Back pain often starts with a simple question that turns into a frustrating loop. You bend, lift, twist, sleep wrong, sit too long, or recover from an injury, and then the pain stays. An X-ray may look unrevealing. An MRI may show “changes,” but nobody explains whether those findings matter. You’re still hurting, still limited, and still unsure what the actual problem is.
That’s why learning how to diagnose back pain matters. A good diagnosis isn’t just a label. It guides what to treat, what to avoid, when imaging helps, when it misleads, and whether you need a pain specialist, urgent evaluation, or a surgical opinion.
Understanding the Back Pain Puzzle in Illinois
For many adults in Oak Lawn, Palos Hills, Palos Heights, Orland Park, Bridgeview, Hickory Hills, Alsip, Burbank, Worth, and Evergreen Park, the hardest part of back pain isn’t only the pain itself. It’s the uncertainty.

Back pain is common, but a clear diagnosis is often not. Only 10% of doctor visits for back pain result in a definitive diagnosis, which highlights how difficult accurate identification can be in routine care, according to back pain statistics reviewed here. That gap explains why many patients go from visit to visit hearing different possibilities without getting a confident answer.
Why diagnosis gets missed
The spine is mechanically complex. Muscles, discs, facet joints, sacroiliac joints, nerves, ligaments, posture, work demands, prior injuries, and stress can all influence symptoms. Two people can describe “low back pain” and have completely different pain generators.
Pain also doesn’t always line up neatly with a scan. Some patients have severe pain with relatively modest imaging findings. Others have striking MRI abnormalities and very little functional limitation. If a clinician treats the image instead of the patient, the diagnosis often goes sideways.
Practical rule: The goal isn’t to find any abnormality. The goal is to find the abnormality, movement pattern, nerve issue, or pain source that actually matches your symptoms and exam.
What a specialist is trying to solve
An interventional pain specialist approaches the problem differently from a general urgent care visit. The question isn’t just “Do you have back pain?” It’s more specific:
Where is the pain generator
Is it disc-related, joint-related, nerve-related, muscular, sacroiliac, post-surgical, or referred from somewhere else?What pattern does it follow
Does it worsen with standing, walking, bending, twisting, sitting, coughing, extension, or transitional movements?What is the safest next step
Observation, medication adjustment, selective imaging, diagnostic testing, injection-based confirmation, or a surgical referral?
That process matters because treatment should follow diagnosis, not guesswork. If you’re trying to understand your options for pain conditions treated in a Chicago Ridge interventional clinic, the first step is building the diagnosis the right way.
Your Story The Most Important Diagnostic Clue
The most useful part of a back pain evaluation usually happens before anyone orders a test. It starts when you describe what the pain feels like, how it began, what it interrupts, and what makes it change.

A rushed history leads to broad guesses. A detailed history often narrows the field quickly.
The details that actually matter
When a specialist asks you to describe the pain, the wording matters. “Sharp,” “burning,” “aching,” “pressure,” “electric,” or “stabbing” can point in different directions. So can the map of the pain.
Think through these points before your visit:
How it started
Did the pain begin after lifting, a fall, a work injury, a car accident, surgery, or without a clear trigger?Where it travels
Pain that stays in the low back suggests one set of possibilities. Pain that shoots into the buttock, thigh, calf, or foot raises different questions.What changes it
Pain that worsens with sitting can mean something different from pain that worsens with standing or walking. Pain during twisting is different from pain during extension.What time pattern it follows
Constant pain, morning stiffness, end-of-day worsening, pain that wakes you at night, or pain that flares only with certain activities all help shape the differential diagnosis.What it’s stopping you from doing
Can’t stand to cook, can’t drive, can’t work, can’t sleep flat, can’t put on shoes, can’t walk through a store, can’t lift your child. Functional loss often tells more than a pain score alone.
Why specialists ask so many follow-up questions
A back pain visit can feel oddly specific. You may be asked whether the pain gets worse when you cough, whether leaning forward helps, whether one side hurts more, or whether numbness appears before pain or after it.
Those questions aren’t filler. They help sort out common patterns such as nerve irritation, facet-mediated pain, sacroiliac joint dysfunction, muscular strain, vertebral compression fracture, or stenosis-like symptoms.
A careful history also helps avoid chasing the wrong finding. If an MRI later shows several age-related changes, your symptom pattern helps determine which finding is relevant and which one is background noise.
When the history is precise, imaging becomes a confirmation tool. When the history is vague, imaging often creates more confusion.
