Why Post-Laminectomy Pain Treatment Matters for Your Recovery
Post-Laminectomy Pain Treatment addresses persistent or recurring pain after spinal surgery, a condition affecting up to 20 percent of patients who undergo procedures like laminectomy. Here’s what you need to know:
Key Treatment Options:
- Epidural steroid injections – Provide significant relief for discogenic back pain
- Radiofrequency ablation – Targets specific nerve pathways causing pain
- Spinal cord stimulation – Advanced neuromodulation for chronic nerve pain
- Multimodal pain management – Combines NSAIDs, physical therapy, and nerve blocks
- Physical rehabilitation – Core strengthening and mobility exercises
When to Seek Treatment:
- Pain similar to pre-surgery symptoms
- Sharp, stabbing sensations radiating into legs
- Numbness, tingling, or muscle weakness
- Pain that worsens 6-12 weeks after surgery
You expected relief after back surgery. Instead, the pain persisted—or even returned. This frustrating reality is called post-laminectomy syndrome, also known as failed back surgery syndrome. It doesn’t mean your surgery was a failure or that nothing can be done. It means the underlying pain generators weren’t fully addressed, or new issues developed during healing.
The good news? Modern interventional treatments can target the specific source of your pain without requiring another major surgery. From precise nerve blocks to advanced neuromodulation, today’s approaches focus on restoring your quality of life through minimally invasive, personalized care.
Common causes include scar tissue pressing on nerves (epidural fibrosis), recurrent disc problems, spinal instability, or nerve damage. The pain might feel dull and achy in your back, or sharp and electric down your legs. Some patients experience numbness or weakness that limits walking, standing, or even sleeping.
