Understanding a Common Cause of Chronic Back Pain
Degenerative disc disease is one of the most common causes of chronic low back and neck pain. Despite its name, it’s not a disease but a natural part of aging where the cushioning discs between your vertebrae gradually wear down.
Quick Overview: What You Need to Know
- What it is: A condition where spinal discs lose water, height, and flexibility due to aging.
- Who it affects: Nearly everyone shows some disc degeneration by age 60, but only about 5% develop painful symptoms.
- Common symptoms: Low back or neck pain (worse with sitting, bending, or twisting), radiating pain, numbness, or tingling.
- Key fact: Pain doesn’t always worsen; many people improve as the spine restabilizes over time.
- Treatment approach: Most cases respond well to non-surgical options like physical therapy and interventional pain management.
Your spinal discs are shock absorbers between your vertebrae. Think of them as jelly-filled cushions with a tough outer layer and a soft, gel-like center. Young discs are about 80% water, but with age, they naturally dry out, lose height, and become less flexible.
The term “degenerative disc disease” is a misnomer. While the discs do degenerate (break down), this is a normal aging process, not a disease. Importantly, disc degeneration doesn’t always cause pain. Many people have degenerated discs on an MRI scan but experience no symptoms.
For those who do develop chronic pain, effective treatments exist. Modern pain management focuses on reducing inflammation, strengthening supporting muscles, and restoring function—often without surgery.
What Causes Degenerative Disc Disease and What Are the Symptoms?
Your spine is a stack of bones (vertebrae) with soft cushions—your intervertebral discs—between them. These discs allow you to bend, twist, and absorb shock.
Each disc has two parts: a tough, fibrous outer layer called the annulus fibrosus, which contains nerve endings, and a soft, gel-like center called the nucleus pulposus, which provides cushioning.
What Causes Discs to Degenerate?
The main cause of degenerative disc disease is aging. Several specific changes happen to your discs over time.
Disc dehydration is the biggest factor. The gel-like center loses water, causing the disc to lose height and flexibility. This reduces cushioning and puts more stress on the spine.
Daily wear and tear creates tiny tears in the outer ring, which can spark inflammation and pain. Sometimes, inflammatory proteins from the inner gel leak out and irritate nearby nerves.
Injuries, whether a single bad fall or smaller, repetitive stresses from poor posture, can accelerate disc breakdown.
Risk Factors for Degenerative Disc Disease
While everyone’s discs age, certain factors increase the likelihood of painful symptoms.
- Genetics plays a surprisingly large role. Some people are predisposed to earlier or more severe disc problems. Scientists are working on identifying novel genetic markers for the risk of spinal pathologies to help predict and prevent these issues.
- Obesity puts extra strain on your spine, accelerating wear and tear.
- Smoking is particularly harmful. It reduces blood flow to your discs, cutting off nutrients needed for repair. Smokers often experience worse pain.
- A physically demanding job involving repetitive heavy lifting, twisting, or vibration increases stress on discs.
- Being female may also increase risk, possibly due to hormonal factors affecting disc integrity.
Common Symptoms of Degenerative Disc Disease
Disc degeneration doesn’t always hurt. Many people have it and feel nothing. But when symptoms do appear, they can range from mild to disruptive.
Most pain occurs in the low back (lumbar spine), as this area carries the most weight. About 90% of disc problems from degenerative disc disease happen here. Pain can also appear in the neck (cervical spine).
The pain itself varies, from a dull ache to sharp sensations. It often worsens when you sit, as sitting puts about three times more pressure on lower back discs than standing. Bending, lifting, or twisting also makes it worse. Many people find relief from walking, changing positions, or lying down.
The pain is often intermittent, with flare-ups lasting days or months, followed by periods of calm.
When a disc presses on a nerve, you might feel radiating pain. In the lower back, this can cause sciatica—pain shooting down your buttock and leg. In the neck, pain can travel down your arms and into your hands.
Numbness, tingling, and muscle weakness in the arms, hands, legs, or feet are other signs of nerve involvement.
Foot drop—difficulty lifting the front of your foot—is a more serious symptom that signals significant nerve damage and requires prompt medical evaluation.
These symptoms can be worrying, but effective treatments exist. For more information about related spinal conditions we address, visit our page on conditions we treat.
Diagnosis, Stages, and Related Conditions
Diagnosing degenerative disc disease at Midwest Pain and Wellness involves a comprehensive evaluation to understand your complete story.
We start with your medical history, asking when the pain began, what activities trigger it, and if the pain travels. We’ll also discuss past injuries, lifestyle, and family history. Next, a physical examination assesses your range of motion, reflexes, muscle strength, and sensation to find clues about which nerves might be affected.
