A sciatica flare often starts the same way. You bend to pick something up, stand after a long drive, or roll out of bed and feel a sharp, electric pain shoot from the low back into the buttock and down the leg. Walking feels awkward. Sitting feels worse. You start wondering whether you need an MRI, a chiropractor, an injection, surgery, or just a few days to let it calm down.
The right answer depends on why the nerve is irritated, how severe the symptoms are, and whether the problem is settling down or starting to affect strength and daily function. Knowing how to treat sciatica pain means following the problem in order. Start with safe self-care, get the right diagnosis if symptoms persist, and escalate only when the next step is justified.
At a pain and wellness clinic, that decision-making matters. Sciatica isn’t managed well by guessing, random stretches from the internet, or repeated rounds of medication without a plan. It improves most reliably when treatment matches the actual pain generator.
Understanding That Shocking Leg Pain Called Sciatica
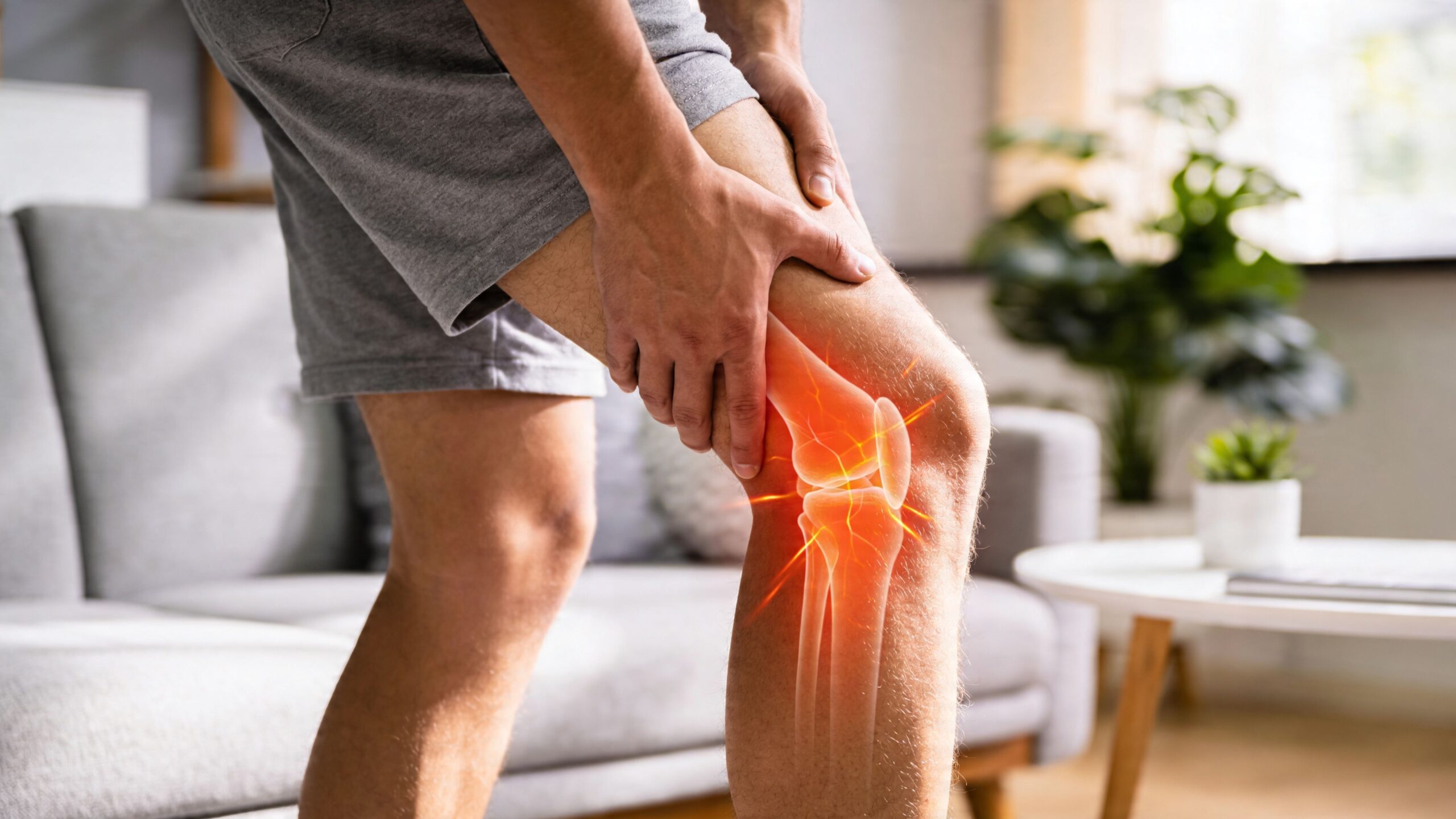
Sciatica is a symptom, not a final diagnosis. The term describes pain that travels along the sciatic nerve pathway, usually from the low back or buttock into the leg. That pain may feel burning, stabbing, aching, or electric. It can also come with tingling, numbness, or weakness.