Why mood, stress, and work questions belong in a back pain visit
Patients are often surprised when a pain specialist asks about sleep, mood, fear of movement, job stress, compensation issues, or ongoing legal claims. Some worry the doctor is implying the pain is “just stress.” That isn’t the point.
Multidimensional pain assessments that combine pain scores, function scales, and psychological screening improve treatment planning and outcomes in chronic low back pain, and factors such as kinesiophobia, catastrophizing, or depression can amplify pain perception, as described in this review on chronic low back pain assessment.
That matters in real practice. A patient with a modest mechanical issue can become severely limited if every movement is feared. A workers’ compensation patient may have true structural pain plus anxiety about returning to a physically demanding job. A person recovering from an injury may guard so much that secondary pain patterns develop around the original problem.
What to bring to the visit
A short written summary helps more than is often realized.
Bring a symptom timeline
List when the pain started, what happened around that time, and what has changed since.List prior treatments
Include medications, injections, chiropractic care, urgent care visits, surgery, therapy, and what each one did or didn’t change.Note your function
Write down three daily activities the pain is limiting right now.Bring prior imaging reports
If you already had X-rays, MRI, CT, or EMG testing, bring the reports and images if available.
If you want to understand how a specialist with this kind of diagnostic approach evaluates complex spine and nerve pain, you can review Dr. Donkoh’s clinical background and interventional focus.
Recognizing Back Pain Red Flags Without Panic
Most back pain is not an emergency. That’s reassuring, but it shouldn’t lead to complacency. Some symptom clusters do need urgent attention. The key word is clusters.
A major mistake in back pain care is overreacting to one isolated feature while ignoring the full clinical picture. A systematic review found that individual red flags have limited standalone diagnostic accuracy, and the likelihood of serious pathology rises much more when multiple red flag criteria occur together, as summarized in the NCBI review on back pain evaluation.
What red flags actually mean
“Red flag” doesn’t mean diagnosis. It means a sign that raises concern and changes how carefully and how quickly the patient should be assessed.
Examples can include severe trauma, major neurologic change, signs of infection, possible cancer-related symptoms, or bowel and bladder dysfunction. But one item by itself can be misleading. Age alone is not a diagnosis. Recent minor strain isn’t the same as major trauma. A single vague symptom rarely settles the issue.
That’s why a specialist looks at timing, severity, progression, exam findings, medical history, and combinations of symptoms before deciding on urgent imaging or referral.
When to seek care
| Symptom | What It Could Mean | Action to Take |
|---|---|---|
| New loss of bladder or bowel control with back pain | Possible severe nerve compression affecting the lower spinal canal | Go to the ER immediately |
| Rapidly worsening leg weakness | Progressive neurologic compromise | Go to the ER immediately |
| Back pain after major trauma | Possible fracture or structural injury | Seek emergency evaluation |
| Fever with significant back pain, especially if you also feel ill | Possible infection | Call urgently and seek same-day medical evaluation |
| Unexplained weight loss with persistent back pain | Possible systemic illness requiring prompt workup | Call the clinic or your physician promptly |
| New numbness in the groin or saddle area | Possible severe nerve involvement | Go to the ER immediately |
| Back pain with a history of cancer and changing symptoms | Possible metastatic or related spinal involvement | Call urgently for prompt evaluation |
| Pain that is progressing despite rest and routine care, especially with neurologic symptoms | May need expedited imaging or specialist assessment | Call the clinic promptly |
What usually doesn’t require panic
Many people worry that severe pain automatically means severe damage. It doesn’t. Pain intensity alone can be dramatic even when the underlying issue is not dangerous. Muscle spasm, acute disc irritation, and inflamed joints can all be intensely painful.
The opposite is also true. Some serious conditions don’t announce themselves with dramatic pain at first. That’s why pattern recognition matters more than trying to rank pain on a simple scale.
A useful question is not “Is this pain bad?” It’s “Is this pain changing along with weakness, numbness, bladder symptoms, fever, or other concerning features?”
Why false positives matter
If clinicians react to every isolated red flag with reflexive imaging, many patients get pulled into unnecessary tests and procedures. That creates anxiety and can steer treatment toward findings that don’t actually explain the pain.
A careful clinician tries to avoid both errors. Missing serious pathology is dangerous. Overcalling routine findings is also harmful. Good triage requires calm judgment, not alarm.
For patients in Hickory Hills, Alsip, Bridgeview, and nearby Illinois communities, that often means calling for guidance when symptoms change instead of guessing, waiting too long, or assuming every flare requires an ER visit.