The most important first step is accurate diagnosis. Advanced imaging like MRI and fluoroscopy, combined with physical examination, helps pinpoint exactly what’s causing your pain. This precision allows for targeted treatment rather than trial-and-error approaches.
I’m Dr. Yaw Donkoh, a double board certified physician in anesthesiology and interventional pain management at Midwest Pain And Wellness. With fellowship training from the University of Iowa Hospitals and years of experience in Post-Laminectomy Pain Treatment, I focus on evidence-based, minimally invasive procedures that help patients reclaim their lives without relying on opioids or repeat surgeries. Our approach combines careful diagnosis with personalized treatment plans designed around your specific pain generators and recovery goals.
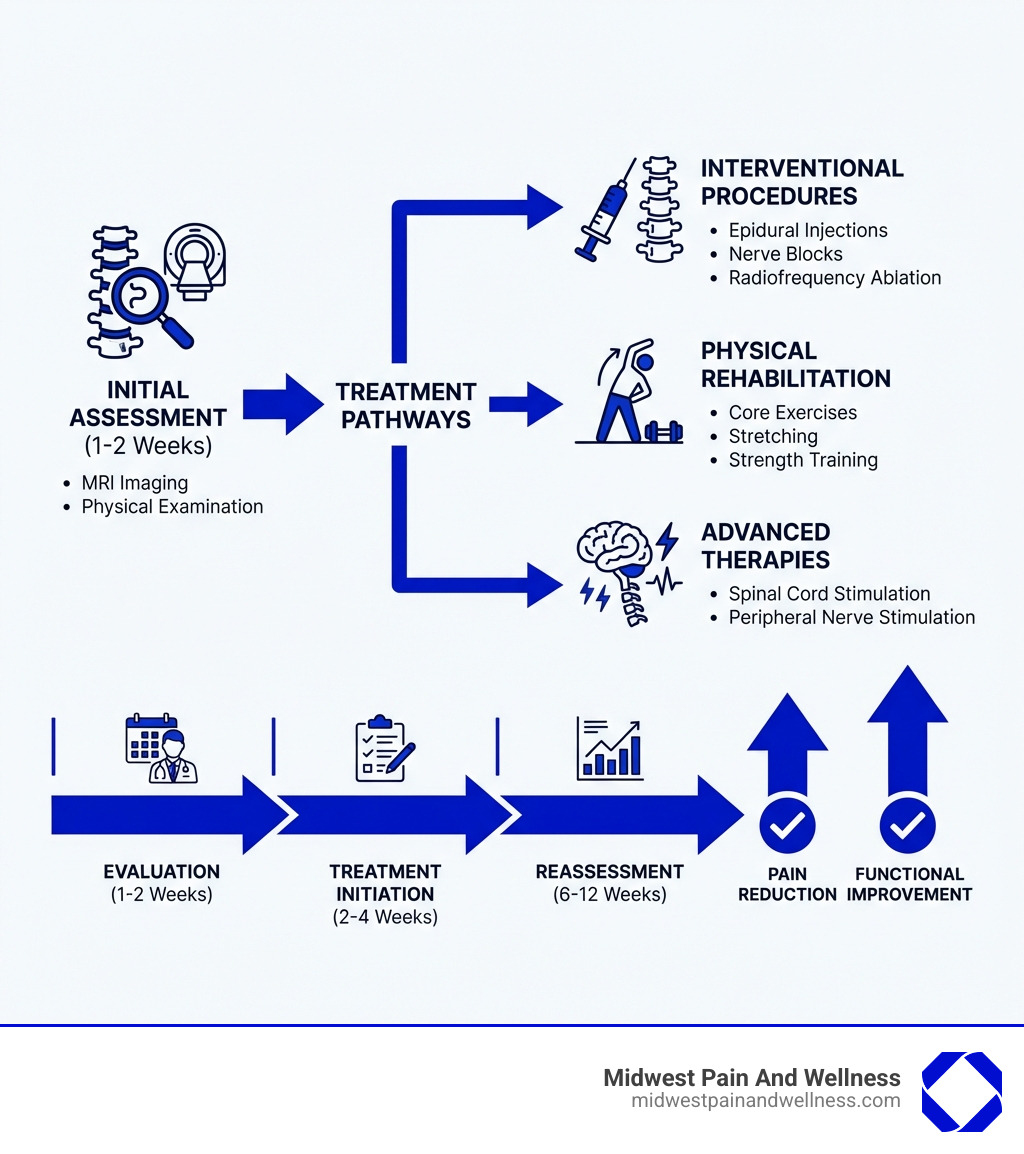
Understanding Post-Laminectomy Syndrome and Its Causes
When we talk about Post-Laminectomy Pain Treatment, it’s crucial to first understand what post-laminectomy syndrome (PLS) truly is. It’s not a simple diagnosis, but rather a complex condition describing persistent back or neck pain that can also affect the arms and legs after spinal surgery. While the term “failed back surgery syndrome” (FBSS) is sometimes used, we prefer to focus on PLS as it emphasizes the post-surgical nature of the pain, rather than implying the surgery itself was a failure.
This syndrome affects a significant number of people. Statistics show that up to 20 percent of Americans who undergo spinal surgery each year experience some degree of persistent back or neck pain. This means that for many, the relief they hoped for doesn’t fully materialize.