To see inside your spine, we use imaging tests:
- X-rays show the bones, revealing narrowed disc spaces or bone spurs.
- MRI (Magnetic Resonance Imaging) is our most valuable tool. It creates detailed pictures of discs and nerves, showing dehydration, bulges, herniations, and nerve compression.
- A CT scan provides excellent detail of bone structures.
- Electromyography (EMG) or nerve conduction studies may be used to measure nerve and muscle function if significant damage is suspected.
Degenerative Disc Disease vs. Arthritis of the Spine
Patients often ask, “Is this degenerative disc disease or arthritis?” The two are closely related and often appear together.
| Feature | Degenerative Disc Disease | Arthritis of the Spine (Osteoarthritis) |
|---|---|---|
| Primary Focus | Wear and tear of the intervertebral discs | Wear and tear of cartilage in the facet joints (small joints connecting vertebrae) |
| Key Changes | Disc dehydration, loss of height, tears in annulus, disc bulges/herniations | Cartilage breakdown, bone spur formation, inflammation in facet joints |
| Consequences | Reduced disc cushioning, nerve compression by disc material | Joint stiffness, pain, nerve compression by bone spurs |
| Relationship to Aging | Natural part of aging; discs dry out and collapse | Natural part of aging; cartilage wears thin |
| Overlap | Often co-exist; disc degeneration can lead to increased stress on facet joints, accelerating arthritis | Arthritis can destabilize the spine, further impacting disc health |
These conditions feed off each other. As discs lose height, it puts more pressure on the facet joints, leading to arthritis. Bone spurs from arthritis can then narrow the space for nerves. Degenerative disc disease is a form of spinal arthritis; they are two parts of the same aging process.
Disc degeneration can also set the stage for several related conditions:
- Spinal stenosis occurs when the spinal canal narrows from bulging discs or bone spurs, squeezing nerves. Learn more about Spinal Stenosis & Degenerative Spine Disease.
- A herniated disc develops when the disc’s outer layer tears, allowing the inner gel to press on a nerve.
- Spondylolisthesis is when one vertebra slips forward over another due to instability.
- Radiculopathy is the medical term for radiating pain, numbness, and weakness from a pinched nerve.
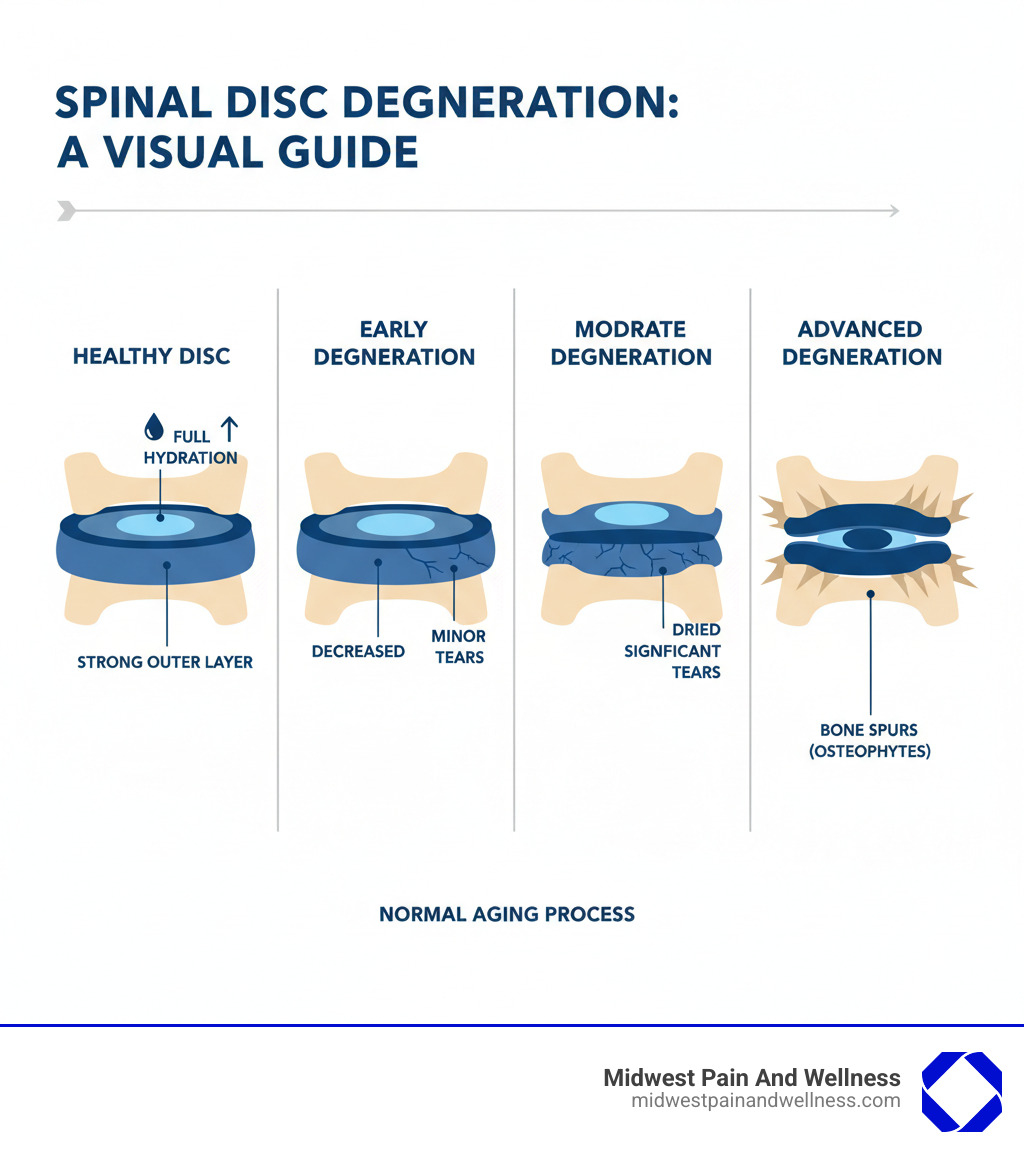
The Four Stages of Degeneration
Disc degeneration typically progresses through stages over many years, though not everyone experiences all four.
- Stage 1: Dysfunction: Microscopic tears appear in the disc’s outer layer, causing occasional pain.
- Stage 2: Dehydration: The disc’s core loses water and height, leading to more persistent pain. The disc appears dark on an MRI.
- Stage 3: Stabilization: The body forms bone spurs to stabilize the segment. This can reduce painful motion but may also pinch nerves.
- Stage 4: Collapse: The disc has significantly shrunk or collapsed. Nerve compression is common, though pain may decrease as the segment essentially fuses itself.
