A lot of patients walk in after months of trying to “push through” neck or back pain. Someone from Oak Lawn may stop turning their head fully when backing out of the driveway. Someone in Burbank may notice that standing at the kitchen counter, getting out of bed, or sitting through work becomes its own kind of daily negotiation.
Referring providers see the same pattern from the other side. Imaging may show age-related change, but the symptom story matters more. Pain with extension, rotation, loading, and prolonged standing often points us toward the posterior elements of the spine, especially the facet joints.
A facet joint injection procedure is one of the most useful tools we have when the pain pattern suggests a facet-mediated source. It is targeted, image-guided, minimally invasive, and consistent with an opioid-sparing plan of care. For patients across Palos Heights, Worth, Bridgeview, Hickory Hills, Alsip, Evergreen Park, Orland Park, and the surrounding Illinois communities, it often helps answer two important questions at once: Is the facet joint the pain generator, and can reducing inflammation there improve day-to-day function?
Your Guide to Facet Joint Injections for Spinal Pain Relief
Facet-mediated pain is common, but it is often misunderstood. Many patients assume every spine problem must be a disc problem, a pinched nerve, or something that automatically requires surgery. In practice, the small paired joints at the back of the spine can be major pain generators.
According to the NCBI review on facet joint pain and injections, facet joint pain is estimated to be the source in up to 45% of low back pain patients and 67% of patients with neck pain, and injections provide temporary relief for approximately 75% of patients. Those numbers explain why this procedure remains a core part of modern spine care.
When this procedure moves up the list
A typical patient has already tried some combination of:
- Activity modification: Cutting back on lifting, twisting, or long car rides.
- Medication: Usually anti-inflammatory medication, acetaminophen, or other non-opioid options.
- Rehabilitation: Physical therapy, home exercise, or chiropractic treatment.
- Time: Waiting to see whether the pain settles on its own.
When those measures fail, the next step should be precise, not broader. A facet joint injection procedure makes sense when the pain pattern, physical exam, and imaging together suggest that a specific joint or set of joints is inflamed.
What the procedure does
This injection places medication directly into the suspected facet joint. That matters because broad pain treatment often blurs the picture. A targeted injection does not.
The local anesthetic gives short-acting information. If the painful movement becomes easier soon after the procedure, that supports the diagnosis. The steroid then aims to calm inflammation in and around the joint.
A well-selected facet injection is not just a shot for pain. It is a test with therapeutic value.
What works and what does not
What works is matching the procedure to the symptom pattern. Localized neck pain, low back pain that worsens with extension or rotation, stiffness after rest, and pain that fits the mechanics of a facet joint can respond well.
What does not work is using a facet injection as a catch-all for every kind of spinal pain. If the dominant complaint is shooting pain below the knee, marked numbness, or weakness from nerve root compression, another procedure may fit better.
For new patients and referring providers in Illinois, that distinction matters. Good interventional pain care starts with identifying the right structure, not just offering the nearest injection.
Understanding Your Facet Joints and How They Cause Pain
Think of the facet joints as the knuckles of the spine. They are small joints at the back of each spinal level that help guide motion and keep one vertebra from moving too freely on the next.
When they move normally, you do not notice them. When they become inflamed, arthritic, or mechanically irritated, they can dominate the whole pain picture.
