Pain rarely arrives at a convenient time. It shows up when you’re carrying groceries in Oak Lawn, bending into the trunk after a stop in Palos Hills, trying to get through a workday in Evergreen Park, or walking across a parking lot in Orland Park and realizing your back, knee, shoulder, or neck is now controlling the schedule.
When patients ask me, “How steroid injection works?”, they usually aren’t asking for a chemistry lecture. They want to know whether the injection will help, how fast it may help, what the trade-offs are, and whether it’s a smart next step or just a temporary patch. Those are the right questions.
A steroid injection can be very useful. It can also be misunderstood. It doesn’t rebuild damaged tissue. It doesn’t erase arthritis. It doesn’t cure every source of pain. What it can do, in the right patient and in the right location, is reduce inflammation enough to calm pain and create a window for better movement, sleep, rehab, and function. That’s why I use it as one tool inside a broader pain management plan, not as a magic fix.
Living with Pain in the Chicago Suburbs
A common story sounds like this. Someone in Palos Heights wakes up stiff, tries to “walk it off,” and finds that the pain settles in deeper by noon. A resident in Bridgeview can still get through errands, but every step on a painful knee changes how they move. Someone in Hickory Hills sits through a commute, stands up, and feels a sharp pull down the leg.
That kind of pain changes behavior quickly. People stop exercising. They avoid stairs. They sleep poorly. They start taking more over-the-counter medication than they want to. In many cases, they aren’t just dealing with pain. They’re dealing with swelling, nerve irritation, joint inflammation, muscle guarding, and loss of confidence in their own body.
When relief matters, but so does the diagnosis
Steroid injections became popular because they can reduce inflammation in a targeted area without relying only on oral medication. For some patients, that matters a great deal. A calmer nerve root, less irritated joint lining, or less inflamed bursa can make daily life much more manageable.
But the main question isn’t whether steroid injections exist. It’s whether they fit your pain pattern. Shoulder pain, knee arthritis, sciatica, sacroiliac pain, and facet-related back pain don’t all respond the same way. Before talking about injections, I want to know what structure is causing the pain, what treatments you’ve already tried, and what functional goal matters most to you.
Patients who are sorting through back, neck, joint, or nerve symptoms often start by reviewing the range of conditions we treat so the pain pattern has some clinical context.
Pain relief is useful. Pain relief with a clear diagnosis is much more useful.
The misunderstanding I see most often
Many people hear “steroid shot” and think of a simple anti-inflammatory booster. That’s incomplete. The medication works through a specific biologic process, and the location of the injection matters just as much as the drug itself.
It also matters what the injection is supposed to accomplish. Sometimes the goal is to settle a spinal nerve enough for the patient to tolerate movement again. Sometimes it’s to reduce inflammation in a joint that has become too painful for normal activity. Sometimes it’s part of a diagnostic process that helps confirm the pain generator.
That’s why a thoughtful plan matters more than a rushed procedure. In Chicago Ridge and the surrounding Illinois communities of Worth, Alsip, Burbank, and beyond, patients deserve a straight answer about both the benefits and the limits.
The Science of Relief How Steroids Calm Inflammation
A patient may come in hoping the shot will “fix” the problem. What I explain is more precise. The injection is meant to quiet an overactive inflammatory response in a specific location so pain drops enough for the body to move, sleep, and function better.
When tissue stays irritated, the body keeps releasing inflammatory chemicals. Those signals increase swelling, sensitize nearby nerves, and make normal movement hurt more than it should. In the right setting, a corticosteroid can interrupt that cycle.
