A patient from Orland Park comes in after missing another week of work because of migraines, or after months of neck pulling and spasm from cervical dystonia that makes driving and sleeping difficult. The first question is often practical, not academic. How long will Botox help?
For medical Botox, the usual answer is about 3 to 4 months, but that number needs context. In pain medicine, I use Botox for treatment goals such as fewer migraine days, less muscle overactivity, better function, and less reliance on short-term rescue medication. Cosmetic use can help frame the discussion, but it is not the main issue for patients in Oak Lawn, Palos Hills, Palos Heights, Worth, Bridgeview, Hickory Hills, Alsip, Burbank, Evergreen Park, Orland Park, and nearby Illinois communities who are looking for opioid-sparing relief.
Duration matters because treatment planning affects real life. Patients need to know whether relief may last long enough to justify time off work, transportation, insurance authorization, and repeat visits every few months. The timeline also varies by condition, muscle pattern, dose, and individual response.
Botulinum toxin type A is widely used in both medical and aesthetic care, with more than 4.7 million procedures performed in 2023, according to the American Society of Plastic Surgeons 2023 procedure statistics. In practice, the more useful point is that Botox has a familiar treatment window. Patients and physicians can usually plan around it, then adjust based on symptom relief and function rather than guesswork alone.
Your Guide to Botox Duration for Pain Relief
People usually don’t ask how long does Botox last out of curiosity alone. They ask because they’re deciding whether it’s worth arranging rides, time off work, childcare, insurance paperwork, and the emotional energy that comes with trying one more treatment.
For pain conditions, that question deserves a direct answer. Most patients can expect Botox to last around 3 to 4 months, but medical Botox is used differently than cosmetic Botox. The muscles targeted are different, the dosing strategy is different, and the treatment goal is different. In aesthetics, the target may be forehead movement or crow’s feet. In pain management, the aim may be fewer migraine days, less neck spasm, less pulling, and better day-to-day function.
What that answer means in real life
If Botox is being used for chronic migraine, the treatment schedule is typically built around a 12-week cycle in medical practice. If it’s being used for cervical dystonia, the timing is also often planned around a similar interval, but the exact response can be more individualized because the involved muscles, severity, and dose vary from patient to patient.
Cosmetic results can help give context, but they don’t tell the whole story for pain care. A person comparing forehead Botox to migraine Botox is comparing two related treatments with different treatment maps and different clinical endpoints.
Relief should be judged by function, not only by whether the medicine is still technically active. For migraine, that may mean fewer attacks. For cervical dystonia, it may mean less pulling and easier head position.
Why patients in Illinois should think beyond one injection
A single Botox session isn’t usually the whole strategy. Chronic migraine and cervical dystonia are ongoing conditions, so treatment works best when patients understand the cycle from onset to peak effect to gradual wearing off.
That matters for patients across Chicago Ridge and the surrounding Illinois suburbs, especially those looking for opioid-sparing care. A well-planned Botox schedule can be part of a broader pain management approach that focuses on function, prevention, and consistency instead of chasing symptoms after they flare.
Here’s the practical framework patients should use:
- Know the average: Most Botox effects last about 3 to 4 months.
- Know the condition: Migraine and cervical dystonia follow medical protocols, not cosmetic norms.
- Know the goal: The point is steadier control of symptoms, not a one-time fix.
- Know the plan: Repeat treatment is usually part of the design, not a sign that something failed.
How Botox Works A Simple Explanation
Botox works like a temporary pause button between a nerve and a muscle. The nerve normally sends a signal telling the muscle to contract. Botox interrupts that signal for a while, so the muscle becomes less active.
That’s why Botox helps in both cosmetic and medical settings. If a facial muscle keeps folding the skin, reducing contraction can soften lines. If head or neck muscles are contributing to a pain condition, reducing overactivity can lower strain, spasm, or symptom burden.
It pauses communication, not the muscle itself
A simple way to think about it is this: the muscle is still there, and the nerve is still there, but the message between them gets dampened. Botox doesn’t erase the muscle, and it doesn’t permanently damage the nerve. It creates a temporary reduction in the chemical signaling that drives contraction.
In more technical terms, Botox inhibits acetylcholine release at the neuromuscular junction by affecting SNAP-25. Patients don’t need to memorize that, but it explains the key point. The treatment is temporary by design.