What to Expect During a Focused Back Pain Exam
A good back exam is not a ceremonial stop before imaging. It’s where the diagnosis starts becoming objective.
Without proper diagnosis, 31% of people with back pain fail to recover fully within six months, and a step-wise approach that includes a hands-on physical examination with neurological evaluation is critical for diagnostic precision, according to this overview of back pain diagnosis and recovery.
First impressions matter
The exam often starts before you’re on the table. A clinician watches how you stand up, how you walk, whether you lean to one side, whether your stride is guarded, and whether changing positions clearly aggravates symptoms.
Those observations matter. A patient who can sit comfortably but has pain with extension gives a different clue than one who struggles to sit and keeps shifting weight off one side. The way you move often reveals more than a static pain rating.
What the hands-on exam is looking for
The physical exam usually includes several layers:
Inspection and posture
Is there spinal asymmetry, protective leaning, loss of normal curve, or visible guarding?Palpation
The doctor checks for tenderness, muscle spasm, trigger points, and whether the pain is centralized or off to one side.Range of motion
Bending forward, leaning backward, and rotating can reproduce different pain patterns. Flexion-dominant pain and extension-dominant pain don’t suggest the same structures.Neurological testing
Reflexes, muscle strength, and sensation help determine whether a spinal nerve may be irritated or compressed.
Special maneuvers that help narrow the cause
Some tests sound technical, but the ideas are simple. The exam tries to reproduce your pain in a controlled way so the doctor can identify the likely source.
The straight-leg-raising test is a common example. In the review cited earlier, it’s considered positive if lifting the straightened leg causes ipsilateral leg pain below 60°. That pattern can support suspicion for lumbar nerve root irritation.
The crossed straight-leg-raising test is often more specific for disc herniation. The Stork test can help in selected cases when spondylolysis is a concern.
If a movement reproduces your usual pain in a predictable pattern, that finding is useful. If it only causes general tightness that feels unrelated to your usual symptoms, it may not be diagnostically meaningful.
Why the exam still matters even if you already had imaging
A scan can show anatomy. It doesn’t show which structure hurts when you bend, which movement compresses a nerve, or whether the symptoms follow a nerve distribution.
That’s why two patients with similar MRI findings can need completely different treatment plans. One may have pain from a facet joint pattern. Another may have radicular symptoms from a disc issue. Another may have mostly muscular overload with no procedure needed at all.
What patients should do during the exam
Try not to minimize or exaggerate. The exam works best when you describe what you feel.
A few simple habits help:
Point with one finger if you can
Diffuse pain descriptions are common, but the most intense focal area is often informative.Say whether the maneuver reproduces your usual pain
“That’s my exact pain” means more than “I feel stretching.”Mention numbness, tingling, or weakness clearly
These symptoms change the differential diagnosis.Tell the doctor if a movement causes delayed pain afterward
Some provocative movements don’t peak until minutes later.
A focused exam doesn’t solve every case on the spot, but it usually identifies whether the next step should be watchful care, imaging, electrodiagnostic testing, or a targeted diagnostic procedure.
When Imaging Helps and When It Hinders Your Diagnosis
Many patients assume the fastest path to an answer is an MRI. That’s understandable. If your back hurts, you want a picture. But in non-emergent back pain, that instinct can lead to confusion.
Evidence-based guidelines emphasize that routine early MRI in chronic low back pain without red flags is associated with higher rates of unnecessary interventions without better long-term outcomes, and many spinal abnormalities are also common in people without pain, as discussed in this evidence review on imaging for low back pain.
