A lot of people looking for sports medicine naperville aren’t dealing with a dramatic fresh injury. They’re dealing with the stubborn version. The knee that still swells after pickleball in Orland Park. The shoulder that never felt right after old baseball seasons in Oak Lawn. The low back pain that started as “just tightness” and now limits golf, lifting, sleep, and work.
That’s where sports medicine becomes much more than sideline care. It becomes a way to sort out what still hurts, why it still hurts, and what can restore function when the usual advice hasn’t done enough.
Naperville has earned a strong reputation in this space. At the same time, the people who need this kind of care live all across the southwest Chicago suburbs, including Palos Hills, Palos Heights, Worth, Bridgeview, Hickory Hills, Alsip, Burbank, Evergreen Park, and Orland Park. Many are not competitive athletes. They’re active adults who want to move without paying for it later.
Your Guide to Sports Medicine in the Chicago Area
A man in Palos Hills gets through the workday, then skips basketball because his knee swells every time he tries to cut or pivot. A golfer in Orland Park shortens his backswing because low back pain lingers for two days after a round. A runner in Evergreen Park keeps restarting, then stopping again, because the same shin, hip, or heel pain keeps coming back.
Those patients need more than general advice to rest and wait.

Sports medicine in the Chicago area serves active adults, former athletes, weekend competitors, and people whose jobs put repetitive stress on the body. In practice, many are dealing with a problem that started as a strain, sprain, overuse injury, or old sports injury and then turned into persistent pain. By the time they look for help, they are often asking a different question. Not "What happened?" but "Why does it still hurt months later?"
That is where a stronger sports medicine evaluation matters. The goal is not only to name the injury. The goal is to identify the structure still driving pain, determine why first-line treatment has stalled, and choose the next step that restores function with the least disruption. For some people, that means refining rehab. For others, it means image-guided injection care, regenerative treatments, or another non-opioid interventional option when physical therapy alone has not been enough.
Who this helps most
This kind of care is often the right fit for adults with:
- Lingering joint pain after a "minor" injury that never fully settled down
- Pain during activity that improves with rest, then returns as soon as training resumes
- Back or neck symptoms triggered by rotation, lifting, impact, or repetitive motion
- Older sports injuries that flare more often with age, workload, or degenerative change
In my experience, the people who benefit most are not looking for a shortcut. They have usually already tried the basics. They want a clear diagnosis, a realistic plan, and treatment that helps them get back to work, sleep, exercise, and daily life without relying on opioids or stopping the activities they value.
If pain is limiting how you move, train, or recover, sports medicine may be the step that turns an unresolved injury into a treatable problem.
Understanding the Full Scope of Sports Medicine
Sports medicine works best when people stop thinking of it as one doctor, one test, or one treatment. It’s a team-based field. Different specialists handle different parts of the same problem.
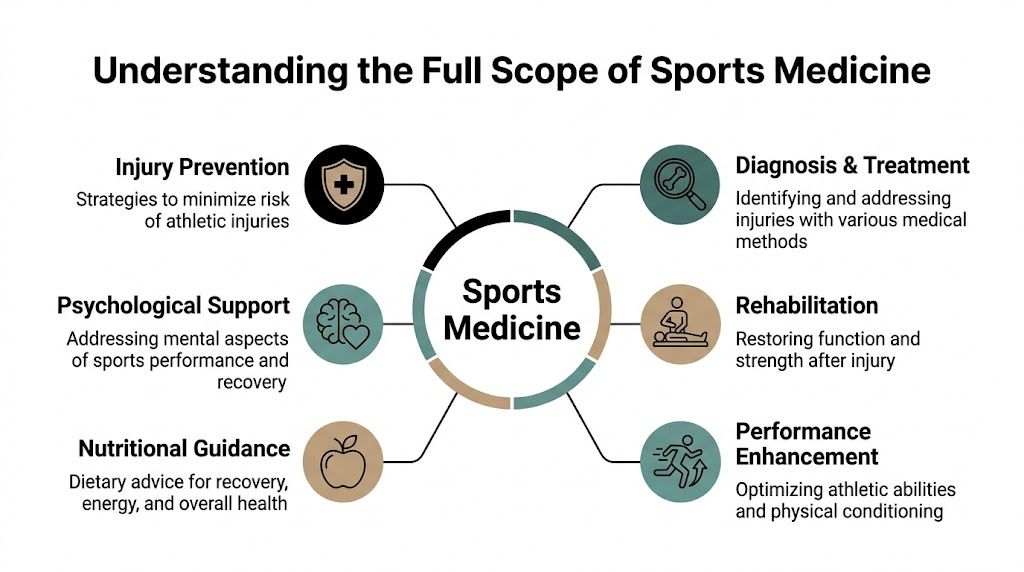
What sports medicine actually includes
Consider a pit crew. One person isn’t doing everything.