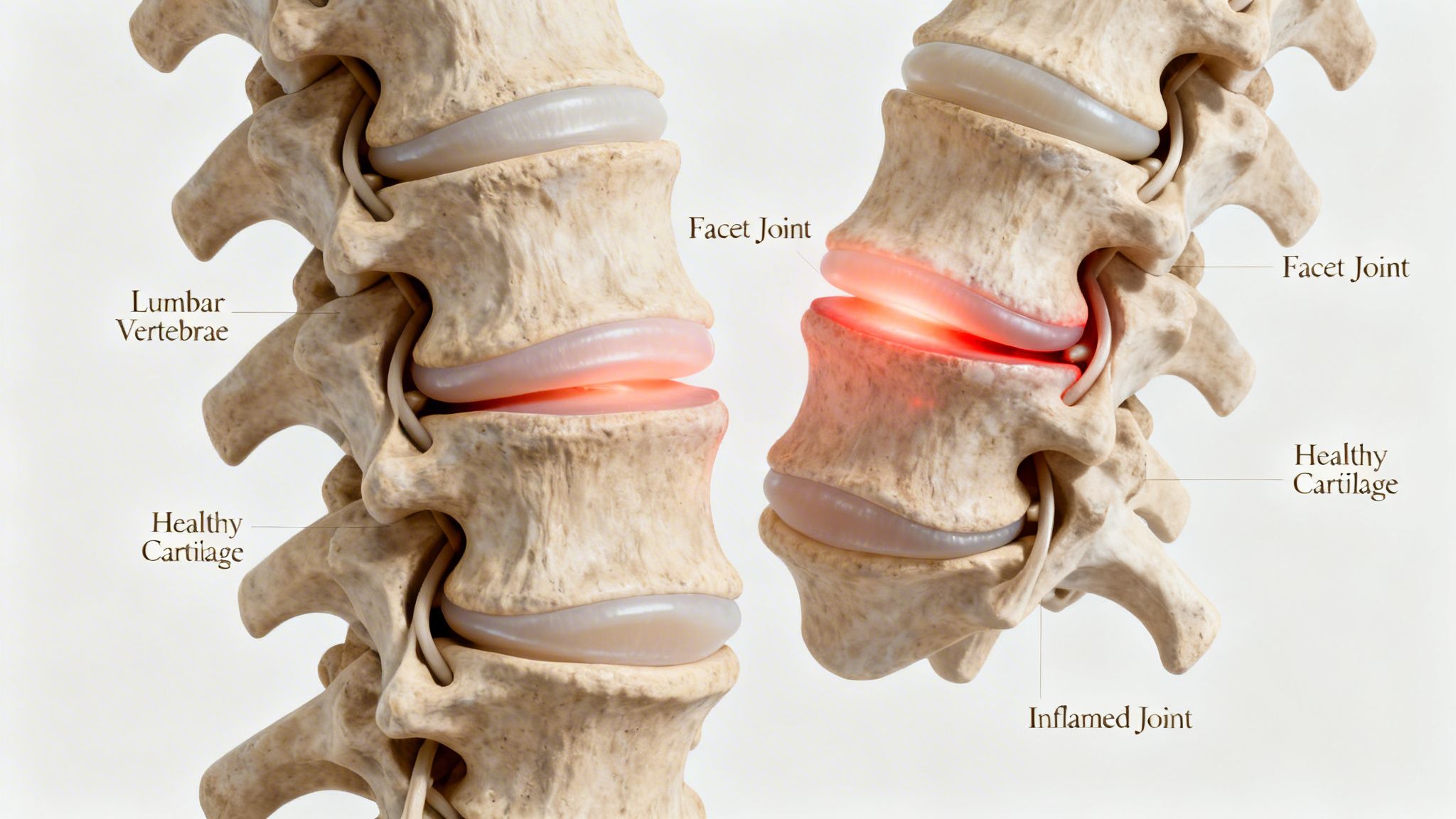
How these joints become painful
Facet joints are synovial joints. They have cartilage, a capsule, and a rich nerve supply. That combination helps explain why they can hurt so much when irritated.
Common clinical drivers include:
- Degenerative arthritis: Cartilage wear can lead to inflammation and painful loading.
- Capsular irritation: The joint capsule itself can become a pain source.
- Instability or altered mechanics: A painful disc or weak supporting musculature can change how force travels through the back of the spine.
- Osteophyte impingement: Bony overgrowth can contribute to irritation around the joint.
These are among the conditions described in the NCBI review above, and they are part of the broader spine conditions clinicians sort through in practice. Patients dealing with related diagnoses can learn more through this overview of conditions we treat.
