Understanding the Impact of Migraine and Why Prevention Matters
How to prevent migraine headaches? Prevention strategies include:
- Identify and avoid personal triggers – Keep a headache diary to track foods, stress, sleep patterns, and environmental factors
- Maintain consistent lifestyle habits – Regular sleep schedule, meal times, and exercise routine
- Manage stress effectively – Practice relaxation techniques, meditation, or cognitive behavioral therapy
- Consider preventive medications – Beta-blockers, anticonvulsants, antidepressants, or CGRP inhibitors if attacks occur frequently
- Stay hydrated and exercise regularly – Aerobic activities like walking or cycling for 15-20 minutes daily
- Explore interventional treatments – Botox injections for chronic migraine, nerve blocks, or biofeedback therapy
Migraines aren’t just bad headaches. They’re a disabling neurological condition that affects more than four million adults with chronic migraine in the United States alone. The throbbing pain, nausea, and extreme sensitivity to light and sound can last anywhere from hours to days, forcing people to retreat to dark, quiet rooms and miss work, family events, and everyday activities.
Migraines affect women three times more often than men, and most people experience their first attack between ages 10 and 40. The condition is actually the second leading cause of disability worldwide, but here’s the encouraging news: preventive treatment decreases migraine frequency by 50% in approximately 50% of patients who try it.
The key to prevention lies in understanding that migraines progress through distinct stages and respond to multiple intervention points. Some people can manage their condition through lifestyle changes alone, while others benefit from a combination of behavioral strategies and medical treatments.
I’m Dr. Yaw Donkoh, double board-certified in anesthesiology and interventional pain management, and I’ve helped countless patients develop personalized plans for how to prevent migraine headaches through a comprehensive, minimally invasive approach. At Midwest Pain and Wellness, we focus on identifying your unique triggers and creating treatment strategies that reduce attack frequency without relying on opioids.
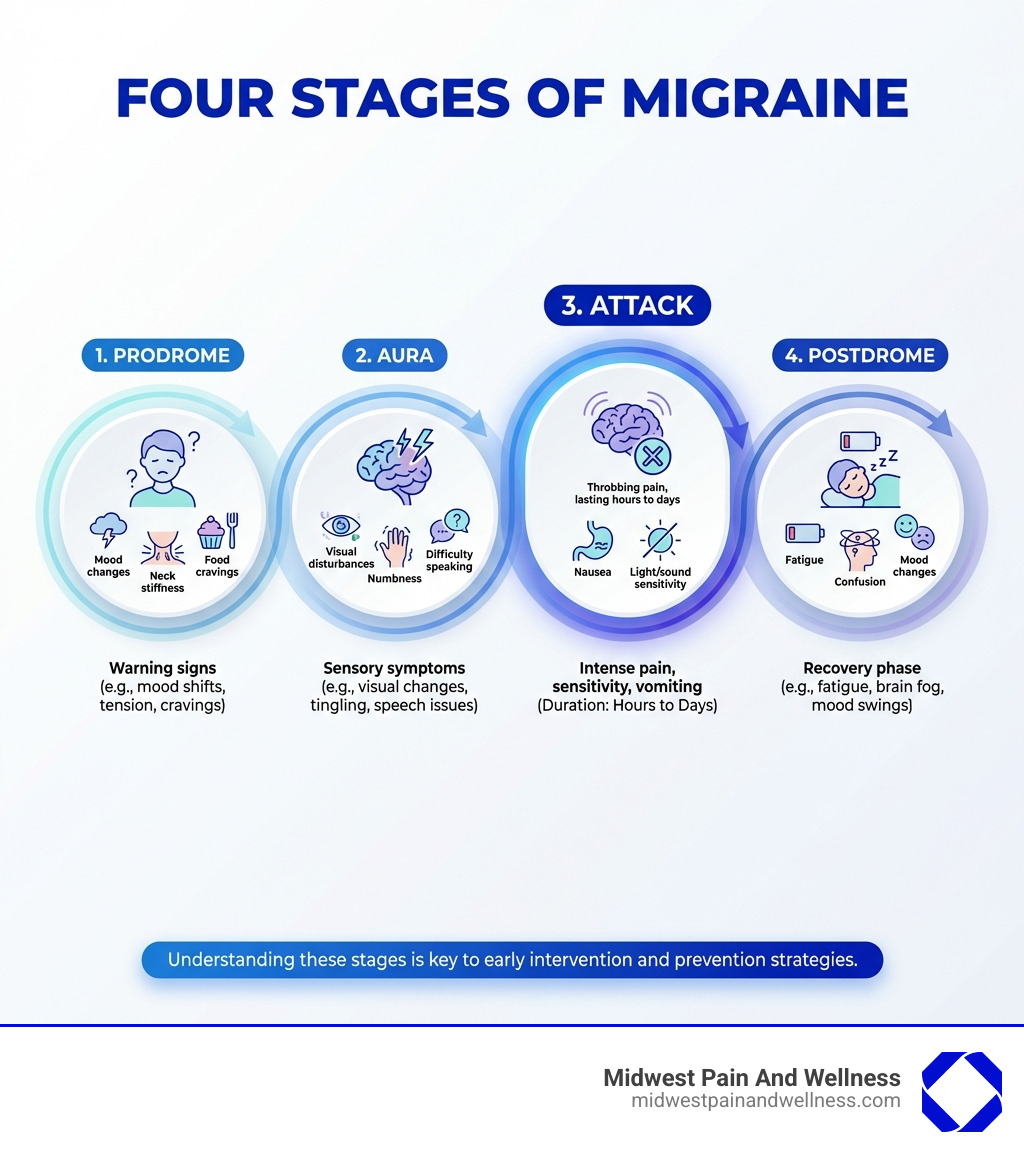
Identifying and Avoiding Common Migraine Triggers
Understanding what sets off your migraines is the cornerstone of prevention. While the underlying cause of migraine remains a mystery, specific stimuli, known as triggers, can make an attack more likely. Think of it like a light switch: the migraine is the light, and triggers are what flip the switch. Often, it’s not a single trigger but a combination that pushes you over the edge.