Understanding your stage helps us create a targeted treatment plan. An advanced stage doesn’t automatically mean surgery or a lifetime of pain.
A Modern Approach to Treatment and Pain Management
If you’re dealing with pain from degenerative disc disease, relief is within reach. At Midwest Pain and Wellness, we start with the most conservative approaches, aiming for comprehensive, opioid-free pain management that gets you back to your life.
Conservative Treatments First
Most people find significant relief without surgery. We begin with conservative treatments that work with your body to reduce pain and improve function.
- Physical therapy is the foundation of treatment. A therapist guides you through exercises to strengthen core muscles, improve flexibility, and learn proper posture. This builds long-term spine protection.
- Medications play a supporting role. Over-the-counter nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen reduce inflammation, while acetaminophen helps with pain. For severe flare-ups, a short course of oral corticosteroids may be prescribed.
- Heat and cold therapy can manage daily discomfort. Try alternating ice packs and heating pads on the area for 10-15 minutes at a time. Ice reduces inflammation, while heat soothes soreness.
- Holistic therapies like acupuncture, yoga, and meditation can be part of a personalized care plan. Our doctors stay current with research, such as this Review of the Current Diagnostic and Treatment Strategies. See our full range of procedures we use for treatment.
Advanced Treatments for Degenerative Disc Disease
When conservative treatments aren’t enough, our expertise in interventional pain management provides more options. We use a multi-modal approach for long-term, opioid-free relief.
- Epidural steroid injections deliver powerful anti-inflammatory medication directly to the inflamed spinal nerves. This can provide significant relief, creating a window for more effective physical therapy.
- Radiofrequency neurotomy can be remarkably effective if pain comes from arthritic facet joints. This procedure uses controlled heat to interrupt pain signals from the joint nerves, with relief often lasting six months to several years.
- Minimally invasive procedures allow us to address nerve compression with faster recovery times and less discomfort.
- Regenerative medicine offers innovative treatments like Platelet-Rich Plasma (PRP) and cell-based therapies that use your body’s own healing mechanisms to promote tissue repair. Learn more about our Regenerative Therapy (PRP & Cell-Based Options) in Chicago Ridge.
- Surgery is always our last resort. For a small percentage of patients with severe, persistent pain, options like spinal fusion or artificial disc replacement may be necessary. We work closely with spine surgeons to ensure surgery is the right choice for you.
Lifestyle Changes and Prevention Strategies
While degenerative disc disease is largely a natural part of aging, your daily choices can significantly impact your symptoms and potentially slow the progression of disc degeneration.