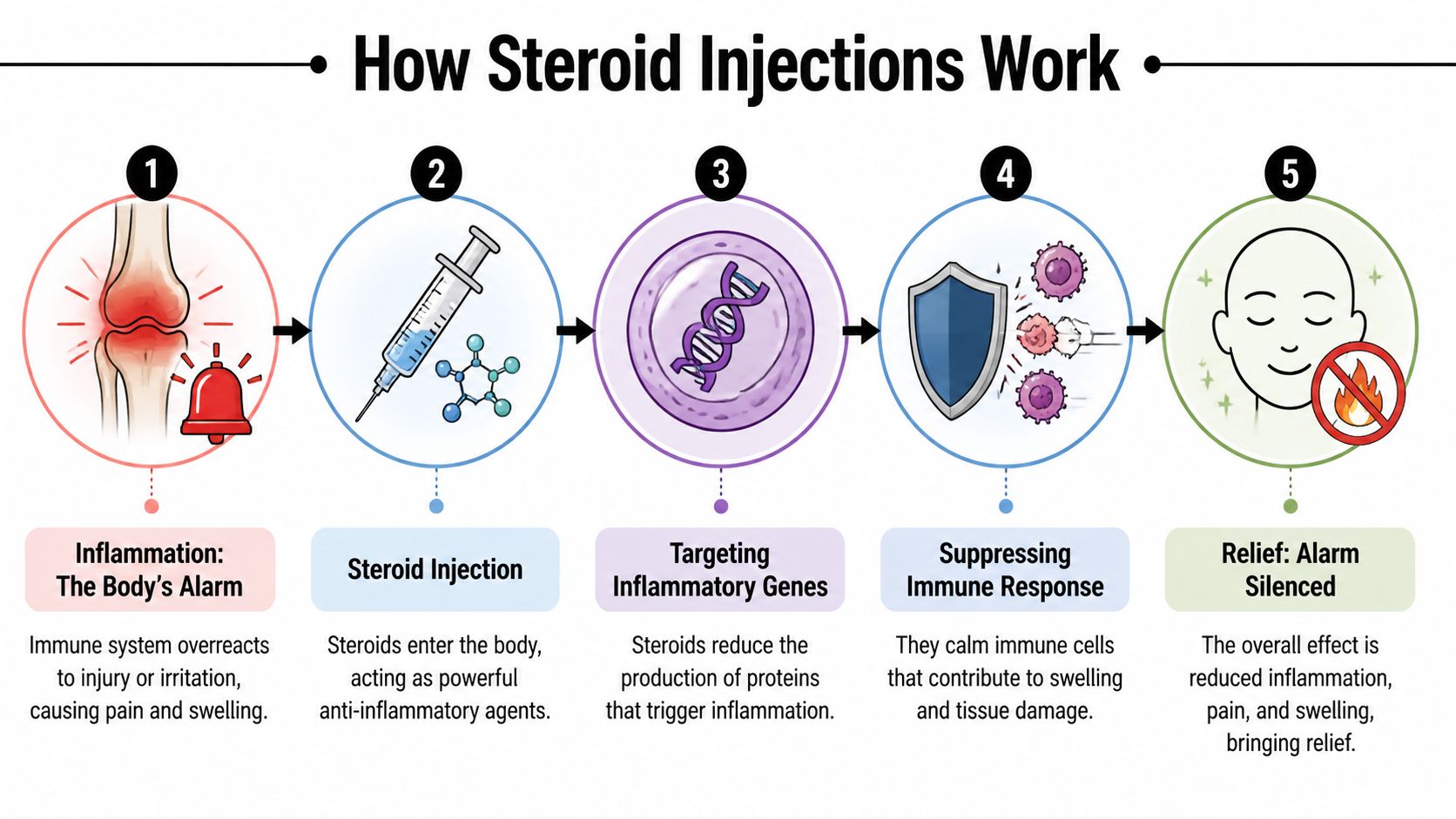
What happens after the medication reaches the tissue
At the cellular level, the steroid enters cells and binds to glucocorticoid receptors in the cytoplasm. That complex then moves into the nucleus and changes gene expression, which lowers production of inflammatory mediators. It also reduces prostaglandin activity and alters parts of the immune response, helping calm the cascade described in this review of corticosteroid mechanisms.
For patients, the practical meaning is simpler. The medication does not just “numb pain.” It changes the local chemistry that is keeping the tissue inflamed and the nerves irritated.
Formulation matters too. Some steroids are more soluble and tend to act sooner, while others are less soluble and remain in the tissue longer. That difference affects onset, duration, and where I may or may not want to use a particular product. In pain medicine, technique and drug selection go together. Patients comparing image-guided pain procedures and injection options are often surprised by how much those details matter.
Why the shot doesn’t always work instantly
Many injections include a local anesthetic along with the steroid. The anesthetic can give early relief because it temporarily blocks pain signals. The steroid works on a different timetable.
A patient often feels the response in phases:
- Early phase: The numbing medicine may reduce pain first.
- Interim phase: The anesthetic wears off, and symptoms can return for a short time.
- Anti-inflammatory phase: The steroid gradually reduces local inflammation over the next several days.
The same review notes that more soluble steroids may begin helping within hours, while less soluble preparations can take longer to show their full effect. That is one reason I ask patients not to judge the result too quickly after the procedure.