Pain patterns that often fit facet syndrome
Facet pain is usually more mechanical than electrical. Patients often describe aching, stiffness, and pain with certain positions rather than constant burning or numbness.
In the neck, an irritated facet joint may cause pain into the shoulder girdle or contribute to headache patterns. In the low back, pain can settle into the paraspinals, buttock, or upper thigh.
That pattern matters because referred pain from the facet joint can mimic other problems without following a classic nerve-root distribution.
If the pain is worst with arching backward, twisting, standing upright for too long, or getting out of a chair after sitting, the facet joints deserve a serious look.
Why imaging alone is not enough
MRI and CT can show arthritis, but they do not prove the painful structure by themselves. Some patients have obvious degenerative change and little pain. Others have significant pain with less dramatic imaging findings.
That is why the physical exam and procedural response are so useful. A facet joint injection procedure helps us move from “possible source” to “probable source” with much greater confidence.
The Facet Joint Injection Procedure A Step-by-Step Walkthrough
Most patients feel better once they know exactly what happens on procedure day. The process is straightforward, deliberate, and built around accurate needle placement.
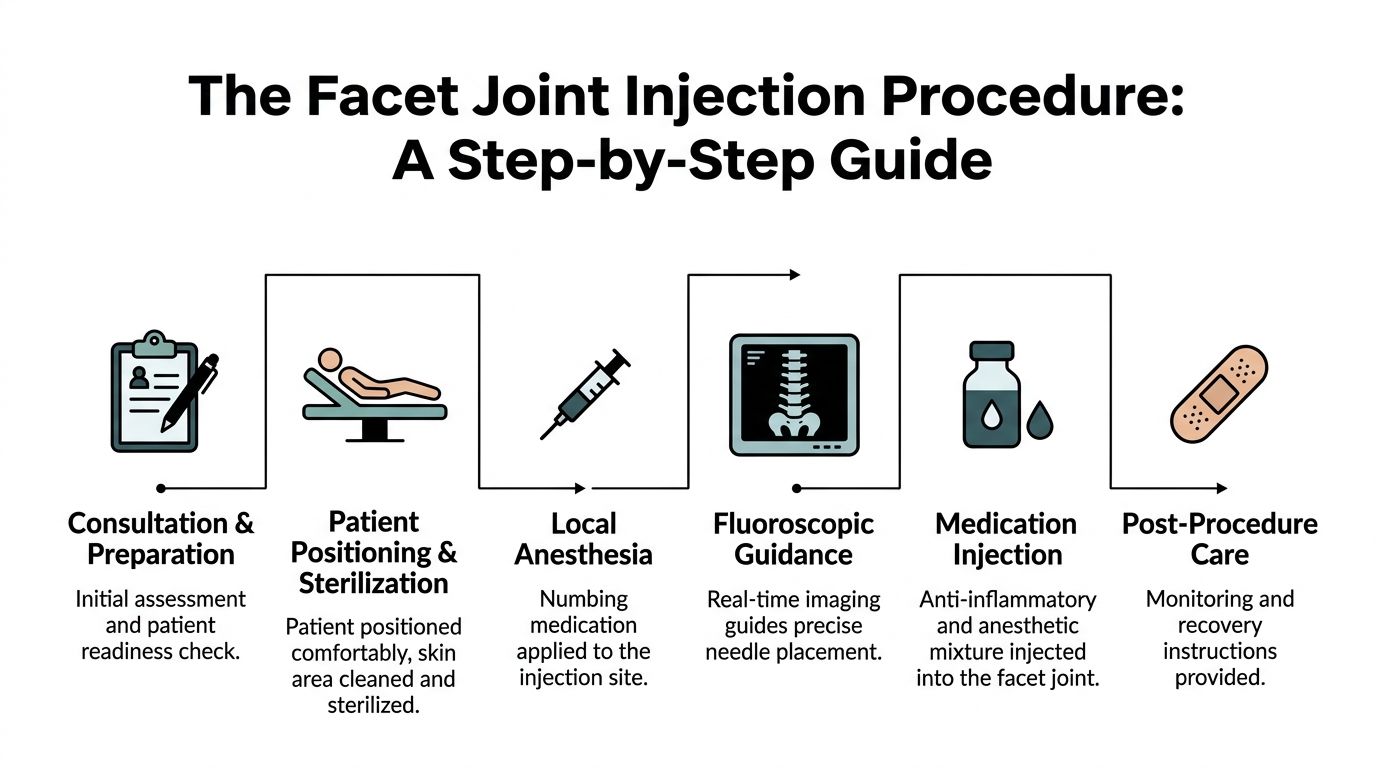
Before the injection
The visit starts before anyone touches a needle. We confirm the target level, review medications, discuss allergies, and make sure the pain pattern still matches the planned procedure.