The sciatic nerve is the large nerve formed by nerve roots in the lower spine. When one of those roots gets irritated or compressed, the brain reads it as pain traveling down the leg. That’s why sciatica feels different from ordinary back strain. Muscle pain tends to stay local. Nerve pain radiates.
What usually causes it
In practice, the most common culprits include a disc problem, spinal narrowing, or inflammation around a nerve root. Some patients have severe leg pain with only mild back pain. Others have both. The pattern matters.
A careful exam helps separate true nerve pain from hip pain, sacroiliac pain, knee pain, or muscular pain that only seems like sciatica. That distinction is important, because treatment changes based on the source. If you’re looking at the range of conditions that can mimic or contribute to leg pain, conditions we treat at Midwest Pain & Wellness include spine, nerve, and joint problems commonly mistaken for one another.
How common sciatica really is
Sciatica is common enough that most families have seen it up close. The lifetime incidence ranges from 10% to 40%, with an annual incidence of 1% to 5%. This commonality has driven a global treatment market valued at over USD 5 billion in 2024, with first-line treatments like NSAIDs holding a dominant 38.61% share, according to Grand View Research’s sciatica treatment market analysis.
Sciatica isn’t rare, and it isn’t something you should just “push through” if the pain is tracking down the leg and interfering with sleep, walking, or work.
What helps most patients is not panic and not neglect. It’s a structured approach.
Your First Moves When Sciatica Strikes
The first question is simple. Is this a routine flare that can be watched closely, or is it an emergency?
Go to urgent care or the ER if these red flags appear
- Loss of bladder or bowel control suggests a serious nerve compression problem that needs immediate medical attention.
- Progressive weakness in the leg matters more than pain alone. If the leg is getting harder to lift, push off, or control, don’t wait it out.
- Rapidly worsening numbness in the groin or saddle area is another sign that needs urgent evaluation.
- Severe pain with fever, recent trauma, or a known cancer history also changes the picture and deserves prompt medical review.
This quick visual summarizes the first decision points.
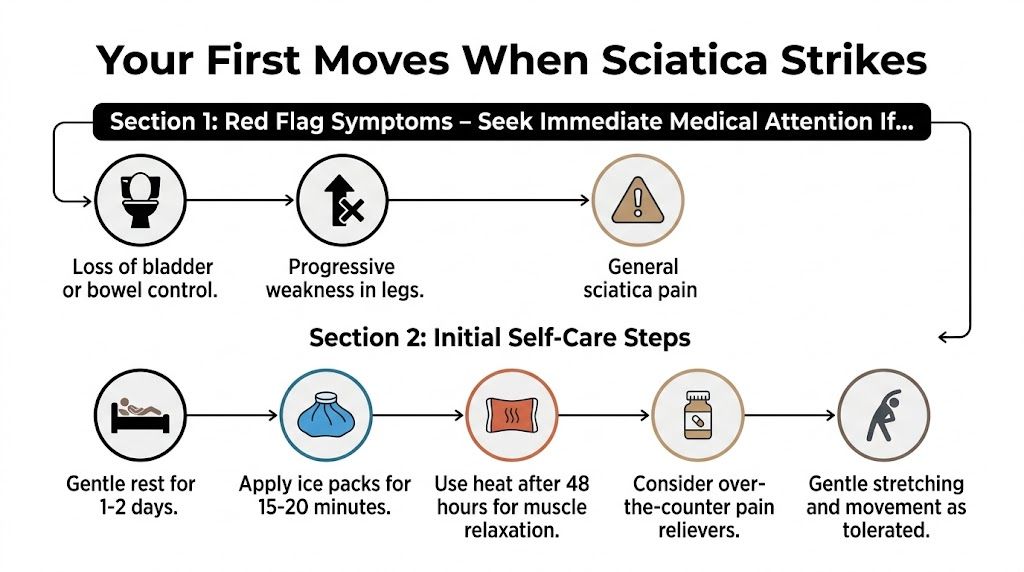
What to do in the first few days
If you don’t have red flags, start with relative rest, not bed rest. That means backing off from the movement that triggered the flare, but still walking short distances and changing position regularly. Staying in bed all day usually stiffens the back, tightens the hips, and keeps the nerve irritated.
