablation, MILD, Vertiflex, or another opioid-sparing option instead of stem cell treatment.
Midwest Pain & Wellness approaches this the way pain medicine should work. First, the team identifies the pain generator. Then they recommend the least wasteful, most medically sensible option. If regenerative treatment belongs in the plan, they explain why, where it fits, and what the financial side looks like.
Scheduling is straightforward through the clinic’s appointment request page for Midwest Pain & Wellness. Patients from Oak Lawn, Palos Hills, Palos Heights, Worth, Bridgeview, Hickory Hills, Alsip, Burbank, Evergreen Park, and Orland Park can request an evaluation and get a plan based on their actual condition, not a generic online quote.
If you’ve been searching “How much stem cell?” because you’re tired of temporary relief, the next step isn’t guessing. It’s getting the right diagnosis and a treatment recommendation you can weigh against your goals, your budget, and your recovery timeline.
If you’re ready to discuss regenerative medicine, interventional pain treatment, or a workers’ compensation or personal injury pain plan, schedule a consultation with Midwest Pain & Wellness.