Why Effective Headache Pain Management Matters
Headache pain management is essential, as headaches are one of the most common pain conditions globally. They are a leading cause of missed work and school, significantly impacting quality of life. About 40% of people experience tension-type headaches, while 10% suffer from migraines.
For those seeking relief, effective strategies include:
- Acute Treatment: Over-the-counter (OTC) pain relievers for mild headaches or prescription medications like triptans for migraines.
- Non-Drug Approaches: Cold compresses, rest, and stress-relief techniques.
- Preventive Strategies: A regular sleep schedule, avoiding triggers, and consistent exercise.
You should see a specialist if your headaches occur more than twice a week, disrupt daily life, or require pain medication more than nine days a month.
The challenge with headaches is that there are over 150 types, each requiring a unique treatment approach. What works for a tension headache may not help a migraine, and incorrect medication use can worsen the problem.
The good news is that with a proper diagnosis and a personalized plan, most headaches are manageable. Relief is often found through a combination of medications, lifestyle changes, and complementary therapies—without relying on opioids.
This guide will walk you through understanding your specific headache type, identifying your triggers, and finding the right treatment approach for lasting relief.
Understanding Your Headache: Types and Symptoms
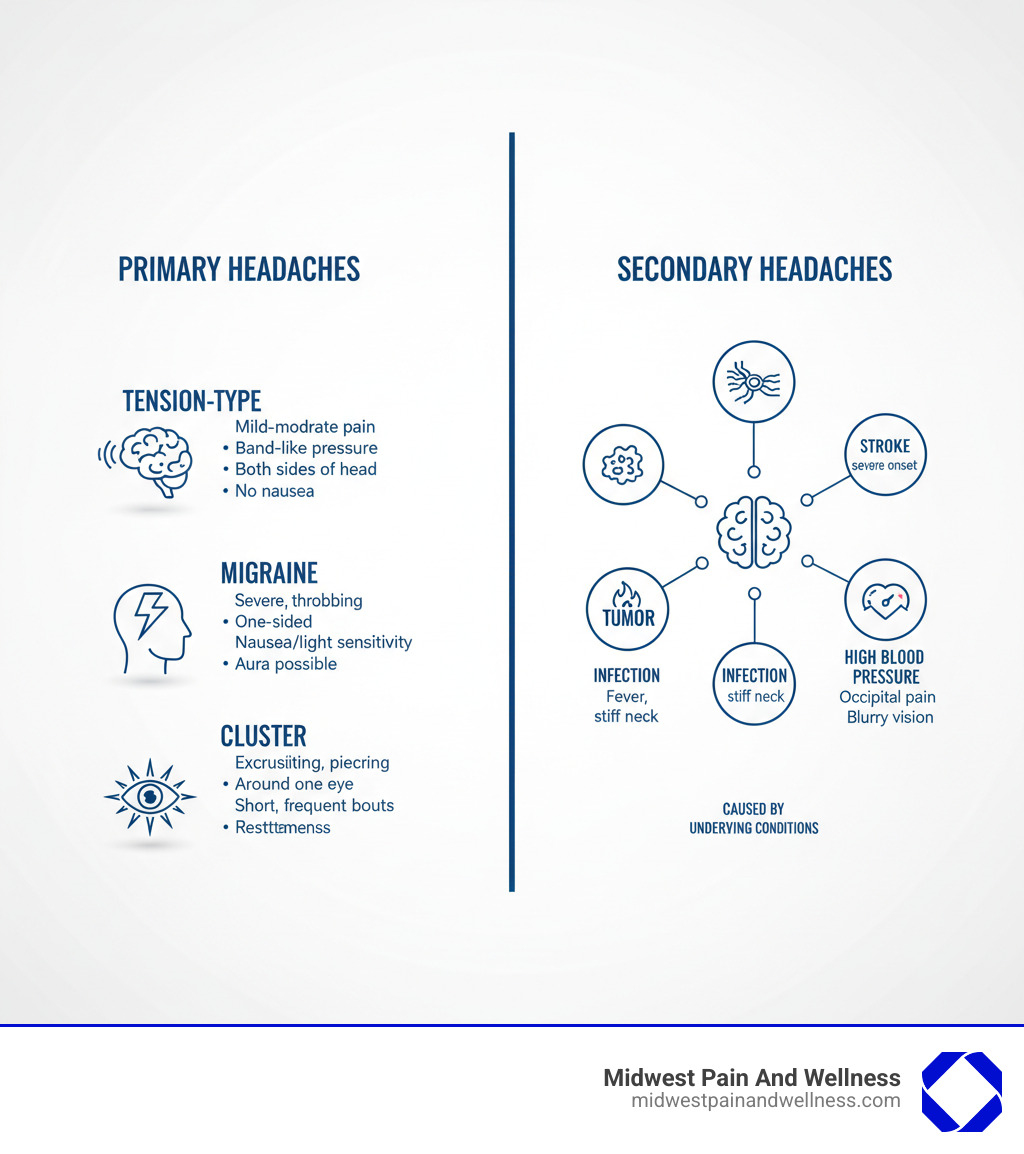
Getting the right treatment starts with understanding what kind of headache you’re dealing with. Doctors classify headaches into two main categories.