Use a simple rhythm:
- Reduce aggravation
Avoid repeated bending, twisting, heavy lifting, and long periods in one position. - Keep gentle movement going
Short walks are often better tolerated than sitting. - Use cold first if the pain is acutely inflamed
Ice can calm an angry flare. - Use heat later if muscles start guarding
Heat often helps once the sharp inflammatory phase eases.
Ice, heat, and over-the-counter medication
Cold is usually more useful early when pain feels hot, sharp, and inflamed. Heat is often more comfortable when muscles in the low back and buttock have tightened up around the problem. Neither fixes the cause, but both can make the body easier to move.
For medication, many patients start with an over-the-counter anti-inflammatory if they can take one safely. That may help if inflammation around the nerve root is part of the problem. Follow label directions and be cautious if you have kidney disease, stomach ulcer history, are on blood thinners, or have been told to avoid NSAIDs.
Practical rule: If a medication takes the edge off but you still can’t sit, sleep, or walk normally after several days, it’s time to stop self-managing and get examined.
What not to do
A lot of bad advice sounds harmless. It isn’t.
- Don’t force aggressive hamstring stretching just because the leg feels tight. Nerves under tension often don’t like being yanked on.
- Don’t stay seated for hours with a heating pad and hope it disappears.
- Don’t start random online exercises before you know whether your symptoms prefer extension, flexion, or a different strategy.
- Don’t keep lifting at full effort through sharp radiating pain because you’re trying to stay tough.
A simple first-week checklist
| What to try | Why it helps | What to avoid |
|---|---|---|
| Short walks | Keeps the body moving without prolonged compression | Long periods of sitting |
| Ice early, heat later | Can reduce irritation or relax guarding muscles | Sleeping on a heating pad |
| OTC anti-inflammatory if appropriate | May reduce inflammatory pain | Taking more than directed |
| Position changes through the day | Reduces sustained pressure on the nerve | Bed rest for days |
If symptoms are easing, that’s encouraging. If they’re stalling, spreading, or making the leg feel less reliable, the next step is a proper diagnosis.
Professional Guidance and The Right Kind of Movement
One of the biggest mistakes patients make is assuming all stretching is good stretching. It isn’t. The right movement can calm a nerve down. The wrong movement can keep compressing or tensioning it. That’s why a professional exam matters before you commit to a home routine.
A pain specialist looks for more than pain severity. The pattern matters. Does the pain go below the knee? Is there numbness in the foot? Does coughing or sitting provoke it? Is there weakness? Does the pain “centralize,” meaning it retreats from the leg toward the back with certain positions?
Why diagnosis comes before exercise
A person with disc-related nerve irritation may improve with one category of movement, while another patient with spinal stenosis may feel worse with that same movement and better with a different strategy. If you skip that distinction, you can spend weeks doing exercises that reinforce the problem.
Prescription options can also fit here when over-the-counter care isn’t enough. Depending on the exam, a clinician may consider a short course of stronger anti-inflammatory treatment, a muscle relaxant if spasm is driving guarded movement, or a nerve pain medication in selected cases. These don’t replace rehab. They make rehab more tolerable.