Why the effect wears off
Botox doesn’t stop working all at once. Over time, the body restores function through nerve recovery and new signaling pathways. As that happens, muscle activity gradually returns.
That gradual return is why patients often describe Botox as wearing off slowly instead of suddenly. It also explains why retreatment is expected. The treatment isn’t failing. The body is resuming normal nerve-to-muscle communication.
A broader medical plan matters here. Clinics that use multimodal pain care may combine Botox with other interventions depending on the diagnosis, exam findings, and functional goals. For an overview of options that can be part of an integrated treatment approach, patients can review procedures used for treatment at Midwest Pain & Wellness.
Botox is temporary because the body is active. Nerves recover, signaling resumes, and muscle activity slowly returns.
Why onset is not immediate
One of the most common misunderstandings is expecting instant relief the day of treatment. Botox needs time to affect nerve signaling. In general observations across practice and patient data, effects often begin within days and become more noticeable later, which is why the timeline after injection matters almost as much as the overall duration.
That delayed onset can be frustrating if you’re in pain and hoping for immediate change. It’s also normal. Knowing that up front helps patients judge their result more accurately and avoid assuming the treatment didn’t work too early.
Botox Duration by Treatment Goal
The biggest mistake patients make is assuming every Botox treatment follows the same timeline and the same rules. It doesn’t. The average duration may sound familiar across use cases, but the goal of treatment changes what matters most.
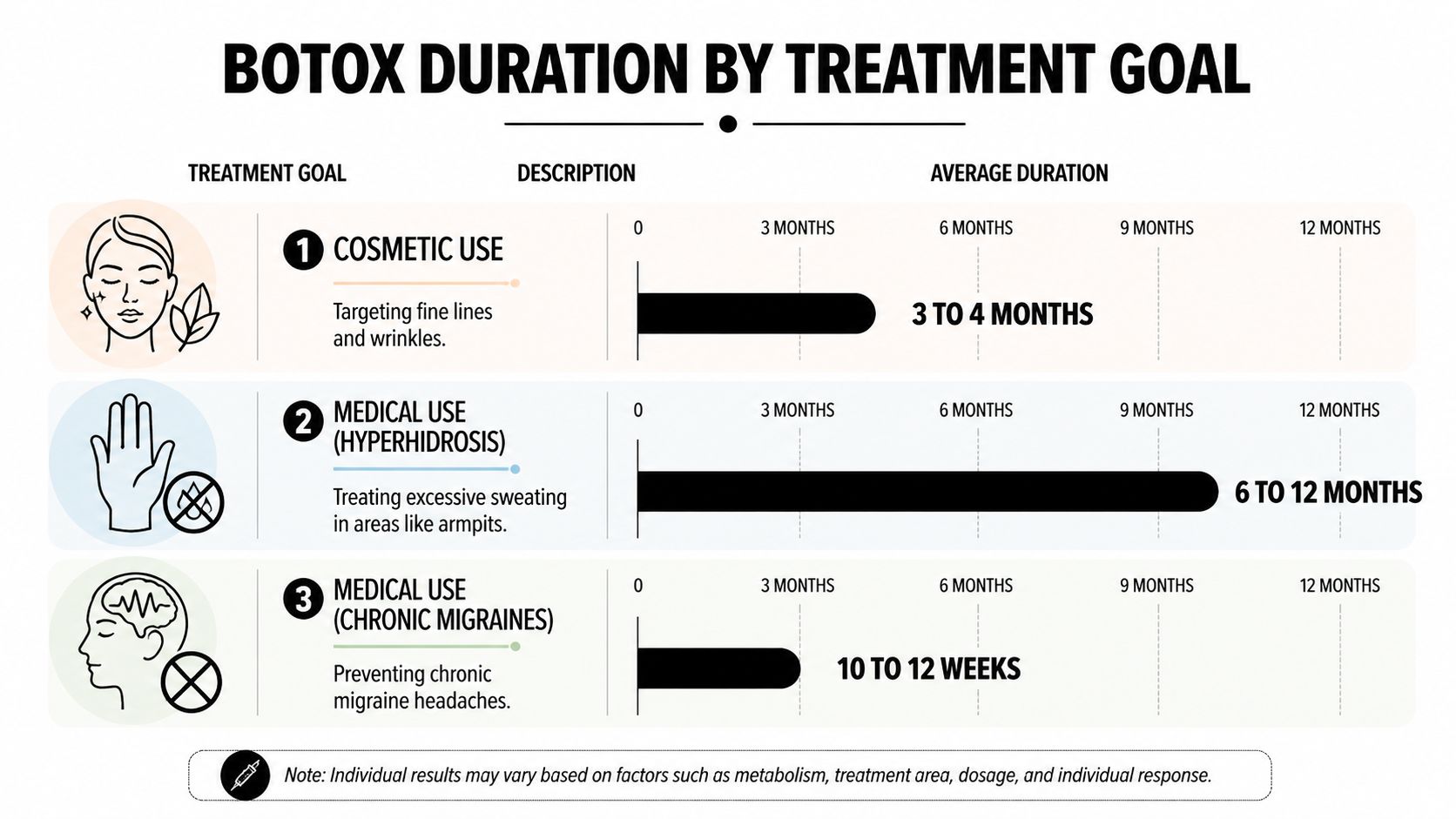
For aesthetic use, patients usually focus on visible movement and wrinkle softening. For chronic migraine, the question is whether headache burden comes down enough to improve life. For cervical dystonia, the focus is usually on abnormal muscle contraction, posture, tightness, and pain. Same drug family. Different use patterns.
A side by side view
| Use Case | Typical Duration | Governed By |
|---|---|---|
| Cosmetic facial treatment | 3 to 4 months | Muscle activity, treatment area, dose |
| Chronic migraine | Approximately 12 weeks | FDA-approved dosing protocol |
| Cervical dystonia | Often around the same medical interval, but individualized | Muscle pattern, severity, dosing plan |
For migraine care, Botox’s effects are governed by FDA-approved dosing protocols such as 155 to 195 units, designed to last approximately 12 weeks, as noted in this medical review of Botox duration and therapeutic dosing.