- Maintain a healthy weight. This is one of the most powerful changes you can make. Every extra pound adds stress to your spinal discs. Losing even a small amount of weight can make a noticeable difference.
- Stay active with low-impact exercise. Regular activity is one of the best things you can do. Choose activities that strengthen muscles without jarring your discs, such as walking, swimming, or water aerobics. Yoga, Tai Chi, and Pilates are also excellent for building core strength and body awareness.
- Quit smoking. Smoking restricts blood flow to your discs, starving them of nutrients and interfering with healing. Quitting gives your discs a fighting chance to repair themselves and respond better to treatment.
- Practice proper posture. When sitting, keep your back supported, feet flat, and take frequent breaks. When standing, keep your head up and shoulders back. For sleeping, use a firm mattress and pillows to support your spine’s natural curve.
- Improve your ergonomics. Set up your workspace to support your body. Adjust your chair and computer screen height to prevent strain.
- Strengthen your core muscles. A strong core—including your abdominal, back, and pelvic muscles—acts like a natural brace for your spine, taking pressure off your discs. Physical therapy is the best way to learn safe and effective exercises.
Here are some beneficial stretches that may help, but always check with your doctor or physical therapist first:
- Cat-Cow Stretch
- Knee-to-Chest Stretch
- Pelvic Tilts
- Gentle Twists
By weaving these lifestyle changes into your daily routine, you’re not just managing symptoms—you’re taking an active role in your spinal health.
Frequently Asked Questions about Degenerative Disc Disease
Living with degenerative disc disease brings many questions. Here are clear answers to common concerns we hear at Midwest Pain and Wellness.
How serious is degenerative disc disease?
Degenerative disc disease is primarily your body’s natural response to aging, not a progressive disease that will inevitably worsen. While nearly everyone shows signs of it by age 60, only about 5% of adults develop chronic pain.
The condition becomes serious when it significantly impacts your quality of life or leads to nerve compression, causing radiating pain, numbness, or weakness. However, it is not life-threatening and doesn’t inevitably lead to disability. With proper management, most people find effective relief.
When should you seek immediate medical attention? If you experience sudden muscle weakness, foot drop (inability to lift the front of your foot), or changes in bowel or bladder control, these can indicate severe nerve involvement that requires urgent evaluation.
Will the pain from degenerative disc disease get worse over time?
This is a common misconception. Despite the name, your pain does not necessarily worsen over time. In fact, many people find their pain improves as the spine naturally stabilizes.
You might experience flare-ups—periods of intense pain—but these often become less frequent and severe as your body adapts. A proactive approach with physical therapy, core strengthening, and lifestyle modifications can support this stabilization process.
What activities should I avoid with degenerative disc disease?
Understanding which activities to avoid or modify can prevent pain flare-ups and protect your spine.
- High-impact activities: Avoid running on hard pavement, jumping, or contact sports. Choose low-impact alternatives like walking, swimming, or cycling.
- Heavy or improper lifting: Always lift with your legs, not your back. Keep the object close to your body and never twist while holding a heavy load.
- Prolonged sitting: This places a significant load on your lumbar discs. Take frequent breaks to stand and stretch, and use an ergonomic chair.
- Twisting motions that trigger pain: Be mindful and gentle with spinal rotations. If a movement causes sharp pain, that’s your body’s signal to stop.
- Smoking: This directly harms your discs by restricting blood flow and accelerating degeneration. Quitting is one of the most powerful things you can do for your spine.
Listen to your body. Your healthcare provider or physical therapist can help you develop a personalized list of safe activities and proper body mechanics.
Take Control of Your Back Pain
Living with back or neck pain from degenerative disc disease can feel overwhelming, but you have more power over this condition than you might think. Disc degeneration is a natural part of aging, and symptoms often improve as the spine stabilizes.
A proactive approach is the game-changer. Understanding your condition, making lifestyle adjustments, and working with the right medical team can help you reclaim your quality of life. Effective relief is achievable through physical therapy, interventional pain management, regenerative therapies, or a combination of approaches.
At Midwest Pain and Wellness in Chicago Ridge, Illinois, we believe in comprehensive, compassionate care. Our double board-certified doctors specialize in opioid-free, multi-modal pain management, creating custom care plans for your unique goals.
You’ve taken the first step by educating yourself. Now, take the next one. If symptoms are affecting your life, you don’t have to face it alone. Our expert team is ready to develop a treatment plan focused on long-term relief.
Your journey to feeling better starts with a conversation. Contact us to start your journey to pain relief and find how our comprehensive approach can help you get back to the life you love.