Common triggers for migraine headaches can vary widely from person to person, but some frequently reported culprits include:
- Fatigue and Sleep Disturbances: Irregular sleep patterns, too little or too much sleep can be a major factor.
- Hormonal Changes: Fluctuations in estrogen, especially around menstrual cycles, pregnancy, or menopause, are significant triggers for many women.
- Sensory Overload: Bright or flickering lights, loud noises, and strong smells (like perfumes or chemicals) can overwhelm the nervous system and initiate an attack.
- Stress: While stress itself is a trigger, sometimes the “let-down” period after intense stress can also trigger a migraine.
- Weather Changes: Barometric pressure changes, storms, or extreme heat can affect some individuals.
- Dietary Factors: Certain foods and drinks are often cited as triggers, which we’ll explore in more detail.
- Dehydration: Not drinking enough water can leave you vulnerable to an attack.
- Medication Overuse: Ironically, taking acute pain relief medications too often can lead to medication overuse headaches, making prevention even more critical.
According to the American Migraine Foundation, a variety of factors can trigger a migraine headache. Identifying your specific triggers requires careful observation and tracking. Once identified, avoiding these triggers becomes a powerful tool in your prevention arsenal. For comprehensive strategies in managing chronic pain conditions, including migraines, explore our insights on chronic pain treatment.
Dietary Changes to Prevent Migraine Headaches?
Diet plays a significant role in migraine prevention for many individuals. While not everyone is sensitive to the same foods, recognizing and eliminating your personal dietary triggers can be a game-changer. The link between specific foods and migraines isn’t always strong for everyone, but if you notice a pattern, it’s worth investigating.
Here are some common dietary culprits and considerations:
- Aged Cheeses: These contain tyramine, an amino acid that can trigger migraines in some people.
- Alcohol and Red Wine: Especially red wine and port, alcohol can be a potent trigger. It can cause dehydration and contain compounds that affect blood vessels.
- Nitrates: Found in processed meats like hot dogs, bacon, and lunchmeats, nitrates can expand blood vessels, contributing to migraine pain.
- MSG (Monosodium Glutamate): A flavor improver often found in processed foods, MSG is a known trigger for some individuals.
- Aspartame: This artificial sweetener is another additive that has been linked to migraines in sensitive individuals.
