Understanding the Burden of Migraine Pain
Effective migraine pain management uses a multi-faceted approach of acute treatments, preventive strategies, and lifestyle changes to reduce attack frequency and severity. While migraines have no cure, proper management significantly improves quality of life.
Quick Overview: Key Approaches to Migraine Pain Management
- For mild to moderate attacks: NSAIDs (ibuprofen, naproxen) or acetaminophen as first-line treatment
- For moderate to severe attacks: Triptans, which work best when taken early
- Preventive medications: Daily medications like beta-blockers, antidepressants, or newer CGRP antagonists for frequent migraines (4+ days per month)
- Lifestyle changes: Consistent sleep schedule, regular meals, hydration, and stress management
- Avoid medication overuse: Use acute medications no more than 2-3 days per week to prevent rebound headaches
- Complementary therapies: Biofeedback, acupuncture, and relaxation techniques as additional support
If you suffer from frequent, severe migraines, you’re not alone. Migraines affect approximately 44.5 million U.S. adults—18% to 26% of women and 6% to 9% of men. More than just a bad headache, a migraine attack can be debilitating, with throbbing pain, nausea, and extreme sensitivity to light and sound that can last for days.
The impact is significant. Migraines are the fourth most common cause of emergency department visits and cost the U.S. over $17 billion annually in direct medical expenses, with even higher costs from lost productivity.
Fortunately, there is hope. Modern migraine management has evolved, offering immediate relief for acute attacks and long-term strategies to reduce their frequency. With evidence-based medications, lifestyle changes, and innovative therapies, more options are available than ever.
This guide will help you understand your migraine patterns, choose the right treatments, and build a comprehensive, opioid-free management plan that works for you.
Migraine pain management terms simplified:
Understanding Your Migraine: Types, Phases, and Triggers
Effective migraine pain management starts with understanding your unique experience. Since migraines are complex and personal, a precise diagnosis, symptom tracking, and trigger identification are cornerstones of treatment.
Diagnosis involves a medical history, a physical and neurological exam, and questions about your symptoms. Providers use criteria from the International Classification of Headache Disorders (ICHD-3) and tools like the POUND mnemonic. While imaging like an MRI or CT scan won’t show a migraine, it may be used to rule out other causes for severe headaches.
Keeping a migraine journal is crucial. This tool helps track symptoms, identify patterns, and pinpoint triggers, providing valuable data for your healthcare provider to tailor your treatment. The American Migraine Foundation offers guidance on keeping a migraine journal.
Types of Migraines and Their Symptoms
Migraines are not a one-size-fits-all headache. There are several types, each with unique characteristics:
- Migraine with Aura (Classic Migraine): About 25-30% of people with migraine experience an aura—temporary neurological symptoms before or during the headache. These are often visual (flashing lights, zigzag lines) but can also include tingling or speech difficulty.
- Migraine without Aura (Common Migraine): The most common type, this features a debilitating headache without the preceding aura phase.
- Chronic Migraine: Diagnosed with 15 or more headache days per month for three months (at least eight being migraines). It is challenging to manage and requires a comprehensive approach.
- Hemiplegic Migraine: A rare, severe form causing temporary weakness on one side of the body, mimicking a stroke.
- Menstrual Migraine: Linked to hormonal changes, occurring around a woman’s menstrual period.
- Migraine without Headache (Silent Migraine): Involves aura and other migraine symptoms without the headache pain.
- Retinal Migraine: A rare type causing temporary vision loss in one eye.
- Status Migrainosus: A severe migraine attack lasting over 72 hours.
Migraines are common, affecting an estimated 12% of people in the United States. They tend to run in families, with up to 80% of individuals having a first-degree biological relative with the condition. Women are also more likely than men to experience migraines.