Cosmetic treatment as a reference point
Cosmetic Botox often lasts 3 to 4 months in common facial areas. Some areas hold results more predictably than others because muscles move differently throughout the day. That’s useful context, but cosmetic experience can mislead medical patients if it’s treated as a direct comparison.
For example, someone may say their forehead Botox lasted a certain amount of time and assume migraine treatment should feel exactly the same. It won’t. The injection pattern, dose, and therapeutic target are not the same.
Chronic migraine follows a medical protocol
For chronic migraine, Botox is used on a structured schedule. The treatment interval is built around prevention, not rescue. Patients often notice that the treatment cycle matters as much as the individual appointment.
A few practical points help set expectations:
- The target is prevention: The goal is not to stop one active headache in the room. It’s to reduce the burden of future attacks.
- The schedule is deliberate: Medical Botox for migraine is planned around an approximately 12-week interval, not around waiting until symptoms return fully.
- The response can build: Some patients judge the first cycle too quickly. In migraine care, consistency often gives a clearer picture than a one-time snapshot.
Cervical dystonia is individualized
Cervical dystonia also tends to be treated on a recurring schedule, but this condition is often more customized from patient to patient. The exact muscles involved can differ. The amount of abnormal contraction differs. So does posture, pain pattern, and how strongly the muscles are recruiting.
That means two people with the same diagnosis may have very different treatment maps. One may experience relief that feels broad and obvious. Another may feel improvement in rotation, head tilt, or muscle pulling before they notice pain reduction.
If you’re comparing your response to someone else’s, compare the diagnosis and treatment goal first. The timeline only makes sense in that clinical context.
Patients who are exploring whether Botox fits into a broader pain plan for migraine, neck pain, or related conditions can review the conditions treated in pain management practice.
The trade-off patients should know
Longer-lasting isn’t the only measure of success. In pain medicine, the better question is whether the treatment gives enough reliable relief to justify repeating it on schedule. A treatment that predictably reduces symptom burden for a known interval can be very useful, even if it isn’t permanent.
That’s why Botox remains part of medical care for selected patients. It offers a temporary effect, but a temporary effect on a repeatable cycle can still create meaningful stability.
