If you're reading this after another missed workday, another canceled dinner, or another morning that started with that familiar pressure behind your eyes, you're not alone. Chronic migraine changes how people plan everything. Many patients stop asking, “Will I get a migraine?” and start asking, “How bad will this one be, and what will I have to miss?”
That constant vigilance is exhausting. You may already have tried rescue medications, dark rooms, caffeine, hydration, supplements, or preventive pills that either didn't help enough or caused side effects you couldn't live with. At that point, a reasonable question is simple: How does Botox help migraines, and is it different from everything else I've already tried?
It is different. Botox for migraine isn't used to stop an attack that's already in progress. It's a preventive treatment for chronic migraine, designed to calm the nerve pathways involved in repeated attacks before they build into the next cycle.
The Relentless Cycle of Chronic Migraine
Chronic migraine rarely stays contained to your head. It reaches into your job, your sleep, your patience, and your relationships. People start planning around noise, light, long drives, weather changes, stress, poor sleep, and even family events they want to enjoy.
One common pattern goes like this. A patient wakes up with a low-grade headache, pushes through work, takes a rescue medication by afternoon, feels foggy by evening, then spends the next day recovering from the migraine or from the medication used to control it. A few better days follow, then the pattern starts again.
That cycle creates frustration because partial relief can be its own problem. If a treatment works only sometimes, people still have to live as if the next attack is right around the corner.
When rescue care isn't enough
Rescue medications matter. They have a role. But they don't replace a prevention strategy when headaches are happening over and over.
Botox treats a different part of the problem. Instead of chasing each migraine after it begins, it aims to reduce how often the migraine process gets started in the first place. For patients living with chronic headache conditions, that shift matters. It changes the goal from survival to control.
A specialist will also look carefully at whether the headache pattern is chronic migraine or whether another pain condition is overlapping. Some patients have neck pain, nerve irritation, or mixed headache patterns that need a broader plan. That's one reason a full evaluation matters, especially when symptoms have been going on for months or years. You can review the broader range of conditions treated in pain management if your symptoms don't fit neatly into one category.
Chronic migraine treatment works best when the diagnosis is precise. A patient can have migraine and another pain generator at the same time.
Why Botox gives some patients new hope
Botox isn't a miracle cure, and it doesn't help every patient. But it is an FDA-approved preventive option with strong clinical evidence behind it for chronic migraine, not just occasional headaches.
That distinction is important. Patients who've already failed several treatments often assume the next option will be more of the same. Botox isn't just “another medication.” It's a targeted procedure that approaches migraine through the nerve endings involved in pain signaling.
For the right patient, that can mean fewer headache days, less disruption, and less dependence on repeatedly taking medication just to get through the week.
How Botox Blocks Migraine Signals Before They Start
A patient may tell me, “My migraines seem to start in my neck or behind my eyes, and once they build, the whole day is gone.” That pattern fits what we often see in chronic migraine. The pain system is already primed before the attack feels obvious.
Botox for migraine is onabotulinumtoxinA. In this setting, it is used to reduce abnormal pain signaling from sensory nerve endings in the head and neck, not for cosmetic purposes. The goal is prevention. Treatment is aimed at interrupting the process that helps migraines build momentum.
Nerves involved in chronic migraine can become overly reactive. When that happens, they release pain-related chemicals such as substance P, glutamate, and calcitonin gene-related peptide (CGRP). Those signals can promote inflammation around the nerve endings and make the central nervous system more sensitive over time. Botox helps by reducing that chemical release at the peripheral nerve level.