The role of directional preference
A useful example is the McKenzie Method®, which uses repeated movement testing to identify whether a patient improves with a certain direction of motion. In acute discogenic sciatica, the McKenzie Method® can achieve significant relief in 70% to 80% of cases. If a patient’s pain centralizes during assessment, they have an 85% likelihood of avoiding injections, according to KC Rehab’s review of McKenzie-based sciatica treatment.
That doesn’t mean everyone should start doing extension exercises on their living room floor. It means assessment first, repetition second.
If pain moves out of the calf and back toward the buttock or low back during repeated testing, that’s usually a good sign. If it spreads farther down the leg, the movement is often wrong for that patient.
Movement that often helps
When the exam supports it, treatment usually focuses on reducing nerve irritation, restoring motion, and building enough core and hip control that the back isn’t repeatedly overloaded.
Common useful categories include:
- Repeated directional movements based on exam findings, often extension-based in disc-related cases
- Walking progression to improve tolerance without sustained sitting pressure
- Core stability work to improve spinal control
- Hip mobility and glute activation when pelvic mechanics are contributing
- Posture and body mechanics training for sitting, lifting, and transitions
Movement that often backfires
Many online treatment plans prove ineffective. Some patients worsen because they keep doing what feels like a “stretch” but is instead increasing neural tension or mechanical compression.
Be cautious with:
- Deep forward bends if sitting and flexion already worsen symptoms
- Aggressive toe-touch hamstring stretches
- Twisting stretches done into pain
- High-impact exercise during an active flare
- Ab workouts that load the spine aggressively before symptoms settle
What guided care should accomplish
A good conservative program should answer three practical questions.
| Question | What you want to see |
|---|---|
| Is pain centralizing or spreading? | Centralizing is generally more favorable |
| Is walking, sitting, or sleeping improving? | Function should trend in the right direction |
| Is strength stable? | No progression of weakness |
If pain remains severe despite well-chosen movement and medication support, or if the exam suggests a structural problem that may need a procedure, that’s when imaging becomes useful.