Why Your Botox Timeline Might Be Different
Two patients can receive Botox for similar complaints and still have different timelines. That doesn’t automatically mean one treatment was done correctly and the other wasn’t. It usually means the body, the muscles, and the treatment plan aren’t identical.

Metabolism changes the pace
Some people process medications faster than others. With Botox, a faster metabolic pace can shorten how long the effect feels noticeable. Patients don’t usually experience that as a dramatic difference on day one. They notice it later, when symptoms start creeping back earlier than expected.
This is one reason online comparisons aren’t very helpful. If a friend says Botox lasted longer for them, that may say more about their physiology than about your result.
Muscle strength matters
Stronger or more active muscles may push through the effect sooner. That’s especially relevant when the treated muscles are used constantly or contract forcefully.
In cosmetic care, highly expressive areas can wear off faster. In pain care, heavily recruited neck muscles or longstanding spasm patterns may also influence how durable the effect feels. The muscle isn’t “resistant” in a simple sense. It may just need a carefully calibrated treatment plan.
Dose and injection pattern shape the result
Botox is not a one-size-fits-all procedure. Dose matters. Placement matters. The muscle selection matters.
For chronic migraine, medical protocols help standardize treatment. For cervical dystonia, the injector often has to map treatment more individually based on exam findings. If the wrong muscles are emphasized, or if the dose isn’t matched well to the pattern of contraction, the duration can feel shorter or less complete.
First treatment versus repeat treatment
First-time patients sometimes expect a perfect, long-lasting result immediately. In real practice, repeat treatment can produce a more stable rhythm over time because clinicians have more information about how your body responded and which muscles mattered most.
A few patterns are common:
- Early treatments can be more revealing than dramatic: The first session often shows how your body responds and where refinement may help.
- Follow-up planning improves precision: Symptom diaries and return visits help guide future dosing and muscle selection.
- Consistency often helps: Patients who stay on an appropriate schedule usually get a clearer sense of what the treatment can realistically deliver.
One Botox cycle is useful information. It isn’t always the final verdict.
Treatment area also changes the timeline
Not every area behaves the same way. Facial zones with repeated movement may fade sooner than less active areas. In medical treatment, the same principle applies. A muscle group under constant daily demand may not feel identical to one that is recruited less aggressively.
That’s why the answer to how long does Botox last has to be individualized after the average is stated. Three to four months is a solid benchmark. It is not a guarantee for every person, every muscle, and every diagnosis.
Planning Your Treatment Schedule for Lasting Relief
A patient from Oak Lawn gets meaningful migraine relief after Botox, then waits until the headaches are back almost every day before calling to schedule the next visit. By the time insurance is cleared and the appointment arrives, the pain pattern is fully active again. That cycle is frustrating and avoidable.
Medical Botox works best when treatment is planned as an ongoing rhythm. For chronic migraine and cervical dystonia, the practical question is not only how long one round lasts. The better question is when to schedule the next round so pain control stays as steady as possible.
The usual treatment arc
After injections, benefit does not show up all at once. Early changes may start within several days, but the effect usually becomes clearer over the first one to two weeks. From there, relief often holds for a few months and then fades gradually rather than stopping on a single date.
That gradual taper matters. Patients sometimes assume they should wait until the treatment has completely worn off. In pain practice, that approach often leads to more bad days, more rescue medication, and a harder reset.
Why repeat treatment is usually scheduled on a set interval
For chronic migraine, Botox is commonly given about every 12 weeks. That schedule reflects how the treatment is used in real medical care, not cosmetic convenience. For cervical dystonia, the interval is also often around 12 weeks, although some patients need adjustment based on response, muscle pattern, side effects, and insurance rules.
The goal is to prevent a full rebound of symptoms.
In my practice, patients usually do better when we review how long relief was meaningful, when function started slipping, and whether the return was gradual or abrupt. That information helps determine whether the next cycle should stay on the same timetable or be discussed more carefully within the limits of standard dosing intervals.
What this means for migraine and cervical dystonia
For migraine, the schedule should match the pattern of headache control. A patient may still have some benefit at week 10 or 11, but if headache frequency is climbing, sleep is worsening, and rescue medication use is increasing, the cycle is already turning.