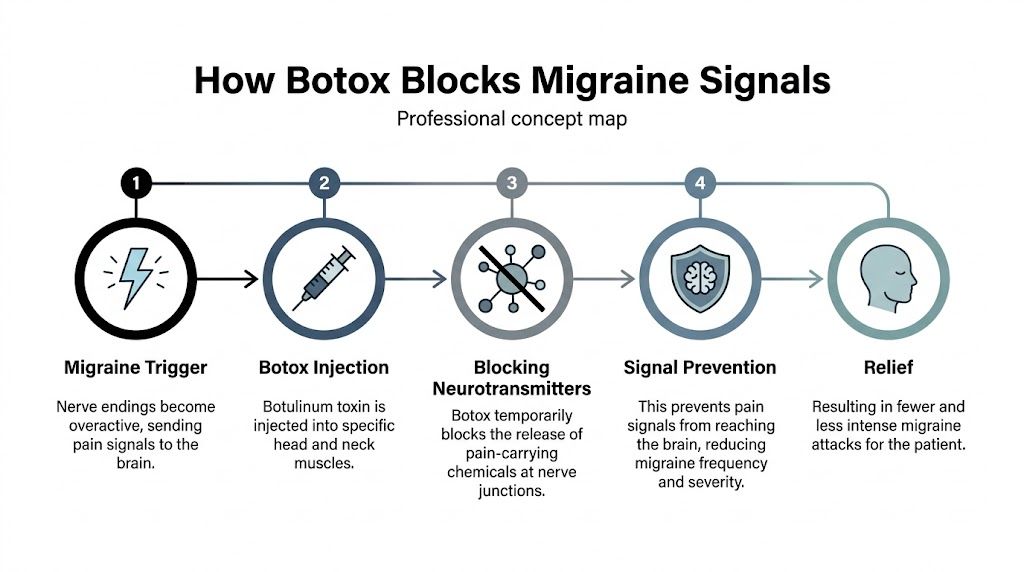
What Botox blocks
The sequence is fairly straightforward:
- Migraine-related nerves are easier to trigger. In chronic migraine, some sensory nerves in the scalp, forehead, temples, and neck stay on high alert.
- Those nerves release pain-signaling chemicals. That release contributes to local irritation and ongoing activation of the migraine pathway.
- Repeated activation lowers the threshold for future attacks. The nervous system becomes more reactive, so smaller triggers can set off larger symptoms.
- Botox reduces signaling at the nerve ending. With less release of those neurochemicals, the cycle is less likely to escalate.
- Over time, the system becomes less irritable. That is why the treatment is preventive rather than immediate.
In plain language, Botox helps quiet the part of the migraine process that keeps feeding itself.
Why it takes time
This treatment does not work like a rescue medication taken during an active attack. It works gradually, across repeated treatment cycles, because the goal is to lower the baseline sensitivity of the migraine network. Some patients notice improvement after the first round. Others need more than one cycle before the benefit is clear.
That trade-off matters. Botox can be a strong option for the right patient, but it asks for patience and follow-through. At a clinic visit in the Chicago Ridge area, including practices such as Midwest Pain & Wellness, I usually set expectations early so patients do not judge the treatment too quickly. If someone stops after one session because the first month was still rough, they may walk away before the preventive effect has had time to build. You can review related interventional pain treatment options used in clinic if migraine overlaps with neck pain or other chronic pain issues.
Practical rule: Judge Botox by whether headache frequency and severity improve over time, not by whether it stops a migraine the same day.
What Botox doesn't do
Botox does not cure migraine, remove every trigger, or guarantee that rescue medication will never be needed again.
It also does not fix the wrong diagnosis. Sinus symptoms, medication overuse, occipital neuralgia, sleep apnea, cervical spine pain, and other overlapping conditions can all complicate the picture. That is one reason a careful consultation matters. A patient may have chronic migraine and a second pain generator at the same time.
A good evaluation usually focuses on four areas:
- Headache pattern: How often headaches occur, how long they last, and whether the pattern meets chronic migraine criteria
- Migraine features: Nausea, light sensitivity, sound sensitivity, aura, dizziness, or other associated symptoms
- Treatment history: Which preventive treatments have already been tried, and whether they failed because of side effects, poor response, or both
- Pain overlap: Neck pain, prior injury, sleep issues, jaw tension, or nerve irritation that may also need treatment
That is where patient selection makes the difference. Botox works best when it is matched to the right headache pattern and used as part of a plan grounded in the patient’s actual symptoms, not a one-size-fits-all approach.