Why repeated injections may help less over time
This is one of the most important trade-offs to understand. A steroid injection can be very helpful, but repeated exposure in the same area may produce reduced efficacy over time. Later injections may have a less pronounced therapeutic effect, and some tissues may tolerate repeated steroid exposure poorly.
That matters most in joints and soft tissues already dealing with degeneration. Steroids can lower inflammation, but they do not rebuild cartilage, repair a tendon, or reverse wear in the spine. In some settings, repeated injections may also affect local cell health and tissue quality. That is why I do not recommend automatic repeat injections on a fixed schedule without reassessing the diagnosis, the response, and the function gained from the last treatment.
Clinical reality: A steroid injection is a biologically active treatment with a specific purpose, not just medicine placed near pain.
What the steroid is really doing
The best way to think about benefit is functional. If the injection reduces pain enough for someone to walk with less limitation, sleep through the night, participate in physical therapy, or avoid escalating opioid use, it has done useful work. If it gives no relief, that information is useful too, because it may tell us the suspected pain generator was not the main problem.
Used this way, steroid injections are a tool. They can create a window for movement, rehabilitation, and better day-to-day function. They are rarely the whole plan, and they should not be presented that way.
Targeting Pain Precisely Four Main Types of Injections
Where the medication goes matters. A steroid placed into a knee joint is being asked to do a different job than a steroid placed around an irritated spinal nerve. Good pain medicine starts with matching the procedure to the anatomy.
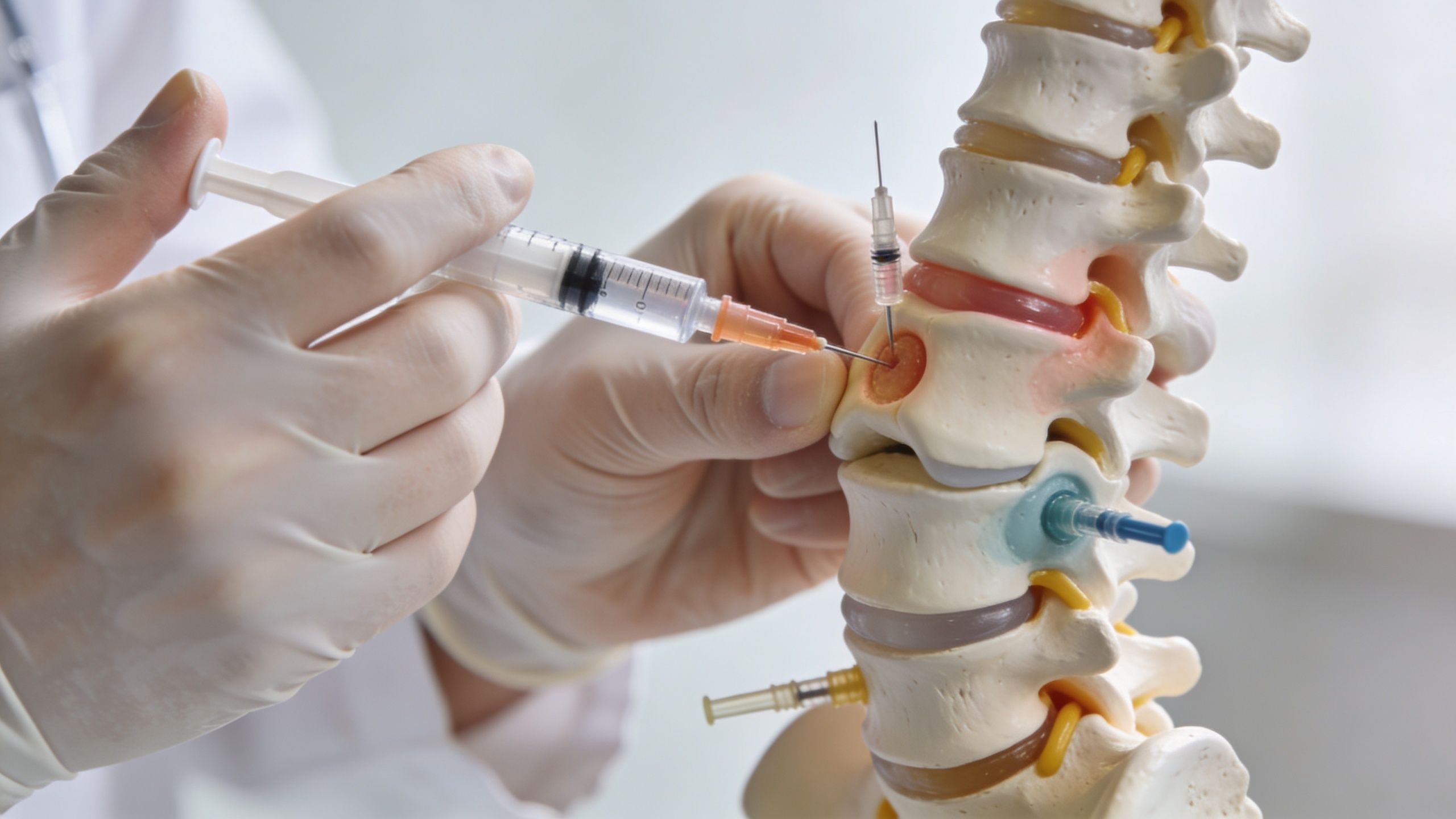
Patients exploring image-guided options often compare the procedures we use for treatment with their own symptoms before a consultation.