Primary headaches are the condition itself, not a symptom of another issue. Secondary headaches are caused by an underlying medical condition. This distinction is crucial because it dictates the treatment approach.
At Midwest Pain And Wellness, effective headache pain management begins with an accurate diagnosis. We identify your specific headache type to create a personalized treatment plan. Learn more about the conditions we treat and how we can help you find relief.
The three most common primary headaches are tension-type, migraine, and cluster headaches. While they all cause head pain, their characteristics, triggers, and treatments differ significantly.
| Feature | Tension-Type Headache | Migraine Headache | Cluster Headache |
|---|---|---|---|
| Prevalence | Most common (approx. 40% globally) | Common (approx. 10% globally) | Less common but severe |
| Pain Quality | Dull ache, pressure, tightness | Throbbing, pulsating, pounding | Excruciating, sharp, piercing, burning |
| Pain Severity | Mild to moderate | Moderate to severe | Severe, debilitating |
| Location | Usually both sides of the head (like a band) | Often one side, but can be both | Always one side, typically around the eye or temple |
| Duration | 30 minutes to a week | 4 to 72 hours (without treatment) | 15 minutes to 3 hours |
| Aggravated by | Not usually aggravated by physical activity | Routine physical activity, light, sound, smells | Restlessness, agitation |
| Associated Symptoms | None or mild sensitivity to light/sound | Nausea, vomiting, sensitivity to light (photophobia), sound (phonophobia), smells (osmophobia), aura (visual, sensory) | Tearing, red eye, nasal congestion, runny nose, sweating, drooping eyelid on affected side |
| Typical Triggers | Stress, lack of sleep, poor posture | Stress, hormonal changes, certain foods, lack of sleep, weather changes | Alcohol, nicotine, strong smells (during a cluster period) |
Tension-Type Headaches
Often described as a tight band around the head, tension-type headaches are the most common type, affecting about 40% of people globally. The pain is a dull, constant ache or pressure on both sides of the head and is typically mild to moderate. Unlike migraines, physical activity doesn’t usually worsen the pain.
Common triggers include stress, lack of sleep, and poor posture. While they can last from 30 minutes to a week, they become chronic when they occur 15 or more days per month, making professional headache pain management essential.
Migraine Headaches
Migraines are a complex neurological condition, not just a bad headache, affecting about 10% of the population and occurring three times more often in women than men. The pain is a moderate to severe throbbing or pulsating, usually on one side of the head.
Key symptoms that distinguish migraines include nausea, vomiting, and extreme sensitivity to light and sound. Physical activity typically worsens the pain, often requiring rest in a dark, quiet room. Some individuals experience an “aura” beforehand, which can involve visual disturbances or tingling sensations. A migraine attack can last from four to 72 hours without treatment.
Cluster Headaches
Cluster headaches are rare but severe and debilitating. They occur in cyclical patterns, or “clusters,” that can last for weeks or months. The pain is excruciating—a sharp, piercing, or burning sensation always on one side of the head, usually around the eye.
Unlike migraine sufferers who seek stillness, the intense pain often causes restlessness and agitation. Associated symptoms, all on the same side as the pain, include eye tearing, a red eye, nasal congestion, and a drooping eyelid. Attacks last from 15 minutes to three hours and can happen multiple times a day. Cluster headaches are more prevalent in men.
Uncovering the Root Cause: Common Triggers and Diagnosis
Identifying your headache triggers is a powerful step in headache pain management. Once you know the “why” behind your pain, you can begin to take control.

An accurate diagnosis is essential for differentiating between headache types and ruling out serious underlying conditions. Genetics can also play a role, as migraines often run in families. If your parents had migraines, your risk of developing them is higher.