What causes this lingering discomfort? The reasons are varied and often multifaceted. Sometimes, the underlying pain generators weren’t completely resolved during the initial surgery, or new problems emerged as the spine healed. Here are some common culprits we identify when developing a Post-Laminectomy Pain Treatment plan:
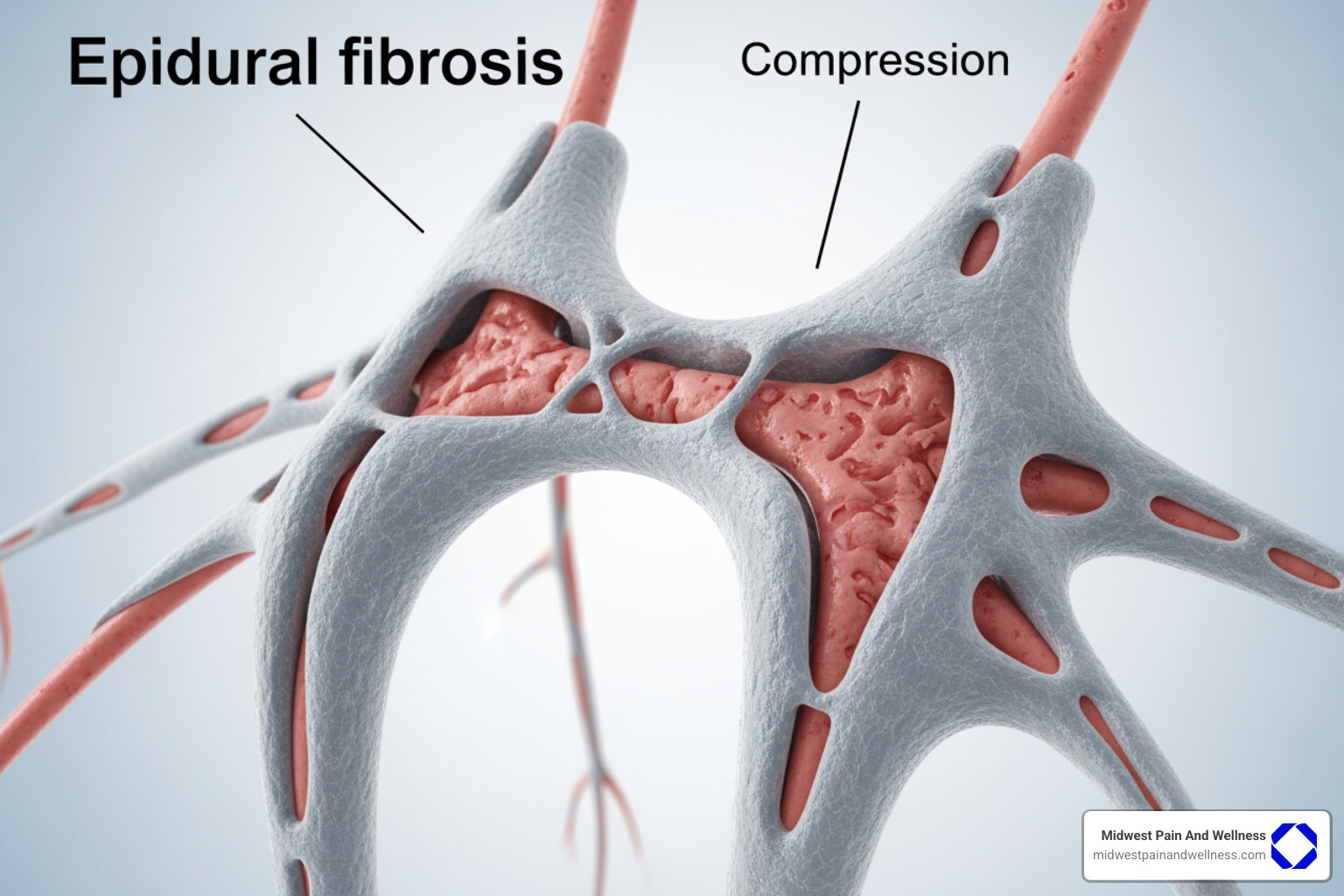
- Scar Tissue Formation (Epidural Fibrosis): This is a prominent theory for persistent pain. After any surgery, the body naturally forms scar tissue. In spinal surgery, this can lead to epidural fibrosis, where scar tissue develops around the nerve roots, potentially compressing them or restricting their movement. Symptoms often appear about 6 to 12 weeks after the procedure, presenting as a burning pain that doesn’t change with position.
- Recurrent Stenosis: Even after a laminectomy to decompress the spinal canal, bone can sometimes grow back, causing a recurrence of spinal stenosis and leading to renewed pressure on nerves. This can also happen if there were technical issues during the initial surgery, leading to incomplete decompression. If you’re experiencing symptoms of spinal stenosis, you can learn more about it on our dedicated page: More info about spinal stenosis.
- Spinal Instability: Removing parts of the spine during procedures like discectomy or laminectomy, especially if the spine was already unstable, can sometimes create greater instability in that area, leading to pain.
- Nerve Damage or Persistent Nerve Changes: Even if nerve compression is successfully relieved, the nerve itself might have suffered damage or residual changes that continue to send pain signals. This can manifest as neuropathic pain.
- Adjacent Segment Disease: This occurs primarily after spinal fusion surgery. When one segment of the spine is fused, the adjacent segments above and below compensate for the reduced mobility. This increased stress can lead to accelerated degeneration of these neighboring discs and joints, causing new pain.