| Part of care | What it does |
|---|---|
| Prevention | Identifies movement patterns, training loads, or biomechanical issues that raise injury risk |
| Diagnosis | Uses exam findings, imaging, and history to identify the pain generator |
| Rehabilitation | Rebuilds motion, strength, coordination, and tolerance |
| Medical treatment | Manages inflammation, pain, tissue irritation, and return-to-activity planning |
| Procedural care | Uses targeted interventions when symptoms persist |
| Surgical care | Steps in when structure, instability, or tissue damage requires repair |
That broad scope exists because sports injuries don’t all behave the same way. A fresh ankle sprain is one problem. Rotator cuff pain that still wakes someone up months later is another. Low back pain after years of lifting, twisting, and impact is different again.
Acute injury and chronic pain are not the same
A lot of standard sports medicine content focuses on acute injuries. That’s important, but it leaves out a large group of adults with persistent pain after the initial healing window.
That group includes the person who already tried rest, anti-inflammatory medication, and physical therapy. It includes the patient whose MRI doesn’t fully explain the pain pattern. It includes the adult whose old football, soccer, softball, dance, or running injuries now overlap with wear and tear.
National demand reflects how common this care is. Over 30 million children and adolescents participate in organized sports annually, and 3.8 million sports-related concussions occur each year in the US, according to Market.us sports medicine statistics. The same source notes that North America held a 37.2% revenue share in the sports medicine market in 2022.
Where a pain specialist fits
A board-certified interventional pain specialist typically enters the picture when the issue is no longer just “rehab it and wait.”
That role often includes:
- Pinpointing pain sources when symptoms come from joints, discs, tendons, nerves, or several at once
- Using image-guided procedures for precision rather than blind treatment
- Reducing reliance on opioids by targeting the structure or nerve pathway involved
- Helping patients function now while other parts of recovery continue
The best sports medicine care is collaborative. It doesn’t compete with orthopedics or rehab. It fills the gap when pain becomes the barrier to progress.
Common Injuries That Lead to Chronic Pain
A 38-year-old runner finishes physical therapy for knee pain, returns to training, and the same pain comes back on stairs, during long drives, and after sitting through work meetings. That pattern is common in adult athletes and active adults. The original injury may have started on the field, in the gym, or during a weekend race, but the chronic pain that follows often affects far more than sports.
The cases that linger are often the ones that looked minor at first. A sore shoulder after tennis. Heel pain during a training block. A back flare after lifting. If symptoms keep returning, the problem usually has shifted from a short-term strain to a more persistent pain source involving tendon tissue, a joint, a nerve, or several structures at once.
Tendon injuries that stop acting like minor overuse problems
Chronic tendon pain is one of the most frequent reasons active adults stall out. This includes tennis elbow, golfer’s elbow, patellar tendinopathy, Achilles tendinopathy, and rotator cuff tendinopathy.