Primary Causes and Triggers
Primary headaches arise from the overactivity of pain-sensitive structures in your head. These headaches are often set off by specific triggers. Identifying these is a key part of management. Common triggers include:
- Stress: Emotional and mental strain are major culprits for both tension-type headaches and migraines.
- Sleep Issues: Lack of quality sleep or a disrupted sleep schedule can lead to headaches.
- Poor Posture: Hunching over a desk or phone strains neck and shoulder muscles, often causing tension headaches.
- Diet and Hydration: Alcohol (especially red wine), dehydration, and skipping meals are common triggers. Certain foods containing nitrates or MSG can also be problematic.
- Caffeine: Both excessive caffeine intake and caffeine withdrawal can trigger headaches.
- Environmental Factors: Strong smells, bright lights, loud noises, and weather changes can set off headaches for many people.
How Headaches Are Diagnosed
An accurate diagnosis is the cornerstone of effective headache pain management. Our process begins with understanding your unique headache experience.
- Medical History: We start with a detailed conversation about your headache symptoms (pain quality, location, frequency, duration), triggers, and family history.
- Physical and Neurological Exam: These exams assess your general health and check neurological functions like reflexes, sensation, and coordination to rule out underlying issues.
- Headache Journal: We often recommend keeping a headache journal. Tracking your symptoms, diet, stress levels, and sleep patterns helps identify triggers and guides your diagnosis and treatment plan.
- Diagnostic Tests: While imaging like CT scans or MRIs isn’t usually needed for primary headaches, we may order these tests if a secondary headache is suspected. This is to rule out serious conditions like tumors or aneurysms and ensure we are treating the correct cause.
Comprehensive Headache Pain Management Strategies
At Midwest Pain And Wellness, we create custom care plans that address your unique situation. Our double board-certified doctors use a multi-modal, interventional approach to provide comprehensive, opioid-free headache pain management for long-term relief.
Headache treatment involves two main strategies: acute treatments for immediate relief when a headache strikes, and preventive treatments to reduce their frequency and severity. We prioritize non-opioid therapies, which are effective and safer for long-term use, aligning with CDC recommendations. Their Non-Opioid Therapies for Pain: A Clinical Reference confirms that non-opioid options work well for many types of pain, including headaches.
Acute and Preventive Medication Approaches
Medications are powerful tools for both stopping a headache in its tracks (acute treatment) and reducing their frequency (preventive treatment).
For immediate relief (Acute Treatment):
- Mild to Moderate Headaches: Over-the-counter (OTC) options like ibuprofen, naproxen (NSAIDs), or acetaminophen are often effective. However, overuse can lead to more headaches.
- Severe Headaches & Migraines: Prescription medications are often necessary. Triptans are a first-line treatment for migraines and work best when taken early. Newer options like gepants and lasmiditan offer alternatives. For associated nausea, antiemetics can provide relief.
For long-term prevention (Preventive Treatment):
If headaches are frequent or severe, daily preventive medication can dramatically improve quality of life. Options include:
- Beta-blockers and certain antidepressants (like amitriptyline).
- Anticonvulsants (like topiramate).
- CGRP inhibitors, a newer class of medication that specifically targets a key pathway in migraines.
- Botulinum toxin (Botox) injections for chronic migraines.
The Mayo Clinic offers an excellent resource on how treatment depends on your specific diagnosis and symptoms: Headaches: Treatment depends on your diagnosis and symptoms%20and%20zolmitriptan%20(Zomig)).
Lifestyle Modifications and Complementary Therapies for Headache Pain Management
Medication is just one piece of the puzzle. Lifestyle and complementary therapies are powerful tools for headache pain management.
- Stress Management: Techniques like deep breathing, mindfulness, and yoga can reduce the tension that leads to headaches. Cleveland Clinic offers great insights into Relaxation techniques.
- Biofeedback: This technique teaches you to control bodily functions like muscle tension, helping you prevent tension-type headaches.
- Regular Exercise and Sleep: Consistent, moderate physical activity and a regular sleep schedule help regulate your body and can reduce headache frequency and intensity.
- Diet and Hydration: Eating regular meals, staying hydrated, and avoiding known food triggers are simple yet effective strategies.
- Physical Therapy and Massage: For headaches linked to muscle tension, physical therapy can improve posture, while therapeutic massage can relieve tension in the head, neck, and shoulders.
- Acupuncture: Some people find acupuncture helpful for chronic pain, including certain types of headaches.
Advanced and Chronic Headache Pain Management
For chronic daily headaches (15+ days a month) or migraines that don’t respond to conventional treatments, we offer advanced solutions through our multi-modal, interventional approach.