- Arachnoiditis: This is a more severe and rare condition involving inflammation of the arachnoid membrane, one of the protective coverings of the spinal cord and nerves. It can result from surgery, infection, or other spinal trauma, leading to severe, chronic pain and neurological symptoms.
Beyond these direct surgical consequences, certain lifestyle factors can significantly contribute to the risk and severity of post-laminectomy syndrome. One of the most impactful is smoking. Recent studies, including scientific research on smoking and surgical outcomes, show that individuals who smoke are more likely to develop post-laminectomy syndrome. Nicotine interferes with bone metabolism and blood vessel constriction, which can hinder proper healing and increase scar tissue formation, making it less likely for patients to experience complete pain eradication after spinal surgery. Some surgeons may even decline to operate on active smokers due to these known risks.
Identifying Symptoms of Persistent Pain
The symptoms of post-laminectomy syndrome are as varied as its causes. When we evaluate patients for Post-Laminectomy Pain Treatment, we listen carefully to their descriptions of pain, as this helps us narrow down the potential sources.
Common symptoms include:
- Axial Pain: This is pain felt directly in the spine, either in the lower back (lumbar) or neck (cervical) region. It often feels dull and achy and can be caused by muscle spasm, facet joint arthritis, residual disc herniation, or issues with surgical hardware.
- Radiculopathy: This refers to pain that radiates from the spine into the extremities (legs or arms). It’s often described as sharp, pricking, or stabbing, similar to sciatica. This type of pain indicates nerve root irritation or compression.
- Neuropathic Sensations: Injured nerves can produce a range of unusual sensations, such as burning, tingling, numbness, feelings of heat or cold, or even an electric shock-like sensation.
- Muscle Weakness and Numbness: Patients may experience a feeling of heaviness, actual loss of strength, or persistent numbness in the leg or foot.
- Mobility Issues: The pain can be severe enough to limit daily activities, making it difficult to walk, sit for long periods, sleep comfortably, or participate in exercise.
Sometimes, the pain might be identical to what you experienced before surgery, indicating that the original problem wasn’t fully resolved. Other times, it might be a new type of pain, signaling a new issue. Understanding the nuances of these symptoms is critical for effective Post-Laminectomy Pain Treatment. For those dealing with issues like disc degeneration, which can lead to these kinds of symptoms, we have more information available: More info about degenerative disc disease.
Diagnostic Tools for Post-Laminectomy Pain Treatment
Accurate diagnosis is the cornerstone of effective Post-Laminectomy Pain Treatment. Without precisely identifying the source of your pain, treatment can be a shot in the dark. At Midwest Pain And Wellness, we employ a thorough and systematic approach to evaluation, ensuring we leave no stone unturned.
Our diagnostic process typically includes:
- Comprehensive Physical Examination: Our specialists conduct a meticulous physical exam, assessing your posture, range of motion, muscle strength, reflexes, and sensation. This helps us identify areas of tenderness, muscle spasm, and neurological deficits.
- Detailed Neurological Assessment: This specific part of the exam helps us pinpoint which nerves might be affected and the extent of any nerve damage.
- Advanced Imaging Studies:
- X-rays: Provide views of bone structure and alignment, helping to identify spinal instability or hardware issues.
- MRI (Magnetic Resonance Imaging): Excellent for visualizing soft tissues like discs, nerves, and scar tissue. An MRI can reveal recurrent disc herniation, epidural fibrosis compressing nerves, or inflammation.
- CT Scans (Computed Tomography): Offer detailed images of bone, which are particularly useful for assessing bone regrowth (recurrent stenosis) or the integrity of surgical hardware.
- EMG (Electromyogram): This test measures the electrical activity of muscles and nerves. It can help detect nerve damage, nerve root compression, or other neurological issues contributing to your pain.
Identifying the exact nerve or tissue involved is paramount for precise and measurable progress in your Post-Laminectomy Pain Treatment. If you’re looking for expert guidance, our team of specialists is here to help: More info about our back pain specialists.
The Role of Imaging in Post-Laminectomy Pain Treatment
Beyond standard imaging, we often use specialized techniques to get a clearer picture of your pain generators.