The Four Phases of a Migraine Attack
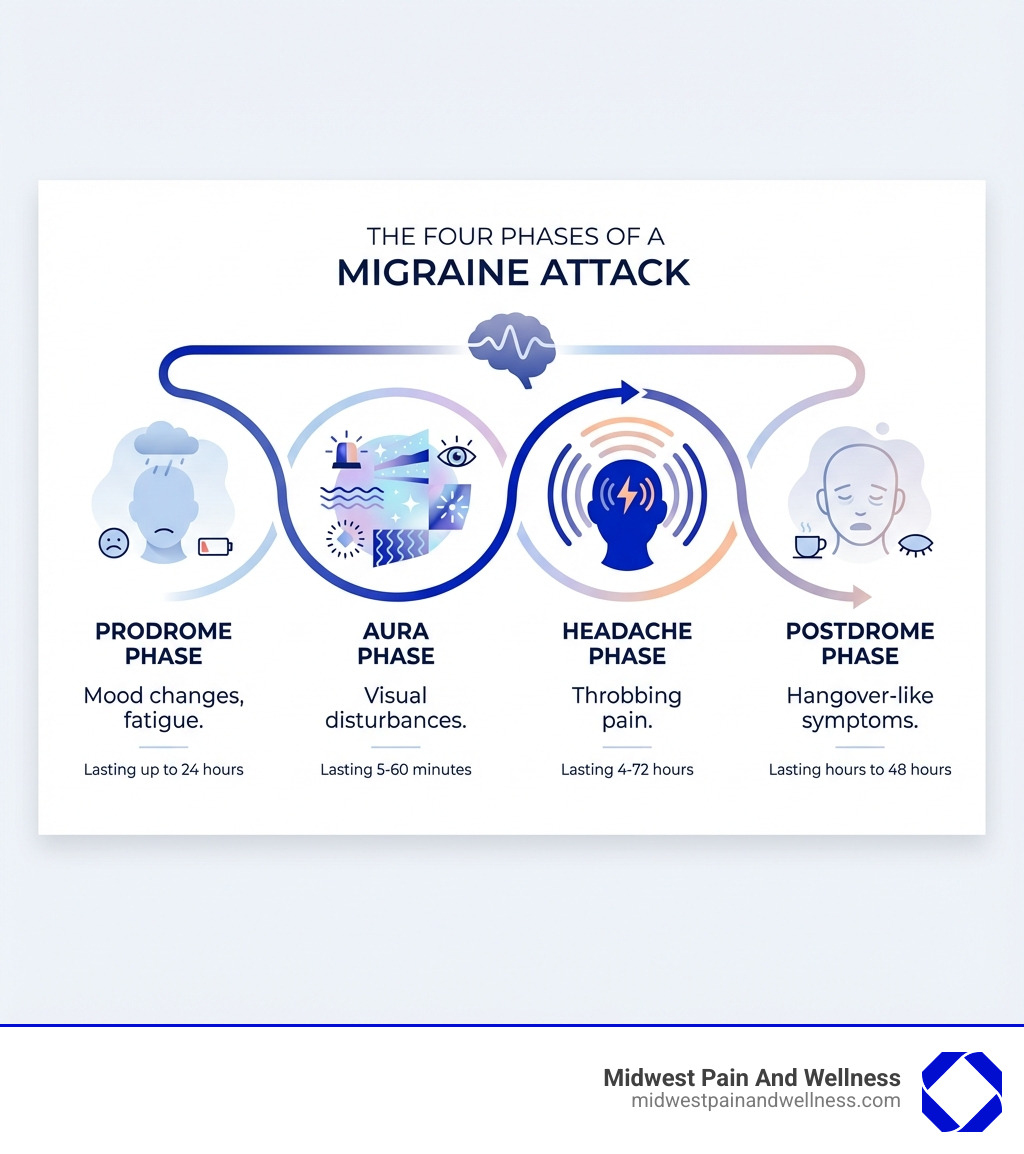
A migraine attack typically progresses through four distinct phases, though not everyone experiences all of them:
- Prodrome Phase (Warning Signs): Up to 24 hours before the headache, subtle warning signs can appear, including mood changes, fatigue, neck stiffness, and food cravings.
- Aura Phase: Lasting 5-60 minutes, this phase involves temporary neurological symptoms, most commonly visual disturbances, but also sensory or speech issues.
- Headache Phase: The main attack lasts 4-72 hours. Pain is typically throbbing and on one side of the head, worsening with activity. It’s accompanied by nausea and extreme sensitivity to light, sound, and smells.
- Postdrome Phase (Migraine Hangover): After the headache, a “migraine hangover” can last up to 48 hours, with symptoms like fatigue, difficulty concentrating, and neck stiffness.
Identifying Common Migraine Triggers
Understanding and avoiding your specific triggers is a cornerstone of effective migraine pain management. While triggers vary greatly, some common culprits include:
- Environmental Factors:
- Sensory Overload: Bright lights, loud noises, and strong smells.
- Weather Changes: Changes in barometric pressure, humidity, or temperature.
- Lifestyle Factors:
- Stress: A leading trigger, including high stress or the letdown period after stress.
- Sleep Changes: Too little, too much, or irregular sleep. Aim for consistency.
- Missing Meals: Skipping meals can cause blood sugar drops that trigger attacks.
- Overexertion: Intense physical activity, particularly without proper warm-up.
- Dietary Factors:
- Caffeine: Caffeine withdrawal or excessive intake.
- Alcohol: Red wine and dark liquors are common culprits.