A good pre-procedure review also addresses practical issues:
- Blood thinners and medical history: These need individualized planning.
- Diabetes management: Steroids can affect blood sugar in some patients.
- Transportation and schedule: Some patients can return to normal activity quickly, but the day should stay light.
Many patients who are considering this treatment are also comparing it with other interventions. A helpful overview of related options appears on this page about procedures used for treatment.
In the procedure room
For lumbar injections, the patient usually lies face down. Positioning is not a minor detail. It affects joint visualization and needle trajectory.
The skin is cleaned carefully. A small amount of local anesthetic numbs the entry point so the deeper part of the procedure is more tolerable.
How imaging guidance improves accuracy
This is not a blind injection. According to the procedural review on image-guided lumbar facet joint injection technique, the clinician advances a 23G spinal needle to the target joint under fluoroscopic or CT guidance. After confirming placement with a small amount of contrast dye, 1 to 1.5 mL of a long-acting steroid such as triamcinolone mixed with an anesthetic such as bupivacaine is injected. That same review notes that injecting more than 1.5 to 2 mL risks rupturing the joint capsule.
Those details matter in real practice.
A facet joint is small. If the needle is off target, the injection may still bathe nearby tissue, but the diagnostic value drops. If the volume is too high, the capsule can rupture and the medication can spread outside the joint. That can blur the result and reduce precision.
What the patient usually feels
Most patients feel pressure more than pain. Some feel a brief pinch with the numbing medicine, then a sense of fullness or mild ache as the joint is entered and the medication goes in.
Typical sensations include:
- Brief skin sting: From local anesthetic.
- Pressure deep in the back or neck: As the needle approaches the joint.
- Temporary reproduction of familiar pain: Sometimes helpful diagnostically.
- Mild post-procedure soreness: Usually short-lived.
If a patient feels sharp radiating pain or anything clearly outside the expected pattern, the procedure should pause and be reassessed. Precision requires constant feedback.
The safest and most useful injection is not the fastest one. It is the one done with careful imaging, low-volume technique, and constant correlation with the patient’s symptoms.
After the injection
Patients are monitored briefly and then discharged with instructions. Some notice immediate improvement from the anesthetic. Others feel sore first and then improve over the following days as the steroid begins to calm inflammation.
The first day is usually simple:
- Take it easy: Light activity is fine unless your clinician gives different instructions.
- Use ice if needed: This helps localized soreness.
- Track your response: What movements improved, and for how long, is clinically useful.
For referring providers, that response pattern matters almost as much as the absolute pain score. Immediate anesthetic relief supports the diagnosis. A later anti-inflammatory benefit supports the therapeutic value.
Evaluating the Benefits Risks and Expected Outcomes
A facet joint injection procedure can help a patient, but it is not magic and it is not permanent. The most productive conversations are the honest ones.
The main benefit is targeted relief in a structure that is often difficult to confirm by history and imaging alone. If the right joint is treated in the right patient, the procedure can reduce pain enough to improve walking, sleep, transfers, driving tolerance, and participation in therapy.