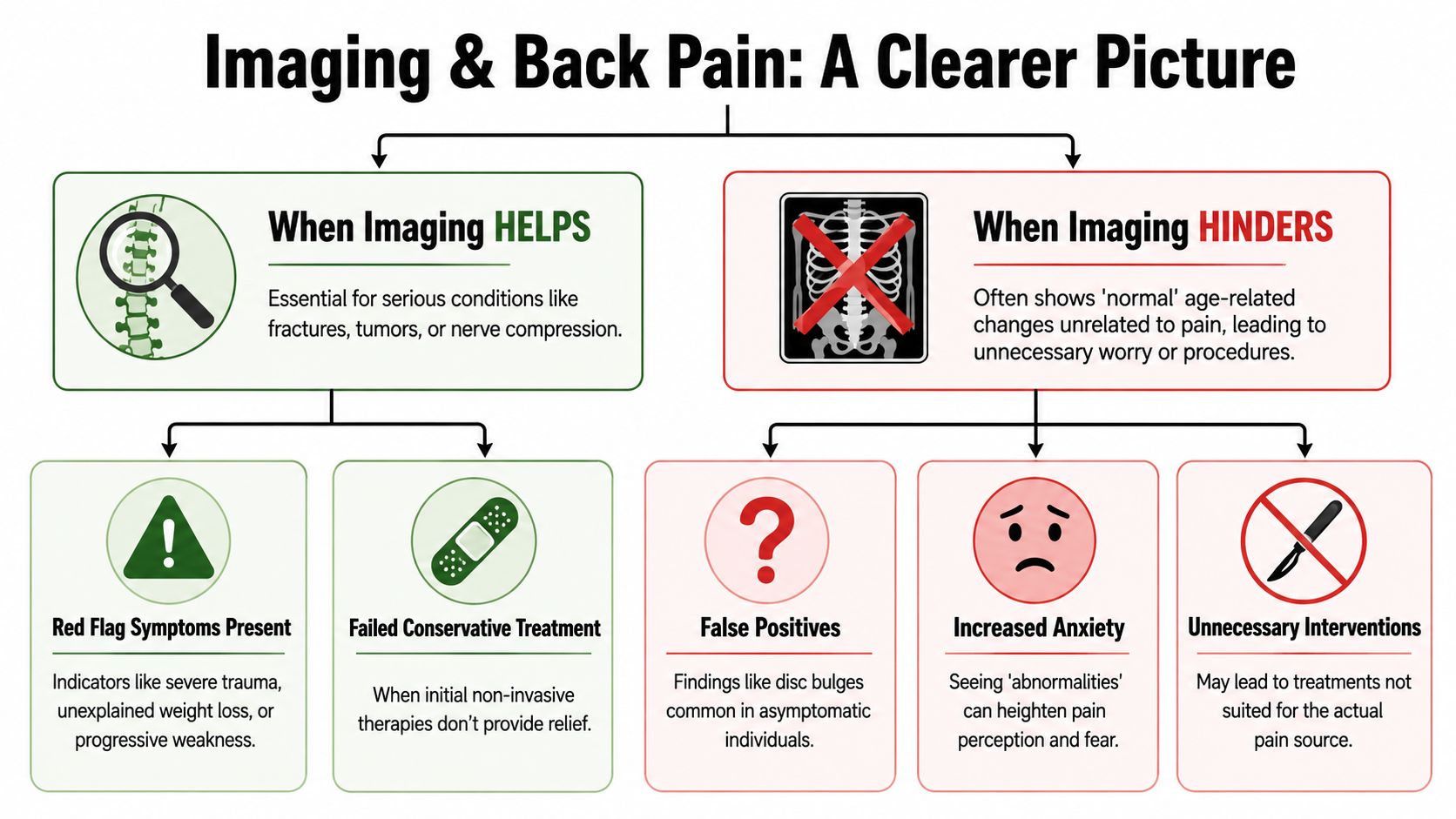
When imaging helps
Imaging is valuable when the clinical question is clear.
A scan can be useful when:
Red flag symptoms are present
Imaging may help identify fracture, infection, tumor, or significant nerve compression.Symptoms persist despite appropriate early care
If pain remains disabling, the exam and history may justify MRI or another study to clarify the next step.A procedure is being planned
Imaging helps confirm anatomy before targeted interventions.The neurologic picture needs clarification
Progressive weakness, significant sensory change, or other objective findings may warrant imaging sooner.
When imaging hinders
Imaging becomes a problem when it’s used as a fishing expedition. The spine ages like every other part of the body. Disc bulges, degenerative changes, and arthritic findings may appear on imaging even when they aren’t the source of pain.
That’s why a “normal X-ray” doesn’t mean nothing is wrong, and an “abnormal MRI” doesn’t prove that every visible change needs treatment.
The best use of imaging is to answer a focused question that came from the history and exam. It should confirm a suspected diagnosis, not replace clinical thinking.
If my MRI is normal, why do I still hurt
This is one of the most common and reasonable questions in pain medicine.
Pain can persist even when imaging doesn’t show a dramatic structural lesion. Several possibilities can explain that mismatch:
The painful structure may be difficult to visualize well on routine imaging
Some pain generators are better identified by exam pattern or diagnostic injection than by static imaging alone.The problem may be functional rather than grossly structural
Movement-based pain, muscular guarding, sensitization, and biomechanical overload may not look dramatic on a scan.The imaging finding may not have been captured at the right level or in the right context
Static imaging doesn’t always reflect what happens under load, during walking, or during specific movements.