Cervical dystonia has a similar pattern, but patients often notice it through function before pain alone. The neck may start pulling again during driving, computer work, reading, or sleep. Once that tightening is firmly back, daily life gets harder fast.
This is one reason symptom memory is unreliable. People remember the bad flare, but not always the week when control first started slipping.
How to plan practically
Set the follow-up before leaving the office. In the Chicago suburbs, delays often come from work schedules, school pickups, winter weather, transportation, or prior authorization. Waiting until the last good week creates unnecessary gaps.
A simple tracking plan helps:
- Record the first signs of return: For migraine, note headache days, light sensitivity, nausea, and rescue medication use. For cervical dystonia, note pulling, spasm, head position, and pain with activity.
- Track function: Write down what changed at work, during driving, while reading, or during sleep.
- Bring the pattern to follow-up: A short diary is more useful than trying to recall three months from memory.
- Plan around real life: If you know travel, a busy work stretch, or insurance renewal is coming, schedule early enough to avoid a lapse.
A good schedule does not make Botox last forever. It does make relief more predictable, which is often what patients in Orland Park, Oak Lawn, and nearby communities need most when they are trying to reduce pain days without relying on opioids.
Tips to Maximize the Longevity of Your Botox Treatment
A common scenario in clinic goes like this: a patient gets meaningful relief for migraine or neck spasm, then assumes the next cycle should work the same even if sleep worsens, trigger exposure rises, home exercises stop, or follow-up gets delayed. Botox still has a biologic time limit, but the quality of those weeks often depends on what happens between injection visits.

What actually helps
Good results come from protecting the treatment window and supporting the condition Botox is being used to treat.
- Follow the specific aftercare you were given: For the first day, avoid rubbing or pressing on treated areas and avoid activity your clinician asked you to postpone. That advice matters more for medical injections than many patients realize because injection sites and muscle targets are chosen for function, not appearance.
- Keep the next cycle on time: In pain medicine, late treatment often means symptoms re-establish themselves before the next session. Once migraine frequency climbs again, or once dystonic pulling becomes the new daily baseline, it can take more effort to get back to prior control.
- Use condition-specific support between visits: For chronic migraine, that usually means regular sleep, hydration, and active trigger management. For cervical dystonia, it often means a physical therapy program focused on posture, scapular control, range of motion, and reducing compensatory muscle strain. Botox can calm overactive muscles. It does not retrain mechanics by itself.
- Bring useful follow-up details: A short note on headache days, rescue medication use, neck pulling, head position, and activity limits helps your clinician decide whether dose, injection pattern, or muscle selection needs adjustment.
Small details matter here.
For cervical dystonia, I often see better durability when patients continue the exercises that reduce secondary muscle overload instead of waiting for tightness to return. For migraine, patients who identify their repeat triggers early often preserve more good days across the cycle than patients who only judge success by whether a severe flare happened.
What tends to shorten the benefit
Repeatedly testing the treated muscles, aggressive self-massage, or chasing cosmetic internet advice does not extend a medical Botox response. It usually adds irritation or confusion.
Another problem is under-treating the rest of the pain picture. If neck posture, poor workstation setup, medication overuse headache, fragmented sleep, or untreated stress patterns are driving symptoms, Botox may still help, but it has to work against more background noise. Patients then feel the treatment "wore off early" when the problem is that the underlying condition was never being managed by Botox alone.
The best long-term strategy
Botox lasts best in a plan that matches the diagnosis. For migraine, that may include trigger control, preventive medication review, and rescue medication limits. For cervical dystonia, it may include physical therapy, activity modification, and periodic reassessment of which muscles are causing the problem that cycle.
At Midwest Pain & Wellness, Botox may be used as one part of an opioid-sparing pain strategy for selected patients in Oak Lawn, Orland Park, and nearby communities. The goal is not to chase a perfect three-month block every time. The goal is to make relief more durable, more functional, and easier to repeat.
Good Botox outcomes come from the right diagnosis, the right muscle targets, the right dose, and follow-up that reflects how the patient is actually functioning.
Shortcuts do not make Botox last longer. A precise treatment plan often does.
Frequently Asked Questions About Medical Botox
Is medical Botox safe
Botox is a well-established treatment, but safe use depends on proper patient selection, diagnosis, dosing, and injection technique. That’s especially important in pain medicine, where the issue isn’t just softening movement. It’s targeting the right muscles for the right reason.