Intra-articular joint injections
These injections place medication directly into a joint space. Typical targets include the knee, shoulder, or hip when arthritis or synovial inflammation is contributing to pain.
A patient with joint pain usually describes stiffness, swelling, pain with weight-bearing or overhead motion, and a sense that the joint itself is the problem. In that setting, placing medication into the joint can reduce inflammation in the lining of the joint and improve motion for a period of time.
This can be helpful when the goal is to get someone moving again, especially if pain has caused them to stop walking, stop exercising, or avoid normal use of the limb.
Epidural steroid injections
These are different. An epidural steroid injection targets inflammation around spinal nerves, often when pain radiates down an arm or leg. That pain pattern is commonly associated with a disc herniation, bony spur, or inflamed nerve root.
For epidural steroid injections, the corticosteroid is often combined with a local anesthetic such as lidocaine or bupivacaine. The anesthetic can provide immediate nerve-blocking relief, while the steroid addresses inflammation over several days. A known clinical issue is the post-injection flare, where pain may briefly worsen for 1 to 2 days before the steroid reaches fuller effect, as described in this patient-facing review of steroid injections.
A quick comparison helps:
| Injection type | Main target | Typical symptom pattern | Main purpose |
|---|---|---|---|
| Intra-articular | Joint space | Joint pain, swelling, stiffness | Reduce local joint inflammation |
| Epidural | Epidural space around spinal nerves | Arm or leg pain, sciatica, radicular symptoms | Calm inflamed nerve roots |
Medial branch blocks
Medial branch blocks are often used when the source appears to be the facet joints in the spine. These joints can produce pain in the neck or low back, especially with standing, twisting, arching, or certain positional changes.
Precision matters at this stage. The procedure targets the small nerves that carry pain signals from the facet joints. Sometimes a medial branch block is mainly diagnostic. If it helps in a pattern that matches the exam, it can support the next step in treatment planning.
That’s very different from taking a “general back pain” approach. Not all back pain comes from discs. Not all spine pain needs the same injection.
Trigger point injections
Trigger point injections are aimed at painful muscle knots and bands of tight tissue. These patients often describe aching, pulling, or pressure that feels muscular rather than deep inside a joint or down a nerve path.
In some cases, the dominant problem isn’t joint inflammation at all. It’s secondary muscle spasm that developed because the body has been guarding an injured or painful area for too long. A targeted muscle injection can interrupt that cycle and make movement easier.
The right injection is the one that matches the pain generator, not the one that happens to be available first.
Your Injection Procedure What to Expect at Our Clinic
Most patients are less worried about the medication than they are about the process. They want to know whether the procedure is precise, whether it will be rushed, and whether someone is confirming the target before placing a needle.
That concern is reasonable. Accuracy matters.

Before the procedure
The visit starts with reviewing symptoms, imaging when relevant, prior treatment response, medications, and the goal of the injection. I want to know whether the aim is diagnostic clarification, short-term symptom control, improved participation in rehab, or relief during a specific period of recovery.
Not every patient should get a steroid injection. If the pain pattern doesn’t fit, if the risk is too high, or if another treatment makes more sense, I say that directly.
Patients who are ready for an evaluation can request one through the clinic’s appointment page.
During the injection
The procedure area is set up for sterility, safety, and efficient workflow. The skin is cleaned carefully. The patient is positioned to give the safest and most accurate access to the target. Imaging guidance such as fluoroscopy or ultrasound is used when appropriate so the medication reaches the intended structure.
From the patient’s perspective, the injection itself is usually much shorter than the anticipation leading up to it. Some feel pressure. Some feel a brief reproduction of their typical pain. Many are surprised that the procedure is more tolerable than they expected.