When Imaging is Needed to Plan Your Next Steps
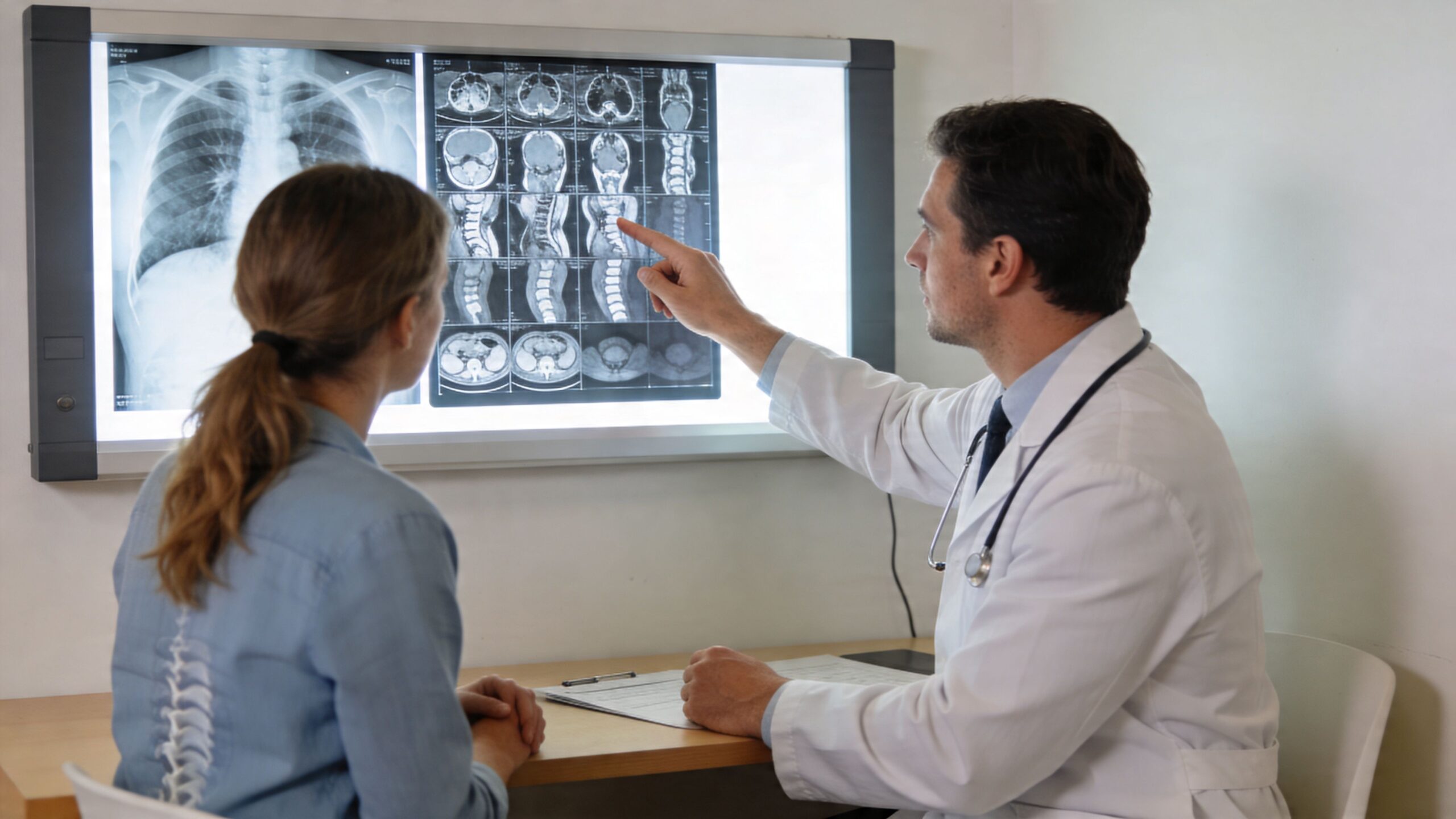
Many patients think the MRI is the diagnosis. It isn’t. An MRI is a tool. It shows structure. Your symptoms and exam show whether that structure is causing the pain.
That matters because spine imaging often reveals disc bulges, arthritis, and narrowing that may or may not be the actual problem. If the image doesn’t match the pain pattern, treating the picture instead of the patient can send care in the wrong direction.
When imaging makes sense
Imaging is usually most helpful when:
- Red flags are present
- Symptoms aren’t improving with conservative care
- There’s weakness, significant numbness, or persistent radiating pain
- An injection or procedure is being considered
- Surgery is on the table and a roadmap is needed
What imaging should answer
A well-timed MRI helps answer practical questions:
- Is there a disc herniation contacting the nerve root?
- Is the canal or foramen narrowed?
- Is one level more involved than another?
- Is there another explanation for the symptoms?
The image should support a treatment decision. If it won’t change the next step, it may not need to be the first step.
X-rays can help in selected cases, especially if alignment or bony change is part of the concern. MRI is usually more informative when true sciatic nerve symptoms are present and a procedural plan is being considered.
The important point is this. Imaging should clarify the target, not replace clinical judgment.
Advanced Interventional Pain Treatments
When sciatica doesn’t respond well enough to time, activity modification, medication, and guided rehabilitation, interventional treatment can help by targeting the source of pain more directly. In such cases, an interventional pain specialist adds a different layer of care than a general musculoskeletal approach.
The goal isn’t to “jump to procedures.” The goal is to use the least invasive treatment that meaningfully improves pain and function.
A useful overview of these options appears on procedures used for treatment at Midwest Pain & Wellness, including image-guided injections, radiofrequency techniques, spinal cord stimulation, and minimally invasive lumbar procedures.
Epidural steroid injections
For true radicular pain from an irritated lumbar nerve root, an epidural steroid injection is often the most direct non-surgical option. The medication is placed near the inflamed nerve root under imaging guidance.