- Aged Cheeses: Tyramine in aged cheeses.
- Processed or Cured Meats: Nitrates and nitrites in processed meats.
- Food Additives: MSG and artificial sweeteners.
- Chocolate: A common, debated trigger.
- Hormonal Changes: Estrogen fluctuations during menstruation, pregnancy, or menopause are a major trigger in women. Oral contraceptives can also play a role.
To effectively identify your triggers, we highly recommend keeping a dedicated headache diary. This helps you track potential connections between your activities, diet, environment, and migraine onset.
Acute Migraine Pain Management Strategies
When a migraine strikes, the goal of acute migraine pain management (or abortive therapy) is to stop pain and symptoms quickly. Treatment aims for rapid pain relief, reduced nausea, and a swift return to daily activities. The American Headache Society offers a useful guide on acute treatments.
First-Line Pharmacological Migraine Pain Management
For mild to moderate migraine attacks, simple over-the-counter (OTC) medications are often the first line of defense:
- NSAIDs (Nonsteroidal Anti-Inflammatory Drugs): Ibuprofen and naproxen are effective choices. Studies show ibuprofen is highly effective for pain improvement (NNT=3-7), with naproxen also being a solid option (NNT=7-10).
- Acetaminophen (Tylenol): Acetaminophen is an alternative for those who cannot tolerate NSAIDs.
- Combination Analgesics: Combination products with acetaminophen, aspirin, and caffeine can be effective for mild to moderate attacks.
It’s important to understand the differences between OTC vs. Prescription Medications and when each is appropriate for your migraine severity.
Triptans: A Targeted Approach for Moderate to Severe Pain
When OTC options aren’t enough, or for moderate to severe migraines, triptans are often the first-line prescription treatment.
- Mechanism of Action: Triptans activate serotonin receptors to constrict dilated blood vessels and block pain pathways.
- When to Use Triptans: They work best when taken at the first sign of a migraine headache.
- Formulations: Available as tablets, nasal sprays, and injections, they offer options for those with nausea. Subcutaneous sumatriptan is one of the most effective, with an NNT of 2 for complete pain relief at two hours.
- Combination Therapy: Combining a triptan with an NSAID (e.g., sumatriptan plus naproxen) is often more effective for complete and sustained pain relief than either drug alone.
A meta-analysis of seven available triptans showed they provided headache relief at two hours in 42% to 76% of patients and complete pain relief in 18% to 50%.
Second-Line and Newer Options
For individuals who don’t respond well to first-line treatments or have specific contraindications, several other options are available:
- Dihydroergotamine (DHE): This medication works similarly to triptans but can have more side effects. It comes in nasal spray and injectable forms.
- Antiemetics: Antiemetics like metoclopramide combat severe nausea and vomiting. They can be used alone or combined with pain relievers for better results.
- Gepants: Gepants (ubrogepant, rimegepant, zavegepant) are a newer class of CGRP receptor antagonists. They don’t cause vasoconstriction, making them safer for patients with cardiovascular risks who cannot take triptans. They may also have a lower risk of medication overuse headache.
- Ditans: Lasmiditan (Reyvow), a ditan, also lacks vasoconstrictive effects, providing another option for those with cardiovascular concerns. However, it can cause sedation, so driving should be avoided for at least eight hours after use.
For more information on these advanced options, you can explore resources on newer therapies like Gepants and Ditans.
When to Seek Immediate Medical Attention
While migraines are generally not life-threatening, certain symptoms warrant immediate medical attention to rule out more serious conditions. Call 911 or go to the nearest emergency department if you experience:
- “Thunderclap” Headache: A sudden, severe headache reaching maximum intensity within a minute (“thunderclap” headache), which can signal a brain hemorrhage.
- Headache After Head Injury: Any severe headache that develops after a fall or head trauma.
- New Neurological Symptoms: New or different neurological symptoms like weakness, numbness, vision changes, or difficulty speaking.
- Stiff Neck and Fever: These, combined with a severe headache, could indicate meningitis.
- First or Worst Headache: The “worst headache of your life” or one that feels significantly different from your usual migraines.
It’s better to be safe than sorry when these red flag symptoms appear.
Proactive and Advanced Migraine Management
Effective migraine pain management also requires proactive strategies to reduce attack frequency and severity. This is vital for chronic or refractory migraines where standard treatments fail. At Midwest Pain And Wellness, our commitment to comprehensive, opioid-free pain management aligns with modern migraine care.
Preventive Strategies to Reduce Migraine Attacks
Preventive strategies aim to reduce migraine frequency, severity, and duration. They improve quality of life and reduce reliance on acute medications, lowering the risk of medication overuse headache. Prevention is considered for those with 4 or more monthly headache days, significant life impact, or when acute treatments are overused or ineffective.