What to Expect During Your Botox Treatment Sessions
You arrive for your appointment in Chicago Ridge after another month built around backup plans. You are not looking for a spa treatment or a quick fix. You want to know how the visit works, how uncomfortable it is, and whether it fits into real life.
Botox for chronic migraine is done with a set medical protocol. The goal is consistent placement in muscle groups and nerve-rich areas involved in migraine, not chasing pain from one day to the next. For patients seen at interventional pain clinics such as Midwest Pain & Wellness, that structure matters because migraine often overlaps with neck pain, jaw tension, or other pain conditions that also need to be sorted out during follow-up.
The treatment uses a series of small injections across areas that commonly include the forehead, temples, back of the head, upper neck, and shoulders. The number of injections can sound intimidating on paper. In practice, the visit is usually short and very tolerable.

What the appointment usually feels like
Each injection is placed with a very fine needle. Patients usually describe the sensation as brief pinches or pressure points rather than one prolonged painful procedure. You are awake, there is no sedation, and you can usually drive yourself home afterward.
Precision matters more than force. Small differences in placement affect comfort, coverage, and side effects. That is one reason many patients prefer to have migraine Botox done in a medical pain practice that regularly treats head, neck, and nerve-related pain.
A typical visit includes:
- A quick symptom review: Your clinician checks headache frequency, flare patterns, medication use, and any side effects from the last cycle.
- Targeted site planning: Injection points follow the established migraine protocol, with adjustments when symptoms or muscle tension justify it.
- The injections themselves: The medication is given in a sequence that usually takes only a few minutes.
- Aftercare instructions: Patients can usually return to normal daily activity the same day.
Why the timing matters
Botox is usually repeated every 12 weeks. That spacing is based on how the medication works over time and how chronic migraine is tracked in clinical practice.
Coming in too early is not usually helpful. Waiting too long can let the preventive benefit fade, which makes it harder to judge the true response. I tell patients to treat the first few rounds as a planned course, not a one-time test.
Consistency gives us cleaner information.
What the first few cycles can look like
The first session rarely tells the whole story. Some patients notice that attacks are less intense before they notice fewer headache days. Others still get migraines, but they recover faster, miss less work, or need rescue medication less often.
Those changes count.
A headache diary helps more than memory, especially if your schedule is busy or your symptoms blur together over several weeks.
| What to track | Why it matters |
|---|---|
| Headache days | Shows whether frequency is changing over time |
| Migraine severity | Helps capture benefit even before frequency drops |
| Attack duration | Shorter attacks can mean meaningful improvement |
| Rescue medication use | Less reliance often signals better baseline control |
| Missed activities | Function matters as much as pain scores |
Trade-offs are part of an honest discussion. Some patients have temporary soreness at injection sites, a heavy feeling in the forehead, or short-lived neck discomfort. A careful consultation also helps separate migraine from overlapping pain generators. If neck or spine pain is part of the problem, it may help to review the procedures used for treatment in pain management as part of a broader plan.
How Effective Is Botox for Preventing Chronic Migraine
Botox has some of the best clinical evidence we have for chronic migraine prevention, and its benefit shows up in day-to-day function, not just in trial charts. In the phase 3 PREEMPT studies published in Cephalalgia, patients receiving onabotulinumtoxinA had fewer headache days over time, and many achieved a meaningful reduction in monthly headache burden after repeated treatment cycles, as reported in the PREEMPT clinical trial publication.
What those results mean in practice
For a patient with chronic migraine, even a partial drop in headache days can change the month. Fewer missed shifts. Fewer family plans canceled at the last minute. Less time spent rationing rescue medication and waiting for the next attack.
The usual benchmark in studies is a 50 percent reduction in headache days. That is useful, but it is not the only definition of success. I look at whether attacks are easier to get through, whether recovery is faster, and whether the patient can count on more stable weeks. Those gains matter, especially for someone who has already failed oral preventives or could not tolerate their side effects.
This also helps set expectations for treatment in a real clinic setting, including here in the Chicago Ridge area. Patients coming to Midwest Pain & Wellness are often balancing work, driving, child care, and other medical appointments. A treatment is only effective if the improvement is large enough to justify repeating it every 12 weeks.