What the evidence supports
The Orthopedic Reviews case series on therapeutic facet joint injections for chronic spinal pain describes meaningful benefit in selected patients, including a 78-year-old female who achieved 80% pain reduction lasting for months after bilateral injections. The same review notes broader findings of 75% success for temporary relief and 74% immediate positive response.
Those are encouraging numbers, but the key phrase is selected patients.
What good outcomes usually look like
Relief is not always dramatic. Sometimes the win is that a patient can stand longer, walk with less guarding, or restart physical therapy without flaring up.
Common positive outcomes include:
- Lower pain during extension and rotation
- Less morning stiffness
- Improved tolerance for sitting to standing
- Better participation in rehab
- Reduced reliance on oral pain medication
In many patients, that is enough to change the trajectory of care.
Limits of the procedure
Not every painful spine has a facet-driven problem. Even when the facet joint is involved, it may not be the only driver. Disc degeneration, stenosis, myofascial pain, sacroiliac pain, deconditioning, and central sensitization can overlap.
That is why a facet injection should not be sold as a cure. It is better understood as a targeted intervention with both diagnostic and therapeutic value.
Risks and trade-offs
The procedure is generally low risk, but “low risk” does not mean “no risk.”
Expected trade-offs include:
- Temporary soreness: Common after needling a joint.
- Bleeding or bruising: More relevant in patients with anticoagulation concerns.
- Infection: Rare, but it is one reason sterile technique matters.
- Steroid effects: Important to discuss in patients with diabetes or certain medical conditions.
A referral makes more sense when everyone involved understands both sides. The upside is targeted relief without opioid escalation. The limitation is that response varies, and durability varies with it.
The best predictor of satisfaction is not promising too much. It is matching the procedure to the right pain pattern and setting realistic expectations from the start.
Comparing Facet Injections Medial Branch Blocks and RFA
Patients often hear three terms in one visit and assume they are interchangeable. They are related, but they are not the same procedure.
The easiest way to think about them is by target and purpose. A facet injection treats the joint itself. A medial branch block tests the nerve supply to that joint. Radiofrequency ablation, often called RFA, aims for longer-lasting relief by interrupting pain signaling through those same medial branch nerves after successful diagnostic workup.
How the three options differ
| Procedure | Primary Goal | Typical Duration of Relief | Role in Treatment Plan |
|---|---|---|---|
| Facet joint injection | Treat inflammation inside the joint and help confirm the pain source | Variable, often temporary | Useful when the joint itself is suspected to be inflamed and both diagnostic and therapeutic value are desired |
| Medial branch block | Diagnose whether the nerves supplying the facet joint are carrying the pain | Short acting by design | Used to confirm candidacy for next-step treatment, especially if longer-term denervation is being considered |
| Radiofrequency ablation | Provide longer-term reduction in pain signaling from the facet joint nerves | Longer than a diagnostic block in appropriate responders | Usually considered after a convincing block response |
When a direct joint injection makes sense
A facet joint injection procedure is often preferred when the suspected problem is active inflammation within the joint or capsule. It is especially useful when the history and exam fit, but the clinician still wants clearer confirmation before escalating to denervation.
This is also a reasonable starting point when a patient needs both symptom control and diagnostic clarification.
When medial branch blocks are more useful
If the clinical question is less about the joint space itself and more about confirming whether the medial branch nerves are transmitting the pain, a block may be the cleaner test.
That distinction matters because some patients do not need repeated intra-articular treatment. They need a path toward a longer-lasting nerve-targeted option.
Where RFA fits
RFA is not the first move for every patient with back pain. It is best used when the workup strongly supports facet-mediated pain and diagnostic blocks are convincing.
For many patients, the pathway looks like this:
- Evaluation: Confirm the pain pattern and rule out competing dominant pain sources.
- Diagnostic clarification: Use a targeted injection or block.
- Longer-term planning: Consider RFA if the earlier steps strongly support the facet as the generator.
For referring providers, that sequence keeps the treatment plan rational. For patients, it explains why one successful injection does not automatically mean “repeat the same thing forever.”