- Caffeine Management: While a small amount of caffeine can sometimes alleviate early migraine pain, too much caffeine or sudden caffeine withdrawal can trigger an attack. If caffeine is a trigger for you, reducing intake gradually is key to avoiding withdrawal headaches. Skipping meals can also be a significant trigger, so maintaining regular eating times is crucial.
| Common Trigger Foods/Drinks | Potential Safer Alternatives |
|---|---|
| Aged Cheeses | Fresh cheeses (e.g., cottage cheese, ricotta) |
| Red Wine, Dark Alcohol | White wine (in moderation), clear spirits (in moderation) |
| Processed Meats (Nitrates) | Fresh, unprocessed meats and poultry |
| Foods with MSG | Whole, unprocessed foods; check labels carefully |
| Foods with Aspartame | Natural sweeteners (e.g., honey, maple syrup) or unsweetened options |
| Excessive Caffeine | Decaffeinated coffee/tea, herbal teas, water |
| Skipped Meals | Regular, balanced meals and healthy snacks |
The Role of a Headache Diary in Prevention
A headache diary is arguably one of the most powerful and accessible tools for how to prevent migraine headaches. It’s your personal detective kit for uncovering the unique patterns and triggers of your migraines. Without a detailed record, it’s easy to overlook connections between your environment, habits, and migraine attacks.
Here’s what a headache diary helps you do:
- Tracking Frequency and Severity: Documenting how often your migraines occur and how intense they are provides a baseline and helps you monitor the effectiveness of any preventive strategies you implement.
- Identifying Patterns: Over time, you’ll start to see correlations. Did a migraine always follow a night of poor sleep? Did it happen after consuming a specific food? Was it linked to a stressful event at work?
- Environmental Factors: Note changes in weather, strong smells, bright lights, or loud noises you encountered before an attack.
- Symptom Duration and Characteristics: Recording how long a migraine lasts and its specific symptoms (e.g., throbbing, nausea, aura) can provide valuable insights for your healthcare provider.
- Medication Effectiveness: Documenting what medications you took and how well they worked (or didn’t) helps refine your acute treatment plan.
By consistently recording this information, you and your pain management doctor can gain clarity on what makes you vulnerable to migraines and develop a targeted prevention plan. For more insights into how a structured approach can help manage complex pain conditions, refer to our guide on functional pain management.
Lifestyle Modifications: How to Prevent Migraine Headaches?
Beyond identifying and avoiding specific triggers, adopting a consistent and healthy lifestyle is fundamental to how to prevent migraine headaches. Many lifestyle factors can directly influence your migraine threshold, making you more or less susceptible to an attack.
At Midwest Pain and Wellness, we often emphasize a comprehensive approach that includes these healthy habits:
- The SEEDS Model: This mnemonic (Sleep, Eat, Exercise, Drink, Stress) summarizes key lifestyle areas to focus on for migraine prevention.
- Sleep: Maintain a regular sleep schedule, even on weekends. Go to bed and wake up at roughly the same time each day.
- Eat: Eat regular meals and avoid skipping them. This helps regulate blood sugar levels, which can be a migraine trigger for some.
- Exercise: Engage in regular physical activity.
- Drink: Stay well-hydrated throughout the day.
- Stress: Implement effective stress management techniques.
- Hydration Importance: Dehydration is a common and often overlooked migraine trigger. Carrying a water bottle and sipping water consistently throughout the day can make a significant difference.
- Consistent Meal Times: As mentioned, skipping meals or having irregular meal times can disrupt your body’s rhythm and trigger migraines. Aim for consistent meal schedules.
- Smoking Cessation: Smoking is detrimental to overall health and can exacerbate migraine symptoms. Quitting smoking is a crucial step for migraine prevention and overall well-being.
Incorporating these practices into your daily routine can significantly reduce the frequency and severity of your migraine attacks. For more strategies on optimizing your health and managing pain effectively, explore our resources on effective pain management strategies.
Stress Management and Sleep: How to Prevent Migraine Headaches?
Stress and sleep are deeply intertwined with migraine frequency and intensity. Effectively managing both is crucial for how to prevent migraine headaches.
Stress Management:
Stress is one of the most frequently reported migraine triggers. While it’s impossible to eliminate all stress, developing healthy coping mechanisms can significantly reduce its impact.
- Mindfulness Meditation: Practicing mindfulness can help you become more aware of your body’s responses to stress and teach you techniques to calm your nervous system.
- Deep Breathing Exercises: Simple deep breathing exercises can quickly activate your body’s relaxation response, reducing tension and anxiety.
- Cognitive Behavioral Therapy (CBT): CBT is a psychological therapy that helps you identify and change negative thought patterns and behaviors related to stress and pain, improving your ability to cope with migraines.