- Fluoroscopy: This is a type of X-ray that shows a continuous X-ray image on a monitor, much like a movie. We use fluoroscopy to guide diagnostic injections precisely to the suspected pain source. This ensures that the medication reaches the correct area, confirming the diagnosis and often providing immediate, albeit temporary, relief.
- Ultrasound: In some cases, ultrasound can be used to visualize soft tissues and guide injections, especially for peripheral nerve issues or muscle-related pain.
These advanced imaging techniques help us to accurately identify issues such as nerve root compression, the presence and location of scar tissue, or potential hardware failure. This precision allows us to move forward with targeted and effective treatment plans. To learn more about the procedures we use, visit: More info about our procedures.
Clinical Evaluation for Post-Laminectomy Pain Treatment
Our clinical evaluation goes beyond imaging. We conduct:
- Diagnostic Blocks: These are minimally invasive procedures where a small amount of local anesthetic is injected into a specific nerve or joint. If the injection temporarily relieves your pain, it confirms that the targeted structure is indeed the source of your discomfort. This is an invaluable tool in guiding our Post-Laminectomy Pain Treatment strategies.
- Detailed Patient History: We take the time to understand your medical history, the nature of your previous surgery, the onset and characteristics of your current pain, and how it impacts your daily life. We also discuss your previous treatments and their effectiveness.
- Mobility Testing: Observing your movement patterns, flexibility, and identifying positions or activities that exacerbate or alleviate your pain provides crucial insights.
Our team of double board-certified physicians collaborates to ensure a comprehensive and accurate diagnosis. We believe that a thorough understanding of your unique situation is the first step toward lasting relief. You can learn more about the dedicated professionals who will guide your recovery here: More info about our team.
Interventional and Non-Surgical Treatment Strategies
Once we have a clear diagnosis, we can develop a personalized Post-Laminectomy Pain Treatment plan. Our philosophy at Midwest Pain And Wellness centers on comprehensive, opioid-free pain management using current, evidence-based therapies. We use a multi-modal, interventional approach, collaborating with other practitioners to create custom care plans for long-term pain relief.
What are the recommended pain management strategies for post-laminectomy syndrome, including pharmacological and non-pharmacological approaches?
Pharmacological Approaches:
- Paracetamol (Acetaminophen) and NSAIDs (Non-Steroidal Anti-Inflammatory Drugs) or COX-2 Inhibitors: These are often the first line of defense for pain and inflammation. For lumbar laminectomy, it’s recommended that paracetamol and an NSAID or COX-2 selective inhibitor be administered preoperatively or intraoperatively and continued post-operatively.
- Opioids: While effective for acute pain, opioids are generally reserved for rescue analgesia post-operatively, used with caution and for short durations. We’re very careful with opioids due to their unpredictable responses, potential for dangerous side effects, and the risk of developing opioid-induced hyperalgesia (where long-term use can paradoxically increase pain sensitivity). Some effective interventions, like gabapentinoids and intrathecal opioid administration, carry significant risks and are often omitted from general recommendations due to these concerns.
- Anti-convulsants and Anti-depressants: For neuropathic pain (nerve-related pain), medications typically used for seizures or depression can be very effective in modulating nerve signals and reducing pain.
Non-Pharmacological Approaches:
- Physical Therapy and Rehabilitation: This is a cornerstone of Post-Laminectomy Pain Treatment. It includes specialized exercises for core stabilization, stretching, and strengthening. Physical therapy helps improve mobility, reduce muscle spasms, and educate patients on proper body mechanics to prevent re-injury. We encourage active patient participation in their recovery.
- Lifestyle Modifications: Adjustments such as smoking cessation, weight management, and ergonomic changes can significantly impact pain levels and overall recovery.
What interventional pain management techniques are available for post-laminectomy syndrome?
Interventional pain management techniques are a key component of our approach, targeting pain precisely with minimally invasive procedures.
- Epidural Steroid Injections (ESIs): These injections deliver anti-inflammatory medication directly into the epidural space around the spinal nerves. ESIs show significant benefit for discogenic back pain and can provide effective short-term pain relief. Research suggests a lateral approach is often superior to a midline approach for ESIs. While generally safe, ESIs do have potential complications, which we discuss thoroughly with our patients.