How specialists judge whether Botox is working
Response should be measured in more than one way. Headache-day counts matter, but they are not the whole story.
A practical assessment usually includes:
- Monthly headache days
- Migraine intensity
- How long attacks last
- Rescue medication use
- Ability to work, drive, sleep, and keep normal plans
That broader view keeps the decision honest. Some patients have a clear reduction in headache frequency. Others still have frequent headaches but function better because the attacks are less severe or less disruptive.
Real trade-offs and realistic expectations
Botox is a proven preventive treatment for chronic migraine. It is not a guaranteed fix, and it is not the right treatment for every type of head pain.
Some patients get strong relief. Some get moderate benefit that still makes treatment worth continuing. Some do not improve enough to stay on it. That is why follow-up matters. In practice, the best candidates are usually patients with a confirmed chronic migraine pattern who want a long-term strategy and are willing to judge progress based on function as well as frequency.
The goal is better control. For many patients, that means life stops revolving around the next migraine.
Is Botox the Right Migraine Treatment for You
Botox is a strong option for the right patient and a poor fit for the wrong one. The key is matching the treatment to the diagnosis rather than hoping one more intervention will somehow cover every kind of head pain.
A simple checklist helps.
Signs you may be a good candidate
You may be a reasonable candidate for Botox if several of these apply:
- Your diagnosis is chronic migraine. The treatment is intended for patients with 15 or more headache days per month.
- You need prevention, not just rescue care. Acute medications may help, but they aren't controlling the overall pattern.
- You've already tried other preventive approaches. Many patients reach Botox after oral preventives didn't help enough or caused side effects.
- You can commit to repeat treatment. Botox works best when it's given on schedule and judged over multiple cycles.
That last point matters more than many people realize. Patients sometimes want to know whether one treatment will answer everything. In migraine prevention, consistency usually tells the story more clearly than a single early response.

When subtype matters
Not every chronic migraine patient looks the same. Some have dizziness, motion sensitivity, or balance-related symptoms that make the picture more complicated. That's where subtype-specific evidence becomes useful.
A 2022 systematic review on botulinum toxin in migraine subtypes found that Botox was particularly effective for vestibular migraine and chronic refractory migraine, with meaningful reductions in headache burden and vertigo-associated disability in vestibular migraine. For patients who've been told their symptoms are “atypical” because dizziness plays a major role, that matters.
Reasons to pause before choosing Botox
Botox may not be the best first move if the diagnosis is unclear or if another issue is dominating the picture. Examples include:
- Episodic migraine rather than chronic migraine
- Another primary headache disorder
- Strong medication overuse pattern
- Untreated sleep, neck, jaw, or post-injury factors that are driving symptoms
A consultation should sort that out. The visit isn't just about saying yes or no to Botox. It's about identifying whether migraine is the main problem, part of the problem, or being confused with something else.
For many patients, the most useful question isn't “Can I get Botox?” It's “Does my headache history make Botox the right next step?”
Your Path to Migraine Relief in the Chicago Area
Patients in Chicago Ridge, Oak Lawn, Palos Hills, Palos Heights, Worth, Bridgeview, Hickory Hills, Alsip, Burbank, Evergreen Park, and Orland Park often need more than a generic migraine handout. They need a local care plan that accounts for chronic headache, neck pain, injury history, work demands, and insurance realities in Illinois.
That matters because migraine doesn't always arrive alone. Many patients also deal with cervical pain, post-injury flare patterns, or spine-related symptoms that complicate the picture. In those situations, Botox may be part of a broader plan rather than the entire plan.
Why a pain clinic perspective can help
Botox fits well within multimodal, opioid-sparing care, especially for patients with overlapping neck and spine pain or for those navigating post-injury and workers' compensation issues. Migraine Canada notes in its discussion of Botox within migraine treatment plans that Botox integrates well into coordinated care and is a durable option that can reduce reliance on systemic medications.