- Biofeedback: This technique uses electronic sensors to monitor your body’s physiological responses (like heart rate, muscle tension, or skin temperature). By seeing these responses in real-time, you can learn to control them, helping you manage stress and potentially reduce migraine frequency. At Midwest Pain and Wellness, we offer biofeedback for migraine prevention as part of our comprehensive treatment plans.
Sleep Hygiene:
Consistent, quality sleep is vital for migraine prevention. Irregular sleep patterns can throw off your body’s circadian rhythm, making you more susceptible to attacks.
- Establish a Regular Sleep Schedule: Go to bed and wake up at the same time every day, even on weekends.
- Create a Relaxing Bedtime Routine: Unwind with activities like a warm bath, reading, or listening to calming music.
- Optimize Your Sleep Environment: Ensure your bedroom is dark, quiet, and cool. Avoid screens (phones, tablets, TV) for at least an hour before bed.
- Limit Naps: If you must nap, keep it short (20-30 minutes) to avoid disrupting nighttime sleep.
- Avoid Caffeine and Alcohol Before Bed: These substances can interfere with sleep quality.
Benefits of Regular Exercise for Prevention
Regular exercise is not just good for your general health; it’s a powerful tool in your migraine prevention strategy. Physical activity can help reduce migraine frequency and severity, making it an important component of how to prevent migraine headaches.
Here’s how exercise helps:
- Endorphin Release: Exercise releases endorphins, natural painkillers and mood elevators, which can help counteract the chemical imbalances associated with migraines.
- Stress Reduction: As we’ve discussed, stress is a major migraine trigger. Exercise is an excellent stress reliever, helping to manage tension and anxiety.
- Improved Sleep: Regular physical activity can lead to better sleep quality, which in turn helps stabilize your migraine threshold.
- Weight Management: Obesity is linked to an increased risk of chronic headaches. Maintaining a healthy weight through exercise can contribute to migraine management.
Types of Exercise:
Focus on regular, moderate aerobic activities.
- Walking and Jogging: These are accessible forms of exercise that can be easily incorporated into most routines.
- Cycling: Whether outdoors or on a stationary bike, cycling is a great cardiovascular workout.
- Swimming: A low-impact option that can be very relaxing.
Important Considerations:
While exercise is beneficial, it’s crucial to approach it mindfully. Very vigorous or sudden, intense exercise can sometimes trigger a migraine in some individuals.
- Ease Into It Gradually: Start with gentle activities and slowly increase intensity and duration.
- Warm Up Slowly: Always include a warm-up period to prepare your body for activity.
- Stay Hydrated: Drink plenty of water before, during, and after exercise.
Scientific research supports the benefits of exercise. A systematic review and meta-analysis published in Scand J Med Sci Sports concluded that aerobic exercise is helpful in patients with migraine, showing a positive impact on migraine frequency.
Medical and Interventional Prevention Strategies
While lifestyle adjustments and trigger avoidance are crucial, for many individuals, particularly those with frequent or severe attacks, medical interventions are necessary to effectively learn how to prevent migraine headaches. It’s important to distinguish between acute treatments (taken to stop a migraine once it starts) and preventive treatments (taken regularly to reduce the frequency, severity, and duration of attacks).
Medication overuse headaches, caused by taking acute pain relievers too frequently, can complicate treatment. This is why a focus on prevention is so critical. Our double board-certified specialists at Midwest Pain and Wellness are experts in evaluating your condition and recommending the most appropriate medical and interventional strategies. We offer comprehensive care for a wide range of conditions, and you can learn more about the conditions we treat on our website.
Preventive Medications and How They Work
Preventive medications are taken consistently, often daily, to raise your migraine threshold and make your brain less susceptible to triggers. Many of these medications were originally developed for other conditions, but their migraine-fighting effects were observed over time.
Here are some common types of preventive medications:
- Beta-Blockers: Medications like propranolol and metoprolol, often used for high blood pressure or heart conditions, can help prevent migraines. They work by blocking the effects of adrenaline, which can narrow blood vessels and impact nerve signals involved in migraines.
- Anticonvulsants (Anti-Seizure Medications): Drugs such as topiramate and valproate sodium (divalproex) are effective for some migraine sufferers. Their mechanism is thought to involve stabilizing nerve cell activity in the brain, reducing the excitability that can lead to a migraine.