- Nerve Blocks: These involve injecting a local anesthetic and/or steroid near specific nerves to block pain signals. For example, lumbar medial branch blocks can be performed under CT or fluoroscopy guidance to diagnose and treat facet joint pain. You can learn more about nerve blocks here: More info about nerve blocks.
- Radiofrequency Ablation (RFA): If a diagnostic nerve block successfully relieves pain, RFA might be recommended. This procedure uses heat generated by radiofrequency waves to “turn off” the pain signals from specific nerves. Lumbar medial branch radiofrequency ablations can be performed on patients with recurrent pain, typically providing relief for six to twelve months.
- Adhesiolysis: This procedure targets scar tissue (adhesions) that may be compressing nerves, breaking it down to free the affected nerves.
The American Society of Pain and Neuroscience (ASPN) provides Evidence-Based Clinical Guidelines for interventional treatments for low back pain, which we follow to ensure our practices are aligned with the latest scientific recommendations. We are committed to providing non-surgical pain relief whenever possible: More info about non-surgical pain relief.
Advanced Neuromodulation for Post-Laminectomy Pain Treatment
For individuals with persistent, chronic neuropathic pain that hasn’t responded to other treatments, advanced neuromodulation techniques can offer significant relief.
- Spinal Cord Stimulation (SCS): This innovative therapy involves implanting a small device that sends mild electrical pulses to the spinal cord, interrupting pain signals before they reach the brain. SCS is a proven treatment for chronic neuropathic pain, including that associated with post-laminectomy syndrome. Patients often undergo a trial period with an external device to ensure effectiveness before permanent implantation.
- Peripheral Nerve Stimulation (PNS): Similar to SCS, PNS targets specific peripheral nerves outside the spinal cord. This can be beneficial for localized neuropathic pain.
These advanced therapies are designed to provide long-term pain relief, significantly improving quality of life for many of our patients. To explore if SCS is right for you, visit: More info about spinal cord stimulator therapy.
Pharmacological and Physical Therapy Approaches
While interventional treatments are powerful, they are often most effective when integrated into a broader Post-Laminectomy Pain Treatment plan that includes medication management and active rehabilitation.
- Optimized Medication Regimen: As mentioned, we strategically use medications like NSAIDs, paracetamol, and COX-2 inhibitors for baseline pain and inflammation. For nerve pain, anti-convulsants or anti-depressants can be invaluable. We carefully monitor and adjust medication to minimize side effects and prevent issues like opioid-induced hyperalgesia. Our goal is to reduce reliance on strong pain medications while still providing effective relief.
- Physical Therapy and Active Rehabilitation: This is not just about exercises; it’s about re-educating your body. Our physical therapy programs focus on:
- Core Stabilization: Strengthening the muscles that support your spine is crucial for stability and reducing strain.
- Stretching and Flexibility: Improving range of motion helps alleviate stiffness and muscle tension.
- Strength Training: Building overall strength supports better posture and reduces the burden on your spine.
- Ergonomics and Body Mechanics: Learning how to move, lift, and sit correctly protects your back from further injury.
We believe that empowering patients with the knowledge and tools for self-management is key to long-term success. Our approach to chronic pain treatment is holistic and patient-centered: More info about chronic pain treatment.
Frequently Asked Questions about Post-Laminectomy Pain
We understand that living with persistent pain after surgery can raise many questions and concerns. Here, we address some of the most common ones we hear from our patients seeking Post-Laminectomy Pain Treatment.
Is a second surgery necessary for post-laminectomy syndrome?
This is a question that weighs heavily on many patients. Our general stance is that revision surgery should only be considered after a thorough evaluation identifies specific, correctable problems that can be addressed surgically. It’s not a decision to be taken lightly, as each subsequent surgery carries increased risks.
Situations where a second surgery might be considered include:
- Recurrent Disc Herniation: A new disc herniation at or near the operated level.
- New Spinal Instability: If the first surgery led to new instability that can be surgically corrected.
- Hardware Malfunction: Issues with previously implanted screws, rods, or other devices.
- Progressive Spinal Stenosis: If bone regrowth or other factors have led to severe recurrent stenosis.