Patients should review their full medical history, medication list, and symptom pattern with the treating clinician. If something doesn’t fit, that matters before the injection, not after.
What side effects should I expect
Side effects depend on the condition being treated and the area injected. In general, patients may notice temporary soreness, localized discomfort, or temporary weakness in treated muscles. The practical question is whether the expected benefit outweighs the expected trade-offs for that specific diagnosis.
For cervical dystonia in particular, this balance needs individualized discussion because reducing overactive muscles can help, but muscle response can vary. That’s why follow-up matters.
Is medical Botox the same as cosmetic Botox
It’s the same general medication class, but the treatment plan is different. Cosmetic treatment focuses on appearance. Medical Botox focuses on symptom control and function.
That difference affects almost everything:
- The goal differs: Fewer migraine attacks or less neck spasm is not the same endpoint as smoother skin.
- The injection map differs: Medical treatment follows a therapeutic pattern, not an aesthetic one.
- The follow-up differs: Pain treatment often depends more heavily on symptom tracking and repeat scheduling.
Will insurance cover Botox for migraine or cervical dystonia
Coverage depends on your diagnosis, plan rules, prior treatment history, and documentation requirements. Some patients need prior authorization. Others may need to show that more conservative therapies were tried first.
The best approach is practical. Ask the office what documentation is needed, what diagnosis criteria apply, and what your insurer typically requires. Don’t assume coverage, but don’t assume denial either.
What happens if I stop Botox treatments
Botox doesn’t create a permanent change in the underlying condition. If you stop treatment, the effect gradually wears off and muscle activity returns. That means symptoms may return toward their baseline pattern over time.
Stopping doesn’t usually create a rebound in the sense many patients fear. More often, the original problem becomes active again as the treatment fades.
How is Botox different from fillers
Fillers add volume. Botox reduces targeted muscle signaling. They solve different problems.
Confusion can arise as some patients hear “injectables” and lump them together. In pain medicine, Botox is used for neuromuscular effect, not for filling tissue.
Take the Next Step Toward Fewer Pain Days in Illinois
If you’ve been asking how long does Botox last, the practical answer is this: most patients can expect about 3 to 4 months of effect, and medical treatment for conditions like chronic migraine and cervical dystonia is commonly planned around a 12-week cycle. The more important point is that this timeline is predictable enough to build into a real treatment strategy.
For patients in Oak Lawn, Palos Hills, Palos Heights, Worth, Bridgeview, Hickory Hills, Alsip, Burbank, Evergreen Park, Orland Park, and nearby Illinois communities, that predictability matters. Chronic pain conditions disrupt work, sleep, concentration, family routines, and mood. A treatment doesn’t have to be permanent to be useful. It has to be appropriate, repeatable, and clinically worth continuing.
When it makes sense to get evaluated
Botox may be worth discussing if:
- Migraine has become chronic: Especially if headaches are frequent and preventive options need review.
- Neck muscles feel persistently tight or pull involuntarily: Cervical dystonia can be missed or mislabeled for too long.
- You want an opioid-sparing option: Botox can fit into a broader pain plan that emphasizes function rather than temporary masking.
- You need a clearer diagnosis: A specialist evaluation can help determine whether Botox is the right tool or whether another intervention makes more sense.
Why a personalized plan matters
The right question isn’t only whether Botox lasts. It’s whether it lasts long enough, works well enough, and fits well enough into your overall care plan to improve daily life.
That judgment should come from an actual medical evaluation, not from general online averages alone. Diagnosis, muscle pattern, symptom severity, prior treatment history, and function all shape whether Botox is a good fit.
If you’re ready to discuss chronic migraine, cervical dystonia, or another pain condition with an interventional pain specialist in Illinois, you can request an appointment with Dr. Yaw Donkoh and the Chicago Ridge team.
If you’re dealing with chronic migraine, neck spasm, or another persistent pain condition in Illinois, Midwest Pain & Wellness can help you evaluate whether medical Botox fits your treatment plan. A consultation can clarify the diagnosis, expected timeline, and whether a repeatable, opioid-sparing approach makes sense for your goals.