- Tricyclic Antidepressants: Amitriptyline and nortriptyline are examples of these antidepressants that can be prescribed at lower doses for migraine prevention. They are believed to affect neurotransmitters like serotonin and norepinephrine, which play a role in pain perception and migraine pathways.
- Anti-CGRP Monoclonal Antibodies (CGRP Inhibitors): This newer class of medications specifically targets calcitonin gene-related peptide (CGRP) or its receptor. CGRP is a protein involved in pain signaling during a migraine attack. By blocking CGRP, these medications can reduce migraine frequency and severity. Examples include erenumab and fremanezumab, which are administered via injection. Other CGRP inhibitors like galcanezumab and eptinezumab also fall into this category.
- Gepants: These are small molecule CGRP receptor antagonists that can be taken orally. Examples like atogepant are specifically approved for daily use in migraine prevention.
It’s important to discuss potential side effects with your doctor, as they vary greatly depending on the medication. Some common side effects across these classes might include fatigue, dizziness, weight changes, or gastrointestinal issues. Your physician will help you weigh the benefits against these potential side effects.
Interventional Treatments and Alternative Therapies
For individuals whose migraines are not adequately controlled by oral medications or who experience significant side effects, interventional treatments and alternative therapies offer additional avenues for prevention. Our team at Midwest Pain and Wellness specializes in these advanced, opioid-free approaches to help you achieve lasting relief.
- Botox Injections: OnabotulinumtoxinA (Botox) injections have been approved for the preventive treatment of chronic migraine, defined as 15 or more headache days per month. It works by blocking the release of certain chemicals involved in pain transmission. We offer specialized Botox for chronic migraine at our Chicago Ridge location.
- Nerve Blocks and Trigger Point Injections: These procedures involve injecting local anesthetics or corticosteroids near specific nerves or into muscle trigger points that are contributing to migraine pain. By numbing or relaxing these areas, they can help interrupt pain signals and reduce migraine frequency.
- Transcutaneous Supraorbital Nerve Stimulation (t-SNS): This is a non-invasive device that uses electrical impulses to stimulate the trigeminal nerve, which is implicated in migraine pathways. It’s applied to the forehead and can be used daily for prevention.
- Acupuncture: Originating from traditional Chinese medicine, acupuncture involves inserting thin needles into specific points on the body. Some studies suggest that acupuncture may have a small effect in reducing episodic migraine frequency compared to sham acupuncture.
- Biofeedback: As mentioned earlier, biofeedback teaches you to control involuntary bodily functions like muscle tension and heart rate, which can help manage stress and reduce migraine susceptibility.
- Nutritional Supplements: Some vitamins and minerals have shown promise in migraine prevention, though evidence varies. These include:
- Magnesium: Studies have shown that magnesium supplementation can reduce migraine frequency and severity for some individuals.
- Riboflavin (Vitamin B-2): High doses of riboflavin may help reduce the number of migraines and their pain.
- Coenzyme Q10 (CoQ10): This antioxidant may also help decrease migraine frequency.
- Feverfew: An herb traditionally used for headaches, some evidence suggests it might reduce migraine frequency. However, always consult your doctor before taking herbal supplements, as quality and safety can vary.
When considering any of these treatments, especially alternative therapies, it’s crucial to do so under the guidance of a qualified healthcare professional to ensure safety and effectiveness.
Frequently Asked Questions about Migraine Prevention
How long does it typically take for preventive medications to become effective?
Patience is a virtue when starting preventive migraine medications. It’s not an instant fix, and it often requires a trial period to find the right medication and dosage for you.
For oral preventive medications (excluding gepants), you typically need about a month to gradually increase the dose (titration phase). Once you reach an effective dose, it can take another two to three months to observe the full benefit and a noticeable decrease in migraine frequency or severity. This means you might need to be on an oral preventive for a total of three to four months before deciding if it’s working.
For Botox injections, which are used for chronic migraine, at least two cycles (administered every three months) are usually recommended before assessing effectiveness. So, you might be looking at six months or more.
CGRP monoclonal antibodies can sometimes show improvement sooner, but a trial period of three to six months is often recommended to fully evaluate their efficacy.
The key takeaway is consistency in adherence. Taking your medication exactly as prescribed, even if you don’t see immediate results, is essential for its potential to work. If you’re not seeing improvement after the recommended trial period, your doctor may adjust the dose, switch to a different medication, or consider combination therapy.
When should someone consider seeking professional help for migraine prevention?