Before recommending another surgery, we exhaust all appropriate conservative and interventional Post-Laminectomy Pain Treatment options. Our focus is always on the least invasive yet most effective solutions. For certain conditions, minimally invasive decompression techniques might be an option: More info about minimally invasive decompression.
How long does it take for nerves to heal after surgery?
Nerve healing is a complex process, and unfortunately, it often takes longer than the resolution of surgical pain. While some patients experience rapid improvement, it’s common for numbness and tingling to persist longer than the initial pain. In 10-20% of cases, pain continues until the nerve fully heals, which can take weeks to months.
Several factors influence nerve recovery and your overall prognosis:
- Severity of Initial Nerve Compression/Damage: More severe or prolonged compression typically means a longer recovery time.
- Underlying Cause of PLS: The specific reason for your persistent pain (e.g., scar tissue vs. new disc herniation) impacts recovery.
- Patient’s Overall Health: Conditions like diabetes can impair nerve healing.
- Adherence to Treatment Plan: Diligently following physical therapy and lifestyle recommendations significantly aids recovery.
- Smoking Status: As mentioned, smoking can impede healing processes, including nerve recovery.
For individuals facing persistent pain, recovery is a journey. We are here to guide you through it, managing your pain and supporting your healing every step of the way. We treat a wide range of conditions, and you can learn more about them here: More info about conditions we treat.
Can lifestyle changes reduce post-surgical pain?
Absolutely! Lifestyle modifications and active patient participation are incredibly powerful tools in Post-Laminectomy Pain Treatment and prevention. You have a significant role to play in your recovery and long-term well-being.
- Smoking Cessation: This is perhaps one of the most critical preventative measures. Research consistently shows that individuals who smoke have poorer surgical outcomes and a higher risk of developing PLS. Quitting smoking improves blood flow, promotes healing, and reduces inflammation, all of which are vital for pain reduction.
- Weight Management: Excess body weight, especially around the abdomen, places additional strain on the spine, potentially exacerbating back pain. Achieving and maintaining a healthy weight can significantly alleviate this burden.
- Ergonomic Adjustments: Paying attention to your posture and workstation ergonomics can prevent unnecessary stress on your spine. This includes proper chair support, monitor height, and regular breaks to move and stretch.
- Regular, Appropriate Exercise: While rest is important immediately after surgery, gradually increasing activity through walking and prescribed physical therapy exercises is crucial. Strengthening your core muscles provides essential support for your spine.
- Healthy Diet and Hydration: A balanced diet rich in anti-inflammatory foods can support healing. Staying well-hydrated and consuming enough fiber is also important to prevent constipation, which can cause straining and discomfort in the healing back.
Actively engaging in these lifestyle changes not only helps manage existing pain but can also reduce the risk of future spinal issues. We offer comprehensive pain management strategies, including guidance on lifestyle modifications, to patients in Naperville and surrounding areas: More info about pain management in Naperville.
Conclusion
Living with persistent pain after a laminectomy can be incredibly challenging, but you don’t have to face it alone. At Midwest Pain And Wellness, we understand the complexities of Post-Laminectomy Pain Treatment and are dedicated to providing compassionate, evidence-based care. Our double board-certified physicians, led by Dr. Yaw Donkoh, specialize in diagnosing and treating this intricate condition with a focus on restoring your quality of life.
We pride ourselves on offering comprehensive, opioid-free pain management solutions, utilizing a multi-modal and interventional approach. This means we combine the latest diagnostic tools with advanced, minimally invasive treatments—from precise injections and nerve blocks to state-of-the-art spinal cord stimulation. We believe in creating custom care plans custom to your unique needs, collaborating with other healthcare professionals to ensure you receive the most effective and holistic treatment possible.
Our goal is not just to alleviate your pain temporarily, but to empower you with lasting relief, helping you return to the activities you love and live a fuller, more active life.
If you are experiencing persistent pain after spinal surgery, don’t let it linger. We invite you to explore the possibilities of modern Post-Laminectomy Pain Treatment with us. Take the first step towards a pain-free future by contacting our clinic.
Schedule your Post-Laminectomy Pain Treatment in Chicago Ridge