- Interventional Procedures: These treatments provide targeted relief. Nerve blocks, injections of local anesthetic near specific nerves (like the occipital nerve), can interrupt pain signals. For chronic migraines, FDA-approved Botox injections can significantly reduce headache days. We offer this specialized treatment in Chicago Ridge, Illinois. Learn more about Botox for Chronic Migraine, Cervical Dystonia in Chicago Ridge.
- Neuromodulation: These emerging non-invasive therapies alter nerve activity with electrical or magnetic pulses to treat and prevent migraines.
- CGRP Inhibitors: These targeted medications are a breakthrough for many people with chronic migraines.
We stay current with the latest research to offer the most effective options. Explore our comprehensive Procedures We Use For Treatment.
Understanding Medication Overuse Headache
Ironically, the medications used to stop headaches can cause them if taken too often. This is called Medication Overuse Headache (MOH) or “rebound headache.” It develops from the frequent use of acute pain relievers, creating a cycle where the end of the medication’s effect triggers a new headache.
MOH is defined as headaches on 15 or more days a month in someone overusing acute medication. The situation can be complicated by other conditions like Opioid-induced hyperalgesia (OIH), where pain sensitivity increases with long-term opioid use.
Breaking the cycle requires stopping the overused medication under professional guidance. Our doctors will help you through this process with a plan that may include gradual withdrawal, starting a preventive medication, and supportive care. Attempting to stop medications abruptly can be unsafe, so we work with you to create a plan for healthier headache pain management.
Recognizing Red Flags: When to Seek Immediate Medical Help
Most headaches are not dangerous, but some can be a warning of a more serious issue. Knowing the difference is a key part of headache pain management.

Your brain itself can’t feel pain, so a headache is a signal from surrounding nerves and tissues. Usually, it’s a response to a simple trigger, but occasionally it’s an alert for a medical emergency. Recognizing “red flag” symptoms empowers you to take prompt action.
Emergency Headache Symptoms
Some headache symptoms require a trip to the emergency room or a 911 call. Seek immediate medical evaluation for:
- A sudden, severe “thunderclap” headache that reaches maximum intensity within a minute. This can signal bleeding in the brain.
- Any headache following a head injury, especially if it worsens.
- A headache accompanied by a fever and stiff neck, which could be meningitis.
- Neurological symptoms like sudden weakness or numbness (especially on one side), difficulty speaking, vision loss, confusion, or loss of balance. These could indicate a stroke.
- A headache that occurs with a seizure.
- A new type of headache after age 50, one that steadily worsens, or one accompanied by a rash or severe eye or ear pain.
It’s always better to be cautious. If you experience any of these red flag symptoms, seek help immediately.
Complications of Poorly Managed Headaches
When headaches are not managed effectively, the consequences extend beyond pain. Poorly managed headaches can lead to:
- Reduced Quality of Life: Chronic pain can interfere with social activities, hobbies, and family time.
- Change to Chronic Headaches: Untreated episodic headaches can become chronic (occurring 15+ days a month), making them much harder to treat.
- Mental Health Issues: There is a strong link between chronic pain and the development of depression and anxiety, which can in turn worsen headaches.
- Professional and Personal Strain: Headaches are a leading cause of missed work and school, affecting productivity and relationships.
- Medication Overuse Headache: As discussed, trying to self-manage frequent headaches with OTC pain relievers can lead to a rebound cycle that worsens the problem.
This is why working with a specialist for consistent headache pain management is so important. A proper diagnosis and treatment plan can prevent these complications and help you reclaim your life.
Conclusion
Living with headache pain doesn’t have to be your normal. Effective headache pain management is achievable. The path to relief begins with a proper diagnosis to understand your specific headache type, as treatment is not one-size-fits-all.
A multi-modal approach is key, combining preventive and acute medications with lifestyle changes and complementary therapies. For those with chronic or severe headaches, advanced interventional procedures like nerve blocks or Botox can provide the breakthrough you need.
At Midwest Pain And Wellness, our philosophy is centered on comprehensive, opioid-free pain management. Our double board-certified doctors create custom care plans for long-term relief, addressing the root causes of your pain and empowering you to take control of your health.
You’ve taken the first step by learning about your options. Now, turn that knowledge into action. Whether your headaches are occasional or chronic, specialized care can make a profound difference.
Ready to start your journey toward lasting relief? Explore our advanced treatment procedures to see how our comprehensive approach can help you reclaim your life from headache pain.