Deciding when to seek professional help for how to prevent migraine headaches is a critical step in managing your condition and improving your quality of life. While over-the-counter remedies and lifestyle changes can help some, there are clear indicators that it’s time to consult with a specialist.
You should consider seeking professional help from a pain management doctor if:
- Life Disruption: Your migraines are significantly interfering with your daily activities, work, school, or personal life. If you’re frequently missing out on events or responsibilities because of migraines, it’s time to act.
- Frequency of Attacks: You’re experiencing frequent migraine attacks, generally considered to be four or more migraine days per month, or if you have more than 10 headache days per month. If you’re having migraines two or three times a week, a preventive strategy is likely warranted.
- Ineffective Over-the-Counter (OTC) Medications: OTC pain relievers (like ibuprofen, acetaminophen, or naproxen) are not providing adequate relief, or you find yourself needing to take them more than two to three days a week. Overusing these medications can lead to medication overuse headaches, creating a vicious cycle.
- New or Worsening Symptoms: You experience a sudden change in headache pattern, severity, or new neurological symptoms (like weakness, vision changes, or numbness) that you haven’t had before.
- Severe Attacks: Your migraines are exceptionally severe, lasting longer than 72 hours, or are accompanied by disabling symptoms like extreme nausea, vomiting, or prolonged aura.
- Concerns about Side Effects: You’re worried about the side effects of your current medications or are looking for alternatives.
At Midwest Pain and Wellness, our double board-certified pain management doctors specialize in diagnosing and treating complex pain conditions like migraines. We understand the nuances of this disabling condition and can help you develop a personalized, opioid-free prevention plan. If you’re wondering what is a pain management doctor?, know that we are experts dedicated to long-term pain relief through advanced, interventional approaches.
Are there specific preventive strategies for menstrual migraines?
Yes, menstrual migraines, which are migraines that occur around a woman’s menstrual cycle, often require specific preventive strategies due to their strong link to hormonal fluctuations, particularly drops in estrogen. These types of migraines tend to be more severe and debilitating.
Here are some specific preventive strategies for menstrual migraines:
- Proactive Medication (Mini-Prophylaxis): For women with predictable menstrual migraines, a short course of preventive medication can be taken just before and during the susceptible window (e.g., a few days before menstruation and during the first few days). This might involve:
- NSAIDs (Nonsteroidal Anti-inflammatory Drugs): Taken daily during the at-risk period.
- Triptans: Low-dose triptans can be taken daily during this window.
- Magnesium Supplementation: Some women find magnesium taken daily throughout the cycle, or specifically around menstruation, to be helpful.
- Birth Control Discussion: For some women, hormonal birth control (oral contraceptives, patches, or rings) can help stabilize estrogen levels, reducing menstrual migraine frequency. However, for others, particularly those with migraine with aura, certain hormonal contraceptives can be contraindicated due to an increased risk of stroke. A thorough discussion with your doctor is essential to weigh the risks and benefits.
- Estrogen Management: In some cases, transdermal estrogen patches or gels can be used around the menstrual period to prevent the sharp drop in estrogen that triggers migraines.
- Continuous Oral Contraceptives: Taking oral contraceptives continuously (without the placebo week) can suppress menstruation and thus prevent the hormonal fluctuations that trigger migraines for some women.
- General Migraine Prevention: Alongside these specific strategies, maintaining overall healthy lifestyle habits, managing stress, and avoiding other identified triggers remain crucial for women with menstrual migraines.
Because hormonal migraines are complex and individualized, working closely with your healthcare provider is paramount to finding the safest and most effective preventive strategy for you.
Conclusion
Living with migraines can be incredibly challenging, but achieving headache-free living is within reach with the right strategies and support. Understanding how to prevent migraine headaches involves a multi-faceted approach, combining lifestyle modifications, trigger avoidance, and, when necessary, advanced medical interventions.
At Midwest Pain and Wellness, our commitment is to provide comprehensive, opioid-free pain management using current, evidence-based therapies. Our double board-certified doctors use a multi-modal, interventional approach, collaborating with other practitioners to create custom care plans custom to your unique needs for long-term pain relief. We believe in empowering our patients in Chicago Ridge, Illinois, and surrounding areas to regain control over their lives, free from the debilitating grip of migraines.
Don’t let migraines dictate your life any longer. Take the first step towards a headache-free future. We invite you to schedule a consultation for migraine relief with our expert team today.