This treatment is best suited for pain that radiates down the leg in a nerve pattern, especially when sitting, bending, coughing, or walking provoke symptoms and conservative care hasn’t created enough progress. The goal is to reduce inflammation around the nerve so the patient can move, sleep, and participate in rehab more effectively.
What it is not. It’s not rebuilding the disc. It’s not guaranteed permanent relief. It’s a targeted anti-inflammatory treatment meant to create a better recovery window.
Medial branch blocks and radiofrequency ablation
Not every patient with “sciatica” has pain primarily coming from a pinched nerve root. Some have a mixed picture that includes facet-mediated back pain, which can trigger referral into the buttock or upper leg and complicate recovery.
A medial branch block is a diagnostic injection used to test whether the facet joints are major pain generators. If that pattern is confirmed, radiofrequency ablation, often shortened to RFA, can interrupt pain signaling from those nerves for a longer period.
This is usually a better fit for mechanical back pain with extension or rotation sensitivity than for classic calf-to-foot nerve pain from a disc herniation. In the right patient, though, it can remove a major source of back pain that keeps aggravating the whole pain cycle.
Spinal cord stimulation
For persistent nerve pain that doesn’t respond to simpler measures, especially after prior spine surgery or in chronic radicular pain states, spinal cord stimulation may be considered. This involves placing leads that deliver electrical signals to alter how pain is processed.
It isn’t a first-line treatment for an early sciatica flare. It belongs later in the pathway, after careful diagnosis and after simpler options have been considered or tried. The right candidate usually has ongoing functional limitation, significant chronic nerve pain, and a pattern that fits neuromodulation.
MILD and Vertiflex for lumbar stenosis
Some patients use the word sciatica for leg pain that is caused by lumbar spinal stenosis, especially when symptoms worsen with standing and walking and improve with sitting or forward bending. In that setting, the treatment pathway can be different.
Two minimally invasive options that may be considered in selected patients are MILD and Vertiflex Superion.
- MILD is a minimally invasive lumbar decompression procedure intended to reduce tissue crowding that contributes to central canal narrowing.
- Vertiflex is an interspinous spacer procedure designed to create more room in specific stenosis patterns.
These options are not interchangeable with epidural injections or RFA. They’re used when anatomy, symptoms, and prior treatment response point toward stenosis as the key problem.
Regenerative options such as PRP
In selected cases, regenerative approaches such as PRP may be discussed as part of a broader treatment plan. These are not standard answers for every sciatic presentation. They may be considered when tissue quality, inflammation, and mechanical pain generators suggest a possible role.
The important point is patient selection. A regenerative procedure doesn’t make sense just because a patient wants to avoid surgery. It has to match the diagnosis.
Comparing Interventional Sciatica Treatments
| Treatment | Primary Goal | Best For | Typical Duration of Relief |
|---|---|---|---|
| Epidural steroid injection | Reduce inflammation around an irritated nerve root | Radiating leg pain from nerve root irritation | Varies by patient |
| Medial branch block | Diagnose facet-related pain | Suspected facet-mediated back pain with referral | Short diagnostic window |
| Radiofrequency ablation | Interrupt pain signaling from facet nerves | Confirmed facet pain contributing to function loss | Longer-lasting, varies by patient |
| Spinal cord stimulation | Modulate chronic pain signaling | Persistent nerve pain, often after failed simpler options | Ongoing therapy with device support |
| MILD | Decompress stenotic tissue | Selected lumbar spinal stenosis cases | Varies by anatomy and patient |
| Vertiflex | Create space in stenotic segments | Selected stenosis patterns with neurogenic symptoms | Varies by anatomy and patient |
| PRP | Support a regenerative treatment strategy | Carefully selected cases | Varies by indication |
How interventional care fits the journey
The right procedure should do at least one of three things:
- Calm inflammation so rehab becomes possible.
- Identify the pain generator when the diagnosis is still mixed.
- Improve function enough to delay, reduce, or avoid larger surgery.
A poor procedural plan usually looks like repeated injections without a clear diagnosis, or jumping into an intervention that doesn’t match the symptom pattern. A strong plan is specific. It ties the history, exam, imaging, and function together.