Early on, pain may show up only during exercise. Later, it starts interfering with ordinary tasks such as gripping a pan, climbing stairs, carrying bags, reaching overhead, or sleeping on one side. That change matters. It suggests the tissue is no longer calming down with routine activity modification alone, and the pain may be sustained by poor load tolerance, irritation at the tendon attachment, or surrounding joint dysfunction.
Knee injuries that outlast the season
Chronic knee pain rarely stays simple for long. Patellofemoral pain can overlap with tendon irritation, swelling, cartilage wear, hip weakness, and movement changes that keep the knee irritated. After an ACL, MCL, or meniscus injury, some adults regain strength but still do not trust the joint. They avoid bending, pivoting, hills, or kneeling because pain or instability keeps resurfacing.
That is where a careful exam matters. Persistent knee pain is not always coming from the structure named in the first diagnosis.
Shoulder pain that spreads beyond the shoulder
Shoulder injuries often begin with pain during reaching, pressing, throwing, or sleeping on the affected side. As symptoms continue, patients start compensating through the neck, shoulder blade, and upper back. Then the pain map gets wider.
I see this often after rotator cuff irritation, bursitis, labral injuries, and chronic impingement patterns. The trade-off is familiar. People stay active enough to get by, but they lose strength, range of motion, and confidence with lifting. Over time, daily function becomes the bigger problem.
Back and pelvic pain in active adults
Low back pain tied to sports and exercise can come from facet joints, discs, the sacroiliac joint, irritated nerves, or muscular guarding layered on top of one of those issues. Rotational sports, repetitive extension, distance running, heavy lifting, and contact play can all contribute.
Once this becomes chronic, the limitations are broader than missed workouts. Sitting through work, driving, sleeping, and getting back to normal exercise all become harder. In adults with persistent symptoms, the question is not just what sport triggered the pain. The question is which structure is still generating it now.
For readers sorting through lingering symptoms, this overview of conditions treated in interventional pain management can help clarify where tendon, joint, spine, and nerve pain fit.
A sports injury becomes a chronic pain problem when it keeps limiting work, sleep, movement, or daily function long after the expected healing window.
When Rest and Physical Therapy Are Not Enough
Rest matters. Good physical therapy matters. Anti-inflammatory strategies, mobility work, and graded strengthening matter too. For many people, those are the right first steps.
But they aren’t always enough.
The main reason is simple. Some patients don’t just have weak muscles or tight tissues. They have a specific pain generator that keeps interrupting recovery. If every attempt at rehab flares the same joint, nerve, tendon insertion, or spinal structure, the body never gets a fair chance to rebuild normal movement.

Signs you may need the next level of care
A more advanced evaluation makes sense when the pattern looks like this:
- You improved, then plateaued and can’t get past the same pain ceiling
- PT exercises keep provoking symptoms instead of building tolerance
- Pain is interfering with sleep or work, not just sports
- You’ve cut activity repeatedly, but the pain returns with each restart
- The diagnosis feels incomplete, especially when imaging and symptoms don’t match cleanly
What interventional pain management adds
Interventional pain management focuses on precision. The goal isn’t to “mask” pain broadly. It’s to identify the pain source and treat it in a targeted way so recovery can move again.
That can include:
- Image-guided injections to reduce inflammation around a joint, nerve root, tendon-adjacent structure, or bursa
- Medial branch blocks when facet-mediated back pain is suspected
- Radiofrequency ablation when those nerves are confirmed pain drivers and need longer-lasting interruption
- Epidural steroid injections for radiating spine-related pain
- Sacroiliac joint interventions when the problem is lower and more mechanical than patients realize
- Spinal cord stimulation in selected chronic cases involving nerve pain
- MILD and Vertiflex Superion procedures for certain patients with lumbar spinal stenosis whose pain limits walking and standing
What works and what usually doesn’t
A realistic sports medicine naperville discussion needs trade-offs, not hype.