Common preventive medications include:
- Beta-Blockers: Propranolol, metoprolol, and timolol reduce the excitability of the brain and blood vessels.
- Antidepressants: Certain antidepressants (e.g., amitriptyline, venlafaxine) can prevent migraines, even without depression.
- Anticonvulsants: Topiramate and divalproex sodium are effective, though the latter is often a second-line choice for women due to potential birth defects.
- CGRP Antagonists (Monoclonal Antibodies): These newer injectable medications (erenumab, fremanezumab, galcanezumab, eptinezumab) target the CGRP pathway, a key player in migraine pain, and have revolutionized prevention.
Preventive medications require time to work, often 2-3 months for oral drugs and 3-6 months for CGRP injections to see full benefits. The American Headache Society offers a position statement on integrating new migraine treatments into clinical practice.
The Dangers of Medication Overuse and Opioids
While acute medications provide necessary relief, their overuse can lead to a significant complication known as Medication Overuse Headache (MOH), sometimes called “rebound headache.”
- Medication Overuse Headache (MOH): Taking acute medications too often (10-15+ days/month) can cause MOH, where the medication itself triggers more headaches. It complicates migraine pain management significantly. To avoid this, limit acute medication use to 2-3 days per week, or ideally, fewer than 10 days per month. The American Headache Society provides a helpful Triptan and NSAID Limits Guide.
- Opioid-Induced Hyperalgesia (OIH): OIH is a paradoxical condition where long-term opioid use increases pain sensitivity. Instead of relieving pain, the opioids make you more sensitive to it. This is a critical concern for chronic pain management.
At Midwest Pain And Wellness, we are dedicated to opioid-free pain management. For chronic conditions like migraine, the long-term risks of opioids (OIH, addiction) often outweigh the benefits. If OIH is suspected, we employ strategies to reduce opioid exposure and manage pain effectively.
Managing Refractory and Severe Migraines
For severe, persistent migraines that don’t respond to conventional treatments (refractory migraine), we explore advanced interventional strategies:
- Interventional Procedures: Our specialists at Midwest Pain And Wellness perform interventional procedures like greater occipital nerve blocks to interrupt pain signals and trigger point injections to relieve muscle-related pain.
- Botox Injections: Botox is an FDA-approved preventive treatment for chronic migraine (15+ headache days/month), administered every 12 weeks to reduce attack frequency and severity.
- Neuromodulation Devices: These non-pharmacological devices stimulate nerves to alter the brain’s pain response. Options include:
- Cefaly Dual: An external trigeminal nerve stimulation (eTNS) device for acute and preventive treatment.
- Nerivio: A remote electrical neuromodulation (REN) wearable that stimulates peripheral nerves in the upper arm.
- gammaCore Sapphire: A non-invasive vagal nerve stimulator for acute and preventive treatment.
When patients feel like they’ve tried everything, it can be incredibly frustrating. However, there is always hope, and we are here to help you explore every avenue. For guidance on what to do when treatment fails, resources are available to help you steer next steps.
Holistic and Specialized Treatment Approaches
Effective migraine pain management often extends beyond medication, embracing a holistic view that includes lifestyle modifications, complementary therapies, and specialized considerations for different patient populations. At Midwest Pain And Wellness, we believe in a multi-modal approach that addresses the full spectrum of factors influencing your migraines.
Lifestyle Modifications for Better Control
Lifestyle adjustments play a crucial role in reducing migraine frequency and severity. We often use the “SEEDS” acronym to guide these changes: Sleep, Exercise, Eat, Diary, Stress.
- Consistent Sleep Schedule: Aim for a consistent 7-8 hours of sleep nightly, even on weekends. An irregular schedule is a major trigger.
- Regular Meals and Hydration: Eat regular, balanced meals to stabilize blood sugar and stay well-hydrated. While identifying food triggers can help, consistency is key. Limit caffeine to under 200mg/day.
- Stress Management Techniques: Since stress is a major trigger, incorporate relaxation techniques like deep breathing, meditation, or yoga. Therapies like CBT and ACT can also help manage stress and pain response.
- Regular Exercise: Regular, moderate aerobic exercise can help prevent migraines. Start slowly, building up to 30 minutes, three times a week. Intense exercise can be a trigger for some.
Complementary Therapies and Their Evidence
Many individuals find benefit from complementary and integrative therapies as part of their migraine pain management plan:
- Biofeedback: This technique teaches you to control bodily functions like muscle tension to reduce migraines, with scientific research on biofeedback for migraine supporting its efficacy.