Procedures work best when they’re part of a broader strategy that includes movement correction, pacing, and a realistic plan for returning to work, exercise, and daily activity.
Considering Surgery and Focusing on Functional Recovery
Surgery has an important role in sciatica care. It’s just not the first answer for most patients. If there is progressive neurologic deficit, intractable pain despite appropriate treatment, or a structural problem that clearly matches the symptoms and isn’t improving, a surgical consultation may be the right move.
The key is to view surgery as one tool for the right problem, not as proof that earlier care failed. Some patients need decompression. Some do better without it. The decision should come from the full picture, not fear.
What outcomes really tell us
There’s a reason clinicians usually start with conservative care. Conservative sciatica treatments can have cure rates over 75%, while surgical outcomes vary. At 12 months, the SPORT trial found 77.1% satisfaction in a surgical group versus 44.7% in a non-surgical group for specific metrics, yet no difference in overall physical functioning, according to the NCBI Bookshelf review on sciatica management.
That’s a useful reminder. Surgery may improve selected outcomes, especially leg pain for the right patient, but it doesn’t automatically solve every aspect of disability or back pain.
Recovery means more than pain scores
Even when surgery is appropriate, the primary target is functional recovery. Can you walk farther, sleep better, sit through work, lift safely, and trust the leg again? Those questions matter more than whether the pain score dropped a few points for a week.
Interventional pain care can still matter before surgery, while a patient is deciding, or after surgery if residual pain remains. In many cases, coordinated care helps patients move from crisis mode into a more stable recovery plan with clearer expectations and fewer medication detours.
A good treatment pathway keeps asking the same question. What helps this patient function better with the least necessary intervention?
Your Next Step Toward Sciatica Relief in Illinois
If you’re dealing with sciatica in Oak Lawn, Palos Hills, Palos Heights, Worth, Bridgeview, Hickory Hills, Alsip, Burbank, Evergreen Park, Orland Park, or nearby Illinois communities, the next step should be specific. Get the pain pattern examined, determine whether the issue is disc-related, stenotic, joint-related, or mixed, and choose treatment based on that finding.
This matters even more for workers’ compensation and personal injury cases. People in physically demanding jobs often need more than short-term pain relief. They need a plan that supports safe return to activity and lowers the chance of repeated setbacks. For patients in physically demanding jobs, specialized interventional plans that combine targeted procedures with physical therapy can reduce injury recidivism by up to 45% compared to conservative care alone, according to Cleveland Clinic-related reference material provided in the verified data.
That’s one reason recurrence prevention matters as much as acute relief. Work demands, lifting mechanics, driving time, deconditioning, and persistent nerve irritation all affect the long game.
If your symptoms aren’t settling, if the leg is becoming unreliable, or if you need a more precise plan than “stretch and wait,” you can request an appointment with Midwest Pain & Wellness. The goal is straightforward. Identify the source, treat it in steps, and help you get back to normal movement without depending on opioids.
Frequently Asked Questions About Sciatica
Can sciatica be cured permanently, or will it come back
Sometimes it resolves fully and stays quiet. Sometimes it recurs, especially if the underlying driver is still there. Disc problems, stenosis, work strain, and poor movement mechanics can all bring symptoms back. The goal is to treat the current flare and reduce the reasons it keeps returning.
How do I know if I need an injection or just more physical therapy
That decision depends on the exam, symptom severity, and whether the pain is improving with the right movement plan. If therapy is centralizing pain and function is improving, more conservative care may make sense. If pain remains severe, sleep is poor, walking is limited, or progress has stalled, an injection may help create a better rehab window.
Is it safe to continue working or exercising with sciatica pain
Often yes, but only within limits that don’t keep provoking the nerve. Gentle movement is usually better than complete rest. Heavy lifting, repeated bending, impact activity, or long sitting may need to be reduced temporarily. If work is worsening leg pain or weakness, get assessed before pushing through it.
If sciatica is disrupting your sleep, work, or ability to move normally, Midwest Pain & Wellness can help you sort out the cause and choose the next appropriate step, from diagnosis and guided conservative care to image-guided, opioid-sparing interventional treatment.