Other tests that can be more useful than repeating scans
When symptoms suggest nerve involvement, EMG and nerve conduction studies can help evaluate whether nerve damage or irritation is present. These tests don’t replace imaging, but they answer a different question. They help determine how nerves are functioning.
In interventional pain practice, diagnostic injections can be especially helpful. A medial branch block, for example, uses numbing medication to determine whether the facet joints are causing the pain. That can be far more actionable than a notation of “facet arthropathy” on a report.
An interventional clinic such as Midwest Pain & Wellness and its treatment procedures fits into the diagnostic pathway. The role is not to chase every MRI finding. It is to use the history, exam, selective imaging, and when appropriate, image-guided diagnostic procedures to identify the structure that matches the patient’s symptoms.
The real trade-off
Ordering imaging too early can feel thorough, but it often changes the conversation before the diagnosis is mature. Patients may become fixated on terms from the report. Referrers may feel pressure to react to findings that are incidental. Treatment can drift toward whatever looks abnormal rather than whatever is clinically relevant.
Selective imaging is slower than reflex imaging. It is also often more accurate.
From Diagnosis to a Personalized Relief Plan in the Chicago Area
Once the pain pattern is clear, treatment becomes more focused. At this point, diagnosis starts paying off.
Not all back pain needs the same plan. A patient with classic radicular symptoms and concordant neurologic findings may need a very different pathway from someone whose pain is mainly extension-based and centered over the facet joints. Another patient may have sacroiliac joint pain after altered gait or prior lumbar surgery. Another may have vertebral compression fracture pain that requires an entirely different strategy.
Matching the diagnosis to the treatment
A few examples show why precision matters:
Disc-related nerve pain
If the story and exam suggest nerve root irritation, treatment may focus on reducing inflammation around the affected nerve, improving function, and watching for neurologic change.Facet-mediated pain
If pain is worse with standing upright, extension, or rotation, and the pattern fits the exam, diagnostic blocks may help confirm the source before longer-acting treatment is considered.Sacroiliac joint dysfunction
Pain below the beltline, asymmetric loading, or post-surgical biomechanical changes may point away from the lumbar discs and toward the SI joint.Compression fracture pain
A patient with sudden focal pain after strain or minor trauma, especially in the right clinical setting, may need a fracture workup rather than routine chronic low back care.
What an opioid-sparing plan usually looks like
A sound plan doesn’t jump straight to the most invasive option, and it doesn’t rely on opioids as the default answer. It usually combines several practical decisions:
Clarify the pain generator first
If the diagnosis is still fuzzy, the next step may be more exam-guided testing, not more medication.Use function as a treatment target
Sleeping better, walking farther, tolerating work duties, sitting through a drive, or climbing stairs often matters more than chasing a perfectly pain-free day.Layer care based on the diagnosis
That may include medication adjustments, activity guidance, targeted physical therapy, bracing in selected cases, image-guided injection therapy, nerve-focused procedures, or minimally invasive decompression when indicated.Escalate only when the findings support it
If the diagnosis points toward a surgical lesion, referral should be timely. If it doesn’t, surgery usually shouldn’t be pushed by an MRI report alone.
Good back pain care is not passive. It is selective. The most effective plan is the one that matches the actual pain generator and the patient’s functional goals.
When a pain specialist makes sense and when a surgeon should step in
Referral to an interventional pain specialist makes sense when the diagnosis is uncertain, when pain persists despite appropriate initial care, when imaging doesn’t match symptoms, when a patient needs diagnostic blocks or injections, or when the goal is to avoid unnecessary opioid escalation.
A surgical opinion becomes more important when there is progressive neurologic deficit, bowel or bladder compromise, structural instability, or a lesion that is clearly surgical based on the full clinical picture.
That distinction matters for patients across Worth, Evergreen Park, Chicago Ridge, Oak Lawn, and Orland Park. Many people don’t need surgery, but they do need a more precise diagnostic process than a routine “rest and wait” approach. Others do need expedited surgical review, and the key is identifying them early rather than after months of uncertainty.
A careful diagnosis won’t remove every ambiguity on day one. But it usually does something just as important. It gives you a rational next step.
If you’re dealing with ongoing back pain in the Chicago Ridge area and want a more precise, opioid-sparing evaluation, Midwest Pain & Wellness offers diagnostic assessment for spine, nerve, and injury-related pain, including interventional options when appropriate.