- Acupuncture: Studies suggest acupuncture, which involves inserting thin needles into specific points, can be as effective as some preventive medications.
- Relaxation Therapy: Techniques like progressive muscle relaxation and guided imagery help reduce stress and muscle tension.
- Cognitive Behavioral Therapy (CBT): CBT helps change negative thought patterns and behaviors related to pain to improve coping.
- Supplements: Supplements like riboflavin (B-2), Coenzyme Q10, and magnesium may help prevent migraines for some, but always consult your provider first.
- Green Light Therapy: Emerging research suggests green light therapy may reduce light sensitivity and headache severity.
Special Considerations for Migraine Treatment
Migraine affects people differently across age groups and life stages, requiring custom approaches:
- Children and Adolescents: For children and adolescents, ibuprofen is often the most effective first-line acute treatment. If it fails, certain triptans may be considered. The American Headache Society provides specific guidance on acute therapy for adolescents.
- Pregnancy and Lactation Safety: Managing migraines during pregnancy and lactation requires careful planning to protect the baby. Non-drug treatments and nerve blocks are preferred. If medication is needed, acetaminophen is generally considered safe. Close collaboration with your obstetrician and headache specialist is essential. For breastfeeding, paracetamol is generally preferred. Review the FDA’s safety guide for pregnancy.
- Contraindications for Vasoconstrictive Migraine Medications: Triptans and ergotamines are contraindicated for patients with cardiovascular conditions (e.g., coronary artery disease, uncontrolled hypertension, history of stroke) because they narrow blood vessels. Safer, non-vasoconstrictive alternatives for these patients include gepants, ditans, and NSAIDs for acute migraine pain management.
Frequently Asked Questions about Migraine Management
We hear a lot of questions about migraine management. Here are some of the most common ones we encounter:
What is the difference between a migraine and a tension headache?
This is a great question, as they can sometimes be confused!
- Migraine: Involves moderate to severe, throbbing pain, often on one side. It’s accompanied by symptoms like nausea and sensitivity to light and sound, worsens with activity, and is often debilitating.
- Tension Headache: A mild to moderate, dull, aching pain or pressure on both sides of the head, like a tight band. It is not accompanied by nausea and doesn’t worsen with activity.
How quickly do migraine medications work?
The speed of relief varies by formulation. Oral pills (NSAIDs, triptans) usually work in 30-60 minutes. Faster-acting nasal sprays and injections can provide relief in as little as 10-15 minutes. For best results, take acute medication at the first sign of a migraine, as waiting can make it less effective.
Can diet really help my migraines?
Yes, diet is a key part of migraine pain management, but it’s highly individual. Key strategies include:
- Regular Meals & Hydration: Don’t skip meals and drink plenty of water, as blood sugar drops and dehydration are common triggers.
- Trigger Foods: A migraine diary can help identify personal food triggers like aged cheese, processed meats, or alcohol.
- Supplements: Some people find relief with supplements like magnesium, riboflavin (B-2), and Coenzyme Q10.
Always work with a healthcare provider to create a dietary plan, as overly restrictive diets can be counterproductive.
Conclusion: Partnering for Your Long-Term Relief
Living with migraines is challenging, but the right approach to migraine pain management makes a life with fewer, less severe attacks possible. We’ve explored the complex world of migraines, from understanding their varied types and phases to identifying triggers and navigating a wide array of treatment options.
The key takeaways are clear:
- Migraines are a real, debilitating neurological condition, affecting millions, and they require a comprehensive, personalized approach.
- Effective management is multi-modal, combining acute relief, preventive strategies, and essential lifestyle modifications.
- Opioid-free approaches are paramount to avoid complications like medication overuse headache and opioid-induced hyperalgesia, aligning with our commitment at Midwest Pain And Wellness.
- You are not alone, and partnering with a dedicated healthcare provider is crucial for developing a treatment plan custom to your unique needs.
The outlook for migraine sufferers is hopeful. While there is no cure, advances in treatment and understanding make effective management more attainable than ever. By being proactive, tracking your symptoms, and embracing a holistic approach, you can significantly reduce the burden of migraines.
At Midwest Pain And Wellness, our double board-certified doctors are here in Chicago Ridge, Illinois, to collaborate with you. We use a multi-modal, interventional approach to create custom care plans for long-term pain relief, focusing on effective, opioid-free solutions. We believe in empowering our patients to become active partners in their health journey.
Don’t let migraines control your life. Take the first step towards a future with less pain and more wellness. Learn more about our opioid-free pain management services and let us help you develop a personalized plan for long-term migraine pain management.