What matters to me is not speed alone. It’s needle placement accuracy, confirmation of the target, and minimizing unnecessary tissue irritation.
Why image guidance matters
Blind injections rely too much on estimation. In pain medicine, a few millimeters can matter. If the goal is to calm a specific joint recess, epidural space, bursa, or nerve-related structure, accurate placement improves the odds that the medicine is treating the actual source.
That’s especially important in the spine. If the symptom is leg pain from a nerve root, the procedure should be built around that anatomy. A vague injection into the general area doesn’t meet the standard I expect.
After the procedure suite
Before the patient leaves, we review what may happen that day and over the next several days. If a local anesthetic was used, early relief can fade. If soreness develops, that doesn’t automatically mean the procedure failed. Expectations have to be realistic from the start.
A few practical points are usually reviewed before discharge:
- Activity: Take it easy the rest of the day unless you’re told otherwise.
- Symptom tracking: Notice whether the pain changes, where it changes, and when.
- Safety: Contact the clinic if symptoms seem out of proportion or concerning.
- Follow-up: The next step depends on the response, not on habit.
That last point is important. Injections shouldn’t happen on autopilot.
Understanding Your Recovery After the Injection
Recovery after a steroid injection is often uneven at first. That’s normal, and it helps to know the pattern before you experience it.
If your injection included a local anesthetic, you may feel early relief. Some patients walk out feeling much better. That can be encouraging, but it isn’t always the long-term result. As the numbing medicine wears off, symptoms can return before the steroid has fully done its work.
The first few days
This is the period when people get confused if no one prepared them properly. It’s possible to have soreness at the injection site. It’s also possible, particularly with certain spine injections, to feel a temporary flare before improvement begins.
That early fluctuation doesn’t mean the treatment failed. The anti-inflammatory effect often takes time to build.
Don’t judge the final result by the first several hours.
When the steroid starts helping
The timeline depends on the formulation used and the tissue being treated. Some preparations act faster. Others take longer to settle in. In general, patients should think in terms of days, not minutes, when they’re waiting for the steroid itself to work.
I usually want patients paying attention to function, not just raw pain intensity. Can you stand longer? Walk more comfortably? Sleep with fewer interruptions? Move the shoulder with less guarding? Those are meaningful signs that inflammation is settling.
What to do after the procedure
The best recovery plan is simple and deliberate.
- Protect the area early: Give the irritated tissue a short period of relative calm.
- Resume movement thoughtfully: Gentle activity is usually better than complete shutdown unless you’ve been told otherwise.
- Use the relief window well: If pain eases, that’s the time to work on better mechanics, conditioning, and movement patterns.
- Report unusual symptoms: Severe or unexpected changes deserve a direct call, not guesswork.
What not to expect
A steroid injection doesn’t erase every source of pain at once. If the underlying problem includes arthritis, instability, stenosis, tendon damage, or longstanding nerve sensitivity, the result may be partial rather than complete.
That’s still valuable when it changes function. A patient doesn’t need a miracle to benefit. They need enough improvement to move forward with the next part of care.
Weighing the Real Benefits Against the Long-Term Risks
Steroid injections earn their place in pain care because they can reduce inflammation fast enough to change what a patient is able to do. For the right diagnosis, that can mean less pain with walking, easier sleep, better participation in physical therapy, and less reliance on opioids or repeated oral medication.
That benefit matters. So does the cost of using these medications too casually.

The benefits that make injections worth considering
A targeted injection can reach tissue that pills treat only indirectly. In a swollen arthritic joint, that may lower inflammation enough to restore useful range of motion. Around an irritated spinal nerve, it may reduce chemical inflammation enough to improve sitting tolerance, standing time, or leg pain.
I tell patients to judge success by function. If an injection lets someone return to therapy, tolerate a workday, or stop waking up every two hours from pain, that is a meaningful medical outcome even if the pain is not gone.
The formulation also matters. Some steroid preparations are more soluble and act sooner. Others remain in the tissue longer and may provide a different duration profile. That does not make one product universally better. It means the medication choice should match the target, the diagnosis, and the reason for doing the injection in the first place.
The long-term concern patients should understand
Steroids can calm inflammation, but repeated exposure is not biologically neutral. The concern is highest when injections are used again and again in weight-bearing joints without a clear plan for what comes next.
A randomized clinical trial involving 140 patients with knee osteoarthritis, summarized in this review of steroid injection risks, found greater cartilage volume loss in the steroid group with no pain benefit over saline. That does not mean every injection damages every joint. It does mean frequency, location, and diagnosis matter.