Your Care Journey at Midwest Pain & Wellness
The quality of a facet intervention depends on more than the injection itself. Candidate selection, imaging review, positioning, technique, and follow-up all shape the result.
That matters for patients coming from Evergreen Park, Palos Heights, Alsip, Orland Park, and nearby Illinois communities, especially when the pain story is complicated by prior injury, surgery, work restrictions, or an active workers’ compensation or personal injury claim.
What careful evaluation looks like
A strong evaluation answers several questions before the procedure is scheduled:
- Does the pain pattern fit a facet source?
- Are there red flags or competing pain generators?
- Have conservative measures already been tried?
- Would a direct joint injection or a different diagnostic path make more sense?
Such evaluation helps avoid many unnecessary procedures. Good interventional care is selective.
Why technique still matters after the diagnosis
According to Spine-health’s review of the facet joint injection procedure, proper patient positioning, including use of an abdominal pillow to gently arch the low back, and oblique fluoroscopic views are important for accuracy. That same review notes that confirmed intra-articular injections yield superior diagnostic specificity of 80% to 90%, which is important when deciding on next-step care such as RFA, including in workers’ compensation and personal injury settings.
That point deserves emphasis. A poorly targeted injection can create confusion. A precise one can clarify the treatment path.
What patients should expect around the procedure
Preparation is usually simple, but details matter.
- Medication review: Especially blood thinners, diabetes medications, and allergies.
- Day-of planning: Keep the schedule light and ask whether a driver is recommended for your case.
- Recovery: Expect mild soreness to be possible, and pay attention to how your familiar pain behaves afterward.
For a new patient, the best next step is a full evaluation rather than guessing whether the facet joint is the source. Appointment requests can be made through this scheduling page.
The most effective opioid-sparing care is not one procedure in isolation. It is a plan that uses the right procedure at the right time, then builds on that response with rehabilitation and follow-up.
The broader treatment philosophy
A facet joint injection procedure fits best inside a multimodal plan. That may include physical therapy, home exercise, medication review, other image-guided interventions, or progression to medial branch blocks and RFA when appropriate.
That is especially important in Illinois patients trying to stay active, keep working, or recover after an injury. Pain care should improve function, not just reduce a number on a pain scale.
Frequently Asked Questions About the Procedure
Will the injection cure my back or neck pain
No. It can reduce inflammation, improve function, and help confirm that the facet joint is the pain source. Some patients get meaningful temporary relief. Others improve enough to move to a better long-term strategy.
Can I drive myself home
That depends on the exact plan, the body region treated, your medical history, and whether any additional medication is used around the procedure. Ask for instructions before the appointment rather than assuming.
How fast can I get back to normal activity
Many patients resume normal activity quickly, often within a short recovery window. The practical advice is to take the rest of the day lightly and then follow the instructions given for your specific case.
Will insurance cover a facet joint injection procedure
Coverage varies by plan, diagnosis, prior treatment history, and documentation requirements. In practice, insurers often want a clear clinical rationale and evidence that conservative care has already been attempted.
How many injections can I have
There is no one-size-fits-all answer. The right number depends on your diagnosis, your response, your medical history, and whether the injection is being used diagnostically, therapeutically, or as part of a pathway toward another procedure.
What if the injection helps only briefly
A brief but meaningful response can still be useful. It may confirm the pain generator and support a different next step, such as a medial branch block or radiofrequency ablation, rather than merely repeating the same injection.
If neck or back pain is limiting your daily life in Oak Lawn, Palos Hills, Palos Heights, Worth, Bridgeview, Hickory Hills, Alsip, Burbank, Evergreen Park, Orland Park, or nearby Illinois communities, Midwest Pain & Wellness offers evidence-based, opioid-sparing care led by double board-certified interventional pain specialist Dr. Yaw Donkoh. A thorough evaluation can determine whether a facet joint injection procedure fits your pain pattern and whether it should stand alone or be part of a broader treatment plan.