What often works well:
- Accurate diagnosis before treatment
- Procedures paired with active rehab, not used as a substitute for movement
- Targeted care for clearly defined pain generators
- Function-based goals, such as walking farther, returning to golf, sleeping through the night, or tolerating stairs
What usually doesn’t work well:
- Repeating the same PT program when it keeps causing the same flare
- Using opioids as the main long-term answer for mechanical or structural pain
- Getting injections without image guidance or a clear diagnostic purpose
- Chasing every painful area separately when one source is driving the rest
A major education gap remains in this part of care. Fifty percent of sports injury patients can develop chronic pain, and advanced non-surgical options like radiofrequency ablation or spinal cord stimulation are often under-discussed, as described by Rush’s Naperville orthopaedics listing.
Practical rule: If treatment keeps reducing your activity but not reducing your pain, the plan needs to change.
Interventional care isn’t a replacement for sports medicine. It’s often the missing piece for adults whose pain has outlasted the usual first-line approach.
The Role of Regenerative Medicine in Healing
A common scenario in clinic is the adult who finished months of physical therapy, modified workouts, tried anti-inflammatories, and still cannot trust a shoulder, knee, elbow, or tendon to handle normal activity. That is where regenerative medicine may enter the discussion, but only after the diagnosis is clear and the treatment target makes sense.
What PRP is
PRP, or platelet-rich plasma, uses a sample of the patient’s own blood. That sample is processed to concentrate platelet-rich components, then injected into a specific structure under imaging guidance when precision matters.
The goal is to support healing in tissue that has stalled, especially when the problem is degenerative or chronic rather than a fresh injury. In the right setting, PRP can complement a broader plan built around function, load management, and progressive rehabilitation.
Where it may fit best
PRP is usually considered for a narrow set of problems, not for every painful area. Examples include:
- Certain chronic tendinopathies
- Some cases of joint pain tied to degeneration
- Patients trying to postpone surgery
- Persistent pain where first-line care helped only partly, and the anatomy being treated is well defined
This distinction matters. A painful knee is not automatically a PRP knee. A sore shoulder is not automatically a PRP shoulder. Good regenerative care starts with identifying the exact structure involved and deciding whether that tissue is likely to respond.
The real trade-offs
PRP asks more patience from patients than a numbing injection or steroid. Relief is not immediate. Out-of-pocket cost is common. Results also depend heavily on the tissue being treated, the chronicity of the injury, and whether the rehab plan matches the procedure.
I discuss PRP most seriously when the pain generator is localized and the problem has persisted despite appropriate conservative care. I do not present it as a catch-all option for back pain, nerve pain, or every overuse injury. If the main issue is a compressed nerve, significant instability, advanced arthritis, or spinal stenosis, interventional pain procedures often deserve more attention than regenerative treatment.
That is the key point for adults with chronic sports injuries in Naperville, Orland Park, and the rest of the Chicago area. Regenerative medicine can help selected tendon, ligament, and joint problems. Persistent pain that has moved into the spine, sacroiliac joint, facet joints, or irritated nerve pathways often requires a different strategy. For many patients, the better question is not “Do I need PRP?” but “What structure is keeping me from walking, lifting, sleeping, or training normally?”
For readers comparing options, this overview of interventional and regenerative procedures used in treatment shows how PRP fits alongside image-guided injections, radiofrequency ablation, neuromodulation, and minimally invasive spine care.
PRP works best when the diagnosis is specific, the tissue target is appropriate, and the goal is improved function, not hype.
How to Choose Your Sports Medicine Provider
The hardest part for many patients isn’t deciding to get help. It’s figuring out who should lead the workup.
A good provider match depends on the stage of the problem. Fresh fractures, major ligament tears, and instability often need an orthopedic pathway first. Chronic pain after incomplete recovery often needs someone who can diagnose beyond the obvious and offer more than basic medication advice.
Questions worth asking
Bring these questions to any consultation in Naperville or the southwest suburbs of Illinois.
- What happens if physical therapy alone doesn’t solve this? A strong clinic should have a clear next-step strategy.