There is also a dose issue. Natural steroid signaling in the body occurs at very low levels. Injected doses are much higher, and cartilage cells may not tolerate repeated exposure well. That is one reason experienced pain physicians limit how often steroids are repeated and avoid using them as an automatic refill for chronic joint pain.
Local and whole-body trade-offs
The risk discussion should go beyond cartilage. Repeated steroid exposure can affect more than the target site. Temporary hyperglycemia, transient osteopenia, local fat atrophy, and reversible cortisol suppression are among the effects described in this Cleveland Clinic overview of cortisone shot considerations.
For a patient with diabetes, that may change glucose management for several days. For a patient with bone fragility, frequent steroid use deserves more caution. For a patient with an upcoming surgery or active infection concern, timing matters.
This is why I do not present a steroid injection as a simple yes-or-no decision. It is a trade-off decision.
How risk is reduced in practice
Good injection planning starts with accuracy. The painful structure has to match the history, exam, and imaging well enough that the target makes clinical sense.
Then comes restraint.
- Use steroids for the right pain pattern: Inflammatory pain tends to respond better than pain driven mainly by mechanical instability, advanced structural failure, or longstanding central sensitization.
- Choose the formulation thoughtfully: Particulate and nonparticulate steroids do not behave the same way, and the selection depends on the tissue being treated and the safety priorities of that procedure.
- Limit repetition: A second or third injection should have a defined purpose, such as helping a patient progress in rehabilitation or get through a specific pain flare.
- Watch the full medical picture: Diabetes, bone health, infection risk, upcoming procedures, and prior response all affect whether another injection makes sense.
- Use the relief window strategically: The goal is to pair symptom improvement with rehab, movement correction, and reassessment, not to chase short-term relief indefinitely.
Patients deserve honesty here. A steroid injection can be very helpful, especially when inflammation is blocking progress. It can also become counterproductive if it is repeated without regard for tissue health over time.
The best decision balances both.
A Smarter Strategy for Pain Relief in Illinois
The best way to think about steroid injections is this. They are strategic tools, not cures. They can calm inflammation, reduce pain, and create a useful period of improved function. What they do next depends on how intelligently that period is used.
For some patients in Chicago Ridge, Oak Lawn, Palos Hills, Palos Heights, Worth, Bridgeview, Hickory Hills, Alsip, Burbank, Evergreen Park, and Orland Park, the right move is a precisely targeted injection followed by active rehabilitation and reassessment. For others, the right answer may be a different interventional procedure, medication adjustment, regenerative option, or coordination with a surgeon or primary care physician.
What a smarter plan looks like
A stronger pain plan usually includes several parts working together:
- Accurate diagnosis: The treatment has to match the anatomy.
- Image-guided precision: The medication should reach the intended target.
- Opioid-sparing thinking: Use focused interventions to reduce reliance on chronic pain medication when possible.
- Functional goals: Relief should translate into walking, sleeping, bending, working, or recovering better.
- Reassessment: The response to treatment should guide the next decision.
Specialist training is essential. A double board-certified interventional pain specialist isn’t just deciding whether a patient can receive a shot. Their primary task involves deciding whether the injection fits the pathology, whether the expected benefit justifies the risk, and what comes after it.
The question I want patients asking
The most useful question isn’t just, “Will this injection stop my pain?” It’s, “What problem is this injection treating, what benefit should I expect, and what’s the plan if it helps only partly or for a limited time?”
That question leads to better care. It pushes the conversation past quick fixes and toward strategy.
Midwest Pain & Wellness is one Illinois option for patients who need image-guided interventional pain care within a broader, opioid-sparing treatment plan led by Dr. Yaw Donkoh.
If you’ve been wondering how steroid injection works, the short answer is this: it changes inflammatory signaling in a targeted location. The more useful answer is that it works best when the diagnosis is correct, the placement is precise, the risks are respected, and the injection serves a larger recovery plan.
If you live in Chicago Ridge or nearby communities such as Oak Lawn, Palos Hills, Palos Heights, Worth, Bridgeview, Hickory Hills, Alsip, Burbank, Evergreen Park, or Orland Park, and you want a personalized evaluation for back, neck, joint, or nerve pain, schedule a consultation with Midwest Pain & Wellness. The goal is straightforward: identify the underlying pain source, determine whether a steroid injection is appropriate, and build a treatment plan that supports durable relief without unnecessary opioid dependence.