That framework is useful in real practice. A patient may need migraine prevention, but also evaluation of cervical trigger points, referred pain, posture-related aggravators, or another interventional treatment for a separate pain generator. Treating only one layer of the problem can leave patients feeling like the therapy “sort of worked” when the underlying issue is that more than one pain source was active.
What coordinated care looks like
In a practical sense, a complete migraine evaluation in an interventional pain setting may include:
- Headache pattern review: Frequency, triggers, medication use, and functional impact
- Neck and upper back assessment: Looking for musculoskeletal contributors that amplify migraine symptoms
- Treatment sequencing: Deciding whether Botox should stand alone or be paired with other non-opioid interventions
- Insurance and documentation support: Especially important when prior treatments or injury-related claims are involved
For patients in the south and southwest suburbs of Chicago, local access matters. Travel during a migraine isn't trivial, and repeat care is easier when the office is close enough to make regular treatment realistic.
Dr. Yaw Donkoh is a double board-certified interventional pain specialist, and patients who want to understand his background can review the physician profile for Dr. Donkoh. In the Chicago Ridge area, Midwest Pain & Wellness offers Botox for chronic migraine within a broader pain management model that also addresses overlapping pain conditions when needed.
Good migraine care is often local, consistent, and coordinated. That's what helps a preventive treatment actually stay on track.
Frequently Asked Questions About Botox for Migraines
What side effects are most common
Most side effects are temporary and manageable. Patients may notice injection-site discomfort, neck stiffness, or a sense of soreness in treated areas. Some people also worry about eyelid droop or feeling “frozen,” but migraine injections are placed for medical purposes, not cosmetic styling.
The most important point is that Botox for chronic migraine is generally considered well tolerated when given by an experienced clinician using the appropriate protocol. If you've had prior neck pain or unusual reactions to injections, mention that before treatment so the plan can be adjusted thoughtfully.
Will insurance cover Botox for migraine treatment
Coverage depends on your specific plan and your diagnosis. In general, insurers often want documentation that you have chronic migraine and that you've already tried other preventive treatments.
That usually means your clinician's office will submit a prior authorization request and include your history, diagnosis, and prior treatment failures when required. Patients should also expect that insurance rules can change and may differ across plans. The best approach is to ask the office what records are needed and verify your benefits directly with your insurer.
Can I still use rescue medication
Yes. Botox is a preventive treatment, not a rescue treatment.
If you still have breakthrough migraines, you may continue to need an acute plan. In fact, one sign that Botox is helping may be that you still carry rescue medication, but you use it less often and with less urgency because the baseline pattern has improved.
How soon will I know if it's working
Some patients notice early changes, but the most reliable way to judge Botox is over repeated treatment cycles. Track frequency, severity, duration, and how often headaches interfere with work, family life, or sleep.
A headache diary doesn't need to be complicated. A phone note or calendar can be enough if you record consistent information.
Does Botox help every kind of headache
No. It is used for chronic migraine, not every headache disorder.
That's why evaluation matters. A person may think they're having migraine when the main issue is cervicogenic headache, occipital neuralgia, medication overuse, or another condition. Sometimes patients have both migraine and another pain source, and both need treatment.
If I have neck pain too, does that change anything
It can. Neck pain may be part of the migraine picture, a trigger, or a separate diagnosis. That doesn't automatically rule Botox in or out, but it does mean your treatment plan should account for both problems instead of assuming one procedure will solve everything.
What if Botox doesn't help enough
Then the next step is reassessment, not frustration. Your clinician should review whether the diagnosis was correct, whether enough treatment cycles were completed, whether another pain condition is overlapping, and what other non-opioid options make sense.
A good migraine plan isn't built on blind repetition. It's built on measured follow-up and course correction when needed.
If chronic migraine is controlling your schedule, your energy, and your ability to function, it's worth getting a clear diagnosis and a treatment plan built around prevention. Midwest Pain & Wellness provides interventional, opioid-sparing care in Chicago Ridge for patients in surrounding Illinois communities who need a practical next step for chronic migraine and overlapping pain conditions.