- Do you offer opioid-sparing treatment plans? This matters for long-term function and clarity of thinking.
- Are procedures image-guided? Precision matters when treating joints, nerves, and spinal structures.
- How do you coordinate with surgeons, primary care doctors, or rehab teams? Complex pain rarely stays in one lane.
- Do you treat older injuries and degenerative problems, or only acute athletic injuries? Many adults need the first, not the second.
- Can you work with workers’ compensation or injury-related claims if needed? Logistics affect access.
Green flags and caution flags
Here’s a practical way to sort options.
| Green flag | Caution flag |
|---|---|
| The provider explains the pain source clearly | You leave with only a vague label |
| The plan includes functional goals | The plan focuses only on temporary symptom suppression |
| Different options are discussed with trade-offs | One treatment is pushed as the answer for everyone |
| Care is coordinated when needed | You’re left to navigate referrals alone |
Credentials matter too. If you want to understand the training background behind interventional pain care, reviewing a physician profile such as Dr. Yaw Donkoh’s professional background can help you know what board certification and procedure-focused expertise look like.
A good sports medicine naperville search should end with more than a list of names. It should lead you to a clinician who can explain what’s wrong, what the realistic options are, and why one path makes more sense than another.
Your First Appointment and What to Expect
Most first visits go better when patients come prepared. That sounds obvious, but it often changes the quality of the evaluation.
Bring any prior MRI, X-ray, CT, or procedure reports you already have. If you’ve done physical therapy, bring the timeline and a short summary of what helped, what didn’t, and what consistently made symptoms worse. That history often matters as much as the imaging.
It also helps to write down three things before you arrive:
- What activity you want back most
- What movement triggers the pain fastest
- How the problem affects work, sleep, or daily function
If you’re using insurance, have your card and referral information ready if your plan requires it. If the case involves workers’ compensation or personal injury, bring claim details and any paperwork you’ve already received.
Expect the visit to focus on function, not just pain intensity. A useful consultation should connect the story, the exam, the imaging, and the failed treatments into a plan that makes sense.
Frequently Asked Sports Medicine Questions
Do I need to be an athlete to see a sports medicine specialist
No. Many patients are active adults with old injuries, repetitive strain, arthritis, or pain that shows up during walking, lifting, golf, tennis, yard work, or exercise.
What’s the difference between an orthopedic surgeon and an interventional pain specialist
An orthopedic surgeon evaluates structural problems that may require repair or reconstruction. An interventional pain specialist focuses on diagnosing and treating pain generators with image-guided, non-opioid procedures, especially when surgery isn’t the first or best next step.
Can an old sports injury cause pain years later
Yes. Old injuries can change joint mechanics, tissue loading, and movement patterns. Over time, that can contribute to recurring pain, stiffness, tendon overload, or degenerative changes.
Are injections just temporary fixes
Sometimes they’re mainly diagnostic. Sometimes they reduce inflammation enough to allow real rehabilitation progress. The value depends on the target, the reason for doing them, and what happens after the procedure.
When should I worry that pain is becoming chronic
Pay attention when pain keeps returning despite rest, limits daily activity, wakes you up, or blocks progress in therapy. That’s usually the point when a more detailed workup is worth it.
Is avoiding opioids realistic
For many musculoskeletal and spine-related sports injuries, yes. A modern plan often uses targeted procedures, rehabilitation, activity modification, and coordinated specialty care instead of relying on opioid medication as the center of treatment.
If chronic sports-related pain is limiting how you move, train, work, or sleep, Midwest Pain & Wellness offers board-certified, opioid-sparing care for patients across the Chicago area, including communities near Chicago Ridge, Oak Lawn, Palos Hills, Palos Heights, Worth, Bridgeview, Hickory Hills, Alsip, Burbank, Evergreen Park, and Orland Park. The clinic focuses on precise diagnosis, image-guided treatment, and practical plans that help people restore function without making opioids the default answer.



